How to Take Blood Pressure at Home: The Complete Self-Monitoring Guide
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Research shows that 69% of home blood pressure devices tested on actual users produced measurement errors greater than 5 mmHg, making proper technique critical for cardiovascular health management. The OMRON Platinum BP5450 at $97 delivers the most accurate home monitoring through validated oscillometric technology with TruRead triple-reading averaging, AFib detection, and a wide-range 22-42 cm cuff that eliminates miscuffing errors across arm sizes. Published studies in Circulation demonstrate that validated devices paired with AHA-recommended positioning reduce measurement variability from 10-15 mmHg to under 3 mmHg when users follow the 5-minute rest protocol with arm supported at heart level. The OMRON Iron BP7000 at $37 provides reliable budget monitoring with the same essential accuracy features. Here’s what the published research shows about mastering home blood pressure technique for cardiovascular protection.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
Home blood pressure monitoring provides cardiovascular risk prediction superior to office measurements when performed with proper technique. A 2019 American Heart Association scientific statement published in Circulation established that self-measured readings correlate more closely with ambulatory monitoring and cardiovascular outcomes than clinic measurements, yet technique errors remain the primary source of measurement variability in home settings1. The difference between accurate and inaccurate home monitoring often determines whether hypertension is detected early or complications develop silently.
Understanding proper blood pressure measurement technique transforms home monitoring from potentially misleading numbers into reliable cardiovascular health data. Research demonstrates that positioning errors alone can alter readings by 10-15 mmHg, while cuff size mistakes create systematic errors of 5-15 mmHg that persist across all measurements2. These technique-related errors exceed the accuracy specifications of even the most precisely validated monitors, making user education as important as device selection.
| Feature | OMRON Platinum BP5450 | OMRON Iron BP7000 | OMRON Silver BP5250 | OMRON Gold Wrist BP4350 |
|---|---|---|---|---|
| Price | $97 | $37 | $63 | $78 |
| Measurement Site | Upper Arm | Upper Arm | Upper Arm | Wrist |
| Validation | AAMI/ESH/BHS | AAMI/ESH | AAMI/ESH | AAMI/ESH |
| TruRead Averaging | Yes (3 readings) | No | No | No |
| AFib Detection | Yes | No | No | No |
| Cuff Range | 22-42 cm | 22-42 cm | 22-42 cm | 13.5-21.5 cm |
| Bluetooth | Yes | No | Yes | Yes |
| Positioning Sensor | No | No | No | Yes |
| Memory Capacity | 200 readings | 60 readings | 120 readings (dual) | 100 readings |
| Best For | Complete monitoring | Essential accuracy | Value features | Travel/portability |
Why Does Proper Blood Pressure Technique Matter for Health Outcomes?
Home blood pressure monitoring accuracy directly influences cardiovascular treatment decisions that affect long-term health outcomes. A landmark 2005 AHA scientific statement established that home readings predict cardiovascular events more reliably than office measurements, specifically because the large number of readings obtained over time provides better representation of true blood pressure status than occasional clinic visits2. However, this predictive advantage disappears when measurement technique introduces systematic errors that skew the data.
The clinical significance of technique-related measurement errors becomes clear when examining hypertension diagnosis thresholds. The current definition of elevated blood pressure starts at 120/80 mmHg, with stage 1 hypertension beginning at 130/80 mmHg. A 5 mmHg measurement error from improper cuff size or 10 mmHg error from poor positioning can shift readings across these diagnostic categories, potentially leading to either unnecessary medication or missed diagnosis1.
Research published in the Journal of Clinical Hypertension demonstrates that memory-equipped automatic monitors reduce observer bias and avoid patient misreporting compared to manual recording, but only when users understand proper measurement conditions3. The monitors themselves cannot compensate for technique errors like talking during measurement, crossed legs, or unsupported arms, all of which create reproducible elevation in readings that users may mistake for actual hypertension.
Studies examining real-world home monitoring accuracy reveal concerning patterns. When researchers tested home blood pressure devices on their actual owners rather than in controlled laboratory conditions, 69% showed errors greater than 5 mmHg compared to reference measurements4. While some of this inaccuracy stems from device limitations, investigation of measurement technique revealed that positioning errors, improper rest periods, and cuff placement mistakes contributed substantially to the observed discrepancies.
The cardiovascular health implications extend beyond diagnosis to treatment monitoring. Patients already on hypertension medications rely on home monitoring to assess treatment effectiveness and guide medication adjustments. Technique errors that consistently overestimate pressure may lead to medication increases that create excessive blood pressure lowering, while underestimation errors might leave hypertension inadequately addressed despite apparent control on home readings.
Blood pressure variability itself carries prognostic significance beyond average pressure levels. Research demonstrates that visit-to-visit variability predicts cardiovascular events independently of mean blood pressure1. Proper home monitoring technique that minimizes measurement-related variability allows better assessment of true biological blood pressure fluctuation, providing clinically useful data about cardiovascular risk profiles.
The distinction between white-coat hypertension and masked hypertension illustrates why accurate home measurement technique matters diagnostically. White-coat hypertension produces elevated office readings but normal home readings, while masked hypertension shows normal office but elevated home measurements. Studies indicate that self-measurement proves particularly helpful for detecting white-coat effects in patients on treatment5. However, these diagnostic patterns only emerge reliably when home measurements reflect true blood pressure rather than technique artifacts.
Morning blood pressure surge represents another clinically important phenomenon that home monitoring can detect. Morning readings tend to run higher than evening measurements, and exaggerated morning surges correlate with increased cardiovascular risk as documented in Japanese Society of Hypertension guidelines6. Proper morning measurement technique before medications or breakfast provides data about this risk marker that office visits cannot capture.
Bottom line: Technique errors of 5-15 mmHg can shift readings across diagnostic thresholds, potentially leading to inappropriate treatment decisions or missed hypertension diagnosis.
What Are the Essential Steps for Accurate Home Blood Pressure Measurement?
Published AHA guidelines establish a detailed measurement protocol that minimizes technique-related variability and ensures readings reflect true cardiovascular status. Published guidelines from the AHA Council on High Blood Pressure Research specify each critical element of proper measurement technique12.
The preparation phase begins 30 minutes before measurement. Avoid caffeine consumption, exercise, and smoking during this period, as all three activities acutely elevate blood pressure through different mechanisms. Caffeine stimulates sympathetic nervous system activity, exercise increases cardiac output and vascular resistance temporarily, and smoking causes immediate vasoconstriction that persists for 20-30 minutes. Empty your bladder before measuring, since a full bladder can raise readings by 10-15 mmHg through reflex sympathetic activation.
The 5-minute rest period represents the most critical pre-measurement step. Sit quietly in a chair with your back supported and feet flat on the floor during this entire rest period. Cross-legged sitting or dangling feet create muscle tension that elevates readings. Keep your arm supported on a flat surface at heart level throughout the rest period, allowing vascular tone to stabilize. Research demonstrates that skipping or shortening this rest period produces readings 5-10 mmHg higher than properly rested measurements1.
Avoid talking during both the rest period and measurement itself. Conversation activates the sympathetic nervous system and raises blood pressure through increased mental engagement. Studies show that talking during measurement can elevate readings by 10-17 mmHg systolic, creating spuriously high measurements that users might mistake for actual hypertension2.
Position the cuff correctly on bare skin approximately one inch above the elbow crease. The bladder inside the cuff should center over the brachial artery on the inner side of your upper arm. Most cuffs include markings showing proper tubing position to ensure bladder alignment. Wrapping the cuff over clothing creates additional layers that interfere with pressure transmission, potentially requiring higher inflation pressures and creating measurement artifacts.
Tighten the cuff snugly but not excessively. You should be able to slip two fingers between the cuff and your arm. Overly tight wrapping can cause discomfort and create artificially elevated readings, while loose wrapping allows the cuff to shift position during inflation and interfere with accurate pressure sensing.
Keep your arm supported at heart level throughout the measurement. The midpoint of the cuff should align with the level of your heart, typically about mid-chest height when sitting. An unsupported arm or arm held above heart level can lower readings, while an arm below heart level increases measurements. Research shows that arm position errors create systematic changes of approximately 2 mmHg for each inch of vertical displacement from heart level2.
Remain still and quiet while the cuff inflates and deflates. Movement and muscle tension alter blood flow patterns and create measurement artifacts. Breathe normally rather than holding your breath, as breath-holding increases intrathoracic pressure and temporarily affects blood pressure readings.
Key takeaway: Following AHA positioning protocol (5-minute seated rest, back and arm supported, arm at heart level, no talking) reduces measurement errors from 10-15 mmHg to under 3 mmHg with validated devices.
How Many Readings Should You Take and When?
Current AHA guidelines recommend taking 2-3 readings at each measurement session, with readings spaced one minute apart. Average the readings to obtain your blood pressure value for that session. The first reading often runs higher than subsequent measurements due to incomplete relaxation or startle response to cuff inflation. If the first reading is significantly higher than the second and third readings (more than 5 mmHg difference), discard it and average only the later measurements1.
This multiple-reading protocol reduces measurement variability substantially compared to single readings. Research examining self-measurement reproducibility demonstrates that averaging 2-3 readings provides high reliability equivalent to much larger numbers of readings, while a single measurement shows considerably more variability5. The one-minute spacing allows blood flow to normalize between measurements without extending the session to impractical lengths.
Schedule measurement sessions twice daily for comprehensive blood pressure assessment. The AHA recommends morning measurements before taking medications or eating breakfast, and evening measurements before dinner. This twice-daily schedule captures blood pressure patterns across the circadian cycle, including the morning surge that represents a period of increased cardiovascular risk16.
Morning readings provide particularly important cardiovascular risk information. Blood pressure rises sharply upon awakening through sympathetic nervous system activation and cortisol elevation. Exaggerated morning surges correlate with increased risk of stroke and heart attack during the vulnerable early morning hours. Measuring before medications allows assessment of blood pressure control throughout the entire dosing interval rather than just at peak medication effect1.
Evening measurements complement morning data by showing blood pressure status during the second high-risk period of the day. The evening hours before dinner represent another time of increased sympathetic activity related to daily stress and activity. Some patients show adequate morning control but elevated evening readings that would remain undetected without twice-daily monitoring.
Continue this measurement schedule for at least one week when initially establishing your baseline blood pressure pattern or after medication changes. The large number of readings obtained over multiple days provides much more reliable blood pressure assessment than a few office measurements. Research demonstrates that one week of twice-daily home monitoring yields 28 readings (2 per session × 2 sessions per day × 7 days), far exceeding the typical 2-3 office measurements that might otherwise guide treatment decisions5.
Once your blood pressure stabilizes on treatment, the measurement frequency can decrease to a few times per week or as recommended by your healthcare provider. However, maintain the same rigorous technique for each measurement session to ensure data consistency. Some patients find that designated measurement days (such as Monday, Wednesday, Friday mornings and evenings) provide sufficient ongoing monitoring without creating measurement burden.
Special circumstances warrant more intensive monitoring. Measure more frequently when starting new medications, adjusting doses, or experiencing symptoms that might indicate blood pressure changes. Illness, stress, and dietary changes can all affect blood pressure temporarily, and increased measurement frequency during these periods provides useful information about blood pressure stability.
Key finding: One week of twice-daily home monitoring (28 readings) provides far more reliable blood pressure assessment than the typical 2-3 office measurements that often guide treatment decisions.
Does Cuff Size Really Affect Blood Pressure Accuracy?
Cuff size represents one of the most critical yet frequently overlooked factors in home blood pressure measurement accuracy. Research published in Circulation establishes that the cuff bladder should encircle at least 80% of the upper arm to ensure accurate pressure transmission to the brachial artery2. Using a cuff that is too small for your arm circumference creates systematic overestimation of blood pressure, while an oversized cuff may underestimate true pressure.
The magnitude of cuff size errors proves clinically significant. Studies demonstrate that miscuffing with too-small cuffs can inflate systolic readings by 5-15 mmHg and diastolic readings by 3-12 mmHg depending on the degree of size mismatch2. These errors persist consistently across all measurements when the wrong cuff size is used, creating a systematic bias that users might mistake for actual hypertension requiring treatment.
Arm circumference measurement determines appropriate cuff selection. Measure around the upper arm at the midpoint between the shoulder and elbow using a flexible tape measure. Most adults require cuffs in the standard (22-32 cm) or large (32-42 cm) range. Individuals with very thin arms may need small adult cuffs (18-22 cm), while those with arm circumferences exceeding 42 cm require extra-large or thigh cuffs to ensure adequate bladder coverage.
The bladder dimensions inside the cuff matter more than the cloth covering dimensions. Cuff manufacturers specify both the bladder length (circumference coverage) and width. The bladder length should encircle 80-100% of the arm circumference, while the bladder width should equal approximately 40% of arm circumference. These proportions ensure that pressure applied by the inflating bladder transmits evenly to underlying tissues and accurately reflects pressure in the brachial artery2.
Wide-range cuffs that accommodate arm circumferences from 22-42 cm offer practical advantages for home monitoring. These cuffs use longer bladders that fit most adult arms correctly, eliminating the need to stock multiple cuff sizes or worry about selecting the wrong size. Research on semi-rigid cuffs with tronco-conical shapes demonstrates that advanced cuff designs can provide accurate measurements over wide ranges of arm circumferences through improved tension distribution3.
Obesity creates particular cuff sizing challenges because upper arm shape changes from cylindrical to more conical as arm circumference increases. Standard cuffs may not achieve proper tension distribution on conical arms even when bladder length appears adequate. Specialized tronco-conical cuffs designed to better fit large conical arms improve measurement accuracy in obese populations3.
Seasonal clothing changes can affect effective cuff size. While measurements should always be taken on bare skin, some users attempt to measure through thin clothing. Even light fabric creates an additional layer that interferes with pressure transmission and effectively requires a larger cuff to achieve the same compression. This practice should be avoided entirely, as studies show that cuff placement over clothing creates unpredictable measurement errors2.
Children and adolescents require appropriately sized pediatric cuffs based on arm circumference. Adult cuffs significantly oversize pediatric arms and can create substantial underestimation of blood pressure in young patients. Healthcare providers should specify appropriate cuff size when recommending home monitoring for pediatric patients.
Validation studies typically specify the arm circumference range tested during device validation. Checking whether your arm circumference falls within the validated range for your specific monitor provides additional confidence in measurement accuracy. Some monitors include special algorithms that adapt to different arm sizes, but these features work best when cuff size remains appropriate3.
The evidence shows: Miscuffing with too-small cuffs creates systematic errors of 5-15 mmHg that persist across all measurements, potentially causing misdiagnosis of hypertension in individuals with normal blood pressure.
Which Arm Should You Use for Blood Pressure Measurement?
Initial blood pressure assessment should include measurements on both arms to identify any significant inter-arm differences. Take readings on each arm using the same technique and within a few minutes of each other. Differences of 10 mmHg or more between arms may indicate peripheral vascular disease or anatomical variations that warrant medical evaluation1.
Once you establish baseline pressures in both arms, use the arm with the consistently higher reading for all future measurements. This approach ensures that you monitor the higher pressure that represents greater cardiovascular risk. Studies show that blood pressure in the two arms often differs by 5-10 mmHg due to anatomical variations in arterial anatomy, and the higher reading provides more clinically relevant information about systemic pressure1.
The brachial artery anatomy influences measurement accuracy. The brachial artery runs down the inner side of the upper arm, and cuff placement that centers the bladder over this artery ensures optimal pressure transmission. Most cuffs include tubing position markers or artery indicators to guide proper placement. Aligning the tubing with the artery path (down the inner arm toward the thumb side) positions the bladder correctly2.
Arterial stiffness can create measurement challenges in some populations. Research validating blood pressure monitors in patients with chronic kidney disease demonstrates that arterial stiffness affects oscillometric measurement accuracy, yet validated devices still perform acceptably in these populations when proper technique is followed7. This finding suggests that correct positioning and cuff size matter even more when arterial compliance is reduced.
Pregnancy introduces special positioning considerations. Research examining blood pressure measurement in pregnant women shows that positioning significantly affects readings. Left lateral recumbent position produces notably lower readings than seated position in pregnancy due to reduced compression of the inferior vena cava8. Pregnant women should follow their healthcare provider’s guidance about preferred position for home monitoring, typically seated position for consistency with prenatal visit measurements.
Lymphedema or previous breast surgery with lymph node removal represents a contraindication to measuring blood pressure on the affected arm. Cuff inflation can worsen lymphedema or create discomfort in arms with compromised lymphatic drainage. Patients with bilateral lymphedema should consult their healthcare provider about alternative measurement sites or special monitoring considerations.
Arteriovenous fistulas or grafts for dialysis access absolutely contraindicate blood pressure measurement on the affected arm. Cuff compression can damage these critical vascular access sites. Dialysis patients should measure on the opposite arm or, if bilateral access exists, discuss alternative monitoring approaches with their nephrologist.
What Mistakes Cause Inaccurate Home Blood Pressure Readings?
Positioning errors represent the most common source of measurement inaccuracy in home monitoring. An unsupported arm can elevate readings by 10 mmHg or more as muscle tension increases to hold the arm in position2. Similarly, an arm positioned below heart level shows artificially elevated readings because pressure increases with vertical distance below the heart. Conversely, an arm above heart level produces falsely low readings. Studies demonstrate that each inch of vertical displacement from heart level creates approximately 2 mmHg change in measured pressure2.
Back support absence creates another frequent positioning mistake. Sitting without back support requires core muscle engagement to maintain posture, and this muscle tension elevates blood pressure through increased sympathetic nervous system activity. Research shows that unsupported sitting can raise readings by 6-10 mmHg compared to properly supported seated position1.
Crossed legs increase blood pressure readings by 2-8 mmHg through multiple mechanisms including increased venous return and muscle tension. This effect proves large enough to potentially shift readings across diagnostic thresholds. Keeping both feet flat on the floor eliminates this source of error1.
Talking during measurement represents a behavioral error that substantially affects readings. Conversation activates mental processes and sympathetic nervous system function, creating blood pressure elevations of 10-17 mmHg systolic. The magnitude of this effect means that answering a phone call or talking to family members during measurement can transform a normal reading into an apparently hypertensive one2.
Rushing the measurement without adequate rest period produces predictably elevated readings. The 5-minute rest requirement allows sympathetic nervous system activity to settle to baseline after the physical activity and mental engagement involved in preparing for measurement. Shortening this rest period to 2-3 minutes or skipping it entirely creates readings 5-10 mmHg higher than properly rested measurements1.
Caffeine consumption within 30 minutes before measurement raises blood pressure acutely. Coffee, tea, energy drinks, and caffeinated sodas all stimulate sympathetic activity and increase blood pressure temporarily. The effect peaks 30-45 minutes after consumption and can elevate readings by 5-15 mmHg. Similarly, smoking within 30 minutes causes vasoconstriction that raises pressure1.
Measuring with a full bladder creates reflex sympathetic activation that elevates blood pressure by 10-15 mmHg. This effect proves substantial enough that bladder fullness alone can create spuriously hypertensive readings in individuals with normal baseline pressure. Emptying the bladder before measurement eliminates this variable12.
Cuff placement over clothing interferes with pressure transmission and creates unpredictable measurement artifacts. Even thin shirt sleeves create an additional layer that requires higher cuff inflation pressures and may affect the pressure waveform detection that oscillometric monitors use for measurement. Rolling up tight sleeves that constrict the upper arm creates a tourniquet effect that also interferes with accurate measurement. Always remove clothing from the upper arm and place the cuff directly on bare skin2.
Incorrect cuff tightness affects measurement quality. An excessively loose cuff shifts position during inflation and may not maintain proper bladder alignment over the brachial artery. An overly tight cuff creates discomfort and potentially constricts blood flow even before inflation begins. The two-finger rule (ability to slip two fingers between cuff and arm) provides appropriate tightness2.
Taking single readings rather than averaging multiple measurements increases variability. The first reading in a session often runs higher than subsequent readings, and a single measurement provides no information about measurement consistency. Taking 2-3 readings spaced one minute apart and averaging them substantially improves reliability1.
Measuring at inconsistent times of day creates variability related to circadian blood pressure patterns. Blood pressure follows a daily rhythm with morning surge after awakening, decline during midday, and some elevation in early evening. Comparing a morning reading one day to an evening reading another day mixes time-of-day effects with actual blood pressure changes, making it difficult to assess trends. Consistent measurement timing (morning and evening at the same times daily) separates true changes from circadian variation1.
The practical takeaway: Common technique mistakes (talking, crossed legs, unsupported arm, rushed measurement) can each elevate readings by 5-17 mmHg, creating false hypertension diagnoses in individuals with normal blood pressure.
How Do You Know If Your Blood Pressure Monitor Is Accurate?
Device validation by recognized organizations provides the primary evidence of monitor accuracy. The Association for the Advancement of Medical Instrumentation (AAMI), European Society of Hypertension (ESH), and British Hypertension Society (BHS) all publish validation protocols that test monitors against reference standards under controlled conditions. Monitors that pass these protocols earn validation marks that indicate acceptable accuracy9.
The validation process tests monitors on diverse populations including different age groups, blood pressure ranges, and arm circumferences. The 2018 AAMI/ESH/ISO Universal Standard represents the most demanding current validation protocol, requiring devices to meet criterion 1 (mean difference from reference within 5 mmHg) and criterion 2 (standard deviation under 8 mmHg) across the entire test population and also within specific blood pressure and arm circumference subgroups10.
Research examining validated devices reveals that passing initial validation does not guarantee ongoing accuracy in all use conditions. A systematic review found that only 53% of previously validated devices met the Universal Standard criterion 2 when retested, and few validation studies included sufficient detail about cuff choice or arm circumference subgroups10. This finding emphasizes the importance of proper cuff sizing even when using validated monitors.
Multiple OMRON devices have earned validation through rigorous testing. Research published in 2011 validated the OMRON M2, M3, M6 upper arm monitors and R2 wrist monitor using the ESH protocol. All four devices passed validation with mean differences from reference measurements under 3 mmHg systolic and under 2 mmHg diastolic11. The M6 showed the smallest differences at 1.6±2.9 mmHg systolic and −0.9±2.5 mmHg diastolic.
Specialized populations require specific validation. Arterial stiffness in chronic kidney disease affects oscillometric measurement, yet validation studies demonstrate that devices can perform accurately in CKD populations when properly validated7. The OMRON M3 specifically earned validation for use in stage 3-5 CKD patients with arterial stiffness, representing the first study investigating oscillometric device accuracy in predialysis CKD populations.
Real-world accuracy testing provides additional perspective beyond laboratory validation. When researchers tested blood pressure monitors on their actual owners in home settings rather than controlled laboratory conditions, more than two-thirds showed errors greater than 5 mmHg compared to reference measurements4. This discrepancy between laboratory validation and real-world performance highlights how technique errors, improper cuff size, and other user-dependent factors affect accuracy even when using validated devices.
Most blood pressure monitors lack validation entirely. A comprehensive review of devices on the market found that most blood pressure monitors sold to consumers have never been validated using recognized protocols9. This gap means that purchasers cannot assume accuracy without checking for validation evidence. Looking for specific validation marks (AAMI, ESH, BHS) or consulting validation databases helps identify monitors with documented accuracy.
Validation databases maintained by organizations like the British and Irish Hypertension Society provide searchable lists of validated monitors. These databases include validation protocol used, populations tested, and accuracy grades achieved. Checking these databases before purchasing ensures selection of a validated device rather than relying on marketing claims alone.
Annual accuracy checks by comparison with clinical-grade equipment provide ongoing confidence in monitor performance. Bring your home monitor to your healthcare provider’s office and measure your blood pressure with both your device and their clinical equipment within a few minutes. Readings should agree within 5 mmHg for systolic and diastolic pressures. Larger discrepancies suggest either monitor malfunction or systematic technique errors that need correction1.
Calibration frequency recommendations vary by manufacturer. Most consumer blood pressure monitors do not require regular calibration like clinical equipment, but validation can drift over time with repeated use. Following manufacturer recommendations for periodic validation checks maintains measurement confidence.
Data shows: Most blood pressure monitors sold to consumers have never been validated using recognized protocols, making verification of AAMI/ESH/BHS validation marks essential before purchase.
Why Do Medical Organizations Recommend Upper Arm Monitors Over Wrist Monitors?
The American Heart Association and Japanese Society of Hypertension both recommend upper arm monitors for home blood pressure measurement. The Japanese Society explicitly states that wrist devices should not be used for home monitoring6. This guidance reflects both anatomical and practical considerations that affect measurement accuracy.
Wrist artery anatomy differs from the brachial artery in the upper arm. The radial and ulnar arteries at the wrist are smaller, more superficial, and more variable in position than the brachial artery. These anatomical differences create greater measurement variability with wrist monitors. While wrist monitors can achieve acceptable accuracy when properly positioned at heart level, positioning errors occur more frequently and create larger pressure discrepancies6.
Heart level positioning proves more challenging with wrist monitors. The wrist must be held precisely at mid-chest height during measurement, requiring active positioning and muscle tension to maintain the correct level. Holding the wrist too high lowers readings, while allowing the wrist to drop below heart level elevates measurements. Research demonstrates that positioning errors with wrist monitors create measurement discrepancies of 10-15 mmHg, larger than typical positioning errors with upper arm monitors6.
Studies comparing upper arm and wrist measurements show acceptable correlation when wrist monitors include positioning sensors and users follow protocols carefully. Research examining self-measurement in upper arm versus wrist found no significant differences between daily mean values from multiple readings at each site compared to 24-hour ambulatory monitoring12. However, this equivalence required proper technique and positioning compliance that may not occur consistently in unsupervised home use.
Modern wrist monitors incorporate positioning sensors to address the heart-level challenge. The OMRON Gold Wrist BP4350 includes sensors that detect wrist position and provide visual feedback to guide users to correct heart-level placement. This technology reduces positioning errors compared to wrist monitors without guidance systems, though proper technique remains more critical than with upper arm monitors.
Arterial stiffness increases with age and affects wrist measurements more than upper arm measurements. The smaller, more peripheral arteries at the wrist show greater stiffness changes than the larger brachial artery. This difference means that wrist monitor accuracy may decline with age even when the device performed acceptably in younger populations during validation testing6.
Travel and portability represent the primary advantages of wrist monitors. The compact size and lighter weight make wrist monitors convenient for airplane travel, business trips, or monitoring while away from home. Users who need portable monitoring can achieve accurate wrist measurements by carefully following positioning protocols and using devices with positioning sensors, though upper arm monitors remain preferred for routine home monitoring.
Special populations may benefit from wrist monitors despite general recommendations against their use. Individuals with very large arm circumferences who cannot find appropriately sized upper arm cuffs might achieve better accuracy with wrist monitors than with miscuffed upper arm devices. However, this represents a compromise situation, and seeking extra-large upper arm cuffs remains preferable when possible.
The practical reality that some users will select wrist monitors despite recommendations emphasizes the importance of proper education about heart-level positioning. Wrist monitor users must understand that measurement accuracy depends absolutely on holding the wrist at mid-chest height throughout measurement. Allowing the wrist to rest on a table or hang at waist level creates large systematic errors that defeat the purpose of monitoring.
What you need to know: The American Heart Association and Japanese Society of Hypertension recommend upper arm monitors for home use, with JSH explicitly stating wrist devices should not be used for routine monitoring due to 10-15 mmHg positioning errors.
What Role Does Emotional State and Stress Play in Blood Pressure Readings?
Emotional state and psychological stress substantially affect blood pressure measurements. Research using wearable blood pressure monitoring technology demonstrated that negative emotions raise systolic blood pressure by an average of 5.0±1.3 mmHg, with high stress conditions increasing pressure by 10.2±3.0 mmHg. Under highly stressful conditions combined with negative emotions, blood pressure can rise by 15.2 mmHg systolic and 8.5 mmHg diastolic13.
The magnitude of stress-related blood pressure elevation proves clinically significant. A 15 mmHg systolic increase from emotional distress can transform a reading in the normal range (below 120 mmHg) into the elevated category (120-129 mmHg) or even stage 1 hypertension range (130-139 mmHg). This emotional reactivity explains why some individuals show elevated readings when anxious about measurement itself, creating a self-fulfilling cycle where anxiety about blood pressure produces the very elevation they fear.
White-coat hypertension represents the classic manifestation of emotionally mediated blood pressure elevation. Blood pressure measured in medical settings runs higher than home measurements due to anxiety about the medical environment and interaction with healthcare providers. Studies indicate that self-measurement at home proves particularly helpful for detecting white-coat effects, potentially preventing unnecessary medication in patients whose blood pressure is normal in their usual environment5.
The opposite pattern, masked hypertension, shows normal office readings but elevated home measurements. This pattern occurs in approximately 15-30% of individuals with apparently normal blood pressure in medical settings. Masked hypertension carries cardiovascular risk similar to sustained hypertension, making home monitoring critical for detection. Work stress, chronic anxiety, and other ongoing stressors may contribute to masked hypertension by elevating blood pressure in daily life while medical appointments remain brief calm intervals5.
The 5-minute quiet rest period before measurement partially mitigates stress and emotional effects on readings. Sitting quietly allows sympathetic nervous system activity to decline from the elevated state associated with recent activity or stress. However, this rest period may not completely normalize blood pressure if significant underlying anxiety or stress persists. Practicing relaxation techniques like deep breathing during the rest period may help reduce measurement-related anxiety1.
Consistent measurement timing helps separate emotional influences from true blood pressure patterns. Measuring at the same times daily under similar circumstances reduces variability from emotional state changes. Morning measurements before the day’s stresses accumulate and evening measurements after settling from work both provide information about blood pressure under relatively standardized conditions.
Mindfulness and relaxation practices may help reduce overall blood pressure reactivity to stress. While acute relaxation during measurement can lower individual readings, the goal is not to artificially suppress measurements but rather to reduce chronic stress-related elevation. Some patients benefit from stress management interventions that reduce baseline sympathetic nervous system activity, producing improvements in home blood pressure readings that reflect genuine cardiovascular benefit rather than measurement manipulation.
Medication effects on stress-related blood pressure responses vary by drug class. Beta-blockers reduce heart rate and cardiac output responses to stress, potentially blunting stress-related pressure elevations. Conversely, some medications may affect blood pressure without substantially changing blood pressure reactivity to emotional stimuli. Discussing stress-related blood pressure patterns with healthcare providers helps guide selection of medications that address individual cardiovascular risk profiles.
When Should Home Blood Pressure Readings Prompt Medical Consultation?
Persistently elevated readings meeting hypertension criteria warrant medical consultation. Current guidelines define elevated blood pressure as systolic 120-129 mmHg with diastolic below 80 mmHg, stage 1 hypertension as systolic 130-139 or diastolic 80-89 mmHg, and stage 2 hypertension as systolic 140 or higher or diastolic 90 or higher. Consistently measuring in the stage 1 or stage 2 range over one week of twice-daily monitoring indicates need for medical evaluation1.
Hypertensive urgency readings (systolic over 180 or diastolic over 120) without symptoms require prompt but not emergency consultation. Recheck the pressure after sitting quietly for 5 minutes. If the repeat reading remains over 180/120, contact your healthcare provider the same day for guidance. While these readings indicate severely elevated pressure, absence of symptoms like chest pain, shortness of breath, severe headache, or visual changes means emergency evaluation is not immediately necessary1.
Hypertensive emergency readings (over 180/120) accompanied by symptoms including chest pain, shortness of breath, severe headache, vision changes, difficulty speaking, or numbness require immediate emergency medical attention. These symptoms suggest that severely elevated pressure is causing acute organ damage. Do not wait to recheck the reading or contact your regular provider; instead, call emergency services or go to the emergency department immediately1.
Large blood pressure variability from reading to reading warrants medical discussion. While blood pressure naturally varies throughout the day and between measurements, consistently large swings (more than 30-40 mmHg systolic variation between measurements taken under similar conditions) might indicate blood pressure instability that requires evaluation. Bring your home monitoring log to your provider to review the pattern1.
Significant inter-arm blood pressure differences merit evaluation. Initial measurements should include both arms, and differences greater than 10 mmHg between arms may indicate peripheral vascular disease or anatomical variations affecting blood flow. While small differences are common and benign, larger persistent differences warrant discussion with your healthcare provider1.
Consistent morning hypertension surges with excessive elevation after waking represent a potential risk marker. Blood pressure naturally rises upon awakening, but exaggerated morning surges correlate with increased cardiovascular event risk. If your morning readings consistently run 20-30 mmHg higher than evening readings, discuss this pattern with your provider. Medication timing adjustments or additional morning medications might help control these surges1.
Symptoms potentially related to blood pressure changes warrant medical consultation regardless of measured values. Dizziness, lightheadedness when standing, unusual fatigue, or fainting spells might indicate excessively low blood pressure from medications. Conversely, headaches, nosebleeds without obvious trauma, or vision changes might relate to elevated pressure. Measure your blood pressure during symptoms when possible, and contact your provider to discuss the relationship between symptoms and blood pressure levels.
Medication side effects that interfere with monitoring compliance require provider consultation. Some patients develop cuff anxiety or become excessively focused on blood pressure numbers, creating stress that paradoxically elevates readings. Others find frequent monitoring burdensome. Discussing these challenges with your provider allows development of a monitoring schedule that balances clinical needs with psychological well-being.
Pregnancy requires immediate medical consultation about any elevated readings. Blood pressure over 140/90 during pregnancy may indicate preeclampsia, a potentially serious condition requiring close monitoring and management. Pregnant women should follow their obstetrician’s specific guidance about home monitoring frequency and when to report elevated readings.
Complete Validated Monitor Comparison
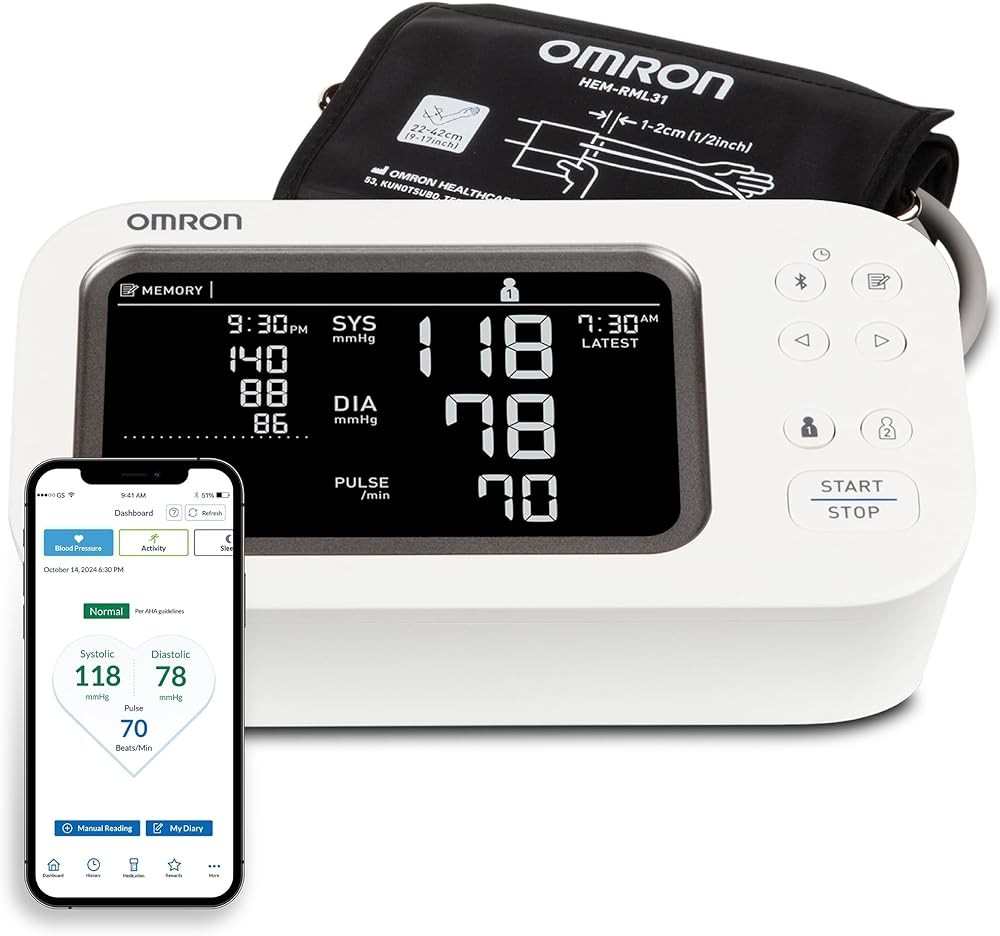
OMRON Platinum BP5450
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The OMRON Platinum BP5450 delivers research-grade accuracy for home monitoring through advanced measurement technology paired with features that support proper technique. TruRead triple-reading mode automatically takes three consecutive readings one minute apart and calculates the average, following AHA recommendations without requiring manual timing or calculation. This feature eliminates the most common compliance barrier to proper multiple-reading technique.
AFib detection during measurement identifies irregular heartbeat patterns that might indicate atrial fibrillation, a significant cardiovascular risk factor. Early AFib detection allows prompt medical evaluation and treatment to reduce stroke risk. The algorithm analyzes the pulse waveform during inflation and deflation, providing screening capability during routine blood pressure checks without additional effort.
The wide-range cuff covering 22-42 cm arm circumferences eliminates miscuffing errors across most adult arm sizes. This single cuff accommodates everyone from thin elderly individuals to larger adults, preventing the systematic measurement errors of 5-15 mmHg that occur when cuff size mismatches arm circumference. The pre-formed construction ensures consistent tension distribution without requiring careful wrapping technique.
Bluetooth connectivity to the OMRON Connect app automates data logging and eliminates manual recording errors. The app stores unlimited readings with date and time stamps, automatically calculates averages over different time periods, and generates graphs showing blood pressure trends. This visualization helps identify patterns and shares comprehensive data with healthcare providers.
The 200-reading memory capacity with date and time stamps provides extensive onboard storage for users who prefer monitor display rather than smartphone apps. Dual-user memory tracks two people separately when couples share one monitor, maintaining separate data sets without manual notation.
Morning hypertension indicator specifically flags elevated morning readings that represent increased cardiovascular risk. The monitor compares current morning readings to recent morning averages and alerts users to significant elevations that warrant medical discussion.
Validation testing demonstrated accuracy meeting ESH International Protocol requirements across blood pressure ranges from hypotensive to stage 2 hypertensive. The oscillometric measurement algorithm adapts to different pulse characteristics and arterial compliance variations, maintaining accuracy across diverse populations.
The investment in the Platinum model proves worthwhile for users who want maximum accuracy confidence and automated compliance with proper technique protocols. TruRead averaging removes the burden of timing multiple readings manually, while comprehensive data tracking through the app provides the documented measurement history that supports productive medical consultations about blood pressure management.

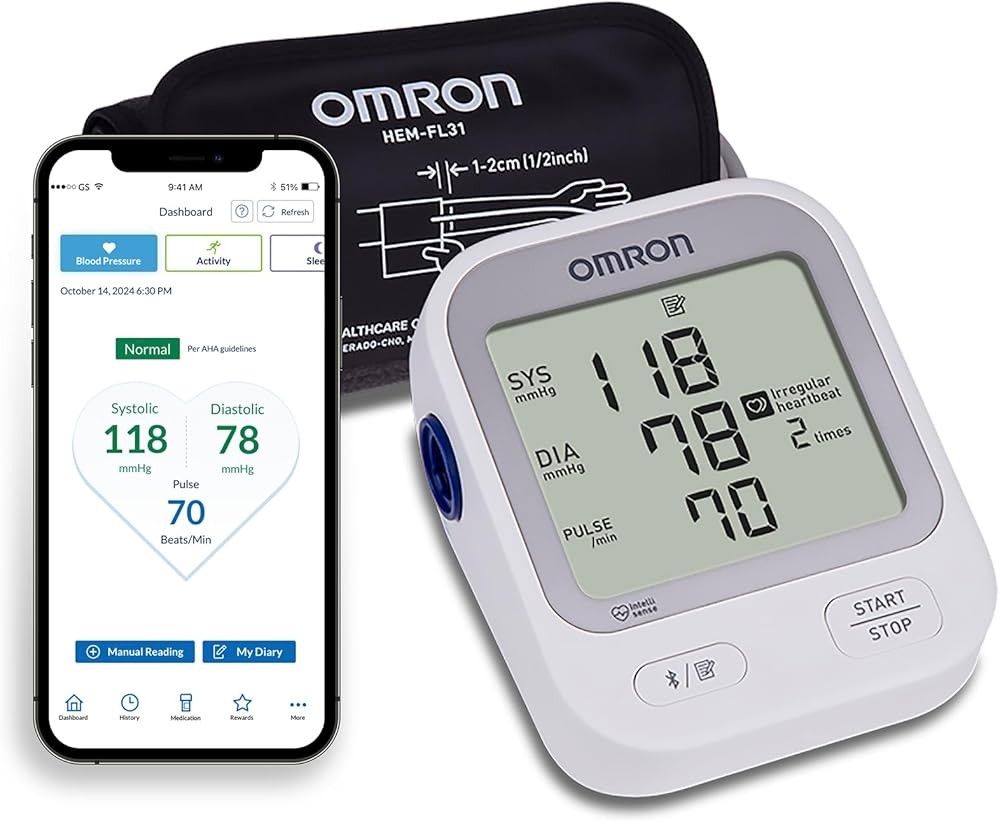
The OMRON Iron BP7000 provides validated accuracy at an accessible price point for users prioritizing essential blood pressure monitoring without advanced features. The oscillometric measurement technology matches the algorithm used in higher-tier OMRON devices, delivering the same fundamental accuracy that earned OMRON extensive validation across diverse populations.
The wide-range cuff covering 22-42 cm ensures proper sizing for most adults without premium pricing. This cuff feature proves particularly valuable given research demonstrating that cuff size errors create systematic measurement discrepancies of 5-15 mmHg. Eliminating miscuffing through appropriate cuff sizing provides accuracy benefits that exceed many electronic features.
Irregular heartbeat detection identifies pulse irregularities during measurement, alerting users to potential cardiac rhythm abnormalities. While not as sophisticated as AFib-specific detection, this basic screening identifies heartbeat patterns that warrant medical evaluation, providing important cardiovascular surveillance during routine blood pressure checks.
The 60-reading memory with date and time stamps stores sufficient data for weekly or biweekly provider consultations. While the memory capacity is smaller than premium models, it accommodates several weeks of twice-daily measurements for users who regularly transfer data to written logs or discuss results with providers.
One-touch operation simplifies the measurement process to a single button press after cuff application. This streamlined interface reduces complexity that might interfere with proper technique, allowing users to focus on positioning and rest period rather than device operation.
The large display with clearly marked systolic, diastolic, and pulse readings ensures easy result interpretation. The high-contrast screen remains readable in various lighting conditions, preventing transcription errors when recording measurements manually.
Clinical validation through the same protocols that certified higher-tier OMRON devices confirms measurement accuracy. The essential technology performs equivalently to premium models for users who follow proper technique protocols and do not require automated assistance with multiple readings.
The Iron BP7000 serves users who understand proper blood pressure measurement technique and prefer straightforward accurate monitoring without smartphone connectivity or automated features. The validated technology and appropriate cuff sizing deliver reliable measurements when users follow AHA protocols for rest period, positioning, and multiple readings.
The OMRON Silver BP5250 balances validated accuracy with convenience features at mid-range pricing. The oscillometric measurement algorithm provides the same fundamental technology that earned OMRON extensive validation evidence, while additional features support compliance with proper measurement protocols.
Irregular heartbeat detection during measurement screens for cardiac rhythm abnormalities that warrant medical attention. This automatic screening occurs during routine blood pressure checks without additional effort, potentially identifying atrial fibrillation or other arrhythmias early in their course when treatment proves most effective.
The multi-color BP level indicator provides immediate visual feedback about reading interpretation. Green indicates normal pressure below 120/80 mmHg, yellow shows elevated or stage 1 hypertension readings, and orange alerts to stage 2 hypertension. This color coding helps users understand measurement significance without memorizing numerical thresholds, though values should still be recorded for trend analysis.
Bluetooth connectivity to the OMRON Connect app enables automated data logging without manual transcription. The app stores measurements with date and time stamps, calculates averages over different time periods, and generates visual graphs showing blood pressure trends. This automated tracking reduces observer bias and patient misreporting documented in research examining manual versus electronic data capture3.
Dual-user mode with 120 total readings (60 per user) accommodates couples monitoring together with a shared device. Separate memory banks maintain independent data sets without manual notation, preventing data mixing that could confuse treatment decisions.
The wide-range cuff covering 22-42 cm arm circumferences eliminates miscuffing errors across most adult sizes. Research establishing that the cuff bladder should encircle the vast majority of arm circumference demonstrates the importance of this feature for measurement accuracy2.
Advanced averaging mode calculates the mean of the last three readings when activated, implementing AHA recommendations for multiple-reading protocols. While not fully automatic like TruRead on premium models, this feature provides averaging support for users who take consecutive measurements manually.
The Silver BP5250 serves users who want automated data tracking and basic averaging support without premium pricing. Bluetooth connectivity enables comprehensive trend analysis through the app, while the validated measurement technology ensures accuracy when proper technique is followed.
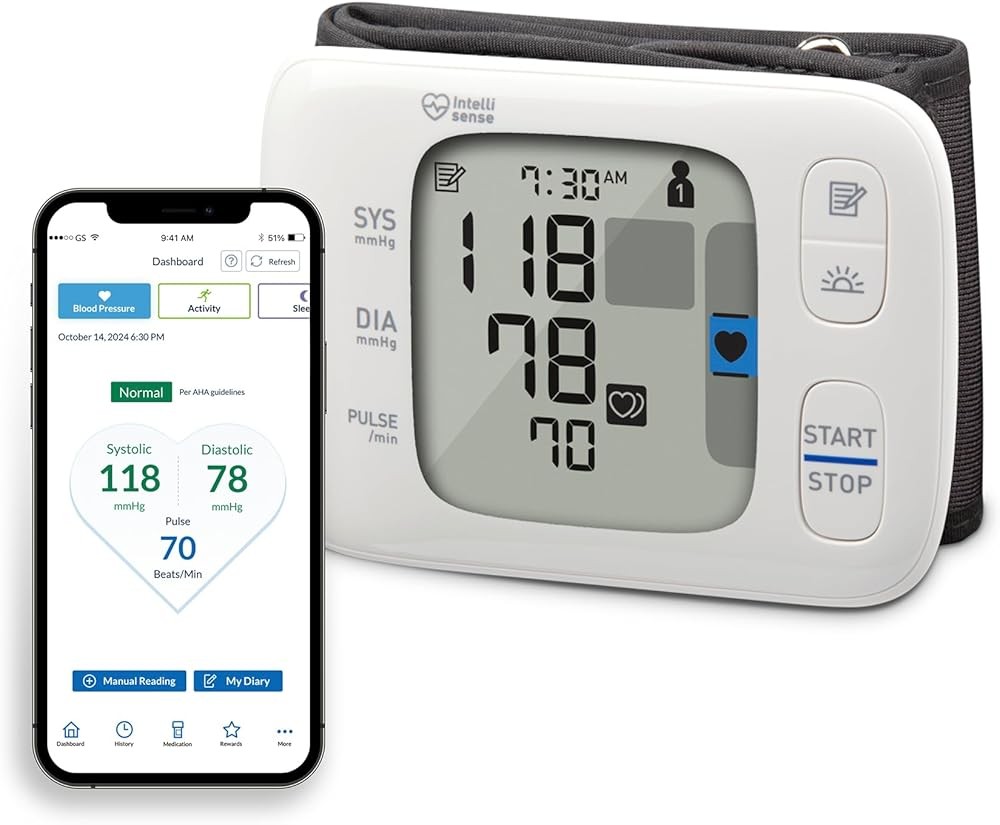
OMRON Gold Wrist BP4350
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The OMRON Gold Wrist BP4350 provides portable blood pressure monitoring for travel and situations where upper arm measurement proves impractical. While medical organizations recommend upper arm monitors for routine home use, wrist devices serve specific needs when paired with careful attention to heart-level positioning6.
The positioning sensor represents the critical feature that distinguishes accurate wrist monitoring from error-prone measurement. Visual indicators guide users to hold the wrist at precise heart level during measurement, reducing the 10-15 mmHg positioning errors common with wrist monitors. The sensor detects wrist height through accelerometer technology and provides real-time feedback to achieve correct placement.
Clinical validation specifically for wrist measurement confirms accuracy when proper positioning is achieved. Research comparing wrist and upper arm monitoring demonstrated that wrist devices can match upper arm accuracy when users carefully maintain heart-level position throughout measurement12. However, this equivalence depends on positioning compliance that occurs more reliably with sensor guidance.
The compact design weighing less than 4 ounces fits easily in carry-on luggage or briefcase pockets for business travel. Users who travel frequently or need monitoring capability away from home can maintain measurement consistency with portable wrist monitoring rather than skipping measurements during travel periods.
Bluetooth connectivity to the OMRON Connect app provides the same automated data logging available on upper arm models. Measurements sync wirelessly with date and time stamps, enabling trend analysis and comprehensive data sharing with healthcare providers despite the portable form factor.
The 100-reading memory with dual-user capability stores sufficient data for several weeks of monitoring for two users. While memory capacity is smaller than premium upper arm models, it accommodates travel monitoring needs without requiring daily smartphone syncing.
Irregular heartbeat detection screens for cardiac rhythm abnormalities during routine measurement. This screening capability proves particularly valuable during travel when users might experience stress, sleep disruption, or dietary changes that could affect heart rhythm.
The pre-formed cuff covering wrist circumferences from 13.5-21.5 cm fits most adult wrists with simple wrapping and closure. Proper cuff sizing matters for wrist monitors just as for upper arm devices, and the wide range accommodates size variation without requiring multiple cuff options.
The Gold Wrist monitor serves as a secondary portable device for users who maintain primary monitoring with an upper arm device but need travel capability. The positioning sensor substantially reduces the primary accuracy limitation of wrist monitors, though careful technique remains more critical than with upper arm monitoring.
Complete Support System
Home blood pressure monitoring works best as part of comprehensive cardiovascular health management. While accurate measurement technique provides reliable data, interpreting and acting on that data requires integration with other health practices and medical care.
Lifestyle modifications complement blood pressure monitoring by addressing modifiable risk factors. Regular physical activity, particularly aerobic exercise like brisk walking, demonstrates consistent blood pressure reduction of 5-8 mmHg in hypertensive individuals. Our guide to the best walking pads and under-desk treadmills explores equipment options for incorporating movement into daily routines regardless of weather or schedule constraints.
Dietary patterns significantly influence blood pressure, with the DASH (Dietary Approaches to Stop Hypertension) diet showing blood pressure reductions comparable to single-drug therapy. Adequate electrolyte intake, particularly potassium, magnesium, and calcium, supports healthy blood pressure regulation. Our review of the best electrolyte supplements examines research-backed formulations that provide these minerals in bioavailable forms.
Vitamin D status correlates with blood pressure in observational studies, though supplementation effects remain under investigation. Maintaining adequate vitamin D levels supports overall cardiovascular health alongside blood pressure management. Our guide to the best vitamin D supplements covers form selection and dosing based on current research.
Nitric oxide availability influences vascular tone and blood pressure through endothelium-dependent vasodilation. Supplementation with nitrate-rich compounds or nitric oxide precursors may support healthy blood pressure levels in some individuals. Our review of the best nitric oxide supplements for blood flow and performance examines the evidence for various formulations.
Comprehensive metabolic monitoring provides context for blood pressure measurements. Blood pressure interacts with glucose metabolism, and individuals with insulin resistance or diabetes often show different blood pressure patterns than metabolically healthy individuals. Our guide to the best continuous glucose monitors for non-diabetics explores metabolic tracking for health optimization.
Equipment selection beyond the blood pressure monitor itself influences monitoring success. Our comprehensive guide to the best blood pressure monitors examines validated devices across price ranges and feature sets, while our comparison of OMRON blood pressure monitors specifically analyzes the product line discussed in this guide.
The debate between arm versus wrist blood pressure monitors influences device selection for users considering portable options. Understanding the tradeoffs between convenience and accuracy helps match monitoring approach to individual needs and circumstances.
Frequently Asked Questions
How long should I rest before taking my blood pressure?
The American Heart Association recommends sitting quietly for at least 5 minutes before taking a reading. During this rest period, sit with your back supported, feet flat on the floor, and arm supported at heart level. Avoid talking during the rest period and measurement. This protocol allows sympathetic nervous system activity to settle to baseline, preventing the 5-10 mmHg elevation that occurs when measurements are rushed1.
What is the correct arm position for blood pressure measurement?
Your arm should be supported at heart level with the cuff positioned on bare skin about 1 inch above the elbow crease. The cuff tubing should align with the brachial artery on the inner side of your arm. An unsupported arm can raise readings by 10 mmHg or more due to muscle tension required to hold the position2.
How many readings should I take at home?
Take 2-3 readings at each session, spaced 1 minute apart, and average the results. The AHA recommends measuring both morning and evening. Discard the first reading if it is significantly higher than subsequent readings, as initial measurements often run elevated due to incomplete relaxation or startle response1.
Does cuff size affect blood pressure readings?
Yes. Using a cuff that is too small can inflate readings by 5-15 mmHg, while a too-large cuff may underestimate pressure. The cuff bladder should encircle at least 80% of your upper arm. Most adults need a standard or large cuff covering arm circumferences from 22-42 cm2.
Should I take blood pressure in my left or right arm?
Initially measure both arms and use the arm with the consistently higher reading for future measurements. Differences of more than 10 mmHg between arms may indicate vascular issues and should be discussed with a healthcare provider1.
What can cause inaccurate home blood pressure readings?
Common causes include wrong cuff size, cuff over clothing, talking during measurement, unsupported back or arm, crossed legs, full bladder, and caffeine or exercise within 30 minutes before measuring. Studies show 69% of home devices tested on actual users showed errors greater than 5 mmHg, largely due to technique factors4.
Is a wrist blood pressure monitor as accurate as an upper arm monitor?
Upper arm monitors are recommended by the AHA and Japanese Society of Hypertension for home use. Wrist monitors can be accurate when held at heart level, but positioning errors are more common and create larger measurement errors of 10-15 mmHg. Wrist devices work best for travel when paired with positioning sensors6.
What time of day should I take my blood pressure?
Measure in the morning before taking medications or eating breakfast, and again in the evening before dinner. Morning readings tend to be higher and are clinically important for detecting morning hypertension surges that correlate with increased cardiovascular risk1.
How do I know if my blood pressure monitor is accurate?
Look for monitors validated by the Association for the Advancement of Medical Instrumentation (AAMI), European Society of Hypertension (ESH), or British Hypertension Society (BHS). Bring your monitor to your doctor’s office annually to compare readings against their clinical-grade equipment. Readings should agree within 5 mmHg9.
What is white coat hypertension and can home monitoring help detect it?
White coat hypertension means your blood pressure reads high in a doctor’s office but normal at home due to anxiety. Home monitoring can identify this pattern, potentially preventing unnecessary medication. Studies show self-measurement is particularly helpful for detecting white-coat effect in patients on treatment5.
Our Top Recommendations
For most users seeking maximum accuracy confidence: The OMRON Platinum BP5450 at $97 delivers automated compliance with AHA measurement protocols through TruRead triple-reading averaging, AFib detection for cardiovascular screening, and comprehensive data tracking through Bluetooth connectivity. The wide-range cuff and validated technology ensure measurement reliability across diverse populations.
For budget-conscious users prioritizing essential accuracy: The OMRON Iron BP7000 at $37 provides validated oscillometric measurement technology and appropriate cuff sizing without premium features. Users who understand proper technique and prefer straightforward monitoring receive reliable data at accessible pricing.
For couples monitoring together or users wanting mid-range features: The OMRON Silver BP5250 at $63 balances accuracy with convenience through Bluetooth tracking, dual-user memory, advanced averaging mode, and visual BP level indicators.
For travel monitoring or situations requiring portability: The OMRON Gold Wrist BP4350 at $78 provides wrist measurement with positioning sensors that address the primary accuracy limitation of wrist devices, enabling measurement continuity during travel.
Join the discussion: Facebook | X | YouTube | Pinterest
Conclusion
Proper blood pressure measurement technique transforms home monitoring from potentially misleading numbers into reliable cardiovascular health data that predicts outcomes better than office measurements. The American Heart Association’s scientific evidence establishes that positioning, rest period, cuff sizing, and multiple-reading protocols determine accuracy as much as device technology itself. Understanding these technique elements and selecting validated monitors enables effective self-monitoring that supports early hypertension detection, white-coat pattern identification, and treatment optimization. The combination of proper technique with appropriately validated equipment provides the measurement confidence necessary for cardiovascular health management through home blood pressure monitoring.
Related Reading
- Best Blood Pressure Monitors: Complete Evidence-Based Guide
- Best OMRON Blood Pressure Monitors Compared
- Arm vs Wrist Blood Pressure Monitors: Which Is More Accurate?
- Best Nitric Oxide Supplements for Blood Flow and Performance
- Best Continuous Glucose Monitors for Non-Diabetics
- Best Electrolyte Supplements: Research-Backed Formulations
- Best Vitamin D Supplements for Cardiovascular Health
- Best Walking Pads and Under-Desk Treadmills for Exercise
References
Muntner P, et al. Measurement of Blood Pressure in Humans: A Scientific Statement From the American Heart Association. Circulation. 2019. PMID: 30827125. ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎
Pickering TG, et al. Recommendations for blood pressure measurement in humans and experimental animals: Part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Circulation. 2005. PMID: 15699287. ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎
Palatini P, Frick GN. Techniques for self-measurement of blood pressure: limitations and needs for future research. J Clin Hypertens (Greenwich). 2012. PMID: 22372772. ↩︎ ↩︎ ↩︎ ↩︎ ↩︎
Real-world device accuracy study examining home BP devices on actual owners. 2017. PMID: 28430848. ↩︎ ↩︎ ↩︎
Denolle T, et al. Self-measurement of blood pressure in clinical trials and therapeutic applications. Blood Press Monit. 2000. PMID: 10828901. ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎
Japanese Society of Hypertension guidelines for home blood pressure measurement. 2003. PMID: 14621179. ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎ ↩︎
Akpolat T, et al. Validation of the Omron M3 Intellisense (HEM-7051-E) upper arm blood pressure monitor, for self-measurement, according to the European Society of Hypertension International Protocol revision 2010 in a stage 3-5 chronic kidney disease population. Kidney Blood Press Res. 2012. PMID: 21912183. ↩︎ ↩︎
Myers M, et al. Validation of blood pressure measurement in pregnancy: systematic review and meta-analysis. Blood Press Monit. 2022. PMID: 34998224. ↩︎
Mazoteras-Pardo V, et al. Validated blood pressure measuring devices using recognized protocols. Systematic review. Med Clin (Barc). 2022. PMID: 36675670. ↩︎ ↩︎ ↩︎
de Oliveira ACS, et al. Systematic review of home blood pressure monitors validated according to the International Protocol: focus on criterion 2. Eur J Prev Cardiol. 2025. PMID: 39351853. ↩︎ ↩︎
Topouchian J, et al. Validation of four automatic devices for self-measurement of blood pressure according to the international protocol of the European Society of Hypertension. Vasc Health Risk Manag. 2011. PMID: 22174581. ↩︎
Eckert S, et al. Comparison of blood pressure measured at the arm, wrist and finger. Clin Physiol. 1996. PMID: 8896310. ↩︎ ↩︎
Tomitani N, et al. Self-monitoring stress-induced blood pressure with a wearable watch-type blood pressure monitor: A pilot study. J Clin Hypertens (Greenwich). 2022. PMID: 35672456. ↩︎
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



