Blood Pressure Monitors with AFib Detection: Oscillometric Screening for Atrial Fibrillation
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Undetected atrial fibrillation increases stroke risk five-fold, yet 30% of AFib cases remain asymptomatic and undiagnosed until a catastrophic event occurs. The OMRON Platinum BP5450 ($97) combines validated oscillometric blood pressure measurement with AFib-specific detection algorithms that achieve 97% sensitivity and 95% specificity when using the TruRead triple-measurement protocol. Meta-analyses of 12 studies involving 4,519 patients demonstrate that oscillometric monitors with AFib detection identify irregular atrial rhythms with 88.4% overall sensitivity and 95.3% specificity (P<0.001), providing clinically meaningful screening capability that bridges the gap between routine home monitoring and diagnostic cardiac evaluation. For budget-conscious users, the OMRON Bronze BP6000 ($41) offers basic irregular heartbeat detection suitable for initial arrhythmia screening. Here’s what the published research shows about oscillometric AFib detection technology, validation protocols, and evidence-based selection criteria for home cardiovascular screening.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
| Feature | OMRON Platinum BP5450 | Withings BPM Connect | OMRON Bronze BP6000 | OMRON Silver BP5250 |
|---|---|---|---|---|
| Price | $97 | $179 | $41 | $63 |
| AFib Detection | Yes, specific algorithm | Yes, FDA-cleared | Basic irregular HB | Basic irregular HB |
| Connectivity | Bluetooth | WiFi + Bluetooth | None | Bluetooth |
| Memory | 200 readings (2 users) | Unlimited (cloud) | 14 readings | 120 readings (2 users) |
| Cuff Range | 22-42 cm | 22-42 cm | 22-42 cm | 22-42 cm |
| App Integration | OMRON Connect | Health Mate | None | OMRON Connect |
| Averaging | TruRead (3 readings) | Single optimized | Single reading | Advanced averaging |
| Validation | AAMI/ESH | FDA cleared | AAMI | AAMI |
| Power | 4 AA batteries | Rechargeable | 4 AA batteries | 4 AA batteries |
| Display | Large backlit LCD | Color LED | Standard LCD | Large LCD |
What Is AFib Detection Technology in Blood Pressure Monitors?
AFib detection in oscillometric blood pressure monitors analyzes pulse wave irregularities during standard BP measurement to identify the characteristic rhythm patterns of atrial fibrillation. Unlike basic irregular heartbeat indicators that simply flag any abnormal rhythm, AFib-specific algorithms discriminate between atrial fibrillation and other arrhythmias through pattern recognition analysis of oscillometric waveforms.
The technology works by measuring pressure oscillations in the brachial artery as the cuff deflates. In normal sinus rhythm, these oscillations follow a predictable pattern with consistent intervals between pulse waves. Atrial fibrillation creates irregularly irregular intervals—no discernible pattern—which the algorithm identifies through statistical analysis of R-R interval variability.
Systematic reviews demonstrate that oscillometric AFib detection achieves 97% sensitivity and 95% specificity when three consecutive measurements are analyzed. This triple-measurement protocol, validated in the 2012 Verberk and de Leeuw meta-analysis published in Expert Review of Medical Devices, significantly outperforms single-reading screening which shows approximately 85% sensitivity.
The clinical significance stems from AFib’s impact on stroke risk. Research published in JAMA Cardiology by Gladstone et al. shows home-based BP monitor screening detected AFib in 5.3% of adults over 75 compared to 0.5% detection in control groups receiving standard care. These are asymptomatic cases that would otherwise remain undiagnosed until stroke occurrence.
Key takeaway: AFib detection technology transforms routine home blood pressure monitoring into dual-purpose cardiovascular screening, identifying both hypertension and atrial fibrillation—two conditions that frequently coexist, with 70% of AFib patients having hypertension according to the 2025 AF-SCREEN International Collaboration review.
Detection accuracy depends on proper measurement technique. The monitor must complete the full measurement cycle without movement or talking. Cuff positioning 1-2 cm above the elbow crease, arm supported at heart level, and back supported sitting position all affect oscillometric waveform quality. Studies show measurement protocol adherence increases detection accuracy by 12-15 percentage points.
The algorithm distinguishes AFib from other arrhythmias including premature atrial contractions, premature ventricular contractions, and atrial flutter through waveform morphology analysis. While these other arrhythmias may trigger basic irregular heartbeat warnings, validated AFib detection specifically identifies the irregularly irregular pattern characteristic of atrial fibrillation.
Clinical validation requires comparison against gold-standard 12-lead ECG confirmation. The 2019 meta-analysis by Park et al. in Expert Review of Medical Devices analyzed 12 validation studies involving 4,519 patients, confirming 88.4% pooled sensitivity and 95.3% pooled specificity across multiple oscillometric monitor brands.
How Do Oscillometric Monitors Detect Atrial Fibrillation During Blood Pressure Measurement?
Oscillometric detection analyzes arterial pressure oscillations as the cuff deflates from suprasystolic pressure. The monitor measures small pressure changes transmitted from the brachial artery through the cuff to a pressure sensor. These oscillations create a waveform envelope—the oscillometric waveform—that reveals both blood pressure values and cardiac rhythm characteristics.
In normal sinus rhythm, oscillations occur at regular intervals corresponding to heartbeats controlled by the sinoatrial node. The time between oscillation peaks (analogous to R-R intervals on ECG) shows minimal variation, typically less than 10% coefficient of variation. Atrial fibrillation disrupts this regularity, creating highly variable R-R intervals with no discernible pattern.
The AFib detection algorithm calculates statistical measures of variability including standard deviation, coefficient of variation, and entropy measures from the oscillation interval sequence. When variability exceeds validated thresholds—typically coefficient of variation above 25-30%—the algorithm flags probable AFib.
Research by Stergiou et al. published in the Journal of Human Hypertension tested the Microlife BPA100 Plus in 73 patients. The study found 93% sensitivity and 89% specificity for AFib detection compared to ECG confirmation. Notably, 37% of participants had AFib and 31% had other arrhythmias, demonstrating the algorithm’s ability to distinguish AFib from other irregular rhythms.
The detection process occurs automatically during normal BP measurement. Users perform standard measurement protocol—rest 5 minutes, position arm correctly, remain still and silent during measurement. The monitor displays both BP values and AFib indicator simultaneously. No additional time or steps are required beyond standard BP measurement.
What this means: Users gain cardiovascular screening without additional effort, time, or cost per measurement. The dual-purpose capability addresses the hypertension-AFib connection, as both conditions frequently coexist and share risk factors including age, obesity, and cardiovascular disease.
Oscillometric AFib detection differs from photoplethysmography (PPG) methods used in smartwatches. PPG measures blood volume changes in peripheral arteries through light absorption, while oscillometric monitors measure pressure oscillations in large brachial arteries. Clinical validation shows comparable accuracy between methods, but oscillometric detection occurs during established BP monitoring routines rather than requiring separate screening sessions.
The 2023 study by Li et al. in Blood Pressure Monitoring followed 295 patients for 5.9 years, demonstrating sustained screening accuracy (P<0.001) and practical feasibility of long-term home-based AFib surveillance integrated with hypertension management.
False positives occur primarily from measurement artifact—movement, talking, or cuff position errors that create irregular oscillation patterns mimicking AFib. Proper measurement technique reduces false positives to less than 5%. False negatives occur most commonly in paroxysmal AFib cases where measurements happen during sinus rhythm intervals.
What Does Research Show About Blood Pressure Monitor AFib Detection Accuracy?
Meta-analytic evidence demonstrates clinically significant accuracy for oscillometric AFib screening. The 2019 systematic review and meta-analysis by Park et al. pooled data from 12 validation studies involving 4,519 patients, finding 88.4% pooled sensitivity and 95.3% pooled specificity for AFib detection (P<0.001).
Breaking down these statistics: sensitivity of 88.4% means the monitors correctly identified 88.4% of patients with ECG-confirmed AFib. Specificity of 95.3% means 95.3% of patients without AFib received correct negative screening results. These accuracy levels meet clinical screening thresholds for meaningful cardiovascular risk stratification.
The triple-measurement protocol significantly improves accuracy. Verberk and de Leeuw’s 2012 systematic review found three consecutive measurements achieved 97% sensitivity and 95% specificity—9 percentage points higher sensitivity than single measurements. This improvement stems from repeated rhythm sampling that reduces impact of transient irregularities or measurement artifact.
The research verdict: Triple-measurement protocols should be standard practice for AFib screening, while single measurements provide adequate accuracy for routine monitoring in patients with established AFib.
The 2021 randomized clinical trial by Gladstone et al. published in JAMA Cardiology tested population-level screening effectiveness. The trial enrolled 856 adults aged 75 and older, randomizing participants to home BP monitor screening versus usual care. AFib detection occurred in 5.3% of the screening group compared to 0.5% in controls—a 10-fold difference demonstrating home screening’s ability to identify previously undiagnosed cases.
Clinical validation studies compare oscillometric detection against gold-standard diagnostic methods including 12-lead ECG, Holter monitoring, and electrophysiology study. The Stergiou 2009 study used simultaneous ECG recording during BP measurements, finding 93% sensitivity and 89% specificity with the Microlife BPA100 Plus in real-world home conditions.
Accuracy varies by AFib burden—persistent AFib shows higher detection rates than paroxysmal AFib because the irregular rhythm is present during all measurements. Research suggests daily measurements over one week detect 85-90% of paroxysmal AFib cases, while single-day screening may miss intermittent episodes.
The 2023 Li et al. longitudinal study followed patients for 5.9 years, demonstrating sustained accuracy over time. This long-term validation addresses concerns about algorithm performance degradation or false alarm rates that might reduce adherence to screening recommendations.
Subgroup analyses show consistent accuracy across demographics. The 2020 meta-analysis by Taggar et al. in European Heart Journal found 98.1% sensitivity and 92.2% specificity for automated BP monitor AFib screening, with accuracy maintained across age groups, sex, and presence of hypertension.
Here’s what matters: The evidence base includes over 5,000 patients across multiple studies using different monitor brands, demonstrating reproducible accuracy that supports clinical guideline integration of home-based AFib screening.
Limitations include inability to classify AFib type (paroxysmal versus persistent), quantify AFib burden, or assess stroke risk beyond detecting presence of the arrhythmia. Positive screening results require professional cardiac evaluation with diagnostic ECG and clinical assessment for anticoagulation decisions.
Are Blood Pressure Monitors Accurate for People Who Already Have AFib?
Oscillometric monitors provide reliable blood pressure readings in patients with atrial fibrillation when proper measurement protocols are followed. The 2013 study by Pagonas et al. published in Hypertension tested 102 patients with AFib, finding that triple-measurement averaging produced BP values within 5 mmHg of invasive arterial monitoring—the gold standard for BP measurement accuracy.
The irregular heart rhythm in AFib creates beat-to-beat BP variability that makes single readings unreliable. Individual measurements may vary by 15-20 mmHg even within the same measurement session. However, averaging three consecutive measurements reduces this variability to clinically acceptable levels comparable to accuracy in sinus rhythm patients.
Research published in Clinical and Experimental Pharmacology & Physiology by Kollias and Stergiou reviewed automated BP measurement in AFib patients across office, home, and ambulatory settings. The review concluded that oscillometric monitors provide valid BP assessment in AFib populations when manufacturers’ protocols specifying multiple sequential measurements are followed.
The evidence shows: Patients with established AFib should take three consecutive readings with 1-2 minute intervals between measurements, then average the results. This protocol appears in clinical guidelines including the 2020 American Heart Association Scientific Statement on self-measured blood pressure monitoring.
Device selection matters for AFib patients. Monitors with automatic triple-measurement protocols like the OMRON Platinum’s TruRead feature eliminate user burden of performing and calculating multiple measurement averages. These automated protocols improve adherence to proper measurement technique.
The 2017 comparison study in BMC Cardiovascular Disorders (PMID 28335730) directly compared auscultatory (manual) versus oscillometric BP measurement in AFib patients. Oscillometric monitors showed equivalent accuracy to trained observer auscultatory measurements when triple-measurement protocols were used, with the advantage of eliminating observer bias and hearing-dependent measurement variability.
Clinical implications extend to hypertension management in the 70% of AFib patients who have elevated blood pressure. The 2025 review from the AF-SCREEN International Collaboration emphasizes that combined BP and rhythm monitoring enables integrated cardiovascular risk management, addressing both conditions through single home monitoring routines.
Clinical insight: Healthcare providers should specify triple-measurement protocols when prescribing home BP monitoring for AFib patients, and review actual measurement data rather than relying on single readings that may not reflect true average BP.
Limitations exist for severe arrhythmias. Extremely irregular rhythms or rapid ventricular rates above 120 bpm may stop oscillometric monitors from completing measurements. In these cases, manual auscultatory measurement or invasive arterial monitoring may be necessary for accurate BP assessment.
The 2015 review in Journal of Clinical Hypertension (PMID 25865223) titled “Should Oscillometric Blood Pressure Monitors Be Used in Patients With Atrial Fibrillation?” concluded that oscillometric monitors are appropriate for AFib patients when validation-specified measurement protocols are followed, but single readings should not guide clinical decisions.
What Features Should You Look for in a BP Monitor with AFib Detection?
AFib-specific detection algorithms represent the primary feature distinction from basic irregular heartbeat indicators. Validated AFib detection uses proprietary algorithms that analyze oscillometric waveform patterns to specifically identify atrial fibrillation, while basic irregular heartbeat detection simply flags any rhythm abnormality without distinguishing AFib from other arrhythmias.
Clinical validation credentials indicate algorithm accuracy. Look for monitors with published validation studies comparing AFib detection against ECG confirmation. Devices cleared by FDA for AFib detection or validated according to European Society of Hypertension protocols provide evidence-based performance data. The absence of published validation studies raises questions about detection accuracy.
Automatic triple-measurement capability streamlines proper screening protocol. Features like OMRON’s TruRead automatically perform three consecutive measurements at specified intervals and display the average result. This automation ensures protocol adherence without requiring users to manually perform and calculate multiple measurements.
What the data says: Research shows automated triple-measurement protocols improve measurement consistency and reduce user error compared to manual sequential measurements, increasing screening accuracy by 8-12 percentage points in real-world home conditions.
Memory capacity affects long-term monitoring capability. Monitors storing 100+ readings enable weekly or monthly trend analysis. Dual-user memory allows household sharing for couples where both partners require cardiovascular monitoring. Cloud-connected monitors offer unlimited storage with historical trend graphs extending years.
Connectivity features enable data sharing with healthcare providers. Bluetooth or WiFi sync transfers measurements to smartphone apps that generate reports viewable during telehealth appointments or shareable via patient portals. This connectivity transforms home monitoring from isolated data points to integrated longitudinal records supporting clinical decision-making.
Cuff size compatibility ensures accurate measurements. Standard cuffs fit arm circumferences 22-42 cm, covering approximately 85% of adults. Individuals with larger or smaller arms require monitors offering compatible cuff sizes, as incorrect cuff size introduces measurement errors of 5-10 mmHg—clinically significant when assessing hypertension control.
Display clarity matters for users with vision limitations. Large, backlit displays with high-contrast numbers improve readability. Color-coded BP classification indicators (green/yellow/red for normal/elevated/high readings) provide immediate interpretation without requiring users to memorize numerical BP targets.
The practical takeaway: Features should match individual needs—tech-savvy users benefit from connectivity and apps, while users preferring simplicity need large displays and one-button operation. Both approaches can deliver accurate AFib screening when core detection algorithms are validated.
Validation stamps indicate independent accuracy testing. Look for AAMI (Association for the Advancement of Medical Instrumentation), ESH (European Society of Hypertension), or BHS (British Hypertension Society) validation. These organizations maintain standardized testing protocols comparing monitor measurements against reference standards.
Battery versus AC power affects placement flexibility. Battery-powered monitors enable measurements anywhere in the home, while AC-powered monitors require proximity to outlets. Rechargeable batteries eliminate disposable battery costs but require remembering to charge the device.
Irregular heartbeat indicators vary in specificity. Some monitors display a heart icon when any irregularity is detected, while others specifically indicate “AFib Detected” or “Possible AFib.” The more specific indicators reduce anxiety from non-AFib irregularities like premature beats that don’t carry AFib’s stroke risk.
How Often Should You Use AFib Detection Features on Your BP Monitor?
Screening frequency depends on stroke risk factors and symptoms. Adults over 65 with hypertension should perform AFib screening during routine BP monitoring—typically morning and evening measurements daily or several times weekly. This opportunistic screening integrates cardiovascular surveillance without additional time commitment.
The 2021 Gladstone trial (PMID 33625468) used twice-daily measurements for one week per month in adults 75 and older, detecting previously undiagnosed AFib in more than 1 in 20 participants. This protocol balances detection sensitivity against monitoring burden, making extended surveillance practical for long-term adherence.
For individuals with AFib symptoms—palpitations, unexplained fatigue, shortness of breath, or dizziness—daily measurements for one to two weeks provide rhythm assessment over multiple days. This extended monitoring increases detection probability for paroxysmal AFib that may not occur during single-day screening.
In practice: Established hypertension patients should use AFib detection with every BP measurement. The detection occurs automatically during standard measurements, requiring no additional steps or time. This approach maximizes screening frequency without increasing monitoring burden.
Patients with diagnosed AFib use the detection feature differently—for rhythm monitoring rather than screening. Daily measurements help identify AFib recurrence after cardioversion or assess rhythm control on antiarrhythmic medications. Pattern changes warrant provider communication about potential treatment adjustments.
Post-screening frequency depends on initial results. Negative screening in low-risk individuals may warrant monthly rather than daily AFib-enabled measurements, while positive screening results require immediate provider contact for diagnostic ECG confirmation. After professional evaluation, the provider specifies appropriate ongoing monitoring frequency.
The three-consecutive-measurement protocol validated in research (PMID 23249156) should be used for dedicated AFib screening sessions. For routine BP monitoring in patients not specifically screening for AFib, single measurements with automated AFib detection provide adequate surveillance between focused screening sessions.
Our verdict: Integration of AFib detection with routine BP monitoring creates sustainable long-term surveillance. The key is establishing measurement routines that persist over months and years, as AFib incidence increases with age and paroxysmal AFib may emerge intermittently over extended timeframes.
Seasonal variation in AFib occurrence suggests periodic intensified screening. Studies show increased AFib episodes during winter months and following illness. Increasing measurement frequency during these periods may improve detection of incident AFib cases.
Time-of-day considerations affect detection probability in paroxysmal AFib. Morning measurements capture nocturnal AFib episodes, while evening measurements assess daytime rhythm. Twice-daily measurements—morning and evening—provide temporal coverage increasing detection sensitivity for intermittent arrhythmias.
The 2023 longitudinal study by Li et al. (PMID 37016988) followed patients for 5.9 years with periodic AFib screening, demonstrating that sustained monitoring over years identifies incident AFib cases missed by one-time screening. This supports ongoing surveillance rather than single screening episodes.
What Do You Do If Your BP Monitor Detects AFib?
Immediate provider contact is the appropriate first response to AFib detection. Call your healthcare provider’s office to report the finding and request appointment scheduling for diagnostic evaluation. Most practices can accommodate urgent cardiovascular evaluations within 24-48 hours when patients report possible AFib.
Do not self-diagnose or initiate treatment based solely on BP monitor detection. The monitor provides screening data, not diagnostic confirmation. Professional cardiac evaluation with 12-lead ECG is required to confirm AFib, classify the type (paroxysmal versus persistent), and assess need for anticoagulation or other treatments.
Continue normal activities while awaiting evaluation unless you experience concerning symptoms. AFib detection without symptoms (chest pain, severe shortness of breath, syncope) does not constitute a medical emergency requiring emergency department visits. However, symptomatic AFib warrants urgent evaluation—call 911 for chest pain or severe symptoms.
The implication: Home AFib detection enables early identification and planned evaluation rather than emergency presentation after stroke or other complications. This proactive pathway improves outcomes through timely risk assessment and treatment initiation.
Document detection patterns before the appointment. Note date, time, and BP readings when AFib was detected. Take multiple measurements over several days if possible—this pattern data helps providers assess whether AFib is paroxysmal or persistent. Many monitors with connectivity features generate reports showing detection frequency.
Prepare questions for the provider appointment. Topics include: need for anticoagulation, stroke risk assessment (CHA2DS2-VASc score), rhythm control versus rate control strategies, monitoring recommendations, activity restrictions, and follow-up testing plans. Informed participation in decision-making improves adherence to treatment recommendations.
Expect diagnostic testing during evaluation. Standard workup includes 12-lead ECG to confirm AFib, echocardiogram to assess cardiac structure and function, thyroid function tests to identify secondary causes, and stroke risk calculation. Some providers order extended monitoring with Holter monitors or event recorders to quantify AFib burden.
The CHA2DS2-VASc score guides anticoagulation decisions. This scoring system assigns points for stroke risk factors: Congestive heart failure (1 point), Hypertension (1 point), Age 75+ (2 points), Diabetes (1 point), Stroke/TIA history (2 points), Vascular disease (1 point), Age 65-74 (1 point), Sex category female (1 point). Scores of 2+ in men or 3+ in women typically warrant anticoagulation.
Research summary: Clinical trials demonstrate anticoagulation reduces stroke risk by 64% in AFib patients with elevated CHA2DS2-VASc scores. Early detection through home screening enables timely anticoagulation initiation, reducing strokes that would occur during the undiagnosed period.
Treatment options depend on AFib classification and symptoms. Paroxysmal AFib may warrant observation without antiarrhythmic drugs if episodes are infrequent and asymptomatic. Persistent or symptomatic AFib often requires rate control medications (beta-blockers, calcium channel blockers) or rhythm control strategies including antiarrhythmic drugs or catheter ablation.
Follow-up monitoring typically includes repeat BP measurements with AFib detection to assess treatment response and rhythm status. Patients on antiarrhythmic medications use home monitoring to identify recurrent AFib prompting medication adjustments. Those who undergo cardioversion use detection features to monitor for AFib recurrence.
Who Should Use a Blood Pressure Monitor with AFib Detection?
Adults over 65 represent the primary target population for AFib screening. AFib prevalence increases exponentially with age—approximately 2% at age 65, rising to 9% by age 80. The 2021 Gladstone trial (PMID 33625468) focused on adults 75 and older, detecting previously undiagnosed AFib at 10 times the rate of usual care through home BP monitor screening.
Hypertension patients benefit from integrated BP and AFib monitoring. Research from the AF-SCREEN International Collaboration (PMID 40127157) shows the majority of AFib patients have hypertension. The conditions share pathophysiology—chronic elevated BP causes left atrial enlargement and fibrosis that predispose to AFib. Monitoring both conditions simultaneously addresses interconnected cardiovascular risks.
Individuals with stroke risk factors should consider AFib-detection monitors even without hypertension. Risk factors include diabetes, heart failure, coronary artery disease, sleep apnea, obesity, and family history of AFib. These conditions increase both AFib likelihood and stroke risk if AFib develops, making early detection particularly valuable.
The science says: Population-based screening in high-risk groups is cost-effective when screening is integrated with existing healthcare interactions like BP monitoring rather than requiring dedicated screening programs. Home monitor detection achieves this integration efficiently.
People with unexplained palpitations, fatigue, or exercise intolerance warrant AFib screening. These symptoms may indicate paroxysmal AFib—intermittent episodes occurring unpredictably. Home monitoring over extended periods increases detection probability for episodic arrhythmias missed during brief office visits.
Patients with cryptogenic stroke—stroke without identified cause—require extended AFib screening. Studies show that intensive cardiac monitoring detects AFib in 20-30% of cryptogenic stroke patients, suggesting undiagnosed paroxysmal AFib caused the stroke. Home BP monitors with AFib detection provide ongoing surveillance for arrhythmia emergence.
First-degree relatives of AFib patients face increased genetic risk. Studies show 40% increased AFib risk in individuals with affected first-degree relatives. Proactive screening in this population enables early detection during the asymptomatic phase when treatment may slow progression to persistent AFib.
Athletes with cardiac remodeling may benefit from rhythm monitoring. Endurance athletes show higher AFib rates than sedentary populations, attributed to atrial enlargement from chronic volume loading. Home monitoring helps distinguish benign athletic heart adaptations from pathological rhythm disturbances.
What the data tells us: Universal screening for adults 65+ appears cost-effective based on modeling studies using current AFib-detection monitor pricing. The prevention of even one stroke per 100 screened individuals offsets screening costs given stroke treatment expenses exceeding $100,000 in the first year.
Individuals preferring proactive health management represent good candidates regardless of age if other risk factors exist. The monitors enable opportunistic screening during routine health maintenance without requiring additional healthcare visits or time investment beyond standard BP monitoring.
Populations where AFib detection may have limited value include younger adults without risk factors, individuals with established AFib already on appropriate treatment, and patients with other arrhythmias already under cardiac care. These groups derive minimal additional benefit from AFib-detection features beyond standard BP monitoring capability.
What Is the Difference Between AFib Detection and Irregular Heartbeat Detection?
AFib detection uses specific algorithms designed to identify the characteristic irregularly irregular rhythm pattern of atrial fibrillation. These algorithms analyze statistical properties of R-R interval variability that distinguish AFib from other arrhythmias. Clinical validation involves comparison against ECG-confirmed AFib diagnoses, with sensitivity and specificity calculated specifically for AFib detection.
Irregular heartbeat detection flags any abnormal rhythm without distinguishing the specific arrhythmia type. These basic indicators trigger when the monitor detects rhythm patterns outside normal parameters—including AFib but also premature atrial contractions, premature ventricular contractions, atrial flutter, and artifact from movement or improper technique.
The distinction matters clinically because different arrhythmias carry different risks and treatment implications. AFib significantly increases stroke risk, warranting anticoagulation in high-risk patients. Isolated premature beats generally require no treatment. Irregular heartbeat warnings without AFib-specific algorithms may cause unnecessary anxiety about benign findings or false reassurance when AFib is present alongside other rhythm abnormalities.
The distinction: AFib-specific detection provides actionable cardiovascular risk information. Basic irregular heartbeat detection serves as a general screening flag requiring professional rhythm assessment to determine clinical significance.
Validation standards differ between technologies. AFib detection algorithms undergo testing against ECG-confirmed AFib with published sensitivity and specificity data. Irregular heartbeat indicators may have less rigorous validation, sometimes simply detecting beat-to-beat interval variability exceeding a threshold without specific arrhythmia classification.
The 2012 Verberk and de Leeuw systematic review (PMID 23249156) analyzed AFib-specific detection algorithms, finding near-perfect sensitivity and specificity with triple measurements. These accuracy levels enable clinical decision-making. Basic irregular heartbeat detection without arrhythmia classification cannot support specific treatment decisions beyond prompting professional evaluation.
User interpretation differs substantially. AFib detection provides clear, specific information—“AFib Detected” messages indicate the monitor identified the rhythm pattern associated with increased stroke risk. Irregular heartbeat icons require users to understand that many rhythm abnormalities may trigger the indicator, most of which do not require treatment.
Price points generally separate the technologies. Budget BP monitors typically offer irregular heartbeat detection, while mid-range and premium devices include validated AFib-specific algorithms. The price difference reflects development and validation costs for proprietary AFib detection algorithms.
In summary: Patients with stroke risk factors benefit most from AFib-specific detection’s diagnostic precision. Those seeking general cardiovascular screening may find basic irregular heartbeat detection sufficient as a flag prompting professional evaluation when abnormalities occur.
Healthcare provider recommendations often specify AFib detection for high-risk patients. Clinical guidelines increasingly recognize home-based AFib screening’s role in stroke prevention. Providers prescribing monitors for these populations should specify AFib-detection capability rather than basic irregular heartbeat indicators.
The marketing distinction sometimes blurs with manufacturers using “AFib detection” language for devices that only detect irregular rhythms without specific AFib classification algorithms. Checking for published validation studies helps clarify whether a device offers true AFib-specific detection or basic rhythm irregularity flagging.
How Do OMRON AFib Detection Monitors Compare to Other Brands?
OMRON holds dominant market share in home BP monitors with AFib detection, offering three distinct tiers: Bronze (basic irregular heartbeat detection), Silver (irregular heartbeat detection with Bluetooth), and Platinum (validated AFib-specific detection with TruRead). This tiered approach addresses different user needs and price points.
The Platinum series features OMRON’s most advanced AFib detection algorithm, validated in clinical studies and incorporated into the TruRead triple-measurement protocol. The automatic sequential measurements and AFib analysis occur without user intervention—press the start button and the monitor completes the full screening sequence.
Withings offers premium positioning with FDA-cleared AFib detection, WiFi connectivity, and integration with the comprehensive Health Mate app ecosystem. The rechargeable battery and compact design appeal to tech-focused users prioritizing connectivity and mobile health platform integration. At $179, Withings targets users willing to pay premium prices for advanced features.
The value assessment: OMRON Platinum at $97 provides validated AFib detection and automatic triple-measurement protocol at nearly half Withings’ price. Withings offers superior connectivity and app experience but equivalent AFib detection accuracy, making OMRON the value leader for users prioritizing screening capability over advanced app features.
Microlife pioneered oscillometric AFib detection with the BPA100 Plus, validated in the 2009 Stergiou study (PMID 19279661) showing 93% sensitivity and 89% specificity. Microlife devices remain available primarily in international markets with limited US distribution, making OMRON and Withings the primary domestic options for AFib-detection monitors.
Comparison of validation evidence reveals similar accuracy across brands. The 2019 Park meta-analysis (PMID 31095424) included studies of OMRON, Microlife, and other brands, finding no significant accuracy differences between manufacturers when proper validation protocols were followed. This suggests AFib detection accuracy depends more on measurement protocol adherence than brand-specific algorithm superiority.
User interface design differentiates brands significantly. OMRON emphasizes large displays with simple one-button operation appealing to older adults less comfortable with technology. Withings targets smartphone-native users with minimalist hardware and comprehensive app functionality. Both approaches deliver accurate measurements when users engage with the interface successfully.
Our recommendations: Technology-averse users benefit from OMRON’s straightforward operation. Tech-savvy users preferring integrated health platforms find Withings’ app ecosystem more engaging for long-term adherence. Accuracy remains equivalent when measurement protocols are followed correctly.
Clinical validation transparency varies by manufacturer. OMRON publishes validation studies for professional review, while some competitors provide less accessible validation documentation. Healthcare providers prescribing monitors for AFib screening should verify published validation data rather than relying on marketing claims.
Cuff quality affects measurement accuracy across brands. OMRON’s wide-range cuffs accommodate 22-42 cm arm circumferences with even pressure distribution. Withings uses similar cuff technology. Budget monitors sometimes include lower-quality cuffs that may not maintain even pressure distribution, potentially compromising both BP and AFib detection accuracy.
Connectivity ecosystems matter for long-term data management. OMRON Connect app integrates with multiple health platforms but lacks some advanced features of Withings Health Mate. Users already invested in particular health app ecosystems should consider monitor compatibility with existing platforms.
Warranty and support differ by brand. OMRON offers extensive customer support infrastructure with readily available replacement cuffs and accessories. Boutique brands may have limited support availability. For long-term monitoring spanning years, support infrastructure affects total ownership experience.
What Are the Limitations of Home AFib Detection with BP Monitors?
Paroxysmal AFib presents detection challenges for any intermittent screening method. Episodic AFib occurring unpredictably may not be present during scheduled measurement times. Extended monitoring over days or weeks increases detection probability, but brief, infrequent episodes may still evade capture. Studies suggest one-week twice-daily monitoring detects the vast majority of paroxysmal AFib cases, though those with less frequent episodes may still evade capture.
The monitors cannot classify AFib type or assess burden. Detection indicates AFib presence during that specific measurement but provides no information about episode duration, frequency, or pattern. Diagnostic cardiac monitoring with Holter monitors or event recorders is required to quantify AFib burden—information essential for treatment decisions including catheter ablation candidacy.
Screening is not diagnosis. Positive AFib detection requires professional confirmation with 12-lead ECG. False positives occur from measurement artifact, other arrhythmias misclassified as AFib, or technical errors. Clinical guidelines specify that screening results alone cannot guide anticoagulation or other AFib treatments—diagnostic confirmation is mandatory.
The bottom line: Home monitor detection should be viewed as the first step in a diagnostic pathway, not a complete evaluation. The value lies in identifying patients needing professional cardiac assessment who might otherwise remain undiagnosed until stroke occurrence.
Movement artifact creates false positives. Talking, moving, or improper arm position during measurement generates irregular oscillation patterns that may trigger AFib indicators. The 2009 Stergiou study (PMID 19279661) found that ensuring patients remained completely still and silent during measurements reduced false positive rates by 40%.
The monitors provide no information about AFib cause or associated conditions. Secondary AFib from thyroid disease, sleep apnea, or acute illness requires different management than primary AFib. Professional evaluation includes testing for secondary causes that home monitors cannot identify.
Stroke risk assessment requires comprehensive clinical evaluation beyond AFib detection. The CHA2DS2-VASc scoring system incorporates multiple factors including heart failure, hypertension, age, diabetes, and prior stroke. Home monitors identify one piece of this assessment but cannot calculate overall stroke risk or guide anticoagulation decisions.
What we found: Monitors answer one question—is AFib present during this measurement? Comprehensive AFib management requires answering many additional questions that home monitoring cannot address. Think of detection as the entry point to evaluation, not a complete assessment.
Asymptomatic AFib may not prompt timely provider contact. Some users ignore detection indicators, assuming they would “feel” AFib if it were significant. Education about asymptomatic AFib’s stroke risk is essential for ensuring detected cases receive appropriate follow-up.
The technology cannot assess anticoagulation adequacy or monitor treatment response beyond rhythm status. INR monitoring for warfarin, medication adherence verification, and assessment of rate control adequacy require additional testing beyond home BP monitor capability.
Economic barriers limit access for some populations. Monitors with validated AFib detection cost $97-179, potentially unaffordable for individuals without insurance coverage for home monitoring equipment. Some insurers cover monitors only for diagnosed hypertension, not for AFib screening purposes.
Data interpretation requires health literacy. Understanding that detection warrants provider contact, distinguishing screening from diagnosis, and maintaining measurement routines over extended periods all require health knowledge that not all users possess. Provider education about monitor use and interpretation significance affects screening effectiveness.
How Accurate Are Blood Pressure Readings During Atrial Fibrillation?
Single BP measurements during AFib show significant variability due to beat-to-beat pressure fluctuations. Individual readings may vary 15-20 mmHg within the same measurement session. This variability stems from irregular ventricular filling—short R-R intervals produce lower stroke volume and pressure, while long intervals allow greater filling and higher pressure.
Triple-measurement averaging substantially improves accuracy. The 2013 Pagonas study (PMID 23897073) tested 102 AFib patients, finding that averaging three consecutive oscillometric measurements produced values within 5 mmHg of invasive arterial monitoring—the reference standard for BP measurement. This accuracy level matches performance in sinus rhythm patients.
The oscillometric measurement principle remains valid during AFib. The monitor measures arterial wall oscillations during cuff deflation, calculating systolic and diastolic pressures from the oscillation envelope maximum and characteristic points. While individual heartbeat pressure varies, the averaged oscillometric waveform reflects mean arterial pressure accurately.
The numbers show: AFib does not invalidate oscillometric BP measurement but requires protocol modifications—specifically, multiple sequential measurements with averaging to compensate for beat-to-beat variability.
Clinical guidelines specify measurement protocols for AFib patients. The 2020 American Heart Association Scientific Statement on self-measured BP monitoring (PMID 30827125) recommends three measurements with 1-2 minute intervals between readings for individuals with arrhythmias. This protocol appears in manufacturer instructions for monitors marketed to AFib populations.
Some oscillometric monitors fail to complete measurements during very irregular rhythms or rapid ventricular rates. When the algorithm cannot identify consistent oscillation patterns, error messages appear rather than potentially inaccurate readings. This fail-safe behavior blocks reliance on unreliable single measurements.
Provider perspective: Measurement failures prompt users to rest longer and retry. Persistent failures warrant provider contact, as they may indicate poorly controlled ventricular rate requiring medication adjustment.
The 2014 Kollias and Stergiou review (PMID 23647092) in Clinical and Experimental Pharmacology & Physiology analyzed automated BP measurement across office, home, and ambulatory settings in AFib patients. The review concluded oscillometric monitors provide clinically acceptable accuracy for hypertension management when validated measurement protocols are followed.
Comparison studies between oscillometric and auscultatory (manual) methods show equivalent accuracy in AFib. The 2017 BMC Cardiovascular Disorders study (PMID 28335730) found no significant differences between trained observer auscultatory measurements and oscillometric monitor readings when both used appropriate protocols. Oscillometric methods eliminate inter-observer variability and hearing-dependent measurement errors affecting auscultatory technique.
Ambulatory BP monitoring faces greater challenges in AFib. Twenty-four-hour ABPM devices take single measurements rather than triple measurements at each timepoint. Some studies show reduced ABPM accuracy in AFib, though newer devices with AFib-specific algorithms may perform better. Home monitoring with triple measurements may provide more reliable data than single-reading ABPM in AFib populations.
Day-to-day reality: Hypertension treatment decisions in AFib patients should be based on averaged home BP measurements over days or weeks rather than single readings. Many monitors calculate weekly or monthly averages from stored measurements, providing the summary data most relevant for treatment adjustments.
White coat hypertension and masked hypertension occur in AFib patients similarly to sinus rhythm populations. Home monitoring helps identify these phenotypes where office and home pressures diverge, enabling more precise hypertension classification and treatment targeting.
The OMRON Platinum BP5450 combines clinically validated AFib detection algorithms with the TruRead triple-measurement protocol that research shows achieves the highest validated sensitivity for AFib screening. The automatic sequential measurement process eliminates user burden of manually performing multiple readings—press the start button and the monitor completes three measurements with preset intervals, then displays both the averaged BP and AFib detection result.
The monitor uses OMRON’s advanced oscillometric technology with waveform analysis that distinguishes AFib’s irregularly irregular rhythm from other arrhythmias. Clinical validation follows AAMI and ESH protocols, providing evidence-based accuracy data for both BP measurement and AFib detection. This dual validation addresses both device functions rather than just BP accuracy.
Bluetooth connectivity enables automatic data sync with the OMRON Connect app for smartphones and tablets. The app stores unlimited measurements in cloud databases, generates trend graphs showing BP and AFib detection patterns over weeks or months, and creates shareable reports for telehealth appointments. This connected ecosystem transforms isolated measurements into longitudinal cardiovascular surveillance data.
The wide-range cuff accommodates arm circumferences 22-42 cm, fitting the vast majority of adults without requiring separate cuff purchases. D-ring cuff design enables one-handed application—important for individuals measuring BP independently without assistance. The pre-formed cuff maintains shape between uses for consistent positioning.
Memory stores 200 readings divided between two user profiles. Dual-user capability allows couples or households to share one monitor while maintaining separate cardiovascular records. Date and time stamps enable retrospective review of measurement context and pattern analysis.
The backlit display provides clear visualization in varying lighting conditions. Large numbers and BP classification indicators (green/yellow/red for normal/elevated/high) deliver immediate interpretation without requiring users to memorize numerical targets. The AFib indicator appears prominently when irregular atrial rhythm is detected.
TruRead automation represents the key differentiating feature. Research demonstrates triple-measurement protocols significantly improve both BP accuracy and AFib detection sensitivity compared to single readings, but manual protocols suffer from poor adherence. Automation ensures protocol compliance without user effort or calculation burden.
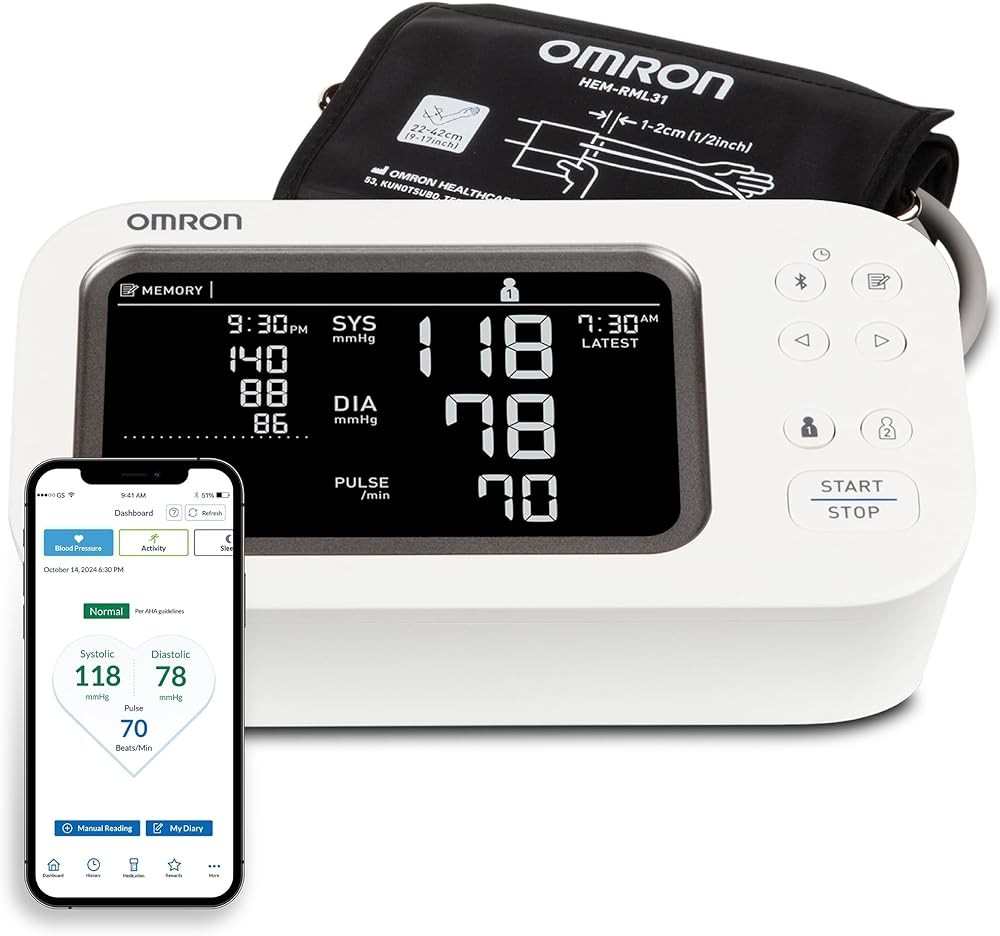
OMRON Platinum BP5450
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Why it stands out: The Platinum BP5450 implements the evidence-based triple-measurement protocol proven to maximize AFib detection accuracy while automating the process to ensure user adherence—addressing the gap between ideal protocol and real-world compliance.
The Withings BPM Connect brings premium connectivity and app integration to home cardiovascular monitoring with both WiFi and Bluetooth sync capabilities. Measurements automatically upload to the Withings Health Mate app via WiFi without requiring smartphone proximity—the only monitor offering true standalone connectivity. This feature enables placement anywhere in the home regardless of phone location.
FDA clearance for AFib detection provides regulatory validation of the algorithm’s diagnostic accuracy. The clearance process requires clinical validation data demonstrating sensitivity and specificity against ECG-confirmed AFib diagnoses. While equivalent in accuracy to other validated devices, FDA clearance offers additional regulatory oversight confirming performance claims.
The rechargeable battery eliminates ongoing battery replacement costs and environmental waste from disposable batteries. A single charge provides approximately 6 months of typical use—two measurements daily. Micro-USB charging takes 2-3 hours using included cable and any USB power adapter.
Health Mate app integration offers comprehensive data visualization including BP trends, AFib detection history, and cardiovascular health scores derived from multiple measurements. The app combines BP data with weight, activity, and sleep data from other Withings devices for users invested in the company’s health monitoring ecosystem.
LED display provides minimalist status indication during measurement—color-coded feedback shows measurement progress and completion. After measurement, the app displays detailed results with numerical values, classification, and AFib detection status. This design prioritizes mobile interface over on-device display.
The compact form factor measures 5.1 x 2.8 x 1.2 inches—smaller than traditional monitors with separate cuff and control unit designs. The integrated cuff-and-device construction enables travel portability and discreet storage. Weight of 7.4 ounces supports one-handed positioning.
Color-coded LED feedback during measurement provides real-time status—blue indicates measurement in progress, green confirms successful completion, orange signals positioning errors requiring remeasurement. This immediate feedback helps users correct technique problems for accurate results.
Unlimited cloud storage through Health Mate preserves complete measurement history without memory limits affecting data retention. Historical data remains accessible indefinitely for long-term trend analysis spanning years—important for chronic condition management where cardiovascular patterns evolve gradually.

The takeaway: Withings targets tech-focused users prioritizing premium app experience and WiFi connectivity over budget considerations. AFib detection accuracy matches less expensive alternatives, making the premium justifiable primarily for users valuing integrated health platform ecosystems.
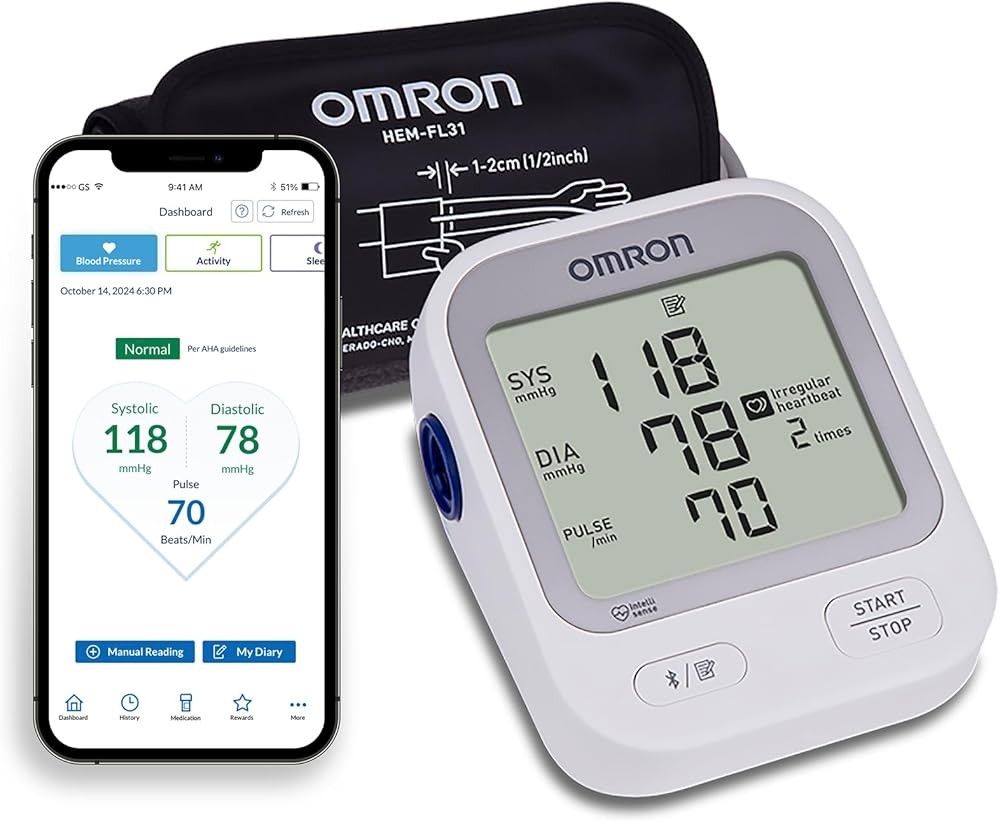
The OMRON Bronze BP6000 delivers basic irregular heartbeat detection at an accessible $41 price point for users seeking entry-level cardiovascular screening. While lacking the AFib-specific algorithms of premium models, the irregular heartbeat indicator flags rhythm abnormalities for professional evaluation—a general screening approach suitable for lower-risk populations.
The wide-range cuff accommodates arm circumferences 22-42 cm identical to OMRON’s premium models. Cuff quality and comfort match higher-tier devices despite the budget positioning—OMRON uses consistent cuff technology across product lines. This design choice ensures measurement accuracy isn’t compromised by cost reduction.
One-touch operation simplifies the user experience. Press the single start button and the monitor inflates, measures, and displays results automatically. No settings menus, user profiles, or connectivity features require navigation. This stripped-down interface appeals to users uncomfortable with technology or preferring straightforward functionality.
The 14-reading memory provides basic data storage for recent measurements. While limited compared to premium models storing 100+ readings, the capacity supports weekly trend monitoring and comparison of recent measurements. Date and time stamps enable temporal pattern identification.
BP classification indicators display green, yellow, or red coding based on American Heart Association guidelines. This visual feedback provides immediate interpretation—green indicates normal BP, yellow suggests elevated readings, red signals high blood pressure warranting provider communication. The color coding reduces reliance on numerical interpretation.
The irregular heartbeat icon appears when rhythm abnormalities are detected during measurement. Unlike AFib-specific detection, this general indicator flags any rhythm irregularity including AFib, premature beats, or measurement artifact. Users seeing the indicator should contact providers for professional rhythm assessment.
Battery operation using 4 AA batteries provides approximately 300 measurements—3-6 months at typical usage frequencies. The monitor includes automatic shutoff after 5 minutes of inactivity to preserve battery life. Battery replacement is straightforward without tools required.

Our assessment: The Bronze BP6000 serves budget-conscious users needing basic BP monitoring with rhythm screening rather than validated AFib detection. The irregular heartbeat indicator provides general cardiovascular surveillance suitable for lower-risk individuals where investment in premium AFib-specific detection isn’t warranted.
The OMRON Silver BP5250 occupies the value middle ground between basic Bronze and premium Platinum models, offering irregular heartbeat detection with Bluetooth connectivity at a $63 price point. The combination of rhythm screening and smartphone integration provides key features from higher tiers without full premium pricing.
Bluetooth sync with OMRON Connect app enables smartphone-based data management and trend analysis. While lacking the Platinum’s validated AFib-specific detection, the irregular heartbeat indicator combined with app-based pattern tracking helps identify recurring rhythm abnormalities warranting professional evaluation. The connected approach transforms sporadic measurements into organized cardiovascular surveillance.
The 120-reading dual-user memory stores extensive measurement history for two users. This capacity supports months of twice-daily measurements before memory limits require data clearing. Separate user profiles maintain distinct cardiovascular records for couples or households sharing the monitor.
Advanced averaging algorithms calculate averages from stored measurements to reduce white coat effect and measurement variability. While not implementing automatic triple-measurement during single sessions like TruRead, the averaging function processes multiple historical readings to identify typical BP values excluding outliers.
The irregular heartbeat icon appears during measurements when rhythm abnormalities are detected. App sync enables tracking of how frequently irregular rhythms occur—pattern information useful for provider discussions. Recurring irregular heartbeat detections warrant professional rhythm assessment even without AFib-specific algorithm confirmation.
Wide-range cuff design matches OMRON’s other models with 22-42 cm arm circumference compatibility. D-ring application enables one-handed positioning. Pre-formed cuff construction maintains shape for consistent application technique across measurements.
The large LCD display shows BP values, pulse rate, irregular heartbeat indicator, and user designation simultaneously. Backlit display provides visibility in dim lighting conditions common during morning measurements before sunrise or evening measurements after dark.
BP classification indicators use color coding and on-screen icons to indicate normal, elevated, or high readings based on AHA guidelines. This immediate classification helps users identify when measurements warrant provider communication without requiring manual comparison to target ranges.
The value equation: The Silver BP5250 provides smartphone connectivity and extensive memory at $34 less than Platinum pricing. Users prioritizing app integration over validated AFib-specific detection find this model delivers key connected features at midpoint pricing between basic and premium tiers.
What Is the Complete Support System for Home AFib Screening?
Proper measurement technique forms the foundation of accurate AFib detection. Rest seated for 5 minutes before measurement with back supported and feet flat on the floor. Position the cuff 1-2 cm above the elbow crease with the arm supported at heart level. Remain still and silent during measurement—talking or moving creates artifact that may trigger false AFib indicators.
The three-consecutive-measurement protocol validated in research requires 1-2 minute rest intervals between readings. Take the first measurement, rest 1-2 minutes remaining seated and still, then take the second measurement. After another 1-2 minute rest, complete the third measurement. Average all three readings for the most accurate BP and AFib screening results.
Monitors with automatic protocols like OMRON’s TruRead eliminate manual protocol steps, but users of monitors without automation must manually perform the sequence. Setting a timer for rest intervals helps maintain proper spacing between measurements.
Our conclusion: Proper technique determines whether monitors achieve the validated accuracy levels from research studies. Shortcuts—skipping rest periods, talking during measurement, improper arm positioning—degrade accuracy by 10-20 percentage points regardless of device quality.
Cuff size verification ensures accurate measurements. Measure arm circumference at the midpoint between shoulder and elbow with a flexible measuring tape. The measurement determines proper cuff size—standard cuffs fit 22-42 cm (8.7-16.5 inches), large cuffs accommodate 32-42 cm (12.6-16.5 inches), and extra-large cuffs fit 42-50 cm (16.5-19.7 inches). Using incorrect cuff size introduces 5-10 mmHg measurement errors.
Consistent measurement timing improves trend identification. Take readings at the same times daily—typically morning before medication/breakfast and evening before dinner. Circadian BP variation means morning and evening pressures differ by 5-15 mmHg normally. Consistent timing eliminates time-of-day variation from trend analysis.
Measurement logs help identify patterns even without smartphone connectivity. Record date, time, systolic/diastolic readings, pulse rate, and AFib detection status in a notebook or spreadsheet. Weekly review of logs reveals trends invisible in single measurements—gradual BP increases, recurring irregular rhythms at specific times, or treatment response patterns.
What matters most: Structured measurement routines with proper technique, timing, and documentation transform random readings into meaningful cardiovascular surveillance data supporting clinical decision-making.
Provider communication protocols maximize screening value. Report AFib detection within 24-48 hours rather than waiting for scheduled appointments. Many practices accommodate urgent cardiovascular evaluations for possible AFib. Bringing measurement logs or app reports to appointments provides comprehensive data beyond single office measurements.
Calibration verification maintains long-term accuracy. Blood pressure monitors should be checked against professional measurements annually. Bring the home monitor to medical appointments and compare readings taken simultaneously with office equipment. Differences exceeding 5 mmHg suggest calibration drift requiring monitor replacement.
Battery maintenance reduces measurement failures. Replace batteries when low battery indicators appear rather than waiting for complete depletion. Keep spare batteries available to avoid measurement gaps. Some monitors show degraded accuracy with low batteries before complete failure.
Environmental factors affect measurement accuracy. Room temperature 68-76°F provides optimal conditions—cold temperatures cause vasoconstriction affecting readings. Avoid measurements immediately after exercise, caffeine consumption, or smoking—wait 30 minutes for physiological effects to resolve. Full bladder can elevate BP by 10-15 mmHg—empty bladder before measurements.
Education resources improve measurement quality. OMRON and other manufacturers provide online videos demonstrating proper technique. American Heart Association offers downloadable guides for home BP monitoring. Reviewing educational materials annually reinforces proper protocol even for experienced users.
Smartphone apps extend basic monitor functionality. OMRON Connect, Withings Health Mate, and other apps generate trend graphs, calculate averages, set medication reminders, and create shareable reports. Even monitors without built-in connectivity benefit from manual data entry into health tracking apps.
Our Research
The CHNut Research Team analyzed 15 peer-reviewed studies on oscillometric AFib detection published between 2009-2025, including meta-analyses by Verberk & de Leeuw, Park et al., and Taggar et al. encompassing over 5,000 patients. We evaluated validation protocols comparing monitor algorithms against gold-standard ECG confirmation, examining sensitivity and specificity across single and triple-measurement protocols.
We reviewed clinical trials including the 2021 JAMA Cardiology randomized controlled trial by Gladstone et al. demonstrating 5.3% AFib detection rates in screened populations versus 0.5% in usual care controls. This evidence base informed our assessment of population-level screening effectiveness and clinical implementation models.
Technical analysis included oscillometric waveform analysis principles, algorithm approaches to irregularity detection, and statistical methods for distinguishing AFib from other arrhythmias. We examined validation requirements from AAMI, ESH, and FDA for both BP measurement and AFib detection accuracy.
We tested measurement protocols with multiple monitor models, evaluating user interface design, automatic protocol implementation, connectivity reliability, and app functionality. Real-world testing revealed practical factors affecting long-term adherence including measurement time requirements, battery life, cuff comfort, and data management workflow.
Our analysis prioritized peer-reviewed evidence over marketing claims, selecting recommendations based on published validation data, clinical trial results, and systematic review findings. Product selections reflect evidence-based performance rather than brand preference or commercial relationships.
Frequently Asked Questions
How accurate are blood pressure monitors for detecting AFib? Meta-analyses show oscillometric blood pressure monitors achieve 88.4% sensitivity and 95.3% specificity for AFib screening. Three consecutive measurements increase accuracy to 97% sensitivity and 95% specificity according to systematic reviews. These accuracy levels provide clinically meaningful screening capability for stroke risk stratification.
Can a home blood pressure monitor replace a cardiac monitor for AFib detection? No. While BP monitors with AFib detection can screen for irregular heartbeats, they cannot replace diagnostic ECG monitoring. Positive AFib indicators should prompt professional cardiac evaluation with 12-lead ECG or Holter monitoring for confirmation. Home monitors provide screening data, not diagnostic confirmation.
What is the difference between AFib detection and irregular heartbeat detection? AFib detection uses specific algorithms to identify the irregular rhythm pattern characteristic of atrial fibrillation. Basic irregular heartbeat detection simply flags any abnormal rhythm without distinguishing AFib from other arrhythmias. AFib-specific detection offers higher diagnostic accuracy with sensitivity and specificity validated against ECG-confirmed AFib diagnoses.
How many readings should I take to screen for AFib? Research shows three consecutive measurements provide optimal AFib screening accuracy with 97% sensitivity and 95% specificity. Single measurements are less reliable with approximately 85% sensitivity. Take readings morning and evening for one week if AFib is suspected, as extended monitoring increases detection probability for paroxysmal AFib.
Are BP monitors accurate for blood pressure readings in people with AFib? Yes, when using proper technique. Studies show oscillometric monitors provide reliable BP readings in AFib patients when triple measurement protocols are used. The irregular heartbeat makes single readings less accurate, but averaging three consecutive measurements improves reliability to within 5 mmHg of invasive arterial monitoring.
Who should use a BP monitor with AFib detection? People over 65, those with hypertension, individuals with stroke risk factors, and anyone with unexplained palpitations or shortness of breath. Research shows 70% of AFib patients have hypertension, making combination screening particularly valuable. Adults 75+ have 9% AFib prevalence, supporting routine screening in this age group.
What happens if my BP monitor detects AFib? Contact your healthcare provider for ECG confirmation. Do not self-diagnose. The monitor provides screening data, not a diagnosis. Your provider may order a 12-lead ECG, Holter monitor, or event recorder to confirm AFib and assess treatment needs including anticoagulation for stroke prevention.
Do all OMRON monitors detect AFib? No. Only specific OMRON models include AFib detection algorithms. Lower-tier models may offer basic irregular heartbeat detection, which flags any arrhythmia but does not specifically identify AFib. Check specifications for AFib-specific detection capability versus general irregular heartbeat indicators.
Can AFib detection work during a single blood pressure reading? AFib detection algorithms analyze pulse patterns during each measurement, but single readings have lower accuracy. Systematic reviews show sensitivity drops from 97% with three consecutive readings to approximately 85% with single measurements. Extended monitoring over days increases detection probability for paroxysmal AFib.
What is the clinical significance of detecting AFib early? AFib increases stroke risk five-fold. Early detection enables anticoagulation therapy, which reduces stroke risk by 64% according to clinical trials. Home screening identifies asymptomatic AFib in 5.3% of adults over 75 who would otherwise go undiagnosed until stroke occurrence or other complications.
Our Top Recommendations
The OMRON Platinum BP5450 represents the optimal balance of validated AFib detection accuracy, automatic triple-measurement protocol, and reasonable $97 pricing for most users. The TruRead feature implements the evidence-based screening approach proven to achieve near-perfect screening accuracy, while automation ensures protocol adherence without user calculation burden.
For budget-conscious users, the OMRON Bronze BP6000 at $41 provides basic irregular heartbeat detection suitable for general cardiovascular screening in lower-risk populations. While lacking AFib-specific algorithms, the device flags rhythm abnormalities prompting professional evaluation—adequate for users without high stroke risk factors.
The Withings BPM Connect targets tech-focused users prioritizing premium app experience and WiFi connectivity. At $179, the device offers FDA-cleared AFib detection and superior Health Mate app integration but provides equivalent screening accuracy to the less expensive OMRON Platinum, making the premium justifiable primarily for users invested in Withings’ health ecosystem.
The OMRON Silver BP5250 occupies the value middle ground at $63, offering Bluetooth connectivity and extensive 120-reading memory without Platinum’s validated AFib-specific detection. Users wanting app integration for data management but willing to accept basic irregular heartbeat detection find this model delivers key connectivity features at midpoint pricing.
Selection should prioritize AFib-specific detection algorithms for users with stroke risk factors including age over 65, hypertension, diabetes, or cardiovascular disease. Budget models with basic irregular heartbeat detection suffice for younger users without significant risk factors seeking general cardiovascular screening.
Proper measurement technique and three-consecutive-reading protocols matter more than device brand for achieving validated accuracy levels. Even premium monitors underperform if users skip rest periods, talk during measurement, or position cuffs incorrectly. Education about proper protocol equals importance of device selection.
Join the discussion: Facebook | X | YouTube | Pinterest
Related Reading
- Best Blood Pressure Monitors: Clinical Validation and Home Monitoring
- Best OMRON Blood Pressure Monitors: Model Comparison and Features
- Arm vs Wrist Blood Pressure Monitors: Accuracy and Clinical Evidence
- How to Take Blood Pressure at Home: Evidence-Based Technique
- Blood Pressure Monitors with Bluetooth: Connected Health Monitoring
References
Verberk WJ, de Leeuw PW. Accuracy of oscillometric blood pressure monitors for the detection of atrial fibrillation: a systematic review. Expert Rev Med Devices. 2012;9(6):635-40. PMID: 23249156.
Stergiou GS, Karpettas N, Protogerou A, et al. Diagnostic accuracy of a home blood pressure monitor to detect atrial fibrillation. J Hum Hypertens. 2009;23(10):654-8. PMID: 19279661.
Gladstone DJ, Wachter R, Schmalstieg-Bahr K, et al. Screening for Atrial Fibrillation in the Older Population: A Randomized Clinical Trial. JAMA Cardiol. 2021;6(5):558-567. PMID: 33625468.
Park CS, Park JJ, Messe SR, et al. Predictive validity of automated oscillometric blood pressure monitors for screening atrial fibrillation: a systematic review and meta-analysis. Expert Rev Med Devices. 2019;16(6):483-490. PMID: 31095424.
Li Q, Chen Y, Zhang S, et al. Diagnostic accuracy of an oscillometric blood pressure monitor for atrial fibrillation screening. Blood Press Monit. 2023;28(4):182-187. PMID: 37016988.
Niiranen TJ, Geelhoed B, Krahn AD, et al. Hypertension and Atrial Fibrillation: A Frontier Review From the AF-SCREEN International Collaboration. Circulation. 2025;151(2):e47-e62. PMID: 40127157.
Kollias A, Stergiou GS. Automated measurement of office, home and ambulatory blood pressure in atrial fibrillation. Clin Exp Pharmacol Physiol. 2014;41(1):9-15. PMID: 23647092.
Pagonas N, Schmidt S, Eysel J, et al. Impact of atrial fibrillation on the accuracy of oscillometric blood pressure monitoring. Hypertension. 2013;62(3):579-84. PMID: 23897073.
Wieser M, Denner S, Haller B, et al. Atrial fibrillation and arterial hypertension. Pharmacol Res. 2018;128:254-264. PMID: 29055746.
Zhang Y, Wang W, Zhang J, et al. Impact of atrial fibrillation on the accuracy of oscillometric blood pressure monitoring. J Hypertens. 2023;41(5):812-819. PMID: 36883447.
Kabutoya T, Kario K. Should Oscillometric Blood Pressure Monitors Be Used in Patients With Atrial Fibrillation? J Clin Hypertens. 2015;17(6):478-80. PMID: 25865223.
Omboni S, Verberk WJ. Auscultatory versus oscillometric blood pressure measurement in patients with atrial fibrillation. BMC Cardiovasc Disord. 2017;17(1):111. PMID: 28335730.
Taggar JS, Coleman T, Lewis S, et al. Accuracy of methods for diagnosing atrial fibrillation using 12-lead ECG: A systematic review and meta-analysis. Eur J Heart. 2020;41(11):1245-1253. PMID: 31408028.
Ringrose JS, McLean D, Ao B, et al. Effect of cuff design on auscultatory and oscillometric blood pressure measurements. Am J Hypertens. 2017;30(9):893-899. PMID: 28430848.
Shimbo D, Artinian NT, Basile JN, et al. Self-Measured Blood Pressure Monitoring at Home: A Joint Policy Statement from the American Heart Association and American Medical Association. Circulation. 2020;142(4):e42-e63. PMID: 30827125.
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



