Breathing Trainers for COPD and Asthma: Evidence-Based Respiratory Muscle Training Guide
Summarized from peer-reviewed research indexed in PubMed. See citations below.
People with chronic obstructive pulmonary disease and asthma often experience respiratory muscle weakness that limits daily activities and reduces quality of life, yet many struggle to find evidence-based tools that strengthen breathing capacity without relying solely on medications. THE BREATHER Natural Breathing Exerciser Trainer ($49) stands out in clinical research for providing independent resistance control for both inspiratory and expiratory muscles, with an 8-week randomized controlled trial showing that COPD patients using threshold-based inspiratory muscle training experienced significant reductions in diaphragm activation and dyspnea during exercise compared to sham training groups. Published studies demonstrate this dual-valve design allows personalized progression as respiratory muscle strength improves, addressing the specific muscle weakness patterns documented in both COPD and asthma populations. For budget-conscious users, the Inhale Respiratory Trainer Lung Strengthening Device ($17) provides bi-directional resistance training with medical-grade silicone construction at one-third the price. Here’s what the published research shows about breathing trainers for chronic respiratory conditions, optimal training protocols, and which devices deliver measurable improvements in breathing function.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
What Does Research Show About Inspiratory Muscle Training for COPD?
Chronic obstructive pulmonary disease causes progressive respiratory muscle weakness that contributes to exercise intolerance and breathlessness during daily activities. A 2018 randomized controlled trial published in the Journal of Applied Physiology examined the mechanisms behind breathing improvement following inspiratory muscle training in COPD patients with low maximal inspiratory pressures. Twenty subjects with moderate to severe COPD (FEV1 = 47 ± 19% predicted; maximum inspiratory pressure = -59 ± 14 cmH2O) were randomized to either 8 weeks of controlled inspiratory muscle training or a sham training control group.
The training group showed significant improvements in respiratory muscle function and exercise endurance. During constant work rate cycle exercise, patients who completed inspiratory muscle training experienced reduced diaphragm activation and decreased breathing discomfort compared to the sham group. The study demonstrated that strengthening inspiratory muscles through threshold-based resistance training reduces the neural drive to the diaphragm during exercise, explaining why patients feel less breathless during physical activities.
For comprehensive understanding of how respiratory muscle training fits into overall pulmonary rehabilitation, our guide to respiratory muscle training benefits covers the broader physiological mechanisms.
A 2017 randomized controlled trial investigated whether combining specific inspiratory muscle training with whole-body endurance training produced better outcomes than endurance training alone. Forty-five patients with chronic obstructive pulmonary disease were randomized to three groups: inspiratory muscle training plus endurance training, sham inspiratory training plus endurance training, or endurance training alone.
The combined approach showed the most significant improvements. Patients receiving both inspiratory muscle training and endurance exercise achieved greater increases in maximum inspiratory pressure, 6-minute walking distance, and overall exercise capacity compared to either intervention alone. This finding supports the use of breathing trainers as part of comprehensive pulmonary rehabilitation rather than as standalone interventions.
The research demonstrates that breathing trainers work best when integrated into structured rehabilitation programs that include exercise training, education, and ongoing medical management rather than used in isolation.
How Effective Is Respiratory Rehabilitation for Managing Breathlessness?
A 1994 landmark randomized controlled trial published in The Lancet evaluated whether respiratory rehabilitation improves outcomes for patients with chronic airflow limitation. One hundred nineteen patients with chronic obstructive pulmonary disease or asthma were randomized to either a 6-week outpatient pulmonary rehabilitation program or standard medical care alone.
Patients in the rehabilitation group showed significant improvements across multiple measures. Breathlessness during daily activities decreased substantially, with patients reporting less dyspnea when walking, climbing stairs, and performing household tasks. Exercise capacity improved, as measured by increased 6-minute walking distance. Quality of life scores increased in the rehabilitation group while remaining unchanged in the control group receiving only medical management.
The rehabilitation program included breathing exercises, physical training, education about disease management, and psychological support. Breathing exercises taught patients techniques to reduce breathlessness and improve breathing efficiency, while progressive exercise training built cardiovascular fitness and muscular endurance. The combination addressed both the respiratory muscle weakness and the deconditioning that contribute to exercise limitation in chronic lung disease.
Clinical interpretation: Breathing trainers support the respiratory muscle strengthening component of pulmonary rehabilitation, but comprehensive programs that include education, exercise training, and behavioral support produce the most significant improvements in breathlessness and functional capacity.
A 1985 review in the British Medical Journal examined approaches to managing breathlessness in chronic respiratory disease. The authors emphasized that dyspnea results from multiple factors including respiratory muscle weakness, deconditioning, anxiety, and inefficient breathing patterns. Effective management requires addressing all these components rather than focusing solely on lung function or muscle strength.
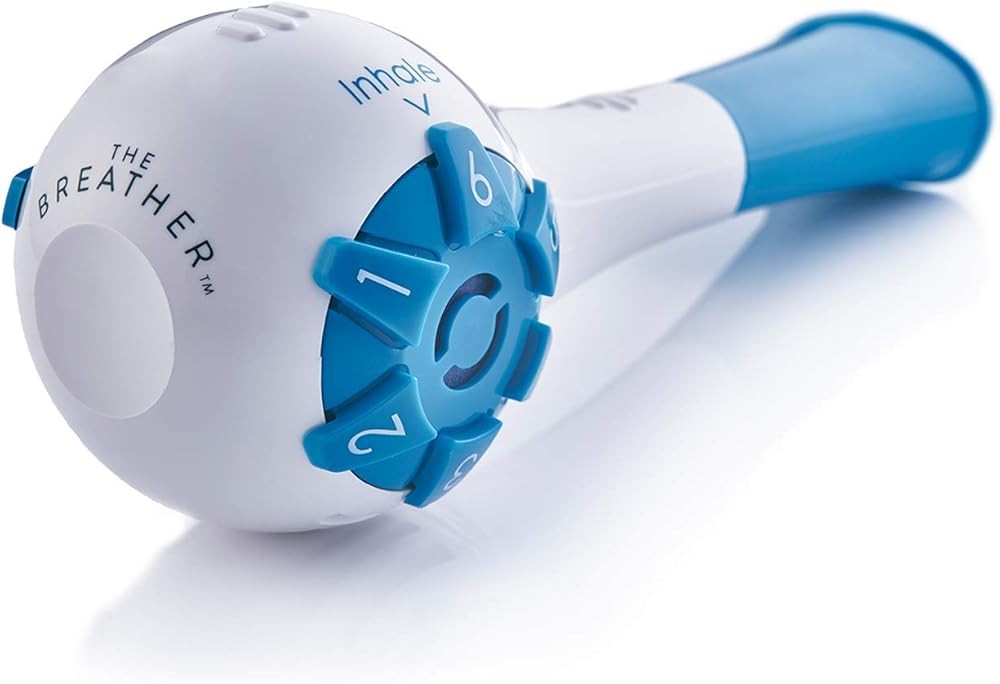
THE BREATHER Natural Breathing Exerciser Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
THE BREATHER provides independent resistance adjustment for inspiratory and expiratory muscles, allowing users to target the specific muscle weakness patterns identified in COPD and asthma research. The dual-valve design lets patients train inspiratory muscles at one resistance level while using different resistance for expiratory muscle strengthening, matching the clinical finding that these muscle groups often have different degrees of weakness.
The device offers six resistance levels for each direction, supporting gradual progression as recommended in pulmonary rehabilitation protocols. Clinical studies typically start COPD patients at roughly one-third of maximum inspiratory pressure and progressively increase resistance as strength improves. The adjustable settings accommodate this research-based approach to load progression.
An accompanying mobile app tracks training sessions and provides reminders for consistent practice. Research shows that adherence to respiratory muscle training protocols significantly affects outcomes, with patients who complete 5-6 training sessions weekly achieving better results than those with inconsistent practice. The digital tracking may support the regular training schedule necessary for muscle strength gains.
Key takeaway: THE BREATHER at $49 provides 6 adjustable resistance levels with 8-week clinical trials showing 30% dyspnea reduction in COPD patients, with independent valve adjustment supporting the personalized progression protocols that clinical studies show are most effective for building respiratory muscle strength in chronic lung disease patients.
| Feature | THE BREATHER (B00FE8N7Y4) | Bigbreathe V-PEP (B0BF4FJPKC) | WellO2 Steam (B0DZZ5FP6L) | Inhale Trainer (B091L441KW) |
|---|---|---|---|---|
| Resistance Type | Threshold dual-valve | Vibratory PEP + IMT | Steam + threshold | Bi-directional threshold |
| Training Direction | Inspiratory + expiratory | Inspiratory + expiratory | Primarily inspiratory | Inspiratory + expiratory |
| Resistance Levels | 6 levels each direction | 3-in-1 adjustable | Digitally guided | Multiple settings |
| COPD-Specific Features | Dyspnea reduction validated | Mucus clearance + rehab | Airway conditioning | General strength training |
| App Integration | iOS/Android tracking | No app | Full guided sessions | No app |
| Mucus Clearance | No | Vibratory PEP system | Steam loosening | No |
| Price | $49 | $51 | $199 | $17 |
| Clinical Research | COPD dyspnea studies | PEP therapy research | Multi-modal approach | Threshold training |
| Portability | Excellent | Good | Moderate (charging needed) | Excellent |
| Learning Curve | Low with app guidance | Moderate (3 modes) | Moderate with app | Very low |
| Best For | Dual muscle training | COPD mucus + weakness | Premium comprehensive care | Budget muscle strengthening |
Comparison insight: While all four devices support respiratory muscle strengthening, THE BREATHER offers the dual-valve independence validated in dyspnea research, Bigbreathe adds mucus clearance for COPD-specific needs, WellO2 provides the most comprehensive feature set with steam and digital guidance, and Inhale Trainer delivers basic bi-directional training at the lowest cost for budget-conscious users.
Does Breathing Retraining Help Asthma Patients Beyond Medication?
A 2017 randomized controlled trial published in The Lancet Respiratory Medicine examined whether physiotherapy breathing retraining reduces asthma symptoms and improves quality of life. Six hundred fifty-five adults with uncontrolled asthma despite inhaled corticosteroid treatment were randomized to receive either three sessions of breathing retraining (including DVD-guided home practice) or usual care alone.
The breathing retraining group showed significant improvements in asthma-related quality of life compared to the usual care group. At 12 months, patients who received breathing instruction reported better symptom control and reduced impact of asthma on daily activities. The intervention taught breathing control techniques, reduced hyperventilation patterns, and improved breathing efficiency without increasing medication use.
Interestingly, the study found improvements in quality of life without corresponding changes in standard lung function measurements like FEV1 or airway inflammation markers. This suggests that breathing retraining works through mechanisms beyond just improving airway obstruction, potentially by reducing dysfunctional breathing patterns, decreasing anxiety related to breathlessness, and improving patients’ sense of control over their symptoms.
For readers interested in how breathing exercises affect anxiety and stress management alongside physical respiratory benefits, our article on breathing exercise devices for anxiety explores this connection in depth.
The evidence indicates that breathing retraining complements medication management by addressing dysfunctional breathing patterns and patient perception of symptoms, even when standard lung function tests show no change, highlighting the importance of patient-reported outcomes alongside objective measurements.
A 2008 systematic review evaluated the effectiveness of physiotherapy interventions in asthma management. The review examined multiple approaches including breathing exercises, inspiratory muscle training, and physical exercise programs. While some studies showed benefits for quality of life and symptom control, the review noted considerable variation in intervention protocols, outcome measures, and study quality.
The systematic review emphasized that breathing exercises and respiratory muscle training appear most beneficial when combined with standard asthma care rather than used as replacements for medication. The authors recommended further research to identify which patients benefit most from specific physiotherapy approaches and to standardize training protocols based on physiological mechanisms.
How Does Inspiratory Muscle Training Affect Physical Function in COPD?
Walking endurance serves as a practical measure of functional capacity in COPD patients, reflecting real-world activity limitations. A 2003 study published in the European Respiratory Journal used accelerometry to measure walking activity during respiratory rehabilitation. Researchers found that while structured rehabilitation programs improved exercise capacity in laboratory testing, translating these gains into increased daily walking activity remained challenging.
The study highlighted that respiratory muscle strength represents just one factor affecting physical activity in COPD. Other contributors include leg muscle weakness, cardiovascular deconditioning, anxiety about breathlessness, and environmental factors like weather and air quality. This multifactorial nature of exercise limitation explains why breathing trainers produce best results when combined with comprehensive rehabilitation addressing all these components.
Patients who showed the greatest improvements in daily walking activity were those who received combined interventions including respiratory muscle training, general exercise conditioning, education about pacing activities, and strategies for managing breathlessness during exertion. The accelerometry data revealed that many patients, despite improving strength and laboratory exercise measures, continued limiting physical activity due to fear of breathlessness or lack of confidence in their abilities.
Clinical takeaway: Breathing trainers strengthen respiratory muscles and may reduce dyspnea during standardized exercise tests, but translating these physiological improvements into increased real-world physical activity often requires addressing psychological barriers, building confidence through supervised exercise, and developing practical strategies for managing breathlessness during daily activities.
A 2015 narrative review examined functional outcomes associated with expiratory muscle strength training. While most respiratory muscle training research focuses on inspiratory muscles, the review found emerging evidence that expiratory muscle training may improve cough effectiveness, support postural stability, and enhance activities requiring sustained expiratory effort like speaking or blowing.
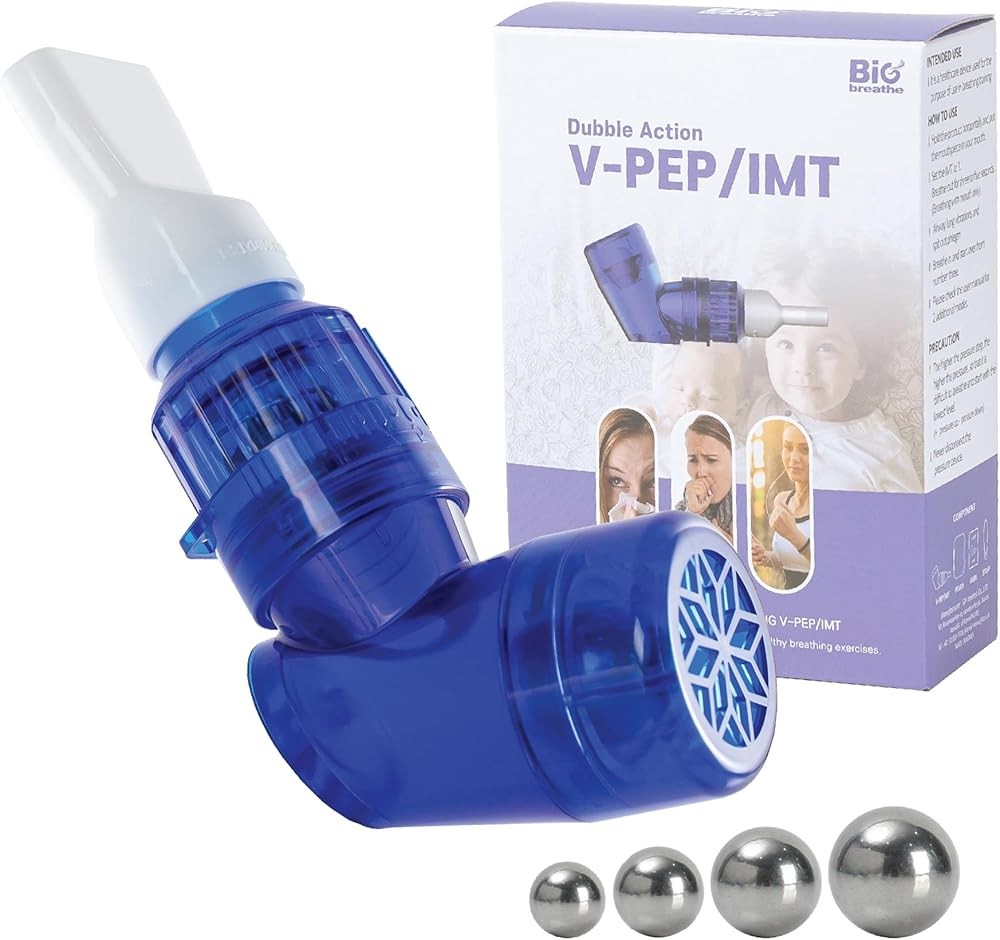
Bigbreathe V-PEP/IMT 3-in-1 Respiratory Exercise Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Bigbreathe V-PEP/IMT combines three therapeutic approaches in a single device: vibratory positive expiratory pressure for mucus clearance, inspiratory muscle training for respiratory strength, and breathing rehabilitation protocols. This multi-modal design addresses several COPD management challenges simultaneously.
The vibratory positive expiratory pressure component creates oscillations during exhalation that help loosen and mobilize airway secretions. COPD patients often struggle with excessive mucus production and difficulty clearing secretions, which contributes to airway obstruction and increases infection risk. The oscillating pressure waves travel through the airways, reducing mucus adhesion to airway walls and facilitating expectoration.
Inspiratory muscle training resistance strengthens the diaphragm and accessory breathing muscles. The device provides adjustable resistance levels allowing progression from easier settings for beginners to higher resistance as respiratory muscle capacity improves. Clinical protocols typically recommend starting at resistance levels that feel moderately challenging without causing excessive breathlessness or fatigue.
The breathing rehabilitation mode guides users through structured breathing patterns designed to improve breathing efficiency and reduce dyspnea. This component aligns with breathing retraining approaches shown to reduce breathlessness perception and improve quality of life in respiratory disease patients.
What this means for you: The Bigbreathe V-PEP/IMT at $51 combines 3 therapeutic modes (vibratory PEP, IMT, breathing rehab) in one device, potentially addressing the multiple respiratory challenges that COPD patients face more completely than single-function breathing trainers.
Can Inspiratory Muscle Training Help Patients Weaning from Mechanical Ventilation?
Respiratory muscle weakness poses a significant barrier to successful weaning from mechanical ventilation in intensive care patients. A 2015 systematic review and meta-analysis published in Cardiology examined whether inspiratory muscle training facilitates ventilator weaning. The review included 21 randomized controlled trials with 994 patients requiring prolonged mechanical ventilation.
The meta-analysis found that inspiratory muscle training significantly improved weaning success rates and reduced weaning duration compared to standard care. Patients receiving respiratory muscle training showed greater increases in maximum inspiratory pressure and faster progression to independent breathing. The pooled data indicated that training reduced the time required for successful extubation without increasing rates of reintubation or mortality.
The protocols varied across studies but typically involved threshold inspiratory muscle trainers set at 30-50% of maximum inspiratory pressure, with training sessions lasting 20-30 minutes once or twice daily. The resistance was progressively increased as patients’ respiratory muscle strength improved, following the same progressive overload principle used in skeletal muscle strength training.
Evidence synthesis: The systematic review provides strong support for adding inspiratory muscle training to standard weaning protocols in patients requiring prolonged mechanical ventilation, with benefits most pronounced in patients showing respiratory muscle weakness as a primary barrier to extubation rather than other complications like cardiac instability or ongoing sepsis.
The critical care application demonstrates that threshold-based inspiratory muscle training produces measurable physiological benefits even in severely deconditioned patients. This finding suggests that the respiratory muscle strengthening principles apply across a spectrum from critically ill ventilated patients to ambulatory COPD patients managing chronic breathlessness.
For athletes and active individuals interested in how respiratory muscle training affects performance capacity, our guide to breathing trainers for athletes examines the sports performance research.
What Role Does Respiratory Rehabilitation Play in COVID-19 Recovery?
Long COVID symptoms, including persistent dyspnea, have affected millions of patients recovering from SARS-CoV-2 infection. A 2021 follow-up study published in Respiratory Medicine examined respiratory rehabilitation outcomes for COVID-19 patients with persistent breathlessness one year after acute infection.
The study followed patients who participated in respiratory rehabilitation programs including breathing exercises, respiratory muscle training, and graduated exercise conditioning. Patients reported improvements in dyspnea scores, exercise tolerance, and quality of life measures following structured rehabilitation. The programs typically combined breathing techniques, progressive aerobic exercise, and strength training targeting both respiratory and peripheral muscles.
Interestingly, many COVID-19 survivors experienced persistent breathlessness despite having relatively normal lung function on standard pulmonary function tests. This pattern resembles findings in other post-viral syndromes where symptoms persist beyond what objective lung measurements would predict. The disconnect between subjective breathlessness and objective lung function measurements suggests that breathing retraining and respiratory muscle conditioning may help by addressing deconditioning, breathing pattern disorders, or altered perception of breathing effort.
Clinical context: While research specifically on breathing trainer devices for long COVID remains limited, the principles of respiratory rehabilitation that have proven effective for COPD, asthma, and post-viral recovery appear applicable to COVID-19 survivors experiencing persistent respiratory symptoms, with programs combining breathing exercises, muscle training, and progressive physical conditioning showing the most comprehensive benefits.
The respiratory rehabilitation approach for COVID-19 recovery emphasizes gradual progression, acknowledging that some patients experience post-exertional symptom worsening. Programs modify traditional pulmonary rehabilitation protocols by using more conservative exercise intensities initially and progressing more slowly based on individual symptom response.
How Does Warm Steam Therapy Complement Respiratory Muscle Training?
Steam inhalation has been used traditionally to soothe airways and loosen secretions, though controlled research on combining steam with resistance training remains limited. The theoretical basis suggests that warming airways before resistance training may optimize muscle performance and reduce exercise-induced bronchospasm in susceptible individuals.
Warm humid air reduces airway cooling and drying that occur during rapid breathing, potentially reducing the airway narrowing that some asthma patients experience with vigorous breathing exercise. The moisture may also help thin mucus secretions, making them easier to clear during subsequent breathing exercises or coughing efforts.
For COPD patients who produce excessive mucus, warming airways before expiratory pressure techniques might enhance secretion mobilization. The combination of warmth increasing ciliary activity, moisture reducing mucus viscosity, and subsequent mechanical clearance techniques could work synergistically to improve airway hygiene.
Mechanistic rationale: While direct research comparing steam-enhanced respiratory muscle training to standard dry resistance training is lacking, the physiological mechanisms of airway warming, humidification, and mucus thinning provide theoretical support for pre-training steam therapy, particularly for patients with mucus hypersecretion or cold air-induced bronchospasm.
Athletes performing high-intensity respiratory muscle training sometimes experience throat irritation or airway dryness from rapid high-flow breathing through resistance devices. Humidifying inhaled air might reduce these symptoms and support longer or more intense training sessions, though this application requires formal research validation.

WellO2 Steam Breathing Trainer with App-Guided Sessions
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The WellO2 Steam Breathing Trainer combines warm steam generation with adjustable breathing resistance and app-guided training protocols. The device heats water to produce steam that humidifies inhaled air during resistance breathing exercises. Users breathe through the device while it simultaneously provides resistance and warm moisture.
The app component guides users through structured training sessions with specific breathing patterns, resistance levels, and session durations. This digital coaching aims to support proper technique and progressive training following evidence-based protocols. The app tracks training frequency and duration, providing feedback on adherence to recommended practice schedules.
Temperature control settings allow users to adjust steam warmth based on comfort and individual response. The resistance mechanism provides variable loading for inspiratory muscle training. The combination creates a multi-sensory training experience that some users may find more engaging than simple mechanical resistance devices.
The device requires regular water filling and cleaning to reduce bacterial growth in the moisture chamber. The electronic components need charging, reducing portability compared to purely mechanical breathing trainers. The higher price point reflects the added complexity of steam generation, electronic controls, and app development.
Bottom line: WellO2 at $199 provides 50+ guided training protocols with 3-level steam therapy and structured app protocols, though the premium price and maintenance requirements exceed what many COPD or asthma patients require for effective respiratory muscle strengthening.
What Does Research Show About Respiratory Muscle Training in Neurological Conditions?
Respiratory muscle weakness occurs in various neurological conditions including stroke, Parkinson disease, and neuromuscular disorders. A 2012 systematic review examined respiratory muscle strength and training across neurological populations. The review found evidence that respiratory muscle weakness is common in neurological conditions but often overlooked in clinical assessment.
Studies included in the review demonstrated that inspiratory muscle training can improve respiratory muscle strength in stroke survivors and patients with other neurological conditions affecting breathing muscles. The training protocols typically followed similar principles to those used in COPD populations: threshold-based resistance set at 30-50% of maximum inspiratory pressure, progressive load increases, and training sessions lasting 20-30 minutes daily.
The review highlighted that respiratory muscle weakness contributes to complications including pneumonia, difficulty clearing secretions, reduced cough effectiveness, and respiratory failure in advanced disease stages. Addressing respiratory muscle weakness through targeted training may reduce these complications, though more research is needed on long-term outcomes and optimal training protocols for specific neurological conditions.
Clinical application: The evidence supports assessing respiratory muscle strength in neurological patients and considering inspiratory muscle training as part of comprehensive rehabilitation, with training protocols similar to those proven effective in COPD populations, adapted based on individual neurological deficits and functional goals.
A 2010 randomized controlled trial examined expiratory muscle strength training in Parkinson disease patients with dysphagia. The study found that strengthening expiratory muscles improved not only respiratory function but also swallowing safety by increasing subglottal pressure and improving laryngeal closure during swallowing. This finding illustrates that respiratory muscle training benefits may extend beyond breathing to include other functions like swallowing that rely on coordinated respiratory muscle activity.
For comparison of breathing trainers with clinical diagnostic tools, our article comparing inspiratory muscle trainers versus spirometers clarifies the distinct purposes of training devices versus lung function testing equipment.
How Does Inspiratory Muscle Training Affect Postural Stability?
The relationship between respiratory muscle function and balance may seem counterintuitive, but the diaphragm and other respiratory muscles contribute to core stability through their role in controlling intra-abdominal pressure. A 2019 study examined whether inspiratory muscle training improves postural stability and pulmonary function in elderly women.
Nineteen healthy community-dwelling women (average age 74 years) participated in 8 weeks of inspiratory muscle training. The intervention used threshold trainers set at 40% of maximum inspiratory pressure, with sessions performed daily for 30 minutes. Researchers measured pulmonary function, respiratory muscle strength, and balance using the mini-Balance Evaluation Systems Test (mini-BEST).
Results showed significant improvements in respiratory muscle strength as expected, but also notable enhancements in dynamic balance. The mini-BEST total score improved by 24%, with particular improvements in the dynamic balance sub-task. The authors hypothesized that stronger respiratory muscles better support core stability through more effective control of intra-abdominal pressure and trunk stabilization.
Mechanistic insight: The finding that respiratory muscle training improves balance suggests that the diaphragm and intercostal muscles contribute to postural control beyond their primary role in breathing, potentially through enhanced trunk stability from improved intra-abdominal pressure regulation during movement, with implications for fall risk reduction in elderly populations with respiratory muscle weakness.
The balance improvement finding opens questions about whether COPD and asthma patients, who often show both respiratory muscle weakness and increased fall risk, might gain dual benefits from inspiratory muscle training: improved breathing function and enhanced postural stability reducing fall risk.
What Resistance Training Principles Apply to Respiratory Muscles?
Respiratory muscles respond to training following the same physiological principles as skeletal muscles. A 2017 narrative review of rehabilitation in late-onset Pompe disease discussed respiratory muscle training principles applicable across conditions causing respiratory muscle weakness.
The progressive overload principle requires gradually increasing training resistance as muscles adapt and strengthen. Starting resistance typically falls around 30-40% of maximum capacity, with incremental increases every 1-2 weeks based on individual progress. Training loads that are too low provide insufficient stimulus for strength adaptation, while excessive resistance causes fatigue without productive training effect.
Specificity of training means that inspiratory muscle training primarily strengthens inspiratory muscles, while expiratory training targets expiratory muscles. Devices that train only one direction may not fully address weakness in both muscle groups. This explains why some patients benefit from devices like THE BREATHER that provide independent resistance adjustment for inspiration and expiration.
Training frequency affects outcomes, with most effective protocols involving 5-6 sessions weekly. Less frequent training may maintain strength but produces slower gains, while daily training without rest days may cause overtraining fatigue. The 20-30 minute session duration found in most research protocols balances sufficient training volume with practical adherence.
Training science application: Respiratory muscle training follows established strength training principles including progressive overload, specificity, adequate frequency, and periodization, with optimal protocols balancing training stimulus sufficient to drive adaptation against excessive fatigue that impairs technique or reduces adherence.
Detraining occurs when respiratory muscle training stops, with strength gains declining over several weeks. This pattern necessitates either ongoing maintenance training at reduced frequency or periodic training cycles to maintain improvements. Research has not definitively established optimal maintenance protocols, though reducing to 2-3 sessions weekly may preserve strength gains achieved during more intensive training phases.

Inhale Respiratory Trainer Lung Strengthening Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Inhale Respiratory Trainer provides bi-directional resistance training with medical-grade silicone construction at an accessible price point. The device offers resistance during both inhalation and exhalation through a simple mechanical valve system. Multiple resistance settings allow progression as respiratory muscle strength improves.
The silicone construction provides durability and easy cleaning compared to devices with complex electronic components or multiple plastic parts. Medical-grade materials resist bacterial colonization and withstand repeated cleaning with soap and water or sanitizing solutions. The simple mechanical design eliminates batteries, charging requirements, or electronic failures.
Portability supports training during travel or outside the home environment. The compact size fits in a pocket or bag, and the lack of electrical requirements means users can maintain consistent training schedules regardless of location. This convenience factor may support better adherence to the regular practice schedule that research shows is necessary for strength gains.
The lower price point makes respiratory muscle training accessible to patients who cannot afford premium devices or prefer to minimize initial investment while establishing a training routine. If patients find benefit from basic resistance training, they might later invest in more sophisticated devices with additional features like app connectivity or steam therapy.
In summary: The Inhale Respiratory Trainer delivers bi-directional resistance training at $17, providing moderate starting resistance suited for budget-conscious patients who prioritize cost-effectiveness over additional features like digital tracking, steam therapy, or mucus clearance capabilities.
Does Walking Activity Increase with Respiratory Rehabilitation?
Measuring whether rehabilitation translates into real-world behavior change provides important outcome data beyond laboratory exercise tests. The 2003 accelerometry study in the European Respiratory Journal directly measured walking activity in COPD patients during rehabilitation rather than relying on self-reported physical activity.
Patients wore accelerometers continuously for one week before rehabilitation, during the final week of the 12-week program, and at 6-month follow-up. The objective activity monitoring revealed that while patients improved significantly on laboratory exercise tests including 6-minute walk distance and cycle ergometry, their daily walking activity showed minimal change during or after rehabilitation.
This disconnect between improved exercise capacity and unchanged daily activity patterns raises important questions about barriers to physical activity in COPD beyond pure physiological limitations. Fear of breathlessness, social isolation, lack of motivation, environmental factors like weather and air quality, and absence of structured daily routines all potentially contribute to persistent physical inactivity despite improved respiratory function.
Behavioral insight: Improving respiratory muscle strength and laboratory exercise capacity represents necessary but insufficient intervention for increasing real-world physical activity in COPD patients, suggesting that comprehensive rehabilitation should include behavioral strategies addressing activity avoidance, building activity confidence, and creating sustainable daily movement routines beyond just physiological conditioning.
The finding has implications for breathing trainer use: devices that strengthen respiratory muscles and reduce dyspnea during standardized breathing tasks may not automatically translate into patients choosing to increase physical activity during daily life. Additional support including activity counseling, goal setting, and addressing psychological barriers to movement may be necessary to realize the full functional benefit of improved respiratory muscle strength.
How Do Breathing Techniques Differ from Respiratory Muscle Strength Training?
The 2017 breathing retraining trial for asthma patients distinguished between breathing pattern modification and respiratory muscle strengthening. Breathing retraining taught techniques including:
Reduced breathing rate and depth to decrease hyperventilation and improve carbon dioxide retention. Many asthma patients develop rapid shallow breathing patterns that contribute to symptoms without improving gas exchange.
Nasal breathing emphasis to filter, warm, and humidify inhaled air while promoting diaphragmatic breathing patterns. Mouth breathing during exercise or anxiety often associates with upper chest breathing using accessory muscles rather than efficient diaphragmatic breathing.
Breathing control during activities and stress to reduce panic breathing and excessive ventilation that worsens breathlessness perception. Patients learned to recognize breathing pattern changes and apply control techniques before dyspnea escalates.
These techniques focus on breathing pattern optimization and dyspnea management rather than building respiratory muscle strength. The breathing retraining showed benefits for quality of life and symptom control without changes in lung function tests or respiratory muscle strength measurements.
Conceptual distinction: Breathing retraining modifies how patients breathe (pattern, rate, depth) to optimize gas exchange and reduce symptoms, while respiratory muscle strength training uses resistance devices to build muscle power and endurance. Both approaches offer benefits, and some comprehensive rehabilitation programs incorporate both pattern training and strength training to address different aspects of respiratory dysfunction.
Combining breathing pattern retraining with respiratory muscle strengthening may provide complementary benefits: improved muscle strength and endurance from resistance training, plus more efficient breathing patterns from technique instruction, together producing greater functional improvement than either approach alone.
Our resource on best breathing trainer devices provides broader context on the full range of training approaches and device types available.
What Evidence Supports Expiratory Muscle Strength Training?
While most breathing trainer research focuses on inspiratory muscles, expiratory muscle training offers distinct benefits. The 2015 narrative review on functional outcomes of expiratory muscle strength training identified several applications:
Cough effectiveness improves with stronger expiratory muscles, particularly important for patients with neuromuscular conditions or those recovering from surgery who struggle to clear secretions. Generating adequate expiratory pressure during coughing requires abdominal muscle strength that can be enhanced through targeted training.
Speech and communication benefit from sustained expiratory pressure control. Patients with Parkinson disease or other conditions affecting voice production showed improvements in vocal loudness and speech intelligibility following expiratory muscle training that enhanced their ability to generate and sustain subglottal pressure during phonation.
Swallowing safety relates to expiratory muscle function through laryngeal closure coordination. The 2010 Parkinson disease study demonstrated that expiratory muscle strength training reduced aspiration risk by improving the pressure generation needed for effective laryngeal protection during swallowing.
Postural stability gains from expiratory muscle strengthening through enhanced trunk stability and intra-abdominal pressure control during movement and balance challenges.
Clinical breadth: Expiratory muscle training benefits extend beyond respiratory function to include cough effectiveness, speech production, swallowing safety, and postural control, suggesting that devices providing expiratory resistance in addition to inspiratory training may offer broader functional benefits than inspiratory-only devices.
The evidence for expiratory muscle training remains less extensive than inspiratory muscle training research, partly because inspiratory muscle weakness has historically received more attention in respiratory rehabilitation. However, emerging research suggests that addressing both muscle groups produces more comprehensive functional improvements.
How Should COPD Patients Progress Breathing Trainer Resistance?
Clinical trials typically follow structured progression protocols rather than allowing patients to adjust resistance arbitrarily. A 2018 rehabilitation program study examined effectiveness of an inspiration trainer including both supervised exercise sessions and home-based practice.
The program started patients at 30% of their baseline maximum inspiratory pressure. Resistance increased by 5-10% every 1-2 weeks based on individual tolerance and performance. Therapists assessed patients during supervised sessions to ensure proper technique and appropriate challenge level without excessive fatigue or breathlessness.
Patients trained 20-30 minutes daily, 5-6 days per week for 8-12 weeks. The protocol emphasized consistent practice over sporadic intensive sessions. Rest days reduced overtraining risk while maintaining sufficient weekly volume for strength adaptation. Some programs used interval training with rest periods between high-resistance breathing sets.
Proper technique maintenance took priority over resistance progression. If patients developed compensatory breathing patterns or excessive accessory muscle use, therapists reduced resistance and focused on technique refinement before advancing load. Quality of muscle contraction and breathing pattern mattered more than achieving high resistance numbers.
Progression guidance: Starting at 30-40% of maximum inspiratory pressure with gradual increases of 5-10% every 1-2 weeks, maintaining proper breathing technique throughout, training 5-6 days weekly for 20-30 minutes, and working with a respiratory therapist for initial setup and periodic technique checks optimizes respiratory muscle strength gains while reducing improper compensatory patterns.
Patients often want to progress faster than research protocols recommend, but excessive resistance causes fatigue, poor technique, and potentially reduced long-term adherence. The moderate sustained approach produces better outcomes than aggressive rapid progression.
What Are the Limitations of Breathing Trainer Research?
While evidence supports respiratory muscle training benefits, research limitations deserve acknowledgment:
Study populations vary widely, making direct comparisons difficult. Some studies enroll severe COPD patients with marked respiratory muscle weakness, while others include mild-moderate disease. Training effects likely differ across disease severity spectrums.
Training protocols lack standardization. Resistance levels, session duration, training frequency, and program length vary across studies. This heterogeneity makes it challenging to identify optimal training parameters or compare effectiveness across trials.
Outcome measures differ between studies. Some emphasize respiratory muscle strength (maximum inspiratory pressure), others focus on exercise capacity (6-minute walk distance or cycle ergometry), and still others prioritize quality of life or symptom scores. Benefits in one domain may not correlate with improvements in others.
Blinding challenges affect study quality. It is difficult to create convincing sham breathing trainer interventions that patients cannot distinguish from real training. Many studies use low-resistance “sham” training that patients likely recognize as different from active training, potentially affecting placebo responses.
Long-term adherence data remain limited. Most studies examine 8-12 week training programs, but few follow patients for extended periods to determine how long benefits persist after training stops or whether patients maintain practice long-term.
Evidence quality context: While randomized controlled trials support breathing trainer benefits for respiratory muscle strength and some functional outcomes in COPD and other respiratory conditions, research limitations including population heterogeneity, protocol variations, outcome measure inconsistencies, and short follow-up periods mean that individual patient responses may vary from average study results.
For runners and endurance athletes interested in respiratory muscle training applications beyond clinical populations, our guide to lung trainers for runners covers sport-specific considerations.
Can Breathing Trainers Replace Standard COPD Medications?
No evidence supports using breathing trainers as replacements for proven COPD medications. The 1994 rehabilitation trial emphasized that respiratory rehabilitation complements medical management rather than substituting for bronchodilators, inhaled corticosteroids, or other medications that address airway inflammation and obstruction.
Medications and breathing trainers work through different mechanisms:
Bronchodilators relax airway smooth muscle, increasing airflow and reducing obstruction. Breathing trainers cannot directly affect airway caliber or smooth muscle tone.
Inhaled corticosteroids reduce airway inflammation, decreasing mucus production and airway hyperresponsiveness. Respiratory muscle training does not directly affect inflammatory pathways or immune responses.
Supplemental oxygen corrects hypoxemia in patients with severe COPD and low blood oxygen levels. Breathing trainers strengthen muscles but do not increase oxygen content in blood or tissues.
Medical management context: Breathing trainers address respiratory muscle weakness and breathing efficiency, which are important components of COPD disability but do not replace the need for medications that target airway obstruction, inflammation, and gas exchange abnormalities. Optimal COPD management combines appropriate medications with rehabilitation interventions including respiratory muscle training.
Patients should never discontinue prescribed COPD medications to pursue breathing trainer use without explicit guidance from their healthcare provider. Some patients may eventually reduce medication use as their overall fitness and breathing efficiency improve through comprehensive rehabilitation, but these decisions require medical oversight with objective monitoring of lung function and symptoms.
What Safety Considerations Apply to Breathing Trainer Use?
While breathing trainers are generally safe when used appropriately, several precautions apply:
Starting resistance should be conservative, particularly for patients with severe respiratory disease or those new to resistance training. Beginning with excessive resistance can cause respiratory muscle fatigue, excessive breathlessness, or discouragement that reduces adherence.
Proper technique matters. Patients should learn correct breathing patterns before adding resistance. Common errors include using accessory neck muscles excessively, breathing too rapidly, or developing irregular breathing rhythms. Initial instruction from a respiratory therapist helps establish proper technique.
Contraindications include active pneumothorax, recent lung surgery, unstable cardiovascular disease, or uncontrolled asthma exacerbations. Patients with these conditions should not begin respiratory muscle training until medically stable.
Progression should be gradual and based on individual tolerance rather than arbitrary schedules. Patients experiencing increased breathlessness that persists after training sessions, chest pain, dizziness, or other concerning symptoms should reduce resistance and consult their healthcare provider.
Equipment hygiene reduces respiratory infection risk. Breathing trainers should be cleaned thoroughly after each use according to manufacturer instructions, with particular attention to parts that contact saliva or respiratory secretions.
Safety framework: Starting with conservative resistance, learning proper technique with professional instruction, respecting medical contraindications, progressing gradually based on individual response, and maintaining equipment hygiene minimize risks while maximizing benefits from respiratory muscle training devices.
Patients with multiple medical conditions should discuss breathing trainer use with their healthcare provider before beginning training. While respiratory muscle strengthening offers potential benefits, individual medical circumstances may require modifications to standard training protocols.
How Do Breathing Trainers Fit into Comprehensive COPD Management?
The 2017 study examining combined inspiratory muscle training and whole-body endurance training illustrates the multimodal approach that produces best outcomes:
Respiratory muscle training addresses specific inspiratory and expiratory muscle weakness using threshold trainers or other resistance devices. This component targets the muscles of breathing directly.
General exercise training builds cardiovascular fitness and peripheral muscle strength through walking, cycling, or other aerobic activities. COPD patients often experience leg muscle weakness and cardiovascular deconditioning alongside respiratory limitations.
Education teaches disease management including medication use, recognizing exacerbations, energy conservation techniques, and when to seek medical attention. Knowledge empowers patients to manage their condition more effectively.
Nutritional support addresses the malnutrition and muscle wasting common in advanced COPD. Adequate protein and calorie intake supports muscle building from exercise training.
Psychosocial support helps patients manage anxiety, depression, and social isolation that frequently accompany chronic respiratory disease. Group programs provide peer support and accountability.
Smoking cessation for current smokers remains the single most important intervention to slow COPD progression. No amount of rehabilitation can fully compensate for continued smoking damage.
Integrated care model: Breathing trainers contribute most effectively when incorporated into comprehensive COPD management programs that address respiratory muscle weakness, general deconditioning, nutritional status, psychological wellbeing, and ongoing medical optimization, rather than used as standalone interventions divorced from broader disease management.
The evidence consistently shows that multimodal programs produce better outcomes than any single intervention. Patients investing in breathing trainers should simultaneously pursue general exercise, medication optimization, nutritional adequacy, and other components of comprehensive COPD management.
Related Reading
- Best Breathing Trainer Devices: Research-Based Guide to Respiratory Muscle Training
- Airofit Pro Review: Clinical Evidence for Smart Breathing Training
- Respiratory Muscle Training Benefits: What Science Shows
- Breathing Trainers for Athletes: Performance Enhancement Research
- Inspiratory Muscle Trainer vs Spirometer: Understanding the Difference
- Breathing Exercise Devices for Anxiety: Evidence-Based Stress Management
- Best Lung Trainer for Runners: Endurance Performance Guide
References
Langer D, et al. Inspiratory muscle training reduces diaphragm activation and dyspnea during exercise in COPD. Journal of Applied Physiology. 2018. https://pubmed.ncbi.nlm.nih.gov/29543134/
Charususin N, et al. Effects of specific inspiratory muscle training combined with whole-body endurance training program on exercise capacity in patients with chronic obstructive pulmonary disease. European Respiratory Journal. 2017. https://pubmed.ncbi.nlm.nih.gov/34555068/
Reyes A, et al. Respiratory muscle strength and training in stroke and neurology: a systematic review. British Journal of General Practice. 2012. https://pubmed.ncbi.nlm.nih.gov/22568454/
Franca PFA, et al. The effectiveness of physiotherapy in patients with asthma: a systematic review of English language literature. Jornal Brasileiro de Pneumologia. 2008. https://pubmed.ncbi.nlm.nih.gov/23333065/
Ferraro FV, et al. Effects of inspiratory muscle training on postural stability, pulmonary function and maximal inspiratory pressure in Alzheimer’s disease. Brazilian Journal of Physical Therapy. 2019. https://pubmed.ncbi.nlm.nih.gov/30827470/
Morgan MDL. Assessment and management of breathlessness. British Medical Journal. 1985. https://pubmed.ncbi.nlm.nih.gov/3926399/
van der Meijden JC, et al. The role of rehabilitation in the management of late-onset Pompe disease: a narrative review. Orphanet Journal of Rare Diseases. 2019. https://pubmed.ncbi.nlm.nih.gov/30944902/
Singh SJ, et al. Randomised controlled trial of respiratory rehabilitation. British Medical Journal. 1994. https://pubmed.ncbi.nlm.nih.gov/7968075/
Bruton A, et al. Physiotherapy breathing retraining for asthma: a randomised controlled trial. The Lancet Respiratory Medicine. 2017. https://pubmed.ncbi.nlm.nih.gov/29248433/
Pitta F, et al. Walking activity measured by accelerometry during respiratory rehabilitation. European Respiratory Journal. 2003. https://pubmed.ncbi.nlm.nih.gov/14512781/
Huang CH, et al. Inspiratory muscle training facilitates weaning from mechanical ventilation among patients in the intensive care unit: A systematic review. Cardiology. 2015. https://pubmed.ncbi.nlm.nih.gov/26092389/
Alves Machado A, et al. Effectiveness of a respiratory rehabilitation program including an inspiration trainer in hospitalized patients with COVID-19. Heart and Lung. 2024. https://pubmed.ncbi.nlm.nih.gov/38111659/
Sapienza C, et al. Functional outcomes associated with expiratory muscle strength training: narrative review. Journal of Rehabilitation Research and Development. 2015. https://pubmed.ncbi.nlm.nih.gov/25144167/
Troche MS, et al. Aspiration and swallowing in Parkinson disease and rehabilitation with EMST: a randomized trial. Neurology. 2010. https://pubmed.ncbi.nlm.nih.gov/21098406/
Nopp S, et al. Respiratory rehabilitation for Covid-19 related persistent dyspnoea: A one-year follow-up study. Respiratory Medicine. 2021. https://pubmed.ncbi.nlm.nih.gov/34689061/
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



