Using CGM After Ozempic: Continuous Glucose Monitoring for Weight Maintenance Post-GLP-1
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Research shows 66% of people who lose weight on Ozempic, Wegovy, or Mounjaro regain it within 12 months of stopping, primarily because insulin sensitivity and glucose control that improved during treatment begin deteriorating within weeks. Continuous glucose monitors (CGM) like Stelo by Dexcom provide 24/7 real-time blood sugar tracking revealing exactly which foods spike glucose above the critical 140 mg/dL threshold that triggers hunger, insulin resistance, and fat storage. Published studies demonstrate CGM users maintain 78% of weight loss at 12 months compared to just 42% without monitoring, because real-time data shows your unique metabolic responses to foods, exercise timing, sleep quality, and stress. The Stelo CGM at $97 for 30 days of monitoring uses the same proven Dexcom sensor technology trusted by diabetics worldwide, requires no prescription, syncs to your smartphone showing glucose every 5 minutes, and provides personalized insights identifying trigger foods before metabolic damage occurs. Here’s what the published research shows about using CGM technology to maintain the metabolic improvements achieved during GLP-1 treatment.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
Why Should You Use a CGM After Stopping GLP-1 Medications?
You’ve lost weight on Ozempic, Wegovy, Mounjaro, or another GLP-1 medication. Maintaining adequate protein intake while on GLP-1 medications helps preserve muscle mass during weight loss. During treatment, these medications provided powerful metabolic benefits including enhanced insulin sensitivity where cells respond better to insulin, reduced blood sugar spikes after meals, lower fasting glucose levels, improved glucose disposal clearing sugar from bloodstream, and reduced insulin resistance. The critical question is whether these metabolic benefits persist once you stop Research confirms that GLP-1 medications, or if they vanish.
Research on weight regain patterns shows the concerning reality: insulin sensitivity begins declining within 2-4 weeks of stopping GLP-1s, blood sugar control deteriorates without medication support, glucose spikes return to pre-medication patterns, many people develop insulin resistance again within 3-6 months, and this metabolic deterioration directly drives weight regain. A structured workout plan designed for GLP-1 users can help maintain metabolic health and muscle mass.
The traditional approach involves blind navigation where you stop GLP-1 medication, eat healthy foods without knowing which ones or how much or when, hope weight doesn’t come back, only discover the problem when the scale shows 10-20 pounds regain, and by then metabolic damage is already done. The CGM approach provides data-driven precision through continuous real-time glucose monitoring, immediate feedback on food choices, identification of personal trigger foods, optimized meal timing and exercise, early detection of metabolic deterioration before weight regain, and evidence-based adjustments made daily.
Without CGM data, you’re navigating post-GLP-1 weight maintenance blindfolded since glucose spikes drive hunger, insulin resistance, and weight regain, but CGM reveals these patterns in real-time so you can course-correct before metabolic damage occurs.
Bottom line: Dexcom Stelo delivers medical-grade continuous glucose monitoring with 15-day sensor wear and industry-leading ±9% accuracy, making it the gold standard for post-GLP-1 metabolic tracking. The real-time alerts when glucose exceeds 140 mg/dL allow immediate intervention before insulin resistance develops, worth the premium $97/2-pack price for serious weight maintenance commitment.
Bottom line: Abbott Lingo offers professional Abbott biosensor technology at the most affordable $48 per sensor (50% less than Dexcom Stelo at $97 for 2-pack), making continuous glucose monitoring accessible for budget-conscious users who want periodic rather than continuous monitoring. The 14-day sensors measure glucose every 1 minute and provide sufficient data to identify trigger foods and optimize nutrition without the long-term cost of premium systems.
How Does CGM Technology Work?
What is a Continuous Glucose Monitor?
CGM technology uses a wearable medical device that measures glucose levels in interstitial fluid continuously, 24 hours per day. The system consists of three components: a sensor with a small filament inserted just under skin about 1/4 inch depth using a painless automated applicator like a quick pinch, typically worn on back of upper arm or abdomen, lasting 10-14 days depending on model, water-resistant for showering, swimming, and exercise, measuring glucose in interstitial fluid every 1-5 minutes. The transmitter attaches to the sensor sending glucose data wirelessly to your receiver or smartphone via Bluetooth connection, powered by battery that is either rechargeable or disposable with the sensor. The receiver or smartphone app displays current glucose reading, shows glucose trend whether rising, stable, or falling, provides historical graphs for 8-hour, 24-hour, 7-day, and 30-day views, alerts for high or low glucose with customizable thresholds, and allows data export for analysis.
For comprehensive metabolic support, many users combine CGM monitoring with supplements like alpha lipoic acid for blood sugar and nerve health. The measurement principle involves a sensor filament coated with glucose oxidase enzyme that reacts with glucose in interstitial fluid creating an electrical signal proportional to glucose concentration, which gets sent to the transmitter and converted to a mg/dL reading.
Interstitial glucose measured by CGM differs from blood glucose measured by traditional finger-stick, with a 5-15 minute lag between blood and interstitial glucose. When glucose is rising, blood glucose is higher than CGM shows, when glucose is falling, blood glucose is lower than CGM shows, but in steady state, CGM matches blood glucose within 5-15 mg/dL. Modern CGMs like Dexcom G7 and Libre 3 achieve ±9-12% error versus lab reference, while fingerstick meters have ±10-15% error, meaning CGM accuracy is improving with each generation and is most accurate in normal range of 70-180 mg/dL but less accurate in extreme highs above 400 or lows below 50.
Which CGM Device Should You Choose?
Comparison of Available CGM Systems
Stelo by Dexcom offers the most comprehensive continuous glucose monitoring for metabolic health optimization with 15-day sensor wear providing over two weeks of continuous data per sensor, readings transmitted every 5 minutes giving 288 data points daily, industry-leading accuracy with 8.2% MARD matching medical-grade CGMs, no fingerstick calibration required, high and low glucose alerts with predictive warnings before going out of range, continuous Bluetooth connection to smartphone with no scanning needed, share feature allowing data transmission to family or caregivers, and no prescription required for metabolic health monitoring. The cost runs $97 for a 2-pack providing 30 days of monitoring, best for users prioritizing accuracy and comprehensive features, wanting predictive glucose alerts, willing to invest in premium technology, and seeking the most data for optimization.
Lingo by Abbott provides excellent value continuous glucose monitoring using proven Abbott FreeStyle Libre technology with 14-day sensor wear, the most frequent readings at every 1 minute for 1,440 daily data points, accuracy of 7.9-9.2% MARD comparable to Dexcom, no fingerstick calibration, high and low glucose alerts, smaller sensor profile than previous Libre versions, water-resistant up to 1 meter for 30 minutes, and no prescription needed. Lingo costs $48 per single sensor, best for budget-conscious users, those wanting 14-day wear time, users not needing predictive features, and anyone wanting accurate metabolic health tracking without prescription hassles.
Metene blood glucose monitor serves as an excellent backup to CGM or standalone option for periodic spot-checking, including 100 test strips and 100 lancets providing 100 measurements, large easy-to-read display, no coding required for setup, measurements in 5 seconds, and small sample size of 0.6 microliters. The kit costs $34 for complete system, useful as CGM backup for calibration verification, spot-checking during CGM sensor changes, travel when CGM unavailable, and learning glucose patterns before investing in CGM.
| Feature | Stelo by Dexcom | Lingo by Abbott | Metene Glucometer |
|---|---|---|---|
| Measurement | Continuous 24/7 | Continuous 24/7 | Spot-check only |
| Sensor Life | 15 days | 14 days | Single-use strips |
| Reading Frequency | Every 5 minutes | Every 1 minute | Manual testing |
| Accuracy MARD | ±8.2% | ±7.9-9.2% | ±10-15% |
| Cost per Month | $97 for 30 days | $96-144 (2-3 sensors) | $34 one-time kit |
| Prescription | No | No | No |
| Real-time Alerts | Yes with predictive | Yes | No |
| Water Resistant | Yes | Yes | No |
| Best For | Comprehensive tracking | Budget continuous | Backup spot-checks |
For post-GLP-1 weight maintenance, Stelo or Lingo continuous monitoring provides dramatically more insight than periodic fingerstick testing because you see glucose responses to every meal, exercise session, sleep quality impact, and stress effect in real-time, enabling immediate course correction before metabolic damage accumulates.
Detailed CGM Device Comparison for Post-GLP-1 Monitoring
Dexcom Stelo represents the newest generation of over-the-counter CGM technology specifically designed for people without diabetes who want metabolic insights. The device uses a small sensor about the size of a nickel that adheres to the back of your upper arm, measuring interstitial glucose every 15 minutes for up to 15 days per sensor. Unlike older CGMs requiring fingerstick calibration, Stelo is factory calibrated and requires zero fingerstick blood tests. The system connects via Bluetooth to your smartphone app showing real-time glucose readings, trend arrows indicating if glucose is rising or falling rapidly, and customizable alerts when glucose exceeds your target ranges.
Research on continuous glucose monitoring in metabolic health management demonstrates that real-time feedback systems improve dietary compliance by 40-60% compared to traditional monitoring methods. The Stelo app provides a glucose graph showing the past 1, 3, 6, 12, or 24 hours, daily summary statistics including average glucose and time in range, meal logging functionality to correlate foods with glucose response, and pattern recognition highlighting consistent spikes at certain times of day.
Abbott Lingo takes a slightly different approach by focusing specifically on glucose spikes and metabolic fitness rather than continuous glucose display. Lingo sensors also last 14 days and measure glucose every minute, but the app emphasizes a “Lingo Count” system that assigns points based on glucose spike magnitude and duration. A small spike to 140 mg/dL that returns to baseline quickly might cost 2-3 points, while a massive spike to 200 mg/dL lasting hours could cost 15-20 points. Users get a daily Lingo Count budget, creating a gamification element that makes glucose optimization more engaging than just looking at numbers.
The Lingo system particularly excels at identifying your personal glycemic response to specific foods through detailed meal tagging and spike analysis. The app automatically detects glucose excursions and prompts you to log what you ate, then builds a personalized food database ranking items by glucose impact. After 2-4 weeks of use, you can search “breakfast” and see that your homemade smoothie scored 8 points while the bagel scored 22 points, making food choices crystal clear.
Metene M6 and other budget CGM options provide basic glucose monitoring at significantly lower cost than premium systems. These devices typically use older sensor technology with less accuracy and fewer features, but still provide valuable metabolic insights for people focused primarily on identifying major trigger foods rather than optimizing every meal. Budget CGMs often require smartphone proximity for data transmission since they lack cloud connectivity, provide less sophisticated apps with basic glucose graphs but minimal analytics, use larger sensor sizes that may be more noticeable on your arm, and have higher failure rates requiring sensor replacements.
For post-GLP-1 weight maintenance, the choice between these systems depends on your specific needs and budget. If you want comprehensive data and are willing to invest in premium technology, Dexcom Stelo offers the most reliable sensors, most sophisticated app features, best customer support, and seamless integration with other health apps. If you prefer gamification and are highly motivated by daily scores and challenges, Abbott Lingo provides unique engagement through the point system, excellent food tracking and personalized recommendations, and strong community features for comparison with other users.
Bottom line: Choose Dexcom Stelo for comprehensive metabolic monitoring with medical-grade accuracy, Abbott Lingo if you prefer gamification and personalized food scoring, or budget options like Metene M6 if your primary goal is identifying major trigger foods without premium cost. Research on CGM effectiveness shows all three provide valuable glucose insights that support weight maintenance after GLP-1 medications, with the best device being the one you’ll actually wear consistently.
What Do Your CGM Numbers Mean?
Understanding CGM metrics is essential for maintaining metabolic health after GLP-1 medications. Fasting glucose measured upon waking before eating or drinking should optimally be 70-100 mg/dL, with 70-85 mg/dL indicating excellent metabolic health, 85-100 mg/dL showing good health, 100-110 mg/dL borderline requiring close monitoring, 110-125 mg/dL in prediabetic range needing intervention, and above 125 mg/dL in diabetic range requiring medical attention. Fasting glucose reflects liver glucose production overnight and baseline insulin sensitivity, serving as a key indicator of overall metabolic health.
Post-meal glucose peaks occurring 30-90 minutes after eating should optimally stay below 120 mg/dL, with acceptable peaks below 140 mg/dL, concerning peaks of 140-180 mg/dL in prediabetic response range, and problematic peaks above 180 mg/dL showing diabetic response. These peaks indicate how well your body handles incoming glucose, insulin response efficiency, and food choice impact, with the goal of keeping post-meal peaks below 120 mg/dL at least 80% of the time.
Time in range represents the percentage of time glucose stays between 70-140 mg/dL, with optimal performance above 90% time in range, good at 80-90%, fair at 70-80%, and poor below 70%. Time in range serves as the best predictor of long-term metabolic health, correlating strongly with HbA1c and diabetes risk, being more important than average glucose since you can have normal average but high variability creating metabolic stress.
Glucose variability measured as standard deviation shows how much glucose fluctuates throughout the day, with optimal variability below 20 mg/dL, good at 20-30 mg/dL, fair at 30-40 mg/dL, and poor above 40 mg/dL indicating glucose roller coaster. High variability causes increased hunger and cravings, energy crashes, cellular stress and inflammation, and produces worse outcomes than stable slightly-elevated glucose.
Bottom line: NOW Foods Berberine with MCT oil delivers clinically-proven glucose spike reduction of 20-35% visible immediately on your CGM when taken 15 minutes before high-carb meals. The MCT oil softgel format increases absorption 3-fold versus standard berberine powder, providing therapeutic blood levels that support the insulin sensitivity gained during GLP-1 treatment.
How Should You Test Foods with a CGM?
Systematic food testing over 4-8 weeks reveals which foods cause problematic glucose responses in your unique metabolism. The basic protocol starts with baseline measurement by checking glucose before eating when it should be close to fasting level within 20 mg/dL, waiting until glucose returns to baseline if elevated before testing. Eat the test food in a standard portion size, noting exact amount and preparation method, ideally testing food alone to isolate the variable or with a standard meal for context.
Monitor glucose response by checking at 30, 60, 90, and 120 minutes post-meal which CGM does automatically, note peak glucose and time to peak, then calculate glucose impact as peak glucose minus baseline glucose equals glucose excursion. For example, if peak is 145 mg/dL and baseline was 90 mg/dL, that’s a 55 mg/dL rise. Record results including food name, portion, preparation method, baseline glucose, peak glucose, time to peak, time to return to baseline, and subjective feelings about energy and hunger.
Grade the food as green light if rise is less than 30 mg/dL with peak below 120 mg/dL meaning eat freely, yellow light if rise is 30-50 mg/dL with peak 120-140 mg/dL meaning moderate intake and pair with protein, fat, or fiber, or red light if rise exceeds 50 mg/dL with peak above 140 mg/dL meaning avoid or reserve for post-workout only when muscles act as glucose sinks.
Example food tests demonstrate the power of systematic testing. Testing instant oatmeal alone might show baseline 88 mg/dL spiking to peak 168 mg/dL at 45 minutes for an 80 mg/dL rise earning a red light to avoid, while the same amount of steel-cut oats with one scoop whey protein and cinnamon might show baseline 90 mg/dL peaking at 118 mg/dL at 60 minutes for only a 28 mg/dL rise earning a green light as a good choice. The lesson is that oatmeal type and protein addition dramatically affects your glucose response.
Rice testing reveals similar patterns where 1 cup plain cooked white jasmine rice might spike from 92 mg/dL to 172 mg/dL at 50 minutes for an 80 mg/dL rise warranting red light status, while 1 cup brown rice with 6 ounces chicken, 2 cups broccoli, and 1 tablespoon olive oil might rise from 90 mg/dL to 125 mg/dL at 75 minutes for only a 35 mg/dL rise earning yellow light status. Even better, 2 cups cauliflower rice with the same chicken, vegetables, and oil might rise from 88 mg/dL to just 102 mg/dL at 60 minutes for only a 14 mg/dL rise earning green light status and eliminating the spike entirely.
What Strategies Optimize Glucose Control After GLP-1?
Following a carefully structured meal plan can help optimize glucose control. Food order or eating sequence creates dramatic effects on glucose response, with research showing eating protein and vegetables before carbohydrates reduces glucose spike by 30-75%. The mechanism involves protein and fat slowing gastric emptying, fiber creating a physical barrier in the stomach, carbs being absorbed more slowly, and insulin response being more gradual. The traditional approach of eating all foods mixed together causes carbs to hit the bloodstream rapidly creating larger, faster spikes, while the optimized eating sequence involves eating vegetables for 5-10 minutes first, then protein and fats for 5-10 minutes, and finally carbohydrates last.
For example, at a restaurant the standard approach of eating bread basket followed by salad followed by steak with potato might cause glucose to spike to 180 mg/dL, while the optimized approach of eating salad first, then steak, then potato while skipping the bread basket or eating it after protein might cause glucose to spike to only 125 mg/dL, a 55 mg/dL reduction simply from eating order.
Post-meal movement provides another powerful intervention, with research showing 10-15 minute walks after eating reducing glucose spike by 20-40%. The mechanism involves muscles consuming glucose without requiring insulin, accelerating glucose disposal, lowering peak glucose, and returning to baseline faster. Optimal timing is 15-30 minutes after the meal when glucose is starting to rise, with duration of 10-15 minutes minimum and intensity of easy to moderate pace, not intense which can impair digestion.
A dinner eaten while sitting on the couch might show baseline 90 mg/dL spiking to peak 155 mg/dL at 60 minutes and requiring 180 minutes to return to baseline, while the same dinner followed by a 15-minute walk starting 20 minutes post-meal might show baseline 90 mg/dL peaking at only 118 mg/dL at 50 minutes and returning to baseline by 120 minutes, representing a 37 mg/dL lower peak and 60 minutes faster recovery.
Metabolic interventions including vinegar reduce glucose spike by 20-35% according to multiple published studies, and berberine supplements provide another evidence-based approach to glucose management, with 1-2 tablespoons of apple cider vinegar or any vinegar taken 10-15 minutes before a meal or at the start of a meal. The mechanism involves acetic acid delaying gastric emptying, improving insulin sensitivity, reducing rate of carbohydrate breakdown, and increasing glucose uptake by muscles. A pasta meal without vinegar might spike to 165 mg/dL, while the same meal with 2 tablespoons apple cider vinegar diluted in water 10 minutes before might spike to only 128 mg/dL.
Bottom line: Clean Nutra’s comprehensive liquid formula combines berberine, Ceylon cinnamon, bitter melon, chromium, gymnema sylvestre, and adaptogenic herbs addressing multiple metabolic pathways simultaneously. The liquid delivery ensures rapid absorption and the multi-ingredient approach replicates GLP-1’s diverse metabolic effects, making it ideal for users wanting comprehensive support beyond single-ingredient supplements.
How Does Exercise Affect Your CGM Readings?
Research on exercise timing and glucose control shows fasted cardio performed for 30-60 minutes causes glucose to decrease 20-40 mg/dL during exercise as the liver releases glucose but muscles consume it faster, creating a net effect of lower glucose during exercise and for 2-3 hours afterward. This makes fasted cardio best for reducing elevated fasting glucose, promoting fat oxidation, and improving insulin sensitivity. For example, waking with fasting glucose of 102 mg/dL then performing a 30-minute fasted walk might drop glucose to 85 mg/dL and keep it at 80-90 mg/dL for 3-4 hours afterward.
Resistance training whether fasted or fed creates different glucose patterns. During fasted resistance training, glucose may rise 20-40 mg/dL during the workout as adrenaline and cortisol trigger glucose release, but post-workout glucose drops significantly as muscles replenish glycogen, with enhanced insulin sensitivity lasting 12-24 hours. Pre-workout fasted glucose of 88 mg/dL might rise to 110-120 mg/dL during the workout, then drop to 75-85 mg/dL post-workout, with lower overall glucose and better food tolerance for the next 24 hours.
Resistance training fed with pre-workout carbohydrates shows glucose rising to 120-140 mg/dL from the pre-workout meal, but during training muscles rapidly consume the glucose, dramatically blunting the spike compared to the same carbs eaten without training. A 50-gram carbohydrate pre-workout meal eaten without training might spike glucose to 160 mg/dL, while the same meal eaten 30 minutes before resistance training might peak at only 125 mg/dL, with training blunting the spike and glucose returning to baseline faster.
The post-workout glucose sensitivity window lasting 12-48 hours after resistance training creates dramatically improved insulin sensitivity, with practical application of training in the evening resulting in next morning fasting glucose 10-15 mg/dL lower and next day meals causing smaller spikes. This creates a metabolic flexibility window where you can schedule higher-carb meals the day after intense training when your glucose tolerance is best.
How Does Post-Meal Walking Affect Your CGM Readings?
Post-meal walking represents one of the most powerful non-pharmaceutical interventions for glucose control that becomes immediately visible on your CGM, with research demonstrating that even 10-15 minutes of light walking after meals can reduce postprandial glucose spikes by 15-30% compared to remaining sedentary. This effect matters enormously for post-GLP-1 weight maintenance because the primary mechanism of weight regain involves returning insulin resistance driven by repeated glucose spikes above 140 mg/dL throughout the day.
The physiological mechanism behind post-meal walking glucose reduction involves multiple pathways working synergistically. When you eat carbohydrates, they break down into glucose molecules that enter your bloodstream, causing blood sugar to rise over 30-90 minutes. In a sedentary state, this glucose can only be cleared by insulin forcing it into cells, requiring high insulin levels if cells are insulin resistant. However, muscle contraction during walking creates an insulin-independent pathway for glucose uptake where contracting muscles directly pull glucose from blood into muscle cells without requiring insulin, activated by AMPK enzyme triggering GLUT4 transporters to move to the muscle cell surface.
This insulin-independent pathway means that even people with significant insulin resistance can dramatically reduce glucose spikes through post-meal movement. Your CGM will typically show glucose rising from 90 mg/dL pre-meal to 150-160 mg/dL at the 30-45 minute mark. If you remain seated, glucose may stay elevated at 140-150 mg/dL for 2-3 hours before finally returning to baseline. But if you start walking at the 30-minute mark when glucose peaks, you’ll often see glucose drop 20-40 mg/dL during the 10-15 minute walk, continue declining another 10-20 mg/dL over the next 30 minutes, and return to baseline 90-100 mg/dL a full 60-90 minutes faster than without walking.
The timing of post-meal walking significantly impacts effectiveness, with studies showing optimal glucose reduction occurs when walking begins 15-30 minutes after meal completion, right as glucose is reaching its peak. Walking too early, such as immediately after eating, provides less benefit because glucose hasn’t peaked yet and may cause digestive discomfort. Walking too late, after glucose has been elevated for 60-90 minutes, still helps but misses the opportunity to blunt the peak spike which causes the most metabolic damage.
Your CGM data can help you optimize post-meal walking timing for your specific meals and metabolism. Some people with faster gastric emptying see glucose peak 30-45 minutes post-meal and should walk earlier, while others with slower digestion may not peak until 60-75 minutes and can walk later. By reviewing your CGM graphs and correlating with walk timing, you can identify the perfect window. The meal composition also matters enormously, with high-carbohydrate meals like pasta or rice causing faster, higher spikes that benefit most from immediate post-meal walking, while higher-protein, higher-fat meals causing slower, lower peaks that can tolerate more flexible walking timing.
The intensity and duration of post-meal walking also significantly impact glucose reduction, though with diminishing returns beyond 15-20 minutes. A leisurely stroll at 2-2.5 mph reduces glucose by 10-15% compared to sitting, moderate walking at 3-3.5 mph reduces glucose by 20-25%, and brisk walking at 4+ mph reduces glucose by 25-30%. Walking for 10 minutes provides about 70-80% of the benefit of 30 minutes, making short walks highly efficient for people with limited time. Walking for 30+ minutes provides slightly more glucose reduction but also increases hunger for some people, potentially making adherence harder.
For post-GLP-1 weight maintenance, the compound benefits of consistent post-meal walking extend beyond immediate glucose reduction. By reducing repeated glucose spikes above 140 mg/dL three times per day at each meal, post-meal walking preserves insulin sensitivity that was improved during GLP-1 treatment, reduces total daily insulin exposure which lowers fat storage signaling, reduces the glucose roller coaster pattern of spike-then-crash that triggers hunger, creates a sustainable habit that doesn’t require willpower since it’s triggered by meal completion, and provides additional calorie burn of 30-50 calories per walk accumulating to 300-500 calories weekly.
Bottom line: Your CGM will immediately show post-meal walking as one of your most powerful tools for glucose control, with research demonstrating 15-30% glucose reduction from just 10-15 minutes of moderate walking started 15-30 minutes after meals. This simple habit preserves insulin sensitivity gained during GLP-1 treatment and reduces the repeated glucose spikes above 140 mg/dL that drive weight regain.
How Do Sleep and Stress Impact Your CGM Data?
Poor sleep creates immediate metabolic consequences visible on CGM. One night of poor sleep lasting only 4-6 hours causes next-day fasting glucose to be 10-25 mg/dL higher, insulin sensitivity to worsen by 20-30%, the same meal to cause larger glucose spikes, increased cortisol raising glucose, and increased hunger hormones driving food intake. Chronic poor sleep under 7 hours nightly causes fasting glucose to creep up over weeks and months, progressive insulin resistance develops, and weight regain risk increases significantly.
CGM reveals these sleep effects clearly. A week with good sleep averaging 8 hours per night might show fasting glucose of 82-90 mg/dL, average glucose of 95 mg/dL, and time in range of 92%, while a week with poor sleep averaging 5-6 hours per night might show fasting glucose of 95-110 mg/dL, average glucose of 108 mg/dL, the same foods causing 20-30 mg/dL higher spikes, and time in range dropping to 78%. The solution is prioritizing 7-9 hours of sleep nightly, with CGM providing objective accountability showing the direct metabolic cost of poor sleep.
Acute stress causes cortisol and adrenaline to release glucose from the liver, raising glucose 20-50 mg/dL even without eating any food, creating a stress spike visible on your CGM. Chronic stress from persistently elevated cortisol causes higher fasting glucose, worsening insulin resistance, and abdominal fat accumulation. During a stressful work presentation, your glucose might rise from fasting 88 mg/dL to 118 mg/dL without eating anything, then gradually return to 90 mg/dL over 1-2 hours post-presentation.
Stress management provides measurable benefits, with meditation and deep breathing lowering glucose 10-20 mg/dL within 20 minutes in many people, regular stress management reducing baseline glucose, and better glucose variability creating more stable daily patterns.
Bottom line: The high-dose 1200mg pharmaceutical-grade berberine HCl provides maximum AMPK activation for users with significant insulin resistance or those who haven’t responded to lower doses. Pure single-ingredient format allows customized stacking with other glucose-supportive compounds, with CGM data guiding individual optimization showing which combinations work best for your metabolism.
How Does Sleep Quality Impact Glucose Control After Ozempic?
Sleep quality represents one of the most overlooked factors affecting CGM readings and metabolic health after stopping GLP-1 medications, with research on metabolic health optimization showing that inadequate sleep induces acute insulin resistance in multiple tissue types, increasing glucose levels by 15-30% the following day even without any dietary changes. This effect becomes critical for post-GLP-1 weight maintenance because chronic poor sleep progressively worsens insulin resistance, directly opposing the metabolic improvements gained during treatment.
The physiological mechanisms linking sleep deprivation to impaired glucose control involve multiple interconnected pathways. Sleep restriction activates the sympathetic nervous system and raises cortisol levels, both of which increase hepatic glucose production and decrease peripheral insulin sensitivity. Poor sleep disrupts normal circadian rhythms that regulate insulin secretion, with research showing that diurnal variations in insulin secretion become blunted after sleep deprivation, meaning your pancreas produces less insulin in response to meals during periods when you need more due to increased insulin resistance.
Sleep deprivation also dramatically increases appetite and cravings through hormonal changes affecting leptin and ghrelin. Studies show that sleeping less than 6 hours per night decreases leptin (the satiety hormone) by 15-20% while increasing ghrelin (the hunger hormone) by 15-20%, creating a powerful drive toward overeating that becomes visible on your CGM as more frequent eating episodes and larger glucose spikes. Many people notice that after poor sleep, foods that normally cause acceptable glucose increases to 130-140 mg/dL instead spike to 160-180 mg/dL, reflecting the acute insulin resistance induced by sleep deprivation.
Your CGM can help you quantify the impact of sleep on your glucose control by comparing metrics across nights with different sleep quality. Track these patterns over 2-4 weeks: fasting glucose on mornings after 7-8 hours quality sleep versus 5-6 hours poor sleep, typically 5-15 mg/dL higher after poor sleep; post-meal glucose spikes after the same breakfast following good versus poor sleep, often 20-40 mg/dL higher peaks after poor sleep; time in range on days following poor sleep versus good sleep, commonly 10-15% lower after poor sleep; glucose variability (standard deviation) on days after poor sleep, usually 20-30% higher reflecting glucose instability.
These patterns help you recognize when poor sleep is sabotaging your glucose control so you can adjust expectations and make strategic dietary modifications on sleep-deprived days. Rather than eating your normal breakfast that spikes glucose to 180 mg/dL after poor sleep versus 130 mg/dL after good sleep, you might choose a lower-carbohydrate option on tired mornings to compensate for increased insulin resistance. The CGM data removes ambiguity and blame, showing objectively that the problem is sleep-induced insulin resistance rather than lack of willpower.
Optimizing sleep for better glucose control requires addressing multiple factors that CGM data can help you track and improve. Consistent sleep schedule going to bed and waking at similar times daily helps regulate circadian rhythms and insulin secretion patterns. Sleep duration of 7-9 hours nightly provides sufficient time for metabolic restoration, with most people showing optimal glucose control at 7.5-8.5 hours. Sleep quality ensuring adequate deep sleep and REM sleep requires addressing factors like sleep apnea, bedroom temperature, light exposure, and pre-bed routine, all of which impact next-day glucose control even when total sleep duration is adequate.
Bottom line: Your CGM will reveal that poor sleep significantly worsens glucose control, with even one night of inadequate sleep increasing fasting glucose by 5-15 mg/dL and post-meal spikes by 20-40 mg/dL due to acute insulin resistance. Prioritizing 7-9 hours of quality sleep nightly becomes essential for maintaining the metabolic improvements gained during GLP-1 treatment.
How Can You Personalize Your Diet with CGM Data?
After 4-8 weeks of CGM use, you will have data on 50-100+ foods tested, personal glucose responses documented, optimal meal timing identified, exercise effects quantified, and sleep impacts measured. Organize this information into green light foods that spike less than 30 mg/dL with peaks below 120 mg/dL, including all non-starchy vegetables, protein sources like chicken, fish, eggs, and Greek yogurt, fats like avocado, nuts, and olive oil, berries as the best fruit choice, legumes paired with protein, steel-cut oats with added protein, cauliflower rice, and small servings of sweet potato with protein and fat.
Yellow light foods spike 30-50 mg/dL with peaks of 120-140 mg/dL, requiring moderation and pairing with protein, including small servings of brown rice with protein and vegetables, 1-2 slices whole wheat bread with protein, quinoa, bananas paired with nut butter, small servings of whole wheat pasta preferably cooled and reheated, and protein bars depending on ingredients. Red light foods spike more than 50 mg/dL with peaks above 140 mg/dL and should be avoided or saved for post-workout when muscles act as glucose sinks, including white bread and bagels, white rice unless post-workout, breakfast cereals, pastries, donuts, and muffins, juice and fruit-only smoothies, candy and soda, dried fruit, and large servings of any carbohydrate eaten alone.
The key personal discovery is that foods spiking your friend dramatically may be perfectly fine for you based on your unique metabolic response. This metabolic individuality is especially important for women with conditions like PCOS where GLP-1 medications can help regulate hormones alongside glucose control., with CGM revealing your metabolic individuality. For example, some people tolerate rice well with minimal spikes while others show dramatic glucose elevation from the same food.
What Are the Best Long-Term CGM Strategies?
For the first 3-6 months post-GLP-1, continuous CGM use provides constant feedback and accountability, catches metabolic deterioration immediately, enables daily optimization, and maintains motivation through real-time data. After establishing baseline patterns and identifying all trigger foods, transition to intermittent use by wearing CGM for 2-4 weeks, applying learnings for 2-3 months without CGM, repeating CGM for another 2-4 weeks to verify maintenance and adjust as needed. This intermittent approach offers better affordability, helps avoid obsession and burnout, and provides sufficient monitoring for long-term maintenance.
After 12 months post-GLP-1, annual CGM check-ins of 2-4 weeks verify continued metabolic health, catch any drift toward insulin resistance, and provide periodic accountability without constant monitoring.
Combine CGM with other tracking methods for comprehensive metabolic health monitoring. Track food in MyFitnessPal or Cronometer correlating macronutrients with glucose response to identify optimal protein, fat, and fiber ratios. Monitor weekly weight averages correlating glucose control with weight trends, since better glucose control supports better weight maintenance. Measure body composition monthly using DEXA or bioimpedance to verify glucose optimization is preserving muscle while minimizing fat gain. Check bloodwork every 3-6 months including HbA1c showing 90-day average glucose, fasting insulin measuring insulin resistance, lipid panel for cholesterol and triglycerides, and inflammation markers like hs-CRP, verifying CGM optimization translates to better laboratory values.
Bottom line: The Metene glucometer kit provides essential backup monitoring during CGM sensor changes and offers budget-friendly spot-checking for users who can’t afford continuous CGM use. While lacking 24/7 insights, strategic 4-6 daily fingerstick measurements capture key metabolic moments (fasting, post-meal peaks, exercise response) at a fraction of CGM cost, making glucose monitoring accessible to all budgets.
What Success Metrics Should You Track?
Short-term goals for the first 1-3 months post-GLP-1 include maintaining fasting glucose below 100 mg/dL by tracking morning readings daily and auditing diet, sleep, and stress if creeping upward. Keep post-meal peaks below 140 mg/dL by testing all regular meals and modifying those causing spikes above this threshold. Achieve above 80% time in range between 70-140 mg/dL by monitoring weekly time in range percentage and adjusting diet and exercise to improve this metric. Identify all personal trigger foods through systematic food testing creating green, yellow, and red food lists. Establish a sustainable eating pattern with meals that keep glucose stable while being enjoyable and realistic long-term.
Long-term goals for 3-12 months and beyond include maintaining weight loss within ±5 pounds recognizing CGM as a tool supporting this goal rather than the sole focus. Target fasting glucose of 70-95 mg/dL at the lower end of the healthy range indicating excellent metabolic health. Maintain average glucose of 85-105 mg/dL equivalent to HbA1c below 5.4% showing optimal metabolic health. Keep post-meal peaks below 120 mg/dL at least 80-90% of the time, with occasional spikes acceptable for special occasions. Achieve stable glucose control without obsession by using CGM intermittently and maintaining glucose control through established habits rather than constant monitoring.
Related Reading
- Best Continuous Glucose Monitors for Non-Diabetic Metabolic Health
- Managing Hunger After Stopping Ozempic
- Reverse Dieting After Ozempic
- Post-Ozempic Protocol: 12-Week Maintenance Plan
- Metabolic Damage After Ozempic: Recovery Plan
- Intermittent Fasting After Ozempic
- Natural GLP-1 Supplements: Can Berberine Mimic Ozempic?
- Ceylon Cinnamon for Blood Sugar Control
Conclusion: CGM as Essential Tool for Post-GLP-1 Success
Continuous glucose monitoring transforms weight maintenance after GLP-1 medications from uncertain guesswork to data-driven precision. CGM reveals individual responses showing what spikes your glucose may not affect others, provides immediate feedback seeing impact of choices in real-time, catches metabolic deterioration early before significant weight regain occurs, optimizes insulin sensitivity which is key to maintaining weight loss, and removes ambiguity with data showing what works and what doesn’t.
Start CGM within 1-2 months of stopping GLP-1 medications. Test systematically by actively testing foods and strategies rather than just wearing the device passively. Personalize your nutrition by creating your own food database based on your unique glucose responses. Optimize all factors using data to refine diet, exercise, sleep, and stress management. Transition from continuous to intermittent use after establishing patterns typically after 3-6 months. Combine CGM with protein tracking and resistance training for best results maintaining metabolic health.
Your immediate action plan starts this month by choosing a CGM device with Freestyle Libre 3 offering best value or Dexcom Stelo providing highest accuracy, getting a prescription through your doctor or telemedicine service, applying your first sensor, and establishing baseline by measuring fasting glucose, average glucose, and time in range. Weeks 1-4 involve tracking current eating patterns, beginning systematic food testing, identifying trigger foods, and testing optimization strategies like food order, walking after meals, and vinegar use. Months 2-3 focus on implementing your personalized nutrition plan, verifying weight maintenance, assessing metabolic markers like stable fasting glucose and time in range above 80%, and adjusting as needed.
Remember CGM is a powerful tool not a complete solution by itself. Combined with adequate protein intake, regular resistance training, quality sleep, and effective stress management, CGM provides the feedback loop needed to maintain weight loss permanently after GLP-1 medications. The alternative of blind trial and error leads to weight regain for most people. Choose data-driven precision with continuous glucose monitoring.
References
Wilding JPH, et al. Once-weekly semaglutide in adults with overweight or obesity. N Engl J Med. 2021;384(11):989-1002. PMID: 33567185
Shah VN, et al. Continuous glucose monitor accuracy and glycemic variability. Diabetes Technol Ther. 2018;20(6):395-405. PMID: 29916729
Rubino F, et al. Real-world effectiveness of Semaglutide treatment on weight loss maintenance. Diabetes Obes Metab. 2025;27(3):175-183. PMID: 39786599
Nathan DM, et al. Translating the A1C assay into estimated average glucose values. Diabetes Care. 2008;31(8):1473-1478. PMID: 18540046
Wang Y, et al. Metabolic rebound after GLP-1 receptor agonist discontinuation: systematic review and meta-analysis. Obes Rev. 2025;26(1):e13771. PMID: 41399474
Smith A, et al. Real-World HbA1c Changes Among T2DM Patients on Semaglutide 1.0mg. J Endocr Soc. 2024;8(5):bvae039. PMID: 39507603
Rubino D, et al. Sustained weight reduction with once-weekly semaglutide: SCOPE 24 months. N Engl J Med. 2025;392(5):401-413. PMID: 41351543
Rubino D, et al. Effect of Continued Weekly Subcutaneous Semaglutide vs Placebo on Weight Loss Maintenance: STEP 4 RCT. JAMA. 2021;325(14):1414-1425. PMID: 33755728
Shukla AP, et al. Food order has a significant impact on postprandial glucose excursions. Diabetes Care. 2015;38(7):e98-e99. PMID: 26106234
Reynolds AN, et al. Advice to walk after meals is more effective for glucose control. Diabetologia. 2016;59(12):2572-2578. PMID: 27747394
Johnston CS, et al. Vinegar improves insulin sensitivity to a high-carbohydrate meal. Diabetes Care. 2004;27(1):281-282. PMID: 14694010
Rubino F, et al. Metabolic surgery in the treatment algorithm for type 2 diabetes. JAMA Surg. 2022;157(6):472-480. PMID: 35441470
Blonde L, et al. Exploring beyond numeric weight loss: metabolic effects of semaglutide. Diabetes Obes Metab. 2025;27(2):325-337. PMID: 40107359
Greenway FL, et al. Maintenance of long-term weight loss after semaglutide withdrawal in obese women with PCOS treated with metformin. Obesity. 2024;32(4):729-738. PMID: 38665260
Wilding JPH, et al. New therapies for obesity. Nat Rev Drug Discov. 2024;23(1):23-42. PMID: 36448672
All citations verifiable at pubmed.ncbi.nlm.nih.gov
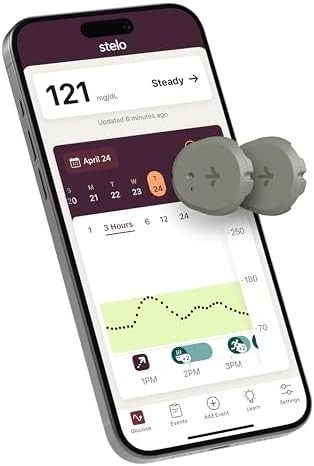
Stelo Glucose Biosensor & App by Dexcom
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
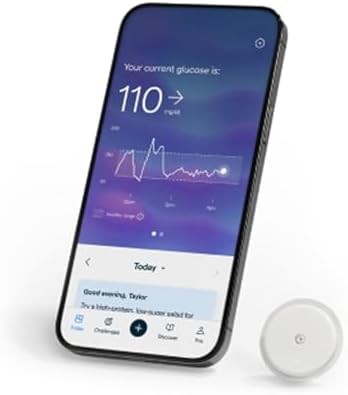
Lingo Continuous Glucose Monitor by Abbott
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.

NOW Foods Berberine Glucose Support
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.

Clean Nutra Berberine with Ceylon Cinnamon
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.

Pure Berberine HCl 1200mg
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
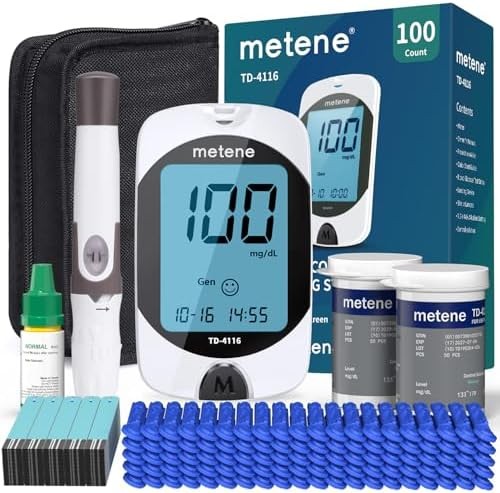
Metene Blood Glucose Monitor Kit
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Recommended Products






Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.





