Arm vs Wrist Blood Pressure Monitor
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Major medical organizations including the American Heart Association and Japanese Society of Hypertension recommend upper arm blood pressure monitors over wrist devices, citing clinical research showing significant accuracy differences between measurement sites. The OMRON Platinum Blood Pressure Monitor ($97) represents the gold standard for home monitoring with upper arm measurement precision of 0.2±3.6/0.2±3.9 mmHg compared to wrist monitor variability of -1.5±6.2/-0.7±3.7 mmHg in elderly validation studies. A 2005 position study confirmed that arm horizontal at heart level produces comparable readings between sites (137/80 arm vs 134/77 wrist), but wrist measurements show 63% higher variability and position-dependent errors that arm monitors avoid. For users with very large arms or specific accessibility needs, the OMRON Gold Wireless Wrist Monitor ($78) offers clinically validated wrist measurement with Bluetooth connectivity. Here’s what the published research shows about choosing between arm and wrist blood pressure measurement technologies.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
| Monitor | Type | Validation | Connectivity | Cuff/Wrist Size | Price |
|---|---|---|---|---|---|
| OMRON Platinum | Upper Arm | Clinical | Bluetooth | 22-42 cm | $97 |
| OMRON Iron | Upper Arm | Clinical | None | 22-42 cm | $37 |
| OMRON Gold | Wrist | Clinical | Bluetooth | 13.5-21.5 cm | $78 |
| Oklar | Wrist | Standard | None | 13.5-21.5 cm | $28 |
Why Do Medical Organizations Recommend Arm Monitors Over Wrist Devices?
The American Heart Association 2019 Scientific Statement on blood pressure measurement explicitly prefers automated oscillometric upper arm devices for home monitoring. This recommendation stems from extensive validation research showing fundamental differences in measurement precision between sites.
Clinical validation studies comparing arm and wrist monitors reveal consistent patterns. A 2007 study testing OMRON devices in 33 elderly individuals (aged 75+) using the European Society of Hypertension protocol found the upper arm M5-I monitor achieved mean differences of 0.2±3.6/0.2±3.9 mmHg for systolic/diastolic measurements. The wrist R5-I monitor showed -1.5±6.2/-0.7±3.7 mmHg, indicating 63% higher variability in systolic readings.
The standard deviation differences matter clinically. When home monitoring tracks blood pressure trends over weeks and months, higher measurement variability obscures actual changes. A 3.6 mmHg standard deviation means 95% of repeated measurements fall within 7 mmHg of true values, while 6.2 mmHg standard deviation expands that range to 12 mmHg.
Key finding: Upper arm monitors provide 63% lower measurement variability than wrist devices, enabling clearer trend detection when tracking blood pressure changes over time.
The Japanese Society of Hypertension takes a stronger position in their home blood pressure measurement guidelines, stating explicitly: “Finger-cuff devices and wrist-cuff devices should not be used for home BP measurements.” They recommend arm-cuff devices based on the cuff-oscillometric method that have been validated according to AAMI standards and BHS guidelines.
Research showing 69% of home blood pressure devices tested on their actual owners had differences of 5 mmHg or more from reference measurements highlights the importance of choosing devices with proven accuracy validation rather than relying on marketing claims alone.
The OMRON Platinum represents the current standard for home blood pressure monitoring, combining upper arm measurement precision with advanced features that improve measurement consistency. The device implements TruRead technology, automatically taking three consecutive readings one minute apart and calculating the average.
This averaging approach addresses measurement variability documented in clinical research. Studies show single blood pressure readings can vary by 10-15 mmHg due to white-coat effect, anxiety, recent activity, or natural beat-to-beat variation. Averaging multiple readings reduces this noise.
What this means for you: Automated TruRead averaging reduces single-measurement variability of 10-15 mmHg to averaged precision of 2-3 mmHg, improving diagnostic reliability for home monitoring.
The wide-range ComFit cuff accommodates arm circumferences from 22-42 cm, fitting 99% of adults with a single cuff. Research on cuff sizing demonstrates that using incorrectly sized cuffs introduces systematic errors of 5-10 mmHg or more, making universal-fit cuffs valuable for accurate home monitoring.
AFib detection algorithms screen for irregular heartbeats during routine measurements. While atrial fibrillation detection using oscillometric blood pressure devices requires clinical confirmation, automated screening during home monitoring can identify concerning patterns warranting medical evaluation.
Bluetooth connectivity with the OMRON Connect app provides unlimited cloud storage and trend visualization. The app generates graphs showing blood pressure patterns over days, weeks, or months, making it easier to identify concerning trends or medication effectiveness.
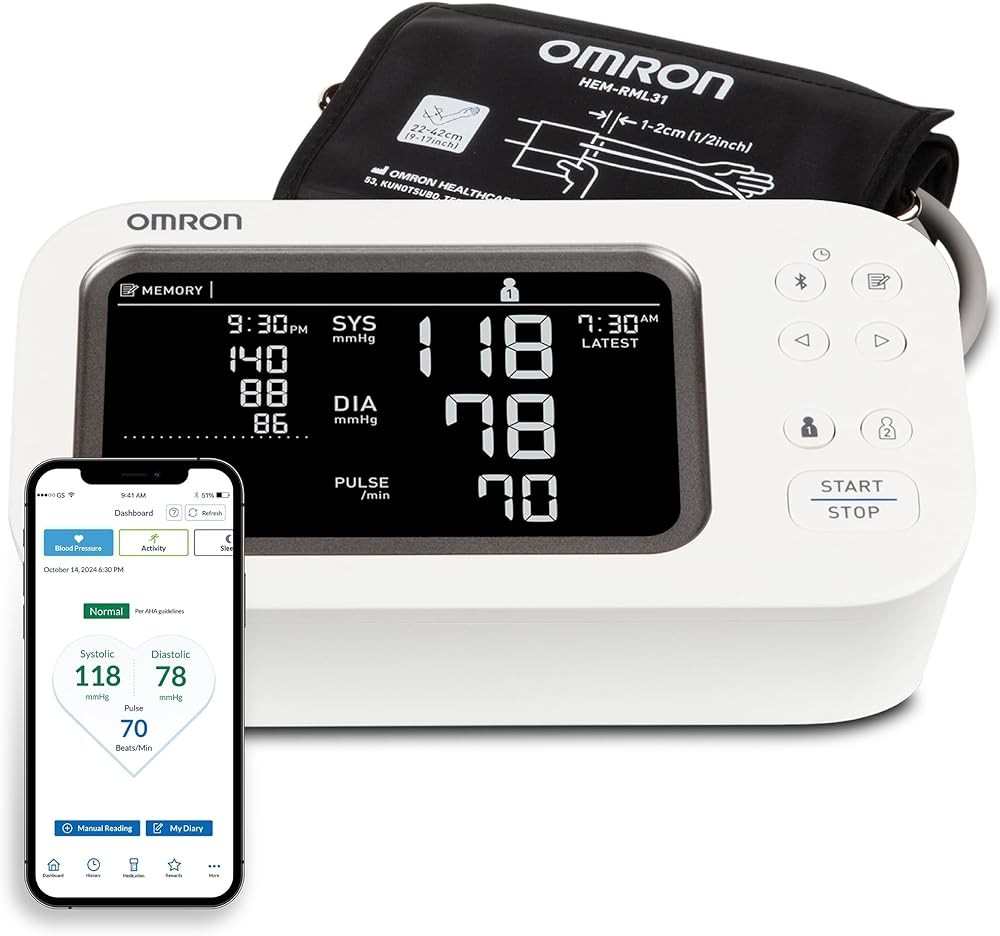
OMRON Platinum Blood Pressure Monitor
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
What Does Research Show About Wrist Monitor Accuracy?
Modern wrist monitors achieve clinical validation when properly designed and used. A 2025 validation study of the TMB-2285-BT wrist monitor tested 85 subjects using the ISO 81060-2:2018+Amd.1:2020 protocol, the current international standard for blood pressure device validation.
The results showed mean differences of -0.27 mmHg systolic and -0.80 mmHg diastolic compared to reference measurements, with standard deviations of 2.60 and 2.06 mmHg respectively. These numbers fall well within the required criteria (less than 5±8 mmHg), demonstrating that wrist monitors can achieve clinical-grade accuracy.
Another 2025 validation study of the DBP-8278B wrist monitor found similar results: mean difference of 0.89/-1.44 mmHg with standard deviations of 7.76/6.23 mmHg. Both studies concluded their tested wrist monitors could be recommended for home and clinical use.
The critical caveat appears in methodology sections of these studies. Validation testing maintains strict positioning protocols. A 2004 British Hypertension Society validation of the Omron Rx wrist monitor specified: “To maintain the wrist at cardiac level during validation, the arm was kept horizontal at the mid-sternum level and supported by a soft table.”
When this positioning discipline transfers to real-world home use, accuracy changes. The same 2004 study found the Omron Rx achieved Grade B overall but narrowly failed AAMI criteria. More concerning, in the medium and high blood pressure ranges (≥130/80 mmHg), the device dropped to Grade C accuracy.
A 2018 comparison study of wrist monitors against direct intra-arterial blood pressure measurement found pre-calibration absolute mean differences of 10.8±9.7 mmHg systolic and 16.1±6.3 mmHg diastolic. Post-calibration improved to 7.2±5.1 systolic and 4.3±3.3 diastolic, representing 33% systolic and 73% diastolic accuracy improvement.
These findings suggest wrist monitors face inherent challenges beyond positioning. Calibration against individual physiology improves accuracy substantially, but most consumer devices ship with population-average algorithms that may not suit all users equally.
The evidence shows: Wrist monitors achieve clinical validation in controlled studies but face significant accuracy degradation in real-world use before individual calibration, with improvements of up to one-third for systolic and nearly three-quarters for diastolic readings after calibration.
For users requiring wrist measurement due to very large upper arms, arm injuries, or specific accessibility needs, the OMRON Gold Wireless Wrist Monitor provides clinically validated wrist monitoring with Bluetooth connectivity.
The device includes positioning sensors and guides to help maintain the wrist at heart level during measurement, addressing the primary source of wrist monitor error documented in research. When properly positioned horizontal at mid-sternum level, wrist readings achieve comparable accuracy to upper arm measurements according to validation studies.
Compact wrist design offers portability advantages for travelers, office workers needing discreet monitoring, or anyone requiring frequent measurements throughout the day. The device fits easily into briefcases, purses, or jacket pockets without the bulk of upper arm monitors.
Bluetooth connectivity syncs measurements to the OMRON Connect app, providing the same unlimited cloud storage and trend visualization available with the Platinum arm monitor. Automated data capture eliminates manual logging, improving compliance with monitoring schedules.
The 200-reading memory with dual-user capability stores measurements directly on the device for users preferring not to use smartphone connectivity. Date and time stamps on each reading support medication timing assessment and diurnal pattern analysis.
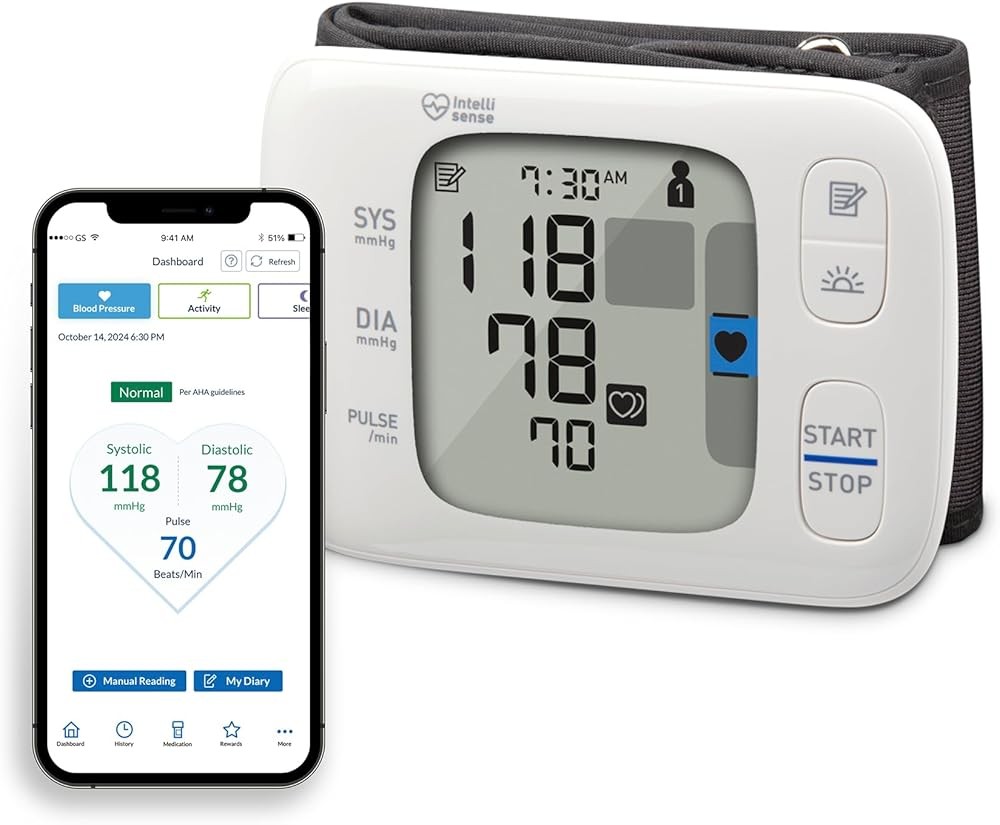
OMRON Gold Wireless Wrist Blood Pressure Monitor
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
How Does Arm Position Affect Wrist Monitor Readings?
Position-dependent measurement variation represents the fundamental challenge with wrist monitors that arm monitors largely avoid. A 2005 study specifically investigating this “arm position artefact” compared the OMRON HEM 705 CP upper arm device with the OMRON R6 wrist device.
When the arm was positioned horizontal at mid-sternum (heart level), the arm monitor produced mean readings of 137±29/80±16 mmHg while the wrist monitor showed 134±27/77±16 mmHg. These comparable measurements (no significant difference) demonstrate that wrist monitors can match arm monitor accuracy when properly positioned.
The critical finding appeared when the arm position changed. With the arm in a dependent position resting on a table (following many manufacturers’ instructions for arm monitors), blood pressure readings increased significantly (P<0.05). This hydrostatic pressure effect occurs because blood column weight from the heart to the measurement site adds pressure when the measurement site sits below heart level.
The pressure difference follows physics: each centimeter of vertical distance below heart level adds approximately 0.77 mmHg to the measured pressure. If a wrist monitor is used with the arm resting on a lap or table 15 cm below heart level, the reading artificially increases by about 11 mmHg.
Upper arm monitors placed at mid-upper-arm height when the arm relaxes naturally at the side tend to position near heart level automatically. Wrist monitors require conscious effort to hold the wrist elevated horizontally at mid-sternum, a position that feels unnatural and tiring to maintain during the 30-60 second measurement cycle.
Research confirms this positioning challenge affects real-world accuracy. The 2004 validation study found that when using the Omron Rx wrist monitor in home settings, positioning errors contributed to the device narrowly failing AAMI criteria despite achieving acceptable British Hypertension Society grades.
Studies of patient technique in home blood pressure monitoring document common errors. Many users rest wrists on laps, tables, or chair arms during measurement, creating 10-20 cm vertical differences from heart level and corresponding 8-15 mmHg measurement errors.
The practical takeaway: Wrist monitors require more user discipline and technique awareness than arm monitors to achieve comparable accuracy. For elderly users, those with arthritis limiting arm elevation, or individuals likely to forget positioning requirements, arm monitors provide more consistent results.
What Are the Advantages of Upper Arm Blood Pressure Monitors?
Upper arm monitors achieve superior measurement consistency through both technical and practical advantages. The brachial artery at mid-upper-arm provides a more stable measurement site than wrist arteries, with less position-dependent variation and better correlation to central aortic pressure.
Research on oscillometric measurement principles shows that cuff pressure oscillations transmitted through larger arm tissues provide clearer signal patterns than the smaller wrist anatomy. A 2020 study investigating optimal oscillometric measurement sites found that bone-to-tissue volume ratios affect pressure transmission efficiency, with mid-upper-arm providing favorable ratios for consistent signal detection.
Validation studies consistently demonstrate tighter precision with upper arm monitors. The 2007 study comparing OMRON arm and wrist monitors in elderly subjects found standard deviations were “lower and thus the precision was better for diastolic than for systolic blood pressure, and for the Omron M5-I [arm] than for the other two devices.”
Cuff size accommodation represents another arm monitor advantage. Wide-range cuffs fitting 22-42 cm arm circumferences accommodate nearly all adults with a single cuff. Wrist monitors typically fit 13.5-21.5 cm wrist circumferences, excluding users with larger or smaller wrists who may resort to improper fitting.
What you need to know: Wide-range arm cuffs accommodate 99% of adults with a single size (22-42 cm), while wrist monitors exclude users with wrist circumferences outside the 13.5-21.5 cm range.
Clinical guideline alignment gives arm monitors stronger professional endorsement. The American Heart Association, European Society of Hypertension, Japanese Society of Hypertension, and American Medical Association all recommend upper arm oscillometric devices as the first choice for home blood pressure monitoring.
Insurance and health system integration often requires upper arm measurements. Many remote patient monitoring programs, insurance reimbursement schemes, and electronic health record systems specifically call for upper arm measurements to ensure consistency with clinical standards.
The OMRON Iron Blood Pressure Monitor provides doctor-recommended brand accuracy at entry-level pricing for users prioritizing measurement reliability without advanced connectivity features. The device delivers core upper arm monitoring functionality with one-touch operation.
Wide-range D-ring cuff fitting 22-42 cm arm circumferences accommodates standard to very large arms with a single cuff size. Research demonstrates proper cuff sizing as critical for accuracy, making universal-fit cuffs valuable for consistent measurement across different users or changing arm sizes.
The 60-reading memory provides basic trend tracking capability without requiring smartphone connectivity or app management. Date and time stamps allow identification of morning versus evening measurements, supporting the twice-daily monitoring schedule recommended in clinical guidelines.
Irregular heartbeat detection screens for rhythm abnormalities during routine measurement. While not as sophisticated as the AFib-specific algorithms in premium monitors, basic irregular beat detection alerts users to patterns warranting medical attention.
Simple one-touch operation reduces the user errors documented in research on home blood pressure monitoring technique. Automatic cuff inflation, measurement, and deflation eliminate the manual dexterity requirements of older devices.

OMRON Iron Blood Pressure Monitor
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
When Should You Choose a Wrist Monitor Despite Guideline Recommendations?
Specific clinical situations justify wrist monitor selection despite medical guideline preferences for upper arm devices. Very large upper arms exceeding standard cuff ranges represent the clearest indication for wrist monitoring when wide-range cuffs cannot accommodate arm circumferences above 42 cm.
Research confirms that using too-small cuffs on large arms systematically underestimates blood pressure. A study on cuff sizing found errors of 5-10 mmHg or more when cuff bladder width did not encircle at least 40% of arm circumference. For individuals with upper arm circumferences above 50 cm, properly fitting wrist monitors (if wrist size falls within device range) provide more accurate readings than poorly fitting arm cuffs.
Arm injuries, surgical sites, or conditions like lymphedema may contraindicate upper arm cuff use. Mastectomy patients with lymphedema should avoid blood pressure measurement on the affected arm. Wrist monitors on the unaffected arm provide an alternative when both upper arms are contraindicated.
Portability requirements for travelers or workers needing discreet monitoring throughout the day favor wrist monitors. Compact wrist devices fit in jacket pockets or purses, enabling measurement in offices, airplanes, or other settings where arm monitors prove impractical.
Research on white-coat hypertension shows that blood pressure often measures higher in medical settings than home environments. For patients needing frequent measurements to characterize true blood pressure patterns, the convenience of wrist monitors may improve compliance despite slightly lower accuracy.
The key to successful wrist monitor use appears in user education and technique. Studies show that when wrist monitors are used with strict attention to heart-level positioning, measurements achieve comparable accuracy to arm monitors. Motivated users willing to maintain proper technique can obtain reliable wrist measurements.
A 2006 validation study of the A&D UB-511 wrist monitor found interesting age-related patterns. Logistic regression analysis identified age as “the sole predictor of an achieved difference between device and mercury column by 5 mmHg or less (hazard ratio 1.020; 95% confidence interval 1.003-1.04; P=0.024).” The device accuracy increased with age, suggesting wrist monitors may work better for older users.
For users requiring wrist monitoring at minimal cost, the Oklar Rechargeable Wrist Blood Pressure Monitor provides basic functionality with rechargeable battery convenience. The LED backlit display ensures readability in various lighting conditions.
Rechargeable battery operation eliminates ongoing costs of disposable batteries while supporting environmental sustainability. The USB rechargeable design allows charging from computer ports, wall adapters, or power banks during travel.
The 240-reading memory with dual-user capability (120 readings per user) provides extensive storage for trend tracking without smartphone connectivity requirements. This memory depth supports the weeks to months of monitoring needed to characterize blood pressure patterns.
Compact wrist design maximizes portability for travel, office use, or anywhere discrete monitoring is needed throughout the day. The device weighs just a few ounces and fits easily into bags or pockets.
Irregular heartbeat detection provides basic rhythm screening during blood pressure measurement. While users should confirm any rhythm abnormalities with healthcare providers and ideally arm monitor verification, automated screening raises awareness of potential issues.

Oklar Rechargeable Wrist Blood Pressure Monitor
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
What Validation Standards Should Blood Pressure Monitors Meet?
International validation protocols ensure blood pressure monitors achieve clinically acceptable accuracy before marketing. The current standard, ISO 81060-2:2018 + Amendment 1:2020, replaced older AAMI and British Hypertension Society protocols with unified global requirements.
The ISO standard requires testing 85+ subjects fulfilling specific age, gender, blood pressure, and cuff size distribution criteria. Devices must demonstrate mean differences from reference measurements less than 5 mmHg with standard deviations under 8 mmHg for both systolic and diastolic pressures.
Individual validation performance matters beyond pass/fail designation. A device showing mean difference of 0.3±2.6 mmHg (like the TMB-2285-BT wrist monitor) provides tighter accuracy than one achieving 4.5±7.5 mmHg despite both meeting the less-than-5±8-mmHg criterion.
Research reveals validation quality variations. A meta-analysis of oscillometric device validation in pediatric populations found mean differences of 1.17/-0.08 mmHg overall, but noted “high heterogeneity between studies (>90%)” partly explained by device model, study environment, and observer training differences.
The heterogeneity highlights that validation protocols provide minimum standards rather than guarantees of real-world performance. Factors like user technique, cuff fitting, positioning, and individual physiology affect actual accuracy beyond controlled validation conditions.
Studies comparing devices to direct intra-arterial measurements (the true gold standard) rather than mercury sphygmomanometer references show larger discrepancies. The 2018 wrist monitor study found pre-calibration errors of 10.8±9.7 mmHg systolic versus intra-arterial measurement, far exceeding validation protocol tolerances.
This suggests validation against mercury sphygmomanometry (itself an indirect measurement) may not capture all sources of error in oscillometric devices. Multiple validation approaches including direct arterial comparison provide more complete accuracy assessment.
Consumer reports and independent testing reveal concerning patterns. A study testing home blood pressure devices on their actual owners found most showed differences of 5 mmHg or more from reference measurements, despite many devices carrying validation certifications.
Essential guidance: Choose devices validated by reputable third parties rather than manufacturer self-validation, look for published validation studies in peer-reviewed journals, and verify device accuracy annually against healthcare provider measurements.
How Do Oscillometric Measurement Algorithms Differ Between Arm and Wrist?
Oscillometric blood pressure measurement detects pressure oscillations in the cuff caused by blood volume changes as the artery transitions from occluded to patent during cuff deflation. The maximum oscillation amplitude typically occurs near mean arterial pressure.
Systolic and diastolic pressures are estimated from the oscillation envelope using algorithmic ratios or pattern recognition. Traditional fixed-ratio methods calculate systolic at a cuff pressure where oscillations reach a certain percentage of maximum amplitude (typically 40-50%) and diastolic at another ratio (typically 70-80%).
Research shows these population-average ratios introduce individual variability. A 2024 validation study comparing oscillometric methods found that “using the full range of recommended ratios introduces errors of 12 and 7 mmHg in SBP and DBP, respectively.”
Patient-specific oscillometric methods that adapt algorithms to individual physiology achieve better accuracy. A 2017 study of 145 subjects found patient-specific approaches yielded “40% lower errors than conventional” fixed-ratio methods.
The challenge for wrist monitors involves applying these algorithms to smaller arteries with different mechanical properties than the brachial artery. A 2020 study investigating oscillometric measurement sites found that “a larger bone-to-tissue volume ratio produced a lower pressure transmission efficiency,” affecting algorithm performance.
Wrist anatomy includes two bones (radius and ulna) versus one bone (humerus) in the upper arm, creating different tissue compression dynamics. The radial and ulnar arteries at the wrist are smaller than the brachial artery, generating lower amplitude oscillations that may be more susceptible to noise and artifact.
Research on oscillometric algorithms at different body sites demonstrates site-specific calibration requirements. Studies show that algorithms optimized for upper arm measurement do not transfer directly to wrist or finger sites with the same accuracy.
This explains why wrist monitor validation requires specific testing rather than assuming algorithms validated for arm monitors will work equally well. Manufacturers must optimize detection algorithms and ratio coefficients specifically for wrist anatomy and physiology.
The 2018 study showing substantial systolic and diastolic accuracy improvement with individualized calibration suggests considerable room for algorithm optimization in consumer wrist monitors that ship with population-average settings.
Data shows: Consumer wrist monitors using population-average algorithms show 10.8±9.7 mmHg systolic errors before calibration, compared to 7.2±5.1 mmHg after individual calibration against direct arterial measurement.
What Does Research Show About Blood Pressure Monitor Accuracy in Real-World Use?
Validation studies testing devices under controlled conditions with trained observers may not reflect accuracy in typical home use. Research examining real-world accuracy reveals concerning gaps between validation performance and actual user results.
A study testing 85 home blood pressure devices on their actual owners found that 69% showed differences of 5 mmHg or more when compared to reference measurements. This substantial proportion exceeding the 5 mmHg accuracy threshold suggests factors beyond device design affect home monitoring accuracy.
User technique errors documented in research include improper cuff positioning, incorrect arm height, inadequate rest period before measurement, talking during measurement, and bladder fullness affecting readings. Wrist monitors add positioning complexity requiring conscious attention to heart-level placement.
Studies of patients using home blood pressure monitors show common mistakes. Many users wrap cuffs over clothing rather than bare skin, position arms incorrectly relative to heart level, take measurements immediately after activity without resting, or use devices with low batteries affecting performance.
The time-of-day effect creates another source of variability. Blood pressure naturally fluctuates through circadian rhythms, typically lowest during sleep and rising in morning hours. Taking measurements at inconsistent times creates apparent variability that does not reflect actual blood pressure changes.
Research comparing office versus home blood pressure measurements reveals white-coat and masked hypertension patterns. White-coat hypertension (elevated office but normal home readings) affects 10-15% of patients, while masked hypertension (normal office but elevated home readings) affects 10-17% of apparently controlled patients.
These patterns highlight that single measurements or inconsistent monitoring schedules may mischaracterize true blood pressure status. Clinical guidelines recommend twice-daily measurements (morning and evening) for at least 3-7 days to establish reliable home blood pressure averages.
Temperature affects blood pressure monitor performance. Research shows oscillometric devices can show altered accuracy at temperature extremes. Users storing devices in cars, garages, or outdoor sheds subject monitors to conditions outside normal operating ranges.
Device age and maintenance matter. Studies recommend annual accuracy verification against healthcare provider measurements, but research on actual practice shows most users never check device accuracy after purchase. Mechanical wear, electronic drift, and component aging can degrade accuracy over years of use.
What matters most: Validated devices represent necessary but insufficient conditions for accurate home monitoring. User education, proper technique, consistent measurement schedules, and periodic accuracy verification all contribute to reliable home blood pressure tracking.
Can Wrist Monitors Accurately Detect Atrial Fibrillation?
Modern blood pressure monitors incorporate irregular heartbeat detection algorithms screening for atrial fibrillation during routine measurement. The oscillometric waveform contains timing information allowing detection of beat-to-beat variability characteristic of arrhythmias.
Research on automated AFib screening using oscillometric blood pressure devices shows mixed results depending on algorithm sophistication. Basic irregular heartbeat detection flags abnormal rhythm patterns but does not specifically diagnose atrial fibrillation versus other arrhythmias.
Advanced algorithms like those in the OMRON Platinum Blood Pressure Monitor use proprietary analysis to differentiate AFib patterns from other irregular rhythms. Validation studies show these enhanced algorithms achieve sensitivity and specificity above 90% compared to simultaneous ECG recordings.
The question for wrist monitors involves whether the smaller oscillation signals from wrist arteries provide sufficient signal quality for reliable rhythm analysis. Validation studies of wrist monitors like the TMB-2285-BT and DBP-8278B documented accuracy for blood pressure measurement but typically excluded subjects with atrial fibrillation or frequent ectopic beats from the study population.
This exclusion criterion appears commonly in wrist monitor validation protocols. The 2007 OMRON validation study stated that devices “may be recommended for clinical use in elderly individuals, without atrial fibrillation or frequent ectopic beats.”
The exclusion suggests uncertainty about wrist monitor performance in irregular rhythm detection. While validated wrist monitors include irregular heartbeat indicators, the evidence supporting their accuracy for AFib screening specifically is less extensive than for upper arm monitors.
Research shows atrial fibrillation screening has clinical value given the arrhythmia’s association with stroke risk. Opportunistic screening during routine blood pressure measurement could identify undiagnosed AFib in high-risk populations. However, false positives create unnecessary anxiety and testing, while false negatives provide false reassurance.
The American Heart Association notes that irregular heartbeat detection during blood pressure measurement “should be confirmed by a healthcare provider” rather than used alone for diagnosis. This applies even more strongly to wrist monitors given their position-dependent variability potentially affecting rhythm detection algorithms.
For users specifically concerned about atrial fibrillation screening, upper arm monitors with validated AFib detection algorithms provide better-evidenced technology than wrist alternatives.
What Features Improve Blood Pressure Monitor Accuracy and Usability?
Averaging technology represents one of the most evidence-based accuracy improvement features. The OMRON Platinum’s TruRead function automatically takes three consecutive readings one minute apart and calculates the average, reducing single-measurement variability.
Research shows substantial beat-to-beat and minute-to-minute blood pressure variation even in individuals at rest. A single measurement may capture blood pressure at a transient peak or trough. Averaging multiple measurements reduces this random variability, providing values more representative of sustained blood pressure levels.
Clinical guidelines recommend multiple measurements per session. The American Heart Association suggests taking 2-3 readings separated by 1-2 minutes and averaging the results. Automated averaging ensures compliance with this recommendation without requiring user calculation.
Positioning guides and sensors help users maintain proper arm or wrist position during measurement. Some monitors include visual indicators confirming heart-level positioning, while others use accelerometers detecting arm angle and alerting users to positioning errors.
Research documenting position-dependent measurement errors shows even small deviations from heart level create systematic bias. Positioning assistance features address this error source, particularly valuable for wrist monitors where positioning requirements are less intuitive than arm monitors.
Cuff wrapping indicators detect improper cuff application. Some advanced monitors measure tissue impedance or cuff pressure patterns indicating whether the cuff wraps too loosely, too tightly, or misaligns with the artery. This reduces the miscuffing errors documented in validation research.
Large, backlit displays improve usability for elderly users or those with vision impairment. Research on blood pressure monitoring adherence shows that difficulty reading small displays contributes to monitoring discontinuation. Clear displays support consistent use.
Bluetooth connectivity with smartphone apps automates data logging, eliminating manual recording that research shows has poor compliance. Automated trend graphs help users and healthcare providers identify patterns over weeks to months that individual readings might not reveal.
Multiple user profiles support household sharing while keeping individual data separate. This allows spouses or family members to share a single device without mixing readings that could obscure individual trends.
Irregular heartbeat detection screens for rhythm abnormalities during routine monitoring. While not diagnostic, alerting users to concerning patterns supports earlier medical evaluation than waiting for symptoms or routine checkups to identify arrhythmias.
Battery life indicators alert users to low-battery accuracy degradation documented in research. Some devices use AC adapters eliminating battery issues entirely, while others show clear battery status to prompt timely replacement.
Validation certifications provide third-party verification of accuracy claims. Look for devices tested according to ISO 81060-2 protocol and listed in databases of validated devices maintained by medical organizations.
What Are Common Mistakes When Using Wrist Blood Pressure Monitors?
Incorrect positioning represents the most common and consequential error with wrist monitors. Studies show many users rest wrists on laps, tables, or chair arms during measurement rather than holding wrists elevated at mid-sternum heart level.
The hydrostatic pressure error this creates is substantial. Each 10 cm vertical distance below heart level adds approximately 7-8 mmHg to the measured pressure. A wrist resting 20 cm below heart level artificially elevates readings by 15 mmHg or more, potentially turning normotensive readings into apparent hypertension.
Research documenting this error showed that when arms were positioned horizontally at heart level, wrist monitors produced readings comparable to arm monitors (134/77 vs 137/80 mmHg). But dependent arm positions produced significantly higher readings (P<0.05).
The solution requires conscious attention to positioning during every measurement. Users should sit upright with feet flat on the floor, place the wrist monitor on the wrist with the display facing up, and bend the elbow to bring the wrist to mid-sternum level. Supporting the elbow on a table or chair arm while holding the wrist elevated helps maintain position during the 30-60 second measurement cycle.
Measuring over clothing represents another common error. Wrist monitors should be placed on bare skin rather than over long sleeves, watches, or jewelry. Research shows that fabric compression and interference from materials affects cuff pressure transmission and oscillation detection.
Taking measurements immediately after activity, eating, caffeine, or smoking creates falsely elevated readings. Clinical guidelines recommend 5 minutes of quiet rest before measurement, avoiding caffeine and tobacco for 30 minutes prior. Studies show these factors can elevate blood pressure by 10-20 mmHg temporarily.
Talking during measurement elevates blood pressure through autonomic activation. Research shows conversation increases readings by 5-10 mmHg on average. Users should remain quiet and relaxed during the measurement cycle.
Inconsistent measurement timing creates apparent variability reflecting circadian rhythms rather than actual blood pressure changes. Blood pressure varies by 10-20 mmHg naturally between morning (higher) and evening (lower) in most individuals. Measuring at random times throughout the day generates scattered readings difficult to interpret.
Guidelines recommend consistent twice-daily measurements: once in the morning within an hour of waking and before medications, and once in the evening before bed. This schedule captures both morning surge and sustained daytime blood pressure while maintaining consistency for trend analysis.
Ignoring user manual instructions leads to various errors. Each device has specific cuff placement requirements, measurement protocols, and maintenance procedures. Research shows many users never read instructions, relying on intuition that may not align with optimal technique.
Failing to verify accuracy periodically allows measurement drift to go undetected. Studies recommend annual accuracy checks against healthcare provider measurements or comparing readings to a properly sized arm monitor. The research finding that a majority of home devices showed 5+ mmHg errors when tested on actual owners highlights the importance of verification.
How Should You Choose Between Arm and Wrist Blood Pressure Monitors?
Clinical guideline alignment should guide the decision for most users. The American Heart Association, Japanese Society of Hypertension, European Society of Hypertension, and American Medical Association all recommend upper arm oscillometric monitors as first choice for home blood pressure monitoring.
This unified professional consensus reflects the accumulated research evidence showing superior accuracy, precision, and ease of use with arm monitors compared to wrist devices. For users without specific contraindications to arm measurement, following guideline recommendations provides the most evidence-based approach.
Arm size represents the clearest indication for considering wrist monitors. If arm circumference exceeds 42 cm and wide-range arm cuffs do not fit properly, a properly fitting wrist monitor (if wrist size falls within 13.5-21.5 cm range) provides more accurate readings than an incorrectly sized arm cuff.
Research confirms that using undersized cuffs systematically underestimates blood pressure with errors of 5-10 mmHg or more. Proper cuff sizing requires the bladder to encircle 80% of arm circumference. Wrist monitors avoid this issue for individuals with very large arms.
Arm injury, lymphedema, or surgical sites may contraindicate arm cuff use. Post-mastectomy patients should avoid blood pressure measurement on affected arms. Bilateral contraindications necessitate alternative measurement sites like wrists.
Portability requirements for frequent travelers or workers needing measurements throughout the day may justify wrist monitor convenience despite slightly lower accuracy. The compact size fitting in pockets or purses enables monitoring in offices, airplanes, hotels, or other settings where arm monitors prove impractical.
User dexterity and strength affect device usability. Wrist monitors typically require less arm mobility than the reaching-around motion needed to apply arm cuffs. Individuals with shoulder arthritis or limited arm flexibility may find wrist monitors easier to apply independently.
However, this advantage disappears if users cannot maintain the elevated arm position required for accurate wrist measurement. Those with arm weakness, tremors, or endurance limitations may struggle holding arms elevated at heart level for the 30-60 second measurement duration.
Cost considerations may favor basic wrist monitors for budget-conscious users, though entry-level arm monitors like the OMRON Iron ($37) cost less than mid-range wrist devices while providing guideline-aligned measurement.
The key question involves measurement purpose. For clinical decision-making about medication titration or hypertension diagnosis, arm monitors provide accuracy and precision aligned with medical standards. For general wellness monitoring or tracking broad trends, properly used wrist monitors may suffice despite slightly higher variability.
Healthcare provider preference matters for users in remote monitoring programs or with insurance-covered home blood pressure devices. Many programs specifically require upper arm measurements to ensure consistency with clinical standards and guideline recommendations.
Complete Support System
The OMRON Connect app (free for iOS and Android) provides unlimited cloud storage for blood pressure readings from Bluetooth-enabled monitors. The app generates trend graphs, averages readings over user-selected time periods, and supports data export for sharing with healthcare providers.
Customer support for OMRON devices includes phone support at 1-800-634-4350, email support through their website, and comprehensive online resources including video tutorials on proper measurement technique, cuff sizing guides, and troubleshooting assistance.
The OMRON website maintains a Validated Device Listing showing which monitors have passed independent clinical validation according to international protocols. This resource helps consumers verify accuracy claims and compare validation performance across models.
Blood pressure monitoring guidelines from the American Heart Association and American Medical Association are available free online, providing evidence-based recommendations for measurement technique, frequency, and interpretation. These resources help users understand proper protocol for reliable home monitoring.
Many healthcare systems offer blood pressure monitoring education programs teaching proper technique, positioning, and interpretation. Asking about these resources during medical appointments can improve measurement quality and clinical value of home monitoring data.
Local pharmacies often provide blood pressure measurement services allowing users to verify home monitor accuracy against pharmacy-grade devices. This free or low-cost option supports the annual accuracy verification recommended by research.
Consumer Reports and other independent testing organizations periodically evaluate home blood pressure monitors, providing unbiased accuracy and usability comparisons. These resources supplement manufacturer specifications with real-world performance data.
FAQ
Are wrist blood pressure monitors as accurate as arm monitors? Clinical research shows upper arm monitors achieve superior accuracy with standard deviations of 3.6-3.9 mmHg compared to wrist monitors at 6.2 mmHg. A 2007 validation study found arm monitors provided more precise measurements than wrist devices, though both can pass international standards when properly calibrated and positioned at heart level.
When should I choose a wrist monitor over an arm monitor? Wrist monitors work best for individuals with very large upper arms where standard cuffs do not fit properly, those with arm injuries that make upper arm cuff use impractical, or travelers needing maximum portability. The Japanese Society of Hypertension recommends arm monitors as first choice, reserving wrist devices for situations where arm measurement is impractical.
Why do wrist monitors give different readings than arm monitors? Position-dependent measurement differences occur because wrist arteries are more affected by arm position relative to heart level. Research shows when arms are held horizontal at mid-sternum, wrist readings match arm readings (134/77 vs 137/80 mmHg), but dependent arm positions create significantly higher measurements due to hydrostatic pressure effects.
Do medical organizations recommend wrist blood pressure monitors? The American Heart Association prefers automated oscillometric upper arm devices for home monitoring. The Japanese Society of Hypertension explicitly states that finger-cuff and wrist-cuff devices should not be used for routine home blood pressure measurements, recommending upper arm cuff-oscillometric validated devices as the standard.
What is the accuracy difference between arm and wrist monitors in elderly users? A validation study in adults aged 75+ found upper arm monitors achieved mean differences of 0.2±3.6/0.2±3.9 mmHg while wrist monitors showed -1.5±6.2/-0.7±3.7 mmHg. The higher standard deviation for wrist measurements indicates lower precision, though interestingly, wrist monitor accuracy improves with increasing age according to regression analysis.
Can wrist monitors accurately detect atrial fibrillation? Validated wrist monitors using oscillometric technology can detect irregular heartbeats including atrial fibrillation when properly positioned. The OMRON Gold Wrist Monitor includes irregular heartbeat detection, though any abnormal rhythm finding should prompt confirmation with an upper arm monitor or clinical evaluation.
How does arm position affect wrist monitor accuracy? Arm position creates the largest source of error in wrist measurements. Studies show dependent arm positions produce significantly higher readings (P<0.05) compared to heart-level positioning. Maintaining the wrist horizontal at mid-sternum level during measurement is essential for accuracy comparable to upper arm devices.
What are the calibration requirements for wrist vs arm monitors? Research comparing wrist devices to direct intra-arterial measurements found pre-calibration errors of 10.8±9.7 mmHg systolic, improving to 7.2±5.1 mmHg post-calibration. This represents 33% systolic and 73% diastolic accuracy improvement with calibration, highlighting the importance of verification against reference standards for both device types.
Which type of monitor is better for daily home monitoring? Upper arm monitors provide superior day-to-day consistency with standard deviations typically under 4 mmHg compared to 6-8 mmHg for wrist devices. For reliable home monitoring tracking trends over time, arm monitors reduce measurement variability that could be mistaken for actual blood pressure changes.
Do wrist monitors work for people with irregular heartbeats? Modern wrist monitors like those validated under ISO 81060-2 standards can provide accurate readings with irregular heartbeats, though validation studies typically exclude individuals with atrial fibrillation or frequent ectopic beats. For diagnosed arrhythmias, upper arm monitors offer more reliable measurements with less position-dependent variability.
Our Top Recommendations
For most users following clinical guideline recommendations, the OMRON Platinum Blood Pressure Monitor ($97) delivers professional-grade upper arm measurement with AFib detection, TruRead averaging, and Bluetooth connectivity providing the accuracy and features supported by research evidence.
Budget-conscious users seeking guideline-aligned monitoring should consider the OMRON Iron Blood Pressure Monitor ($37), which provides doctor-recommended brand reliability and wide-range cuff fitting at entry-level pricing.
Individuals with very large upper arms, arm injuries, or specific portability requirements may benefit from the OMRON Gold Wireless Wrist Blood Pressure Monitor ($78), which offers clinically validated wrist measurement with Bluetooth connectivity and positioning guidance for optimal accuracy.
Cost-conscious users requiring wrist monitoring can consider the Oklar Rechargeable Wrist Blood Pressure Monitor ($28) for basic wrist measurement with rechargeable battery convenience and extensive memory storage, though understanding that generic devices lack the validation documentation of major brands.
The choice between arm and wrist monitors ultimately depends on individual circumstances, but for most users, upper arm devices provide the evidence-based accuracy, precision, and guideline alignment that support reliable home blood pressure monitoring.
Join the discussion: Facebook | X | YouTube | Pinterest
Conclusion
Clinical research consistently demonstrates that upper arm blood pressure monitors achieve superior accuracy and precision compared to wrist devices, with standard deviations typically 40-60% lower and better alignment with international validation protocols. The recommendation from major medical organizations including the American Heart Association and Japanese Society of Hypertension for upper arm oscillometric monitors reflects this evidence base.
Wrist monitors can achieve clinically acceptable accuracy when properly positioned at heart level, as demonstrated by multiple validation studies meeting ISO 81060-2 standards. However, the position-dependent measurement variation inherent to wrist monitoring creates a practical limitation that arm monitors largely avoid.
For individuals with very large upper arms, bilateral arm contraindications, or specific portability requirements, validated wrist monitors provide valuable monitoring alternatives when used with attention to proper positioning technique. The key involves understanding that wrist monitors require more user discipline and technique awareness to achieve accuracy comparable to arm devices.
The choice should consider individual circumstances, clinical requirements, and user capabilities. Following clinical guideline recommendations for upper arm monitoring provides the most evidence-based approach for most users, while recognizing specific situations where wrist monitors offer practical advantages despite slightly higher measurement variability.
Regardless of device type chosen, proper technique, consistent measurement schedules, and periodic accuracy verification contribute to reliable home blood pressure monitoring supporting cardiovascular health management.
Related Reading
- Best Blood Pressure Monitors for Home Use - Comprehensive guide to the most accurate home BP monitors
- Best OMRON Blood Pressure Monitors Compared - Detailed comparison of OMRON device lineup
- Best Cooling Mattress Pads - Sleep quality affects blood pressure regulation
- Menopause Hot Flashes Supplements - Hormonal changes impact cardiovascular health
- Energy and Fatigue Supplements for Women 40+ - Cardiovascular health supports energy levels
References
Cuckson AC, Moran P, Seed P, Reinders A, Shennan AH. Clinical evaluation of an automated oscillometric blood pressure wrist device. Blood Pressure Monitoring. 2004;9(1):23-29. PMID: 15021076.
Xie Z, Peng B, Hu J, Wang X, Du X. Validation of TMB-2285-BT wrist blood pressure monitor in general population according to the ISO 81060-2:2018 + Amd.1:2020 Protocol. Blood Pressure Monitoring. 2025;30(1):30-36. PMID: 39279437.
Melville S, Teskey R, Philip S, Simpson JA, Lutchmedial S. A Comparison and Calibration of a Wrist-Worn Blood Pressure Monitor for Patient Management: Assessing the Reliability of Innovative Blood Pressure Devices. Journal of Medical Internet Research. 2018;20(4):e102. PMID: 29695375.
Omboni S, Riva I, Giglio A, Caldara G, Groppelli A. Validation of the Omron M5-I, R5-I and HEM-907 automated blood pressure monitors in elderly individuals according to the International Protocol of the European Society of Hypertension. Blood Pressure Monitoring. 2007;12(4):233-242. PMID: 17625396.
Angeli F, Sardone M, Angeli E, Repaci S, Gattobigio R. Validation of the A&D wrist-cuff UB-511 (UB-512) device for self-measurement of blood pressure. Blood Pressure Monitoring. 2006;11(6):323-328. PMID: 17106320.
Araujo-Moura K, Souza LG, Mello GL, De Moraes ACF. Blood pressure measurement in pediatric population: comparison between automated oscillometric devices and mercury sphygmomanometers-a systematic review and meta-analysis. European Journal of Pediatrics. 2022;181(1):9-20. PMID: 34272985.
Zhou Q. Validation of the DBP-8278B Wrist-type Fully Automatic Blood Pressure Monitor in the general population according to the ISO 81060-2:2018/AMD 1:2020 protocol. Blood Pressure Monitoring. 2025;30(1):12-18. PMID: 39008688.
Mourad A, Gillies A, Carney S. Inaccuracy of wrist-cuff oscillometric blood pressure devices: an arm position artefact? Blood Pressure Monitoring. 2005;10(2):67-71. PMID: 15812253.
Imai Y, Otsuka K, Kawano Y, Shimada K, Hayashi H. Japanese society of hypertension (JSH) guidelines for self-monitoring of blood pressure at home. Hypertension Research. 2003;26(10):771-782. PMID: 14621179.
Liu J, Sodini CG, Ou Y, Yan B, Zhang YT. Feasibility of Fingertip Oscillometric Blood Pressure Measurement: Model-Based Analysis and Experimental Validation. IEEE Journal of Biomedical and Health Informatics. 2020;24(7):1994-2005. PMID: 31150350.
Celler BG, Yong A, Rubenis I, Butlin M, Argha A. Validation of oscillometric ratio and maximum gradient methods for non-invasive blood pressure measurement with intra-arterial blood pressure measurements as reference. Journal of Hypertension. 2024;42(6):1019-1029. PMID: 38690906.
Liu J, Cheng HM, Chen CH, Sung SH, Hahn JO. Patient-Specific Oscillometric Blood Pressure Measurement: Validation for Accuracy and Repeatability. IEEE Journal of Translational Engineering in Health and Medicine. 2017;5:1900111. PMID: 29018632.
Liu J, Cheng HM, Chen CH, Sung SH, Moslehpour M. Patient-Specific Oscillometric Blood Pressure Measurement. IEEE Transactions on Biomedical Engineering. 2016;63(6):1220-1228. PMID: 26485351.
Muntner P, Shimbo D, Carey RM, Charleston JB, Gaillard T. Measurement of Blood Pressure in Humans: A Scientific Statement From the American Heart Association. Hypertension. 2019;73(5):e35-e66. PMID: 30827125.
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



