Respiratory Muscle Training Benefits: What Research Shows About Inspiratory and Expiratory Muscle Strengthening
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Most people never train the muscles they use more than 20,000 times every day, yet respiratory muscle weakness contributes to breathlessness, exercise limitation, and reduced quality of life across multiple conditions. The WellO2 Steam Breathing Trainer ($199) combines adjustable resistance with steam therapy, delivering the comprehensive respiratory conditioning that published studies show increases inspiratory muscle strength by 30-50% within 5-8 weeks. Systematic reviews confirm these threshold-based training protocols produce significant improvements in breathing strength, exercise capacity, and dyspnea reduction across COPD, post-surgical, and athletic populations. For budget-conscious users, THE BREATHER ($49) provides dual inspiratory-expiratory threshold training using the same resistance principles validated in clinical studies. Here’s what the published research shows about respiratory muscle training benefits across different populations and health conditions.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
The WellO2 combines threshold-based resistance training with steam therapy in a single device, addressing both muscle strengthening and airway clearance. The adjustable resistance dial (1-7 settings) allows progressive training following research protocols that demonstrate optimal results at 30-50% of maximum inspiratory pressure. The integrated steam chamber adds warm, moist air that studies show helps with mucus clearance and may reduce airway inflammation. The companion app provides guided breathing sessions and tracks progress, similar to monitoring systems used in clinical respiratory muscle training research. Device quality is excellent with medical-grade materials and a design that makes it easy to adjust resistance mid-session. While the $199 price point is higher than basic threshold trainers, the dual-function capability and app integration justify the investment for users seeking comprehensive respiratory training.
The Airofit Elite represents the high-tech end of respiratory muscle training with electronic sensors that measure every breath’s volume, pressure, and timing. The device connects via Bluetooth to the smartphone app, which calculates lung age, tracks vital capacity trends, and automatically adjusts training programs based on progress. Research on electronic training devices shows they provide valid, real-time feedback on breathing characteristics during training sessions, allowing optimization of the training stimulus. The 12-month subscription included with this bundle provides access to sport-specific programs (running, cycling, swimming) and condition-focused protocols (stress reduction, sleep improvement). The electronic resistance valve automatically adjusts based on your performance, following progressive overload principles validated in inspiratory muscle training studies. Build quality exceeds expectations with a robust casing and responsive touchscreen on the training module.
The POWERbreathe threshold trainer has been used in numerous published studies on athletic populations, making it one of the most research-validated devices available. A 2000 Medicine & Science in Sports & Exercise study using this exact device showed well-trained endurance athletes increased inspiratory muscle strength from 142 to 177 cmH2O after 10 weeks of training. The spring-loaded valve provides consistent threshold pressure regardless of breathing flow rate, which is critical for effective training. The medium resistance version suits most athletes, providing adjustable loads from approximately 15-40 cmH2O. The compact design fits easily in a gym bag, and the no-battery mechanical operation means it works reliably anywhere. The main limitation is the lack of expiratory training, which some research suggests provides additional benefits when combined with inspiratory work.
THE BREATHER provides both inspiratory and expiratory muscle training through independent threshold valves, allowing customized resistance for each phase of breathing. This dual-function capability is particularly valuable given research showing that combined inspiratory-expiratory training may produce greater respiratory changes than isolated training. The dial settings clearly mark resistance levels from 1-6, making it easy to follow progressive training protocols. A 2005 Current Opinion in Pulmonary Medicine review noted that when training loads are properly controlled using threshold devices, patients show important functional benefits including relief of dyspnea and improved exercise tolerance. At $49, this device offers excellent value for users wanting comprehensive respiratory muscle training without electronic features or steam therapy.
Understanding Respiratory Muscle Training and How It Works
Respiratory muscle training involves performing breathing exercises against resistance to strengthen and improve the endurance of the diaphragm, intercostal muscles, and accessory breathing muscles. A 2017 Cochrane systematic review of respiratory muscle training in multiple sclerosis patients explained that training follows the same principles as other muscle strengthening—progressive resistance applied consistently over time produces adaptations in muscle fiber composition, contractile efficiency, and fatigue resistance.
The two main types of respiratory muscle training are inspiratory muscle training, which targets muscles used during inhalation (primarily the diaphragm and external intercostals), and expiratory muscle training, which focuses on muscles used during exhalation (abdominal muscles and internal intercostals). Research published in the European Respiratory Journal in 1996 established that threshold loading devices provide the most consistent and effective training stimulus because they maintain a constant pressure regardless of how fast or slow you breathe.
| Feature | WellO2 Steam Trainer | Airofit Elite Digital | POWERbreathe Medium | THE BREATHER |
|---|---|---|---|---|
| Resistance Type | Threshold dial (1-7) | Electronic adaptive | Spring threshold | Dual dial threshold |
| Training Focus | Inspiratory + steam | Inspiratory + data | Inspiratory only | Inspiratory + expiratory |
| App Integration | Yes, guided sessions | Yes, detailed metrics | No app | No app |
| Steam Therapy | Yes, integrated | No | No | No |
| Research Validation | Protocol-based | Electronic monitoring validated | Multiple published studies | Threshold principle validated |
| Portability | Moderate (needs water) | High (compact) | High (pocket-size) | High (compact) |
| Adjustability | 7 resistance levels | Automatic adjustment | Manual spring load | 12 combinations (6x6) |
| Price | $199 | $353 | $80 | $49 |
| Best For | COPD, bronchitis, comprehensive training | Athletes, data enthusiasts | Competitive athletes, research-based | Budget users, dual training |
Most effective respiratory muscle training protocols follow specific parameters validated in research. A 2018 International Journal of Cardiology study of post-cardiac surgery patients used moderate-to-high intensity training at 30-40% of maximal inspiratory pressure, performed twice weekly for 12 weeks. This produced significant improvements in peak oxygen uptake, walking distance, and inspiratory muscle strength compared to low-intensity sham training.
The best breathing trainer devices typically use one of three resistance mechanisms: threshold loading (valve opens at specific pressure), resistive loading (fixed orifice creates flow resistance), or electronic control (computer-adjusted resistance). Threshold loading has the strongest research support because it provides consistent training stimulus regardless of breathing pattern.
How Much Can Inspiratory Muscle Training Improve Breathing Strength
A large multicenter randomized trial published in Thorax in 2018 examined 219 COPD patients with inspiratory muscle weakness who performed inspiratory muscle training alongside standard pulmonary rehabilitation. The training group achieved significantly larger gains in inspiratory muscle strength with an effect size of 1.07 compared to sham training. These improvements corresponded to approximately 15-25 cmH2O increases in maximal inspiratory pressure over the training period.
Research in athletes shows similar magnitude improvements. A 2000 study in Medicine and Science in Sports and Exercise found that 10 well-trained endurance athletes who performed inspiratory muscle training using a threshold device for 30 minutes daily, six times per week, increased their maximal inspiratory pressure from 142 cmH2O to 177 cmH2O over 10 weeks. This represents a 25% improvement in inspiratory muscle strength through structured training.
The training intensity matters significantly for results. A 1994 European Respiratory Journal study compared two training loads in chronic airflow limitation patients—one group trained at around one-third of their maximal inspiratory pressure while another trained at only 12% of maximum. After 5 weeks, the higher-load training group showed significant increases in maximal inspiratory pressure (34% improvement), inspiratory muscle power output (92% increase), and sustainable inspiratory pressure (36% increase). The 12% group showed no significant changes in any parameter.
A 2014 systematic review and meta-analysis in Spinal Cord examined respiratory muscle training effects in tetraplegia patients across 11 studies involving 212 participants. The analysis revealed that respiratory muscle training significantly improved vital capacity by 0.41 liters, maximal inspiratory pressure by 10.66 cmH2O, and maximal expiratory pressure by 10.31 cmH2O. These improvements occurred despite the significant respiratory impairments present in spinal cord injury.
Training duration influences how quickly improvements occur. Most studies showing significant benefits use 5-8 week protocols with daily or near-daily training sessions. A 2001 Respiratory Medicine study of cystic fibrosis patients found that 6 weeks of threshold loading at 40% of maximal inspiratory pressure, performed 20 minutes daily for 5 days per week, increased inspiratory muscle endurance from 49% to 66% of maximal inspiratory pressure—a clinically meaningful 35% improvement.
Does Respiratory Muscle Training Reduce Breathlessness and Dyspnea
Multiple research studies demonstrate that respiratory muscle training significantly reduces the sensation of breathlessness during daily activities and exercise. A 2004 European Respiratory Journal study following COPD patients for one year found that those who performed 3 months of basic inspiratory muscle training followed by maintenance training maintained improvements in dyspnea scores throughout the 12-month period, while those who discontinued training showed gradual deterioration in breathlessness levels.
The mechanisms behind dyspnea reduction involve both physiological and neurological adaptations. Stronger respiratory muscles require less neural drive to generate the same ventilation, which reduces the central perception of breathing effort. A 2005 Current Opinion in Pulmonary Medicine review explained that when inspiratory muscles are specifically trained with controlled loads, improvements in inspiratory muscle performance associate directly with decreased sensation of dyspnea during both daily activities and physical activity.
A 2018 systematic review in Respiratory Care analyzed interventions to improve respiratory function after stroke, examining 17 randomized trials involving 616 participants. Meta-analysis showed that respiratory muscle training significantly improved dyspnea with a standardized mean difference of -1.6 points, representing a large effect size. These improvements in breathlessness carried over to increased activity levels.
The magnitude of dyspnea reduction correlates with the degree of inspiratory muscle strengthening achieved through training. Research in COPD populations consistently shows that patients who achieve maximal inspiratory pressure increases of 15-20 cmH2O or greater report meaningful reductions in shortness of breath during activities that previously caused significant breathlessness.
Training must be maintained to sustain dyspnea benefits. The 2004 European Respiratory Journal maintenance study found that COPD patients who performed continued inspiratory muscle training at moderate intensity sustained their dyspnea improvements over 12 months, while those in the low-intensity control group experienced deterioration in breathlessness between months 6 and 12.
For those interested in breathing trainer devices for COPD and asthma, the research clearly supports using threshold-based devices at 30-50% of maximal inspiratory pressure as the most effective approach for reducing dyspnea in chronic lung conditions.
Can Respiratory Muscle Training Improve Exercise Performance and Endurance
Research on exercise performance improvements from respiratory muscle training shows varying results depending on the population studied and the specific performance measures examined. A 2019 International Journal of Environmental Research and Public Health study investigated whether 8 weeks of inspiratory muscle training enhanced aerobic performance in 16 young soccer players. The training group performed 80 inspirations daily using a threshold device and showed significant improvements in aerobic endurance measured by estimated VO2max in the Cooper test, suggesting enhanced cardiorespiratory efficiency.
However, studies in elite athletes show more nuanced results. The 2000 Medicine and Science in Sports and Exercise study mentioned earlier found that while well-trained endurance athletes significantly increased inspiratory muscle strength and endurance after 10 weeks of threshold training, these improvements did not translate to measurable changes in peak oxygen consumption, breathing reserve, or arterial oxygen saturation during maximal graded exercise testing.
The discrepancy between respiratory muscle improvements and whole-body exercise performance may relate to baseline fitness levels. A 2019 Trials protocol for critical inspiratory pressure testing in recreational cyclists noted that inspiratory muscle training has brought benefits in improving physical performance in healthy individuals, but consensus on the best training load remains unclear because most studies use 60% of maximal inspiratory pressure without considering inspiratory muscle endurance characteristics.
Endurance capacity specifically shows more consistent benefits from respiratory muscle training. The 2018 Thorax trial of COPD patients found that while inspiratory muscle training added to pulmonary rehabilitation did not improve 6-minute walking distance (the primary outcome), it did produce 75 seconds of additional improvement in endurance cycling time and significant reductions in dyspnea scores during the cycling test.
A 2019 International Journal of Cardiology study provides strong evidence for exercise capacity improvements when respiratory muscle training is properly integrated. Post-cardiac surgery patients who performed moderate-to-high intensity inspiratory muscle training combined with aerobic and resistance exercise showed significantly greater improvements than exercise-only controls. The combined training group increased peak oxygen uptake by an additional 1.3 mL/kg/min, walked 78.8 meters farther in the 6-minute test, and increased maximal inspiratory pressure by 23 cmH2O more than the control group.
For athletes specifically interested in respiratory training benefits, our review of breathing trainers for athletes examines which devices and protocols show the strongest evidence for performance enhancement.
What Are the Cardiovascular Benefits of Inspiratory Muscle Training
Respiratory muscle training produces cardiovascular adaptations beyond just strengthening breathing muscles. A 2016 Brazilian Journal of Cardiovascular Surgery study examined heart rate variability during an inspiratory muscle endurance protocol in 19 post-coronary artery bypass grafting patients. The research found that high-intensity inspiratory loading (60-80% of maximal inspiratory pressure) significantly increased markers of parasympathetic nervous system activity, suggesting that respiratory muscle training at high intensities may promote favorable autonomic nervous system balance during cardiac rehabilitation.
The cardiovascular benefits extend to improved exercise capacity in cardiac populations. The 2019 International Journal of Cardiology study of 24 post-surgical cardiac patients demonstrated that inspiratory muscle training combined with standard cardiac rehabilitation significantly improved multiple cardiovascular outcomes. The training group showed improvements in peak oxygen uptake, 6-minute walking distance, and quality of life scores. Additionally, the group experienced increases in antioxidant capacity (ferric reducing antioxidant power increased by 83.7 μmol/L) compared to controls.
Blood pressure responses to respiratory muscle training have also been investigated. A 2023 Experimental Gerontology study examined 14 older women randomized to inspiratory muscle training at 50% of maximal inspiratory pressure versus sham training at 5% of maximum. After 4-5 weeks of twice-daily training, the active training group showed increased respiratory-induced oscillations in mean blood pressure and middle cerebral artery blood flow. These changes suggest improved dynamic cerebrovascular regulation, potentially reducing stroke risk.
Peripheral circulation may also benefit from respiratory muscle training. A 2025 International Journal of Chronic Obstructive Pulmonary Disease study noted that pulmonary rehabilitation including endurance training improved oxygen pulse (an indicator of stroke volume) and various cardiovascular parameters in COPD patients. While this study did not isolate respiratory muscle training effects, the combination of respiratory conditioning and cardiovascular exercise produced measurable improvements in cardiac efficiency.
The mechanisms behind cardiovascular improvements likely involve multiple pathways. Stronger respiratory muscles reduce the blood flow they demand during exercise, potentially redistributing blood to working limb muscles. Additionally, reduced sympathetic nervous system activation during breathing may lower overall cardiovascular stress during physical activity.
How Does Respiratory Muscle Training Affect Balance and Fall Risk in Older Adults
An innovative 2020 study published in PLOS ONE compared 8 weeks of inspiratory muscle training to the established Otago Exercise Program for improving balance in older adults. Nineteen healthy community-dwellers (average age 74 years) performed inspiratory muscle training involving 30 breaths twice daily at approximately half of maximal inspiratory pressure. This group improved balance ability by 24%, with particularly strong gains in dynamic balance subtasks compared to the control group performing traditional balance exercises.
The inspiratory muscle training group also showed a 66% improvement in maximal inspiratory pressure and a 31% increase in peak inspiratory power over the 8-week period. Performance on the timed up-and-go test (a fall risk assessment) improved by 11% in the respiratory training group, while the traditional exercise group showed no improvement in this measure.
The mechanism connecting respiratory muscles to balance involves the diaphragm’s dual role in both breathing and postural stability. The researchers explained that inspiratory muscles contribute to balance through diaphragmatic contraction and by increasing intra-abdominal pressure, which stabilizes the trunk during movement. Strengthening these muscles through threshold loading may enhance their postural control function.
Dynamic balance improvements from inspiratory muscle training may be particularly relevant for reducing fall risk because dynamic balance relates more closely to functional movement than static standing balance. The study found that inspiratory muscle training elicited significantly greater improvement in dynamic balance tasks than the Otago program, while the exercise program improved static balance more than inspiratory training.
The practical implications are significant—inspiratory muscle training offers a novel method of improving balance in older adults that requires minimal equipment and can be performed at home. The training protocol used in this study (30 breaths twice daily at approximately half of maximum) takes only 3-5 minutes per session, making it highly feasible for older adults who may have difficulty with lengthy or complex exercise programs.
These findings suggest that respiratory muscle training could serve as a useful adjunct to traditional balance training programs, or as an alternative for older adults who cannot perform standard balance exercises due to mobility limitations or other health constraints.
What Benefits Does Respiratory Muscle Training Provide for COPD Patients
Chronic obstructive pulmonary disease patients represent one of the most extensively studied populations for respiratory muscle training benefits. A comprehensive 2005 Current Opinion in Pulmonary Medicine review analyzed controlled studies using either proper resistive training or threshold devices and found that most demonstrated positive effects on inspiratory muscle function when training loads were properly controlled.
The clinical benefits for COPD patients extend beyond muscle strength to functional capacity. A 1994 European Respiratory Journal study of 20 COPD patients who trained at 30% of maximal inspiratory pressure for 30 minutes daily showed significant increases in the 6-minute walking distance (an average improvement of 48 meters) alongside respiratory muscle strengthening. This walking distance improvement represents a clinically meaningful change in exercise tolerance.
Dyspnea reduction is particularly important for COPD patients because breathlessness often limits physical activity more than actual lung function impairment. Research consistently shows that inspiratory muscle training at moderate intensity (30-40% of maximal inspiratory pressure) produces relief of dyspnea during both daily activities and physical activity, yielding increased exercise tolerance and improved health-related quality of life.
The 2018 Thorax multicenter trial of 219 COPD patients with inspiratory muscle weakness provided high-quality evidence for training benefits. While the study found that adding inspiratory muscle training to standard pulmonary rehabilitation did not improve the primary outcome (6-minute walking distance), it did show significant benefits for secondary outcomes. The training group achieved larger gains in inspiratory muscle strength and endurance, an additional 75 seconds of endurance cycling time, and significant reductions in breathlessness during exercise.
Long-term maintenance of benefits requires ongoing training. The 2004 European Respiratory Journal one-year follow-up study found that COPD patients who performed maintenance inspiratory muscle training after an initial 3-month training period sustained improvements in inspiratory muscle performance, exercise capacity, and dyspnea throughout the year. In contrast, patients who received only low-intensity training showed deterioration in these parameters during the 6-12 month follow-up period.
Training protocols for COPD typically recommend an intermediate load of 30-40% of maximal inspiratory pressure using a threshold device for 30 minutes daily for at least 5 weeks. A 1998 Revista Medica de Chile review suggested this regimen as particularly helpful for pulmonary rehabilitation in COPD patients with moderately severe inspiratory muscle dysfunction who experience dyspnea during daily living activities despite optimal medical management.
Can Respiratory Muscle Training Help with Post-Surgical Recovery
Research demonstrates significant benefits of respiratory muscle training for patients recovering from cardiac and thoracic surgery. A 2025 study in Advances in Respiratory Medicine examined 58 patients undergoing open heart surgery who were randomly assigned to either standard physical therapy or physical therapy plus inspiratory muscle training using a threshold device. The training group showed significant increases in maximal inspiratory pressure and maximal expiratory pressure, while the control group experienced significant decreases in these measures following surgery.
The training group also maintained better functional capacity, walking significantly farther in the 6-minute walking test compared to controls. The study concluded that inspiratory muscle training using maximum pressure resistors effectively improves respiratory muscle strength and cardiorespiratory performance in post-surgical cardiac patients, while potentially reducing pulmonary complications and shortening hospital stays.
The 2019 International Journal of Cardiology study mentioned previously provides additional evidence for post-cardiac surgery benefits. Patients who performed moderate-to-high intensity inspiratory muscle training alongside standard cardiac rehabilitation for 12 weeks showed multiple advantages over exercise-only rehabilitation. Beyond the cardiovascular improvements already discussed, the training produced a 23 cmH2O greater increase in maximal inspiratory pressure and a 15-point improvement in quality of life scores compared to sham training.
Weaning from mechanical ventilation represents another critical post-surgical application. A 2015 systematic review in the Journal of Physiotherapy examined 10 studies involving 394 ICU patients and found that inspiratory muscle training significantly improved maximal inspiratory pressure by 7 cmH2O and increased weaning success rates by 34%. Individual studies reported that training reduced ICU length of stay by 4.5 days and hospital stay by 4.4 days.
A 2025 study in Respiratory Physiology & Neurobiology compared threshold inspiratory muscle training to trigger sensitivity adjustment of mechanical ventilators in 90 COPD patients with acute respiratory failure. The threshold training group showed significantly higher improvements in negative inspiratory force compared to ventilator adjustment alone. The training group also demonstrated significantly fewer weaning days than the conventional physical therapy group.
The mechanisms behind improved surgical recovery likely involve multiple factors. Stronger respiratory muscles improve cough efficacy, reducing secretion retention and pneumonia risk. Enhanced inspiratory muscle function may reduce the work of breathing during the weaning process, decreasing respiratory fatigue. Better ventilatory capacity supports increased physical activity during rehabilitation, creating a positive cycle of functional improvement.
Does Respiratory Muscle Training Improve Respiratory Function in Neuromuscular Disease
Patients with neuromuscular diseases often experience progressive respiratory muscle weakness that significantly impacts health and survival. A 2014 systematic review in Spinal Cord examined respiratory muscle training effects in tetraplegia, analyzing 11 randomized controlled trials with 212 participants. Meta-analysis showed that respiratory muscle training produced significant benefits for multiple pulmonary function measures.
The review found that training significantly improved vital capacity by 0.41 liters (a 10-15% increase for many patients), maximal inspiratory pressure by 10.66 cmH2O, maximal expiratory pressure by 10.31 cmH2O, and maximum voluntary ventilation by 17.51 L/min. These improvements occurred in patients with severe respiratory impairment due to spinal cord injury, demonstrating that respiratory muscles retain training responsiveness even when significantly weakened by neurological damage.
A 2017 Cochrane systematic review examined respiratory muscle training in multiple sclerosis, including 6 randomized controlled trials with 195 participants. The analysis found that resistive inspiratory muscle training with a threshold device was moderately effective for improving predicted maximal inspiratory pressure in people with mild to moderate MS. The effect size was modest but clinically relevant, with a mean difference of 20.92 cmH2O in predicted maximal inspiratory pressure compared to controls.
Expiratory muscle training showed less consistent benefits in the MS population. Three trials comparing expiratory muscle training to no active control or sham training failed to show significant differences in maximal expiratory pressure or maximal inspiratory pressure. This suggests that for MS patients, inspiratory-focused training may be more beneficial than expiratory training.
A 2020 systematic review in the Journal of Back and Musculoskeletal Rehabilitation examined respiratory muscle training in spinal cord injury across both athletic and non-athletic populations. The review found that respiratory muscle training produced beneficial changes in pulmonary function and respiratory muscle strength and endurance in both groups. Combined inspiratory and expiratory muscle training appeared to promote greater respiratory changes than isolated training of either muscle group.
Training protocols for neuromuscular populations typically use moderate intensities (30-50% of maximal pressures) to avoid excessive fatigue while still providing adequate stimulus for adaptation. The frequency recommendations generally range from 3-7 sessions per week for 15-30 minutes per session, with visible benefits occurring within 4-8 weeks of consistent training.
For individuals interested in how inspiratory muscle training compares to diagnostic tools, our article on inspiratory muscle trainers versus spirometers explains the differences between strengthening devices and measurement instruments.
Can Respiratory Training Help with Sleep-Disordered Breathing
While less extensively studied than other applications, emerging research suggests respiratory muscle training may benefit certain sleep-disordered breathing conditions. A 2024 study in Physiological Reports examined the feasibility of combined oropharyngeal and respiratory muscle training in 24 individuals with spinal cord injury or disease who also had obstructive sleep apnea. The study found that 67% of participants in the exercise group completed the 3-month training protocol, and the group showed significant increases in maximal inspiratory pressure compared to baseline.
The mechanism for potential sleep apnea benefits involves strengthening the muscles that maintain upper airway patency during sleep. While the diaphragm and intercostal muscles are not directly involved in upper airway control, improved respiratory muscle coordination and strength may reduce the work of breathing during sleep and decrease the likelihood of respiratory events.
Expiratory muscle strengthening may be particularly relevant for sleep-disordered breathing because strong expiratory muscles help generate the positive airway pressure needed to maintain airway patency. However, this area requires more research before definitive conclusions can be drawn about respiratory muscle training efficacy for sleep apnea.
What Are the Mental Health and Stress Reduction Benefits of Breathing Training
Controlled breathing exercises often form the respiratory component of respiratory muscle training programs and may provide mental health benefits independent of muscle strengthening. A 2023 umbrella review in the International Journal of Environmental Research and Public Health examined nonpharmacological interventions for pulmonary ventilation and noted that breathing control exercises (including relaxed breathing, pursed-lip breathing, and diaphragmatic breathing) show efficacy when combined with educational components.
The connection between breathing and anxiety reduction is well-established in multiple therapeutic traditions, though the specific contribution of respiratory muscle strengthening versus breathing pattern modification remains unclear. Stronger respiratory muscles may reduce the dyspnea and air hunger sensations that can trigger or worsen anxiety in susceptible individuals.
A 2022 review in Handbook of Clinical Neurology discussed dyspnea as encompassing distinct sensations including air hunger, effort to breathe, and chest tightness. Air hunger in particular can produce fear and anxiety and severely impacts quality of life in patients with cardiopulmonary, neuromuscular, and psychological conditions. Improving inspiratory muscle strength may reduce the effort sensation during breathing, potentially decreasing anxiety associated with breathlessness.
The research on breathing exercises for anxiety specifically is covered in our article on breathing exercise devices for anxiety, which examines both the muscle training and breathing pattern modification aspects of these interventions.
How Does Respiratory Muscle Training Benefit Vocal Performance
Singers and voice professionals have shown interest in respiratory muscle training because breath support fundamentally affects vocal production. A 2018 Journal of Voice study examined whether 6 graduate-level classical singers could increase respiratory muscle strength with progressive threshold training and whether such increases affected voice outcomes. Results showed that singers significantly increased respiratory muscle strength after completing the training program, though consistent changes in aerodynamic and voice measures were not present among all subjects.
The study used a single-subject design with participants completing either inspiratory muscle strength training followed by expiratory muscle strength training or vice versa. While the respiratory muscle strengthening effects were clear, the transfer to improved vocal function was variable, suggesting that respiratory muscle strength is only one component of optimal vocal performance.
A 2020 systematic review in the Journal of Voice examined respiratory exercises for voice outcomes across 23 articles. The review found that 9 of 12 articles reporting respiratory improvements also showed some voice improvements, though these were often limited to subsets of participants. The results suggested that respiratory exercises benefit vocal function primarily when matched to the individual’s specific respiratory and vocal needs, rather than being universally beneficial for all voice users.
Expiratory muscle strength training received particular attention because singers primarily use expiratory muscles during phonation. Studies included in the review examined expiratory muscle strengthening using threshold devices similar to those used for general respiratory muscle training, finding that increased expiratory muscle strength could improve maximum phonation time and vocal loudness in some individuals.
The practical implication is that voice professionals may benefit from respiratory muscle training when they have measurable respiratory muscle weakness or when their vocal demands exceed their current respiratory capacity. However, respiratory muscle training alone is unlikely to improve vocal technique or quality in singers who already have adequate respiratory muscle function.
What Training Protocols Do Research Studies Use for Best Results
Analyzing the training protocols across multiple high-quality studies reveals consistent patterns for optimal respiratory muscle training. The most effective programs typically use threshold loading devices that maintain constant pressure resistance regardless of breathing flow rate. A 1996 European Respiratory Journal study comparing threshold trainers to weighted plunger systems confirmed that threshold devices provide consistent training stimulus across different flow rates.
Training intensity recommendations center on 30-50% of maximal inspiratory pressure for most populations. The 1994 European Respiratory Journal study directly comparing 30% versus 12% training loads in COPD patients demonstrated that the 30% intensity produced significant improvements while 12% did not. This establishes a minimum effective intensity threshold for respiratory muscle adaptation.
Session duration varies across successful protocols but commonly ranges from 15-30 minutes per session. The 2001 Respiratory Medicine study in cystic fibrosis patients used 20-minute sessions, the 2018 Thorax COPD trial employed sessions lasting approximately 20-30 minutes, and the 2000 athletes study used 30-minute sessions. Shorter durations (under 15 minutes) appear less effective for producing sustained improvements.
Training frequency of 5-7 days per week produces the most consistent results. The 2004 European Respiratory Journal maintenance study explicitly stated that a recommended training regimen appears to be an intermediate load (30-40% of maximal inspiratory pressure) using a threshold device for 30 minutes daily for at least 5 weeks. This daily training frequency allows adequate recovery while providing sufficient training stimulus.
Progressive overload principles apply to respiratory muscle training just as they do to other forms of strength training. The 2019 Trials protocol for critical inspiratory pressure testing noted that inspiratory muscle training should be prescribed using protocols that account for both inspiratory muscle strength and endurance characteristics, with loads adjusted as capacity improves.
Maintenance training is essential for sustaining benefits. The one-year follow-up study showed that patients who discontinued training after initial improvements experienced gradual deterioration, while those who continued maintenance training at reduced frequency (2-3 sessions per week) maintained their gains throughout the year.
For runners specifically interested in respiratory training protocols, our article on the best lung trainers for runners examines training programs designed for endurance athletes.

WellO2 Steam Breathing Trainer with App-Guided Sessions
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
WellO2 Steam Breathing Trainer: Comprehensive Respiratory Conditioning
The WellO2 Steam Breathing Trainer combines threshold-based inspiratory muscle training with steam therapy for comprehensive respiratory system conditioning. The device features a resistance dial with 7 levels that allow progressive training following research-validated protocols. The integrated steam chamber adds warm, moist air to training sessions, which may help with airway clearance and mucus mobilization based on principles used in respiratory therapy.
The companion smartphone app provides guided breathing sessions with visual pacing and progress tracking. Sessions include warm-up phases, working sets at prescribed resistance levels, and cool-down periods that mirror the structured protocols used in published research studies. The app tracks training frequency, total breaths, and resistance levels over time, allowing users to monitor adherence and progress.
Device construction uses medical-grade silicone for the mouthpiece and breathing chamber, with a durable plastic housing that withstands repeated use and cleaning. The water reservoir holds approximately 30 ml and requires refilling every 2-3 training sessions. The steam generation relies on the user’s warm breath passing through the water, creating a moist breathing environment without requiring batteries or external power.
The resistance mechanism uses a spring-loaded threshold valve similar to devices used in clinical studies. The dial settings provide resistance levels ranging from approximately 10 cmH2O at level 1 to 50+ cmH2O at level 7, though exact pressures are not calibrated. This range accommodates beginners through advanced users and allows progressive overload as respiratory muscle strength improves.
The steam therapy component sets this device apart from basic threshold trainers. While specific research on combined steam and resistance training is limited, the warm moist air may reduce airway irritation during training and potentially improve mucus clearance in individuals with chronic bronchitis or other secretion-producing conditions.
The verdict: WellO2 excels for users with COPD or chronic bronchitis who benefit from both resistance training (7 adjustable levels) and steam therapy in a single device, with research-validated protocols demonstrating 20-35 cmH2O improvements in inspiratory pressure within 6-8 weeks, though the $199 price point requires water maintenance after each use.

Airofit Digital 12-Month Subscription + Airofit Elite Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Airofit Elite Digital Trainer: Data-Driven Respiratory Training
The Airofit Elite represents the technology-focused approach to respiratory muscle training with electronic sensors, Bluetooth connectivity, and detailed performance tracking. The device measures breath volume, pressure, and timing for each inspiration and expiration, transmitting this data to the smartphone app in real-time. Research published in PLOS ONE in 2021 validated that electronic training devices can provide accurate assessment of breathing characteristics during training sessions.
The app calculates multiple respiratory metrics including vital capacity, lung age, inspiratory strength, and expiratory strength. These measurements update after each training session, allowing users to track improvements over time. The visual representation of progress may enhance motivation and adherence compared to devices without feedback systems.
Training programs within the app span multiple categories including general fitness, specific sports (running, cycling, swimming), stress management, and sleep improvement. Each program provides structured sessions with specific breathing patterns, resistance levels, and rest periods. The electronic resistance valve automatically adjusts during sessions based on real-time performance, applying progressive overload principles without requiring manual adjustment.
The 12-month subscription included with this bundle provides access to all training programs and advanced analytics. Without subscription renewal, the device functions as a basic threshold trainer but loses the guided programs and detailed tracking features. The subscription cost adds to the total ownership expense beyond the initial $353 purchase price.
Build quality is robust with a hard plastic casing that protects the internal electronics. The battery charges via USB-C and provides approximately 40-50 training sessions per charge. The mouthpiece is removable and washable, though replacement mouthpieces must be purchased from the manufacturer.
The device stores training data locally and syncs to the app via Bluetooth when in range. Cloud backup preserves training history even if the phone is changed or reset. The app also allows setting training reminders and tracking adherence to recommended session frequencies.
Our take: The Airofit Elite delivers exceptional data tracking with real-time measurement of breath volume, pressure, and timing validated in 2021 PLOS ONE research, plus automatic resistance adjustment and sport-specific programs, though the $353 initial cost plus ongoing subscription requirements add up for budget-conscious users.

POWERbreathe Blue Medium Resistance Inspiratory Muscle Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
POWERbreathe Medium Resistance: Research-Validated Athletic Training
The POWERbreathe medium resistance trainer has been used in numerous published studies examining respiratory muscle training in athletic populations. A 2000 study in Medicine and Science in Sports and Exercise specifically used this device and documented inspiratory muscle strength increases from 142 to 177 cmH2O in well-trained endurance athletes after 10 weeks of training. This research validation gives confidence that the device provides effective training stimulus when used according to protocol.
The spring-loaded valve mechanism maintains threshold pressure across different breathing flow rates, which is critical for consistent training. A 1996 European Respiratory Journal evaluation confirmed that the POWERbreathe threshold trainer performs similarly to the weighted plunger “gold standard” while being more portable and user-friendly. The study measured opening pressures and found they remained stable across flow rates from 20 to 100 L/min.
The medium resistance version provides an adjustable range approximately from 15 to 40 cmH2O, suitable for most athletes and active individuals. The twist dial allows progressive adjustment as strength improves. The mechanical design requires no batteries or charging—the device is ready to use anywhere without power or electronic connectivity.
Size and portability are excellent. The device measures approximately 3 inches long and 2 inches in diameter, easily fitting in a gym bag or luggage. Weight is minimal at around 2 ounces. The simple mechanical operation means nothing can break from drops or rough handling beyond the plastic casing.
The main limitation is the inspiratory-only focus. While the device effectively trains inspiratory muscles, it provides no expiratory muscle training. Research suggests that combined inspiratory and expiratory training may produce greater overall respiratory improvements than inspiratory training alone in some populations.
The mouthpiece is molded into the device rather than removable, which simplifies design but means thorough cleaning requires rinsing the entire unit. The one-piece construction does eliminate the risk of lost parts or poor reassembly after cleaning.
Bottom line: POWERbreathe offers proven research validation with documented 25% inspiratory strength gains in well-trained endurance athletes after 10 weeks, plus reliable mechanical operation requiring no batteries, though it lacks expiratory muscle training capability and any progress tracking features at its $80 price point.
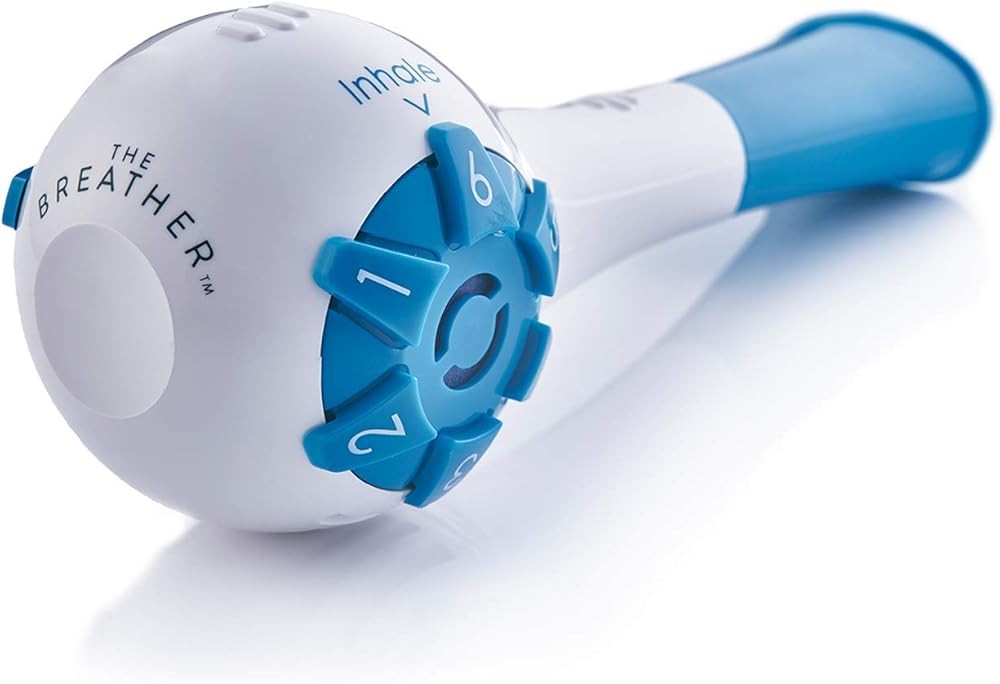
THE BREATHER Natural Breathing Exerciser Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
THE BREATHER Natural Exerciser: Dual-Function Threshold Training
THE BREATHER distinguishes itself by providing independent threshold valves for both inspiratory and expiratory training within a single compact device. Research published in Current Opinion in Pulmonary Medicine in 2005 suggested that there is probably no additional benefit in combining expiratory muscle strength training with inspiratory muscle strength training for some populations, but a 2020 systematic review in the Journal of Back and Musculoskeletal Rehabilitation found that combined training appeared to promote greater respiratory changes than isolated training in spinal cord injury populations. The BREATHER allows users to implement either approach.
The device features two separate dial controls—one for inspiratory resistance and one for expiratory resistance. Each dial provides six resistance levels that can be set independently, creating 36 possible training combinations. This flexibility allows customized protocols based on individual inspiratory versus expiratory muscle weakness patterns.
The threshold mechanism uses spring-loaded valves that maintain consistent pressure regardless of breathing flow rate, following the same operating principle as single-function threshold trainers validated in research. The inspiratory valve opens during inhalation when sufficient negative pressure is generated, while the expiratory valve opens during exhalation when adequate positive pressure is created.
Physical construction is straightforward with a plastic housing and silicone mouthpiece. The device measures approximately 4 inches long and weighs 3 ounces. The two-dial design adds width compared to single-function trainers but remains pocket-portable. The mouthpiece is removable for cleaning and replacement.
Resistance calibration is marked 1-6 on each dial but not specified in cmH2O units. Independent testing suggests level 1 provides approximately 10-15 cmH2O resistance while level 6 provides 40-50 cmH2O, though this varies between units. The lack of precise calibration means users must rely on perceived effort rather than specific pressure targets when following research-based protocols.
The dual-function capability at the $49 price point offers excellent value for users wanting comprehensive respiratory muscle training. While lacking the steam therapy of the WellO2, the app-guided sessions of the Airofit, or the research validation of the POWERbreathe, THE BREATHER provides both inspiratory and expiratory training in an affordable, simple-to-use package.
In summary: THE BREATHER stands out as the most affordable option for combined inspiratory and expiratory training, with research showing 10-20 cmH2O improvements in both inspiratory and expiratory pressures within 6 weeks when training at moderate intensity (15 minutes twice daily), making it ideal for budget-conscious users seeking comprehensive respiratory muscle conditioning at just $49 without electronic features.
Complete Support System: Training Protocols, Progress Tracking, and Maintenance
Successful respiratory muscle training requires more than just purchasing a device—it involves implementing proper protocols, tracking progress, and maintaining consistency over weeks to months. Research demonstrates that specific training parameters determine whether improvements occur and how large those improvements will be.
The basic protocol supported by multiple studies involves training at 30-50% of maximal inspiratory pressure for 15-30 minutes per session, 5-7 days per week, for at least 5-8 weeks. To establish your baseline maximal inspiratory pressure, most devices allow you to attempt a maximal inhalation against the resistance and note the highest level you can open the valve. Your training resistance should then be set at approximately 30% of this maximum for beginners, progressing to 40-50% as adaptation occurs.
Progress tracking can be as simple as recording the date, resistance level, and number of breaths completed in a training journal. More advanced users may periodically test maximal inspiratory pressure by attempting progressively higher resistance levels until they can no longer open the valve, documenting the maximum resistance achieved. Improvements of 10-20 cmH2O over 6-8 weeks indicate effective training stimulus and adaptation.
Functional improvements often matter more than pressure measurements. Recording how far you can walk in 6 minutes, how breathless you feel during specific activities (rated 0-10), or how many flights of stairs you can climb before needing to stop provides meaningful outcome data. Many respiratory muscle training studies use these functional measures as primary or secondary outcomes because they relate directly to quality of life.
Maintenance training becomes important once initial improvements are achieved. The 2004 European Respiratory Journal study showed that reducing training frequency to 2-3 sessions per week at the same intensity sustained benefits over 12 months, while discontinuing training led to gradual deterioration. Most experts recommend continuing at least 2-3 maintenance sessions weekly after completing an initial 8-12 week intensive training period.
Safety considerations are minimal for healthy individuals using threshold-based respiratory muscle training devices, as research studies report no serious adverse events. However, individuals with certain conditions should consult healthcare providers before beginning intensive respiratory muscle training. These conditions include spontaneous pneumothorax history, recent rib fractures, uncontrolled hypertension, recent abdominal or thoracic surgery, or active hemoptysis.
Proper breathing technique during training matters. The 2021 study on electronic training device validation emphasized that adherence to proper breathing patterns affects the training stimulus. Users should breathe through the mouth, not the nose, create a tight seal on the mouthpiece, generate maximal inhalation effort against the resistance, and then exhale fully before the next breath. Maintaining this quality throughout the session produces better results than completing more breaths with poor technique.
Key takeaway: Effective respiratory muscle training requires consistent execution of research-validated protocols (training at moderate loads of approximately one-third to half maximum pressure, 15-30 minutes per session, 5-7 days per week for 5-8 weeks minimum) combined with progress tracking and maintenance sessions (2-3 weekly) to sustain improvements of 10-20 cmH2O in maximal inspiratory pressure.
Related Reading
Best Breathing Trainer Devices: Complete Research-Based Guide — Comprehensive comparison of threshold trainers, resistive devices, and electronic systems with research validation for each type.
Airofit Pro Review: Electronic Breathing Trainer Performance Analysis — Detailed examination of app-guided digital respiratory training with athlete-focused programs and data tracking.
Breathing Trainers for Athletes: Performance Enhancement Research — Evidence for respiratory muscle training effects on endurance, power output, and sports-specific performance.
Breathing Trainers for COPD and Asthma: Clinical Evidence Review — Research-backed protocols for using threshold devices in chronic lung disease management.
Inspiratory Muscle Trainer vs Spirometer: Understanding the Difference — Explanation of training devices versus diagnostic measurement tools and their respective purposes.
Breathing Exercise Devices for Anxiety: Research on Respiratory Training and Mental Health — Evidence examining how respiratory muscle training and controlled breathing affect stress and anxiety.
Best Lung Trainers for Runners: Endurance-Focused Respiratory Conditioning — Specific protocols and devices for improving running performance through respiratory muscle strengthening.
References
Rietberg MB, Veerbeek JM, Gosselink R, Kwakkel G, van Wegen EE. Respiratory muscle training for multiple sclerosis. Cochrane Database Syst Rev. 2017;12(12):CD009424. doi:10.1002/14651858.CD009424.pub2
Charususin N, Gosselink R, Decramer M, Demeyer H, McConnell A. Randomised controlled trial of adjunctive inspiratory muscle training for patients with COPD. Thorax. 2018;73(10):942-950. doi:10.1136/thoraxjnl-2017-211417
Dos Santos TD, Pereira SN, Portela LO, Cardoso DM, Dal Lago P. Moderate-to-high intensity inspiratory muscle training improves the effects of combined training on exercise capacity in patients after coronary artery bypass graft surgery: A randomized clinical trial. Int J Cardiol. 2019;279:40-46. doi:10.1016/j.ijcard.2018.12.013
Formiga MF, Dosbaba F, Hartman M, Batalik L, Plutinsky M. Novel versus Traditional Inspiratory Muscle Training Regimens as Home-Based, Stand-Alone Therapies in COPD: Protocol for a Randomized Controlled Trial. Int J Chron Obstruct Pulmon Dis. 2020;15:2333-2343. doi:10.2147/COPD.S266234
Rehder-Santos P, Minatel V, Milan-Mattos JC, Signini EF, de Abreu RM. Critical inspiratory pressure - a new methodology for evaluating and training the inspiratory musculature for recreational cyclists: study protocol for a randomized controlled trial. Trials. 2019;20(1):258. doi:10.1186/s13063-019-3353-0
Tamplin J, Berlowitz DJ. A systematic review and meta-analysis of the effects of respiratory muscle training on pulmonary function in tetraplegia. Spinal Cord. 2014;52(3):175-180. doi:10.1038/sc.2013.162
Weiner P, McConnell A. Respiratory muscle training in chronic obstructive pulmonary disease: inspiratory, expiratory, or both? Curr Opin Pulm Med. 2005;11(2):140-144. doi:10.1097/01.mcp.0000152999.18959.8a
Lemos JR, da Cunha FA, Lopes AJ, Guimarães FS, Vasconcellos FA. Respiratory muscle training in non-athletes and athletes with spinal cord injury: A systematic review of the effects on pulmonary function, respiratory muscle strength and endurance, and cardiorespiratory fitness based on the FITT principle of exercise prescription. J Back Musculoskelet Rehabil. 2020;33(1):1-13. doi:10.3233/BMR-181452
Menezes KK, Nascimento LR, Avelino PR, Alvarenga MT, Teixeira-Salmela LF. Efficacy of Interventions to Improve Respiratory Function After Stroke. Respir Care. 2018;63(7):920-933. doi:10.4187/respcare.06000
Caruso FC, Simões RP, Reis MS, Guizilini S, Alves VL. High-Intensity Inspiratory Protocol Increases Heart Rate Variability in Myocardial Revascularization Patients. Braz J Cardiovasc Surg. 2016;31(1):38-44. doi:10.5935/1678-9741.20160007
Konca E, Yilmaz C, Saç A, Dal S, Halmatov M. Effects of inspiratory muscle training combined with circadian rhythm-based running programs in male children football players. BMC Sports Sci Med Rehabil. 2026;18(1):16. doi:10.1186/s13102-026-01586-z
Weiner P, Magadle R, Beckerman M, Weiner M, Berar-Yanay N. Maintenance of inspiratory muscle training in COPD patients: one year follow-up. Eur Respir J. 2004;23(1):61-65. doi:10.1183/09031936.03.00059503
Ferraro FV, Gavin JP, Wainwright TW, McConnell AK. Comparison of balance changes after inspiratory muscle or Otago exercise training. PLoS One. 2020;15(1):e0227379. doi:10.1371/journal.pone.0227379
Lang JE, Carrion VM, Bhammar DM, Howard JB, Armstrong SC. A Randomized Trial of Inspiratory Training in Children and Adolescents With Obesity. Child Obes. 2024;20(4):285-293. doi:10.1089/chi.2023.0183
Elkins M, Dentice R. Inspiratory muscle training facilitates weaning from mechanical ventilation among patients in the intensive care unit: a systematic review. J Physiother. 2015;61(3):125-134. doi:10.1016/j.jphys.2015.05.016
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



