Cold Laser vs Red Light Therapy: Which Works Better for Pain Relief?
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Cold laser therapy and red light therapy both use specific wavelengths of light to reduce pain and promote healing, but many people don’t realize these are actually different technologies with distinct advantages. The EMR-TEK Firewave Red Light Panel ($174) delivers 660nm red and 850nm near-infrared LED light across a large treatment area, making it the best choice for whole-body pain relief and recovery based on published photobiomodulation research. A 2018 comparative review in Photobiomodulation, Photomedicine, and Laser Surgery found that LED panels produce therapeutic benefits equivalent to coherent lasers while offering superior safety profiles, larger treatment coverage, and lower cost per milliwatt. For targeted treatment on a budget, the Cold Laser Therapy Device ($99) provides focused 650nm laser light with handheld portability. Here’s what the published research shows about choosing between these two photobiomodulation technologies.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
What’s the Difference Between Cold Laser and Red Light Therapy?
Cold laser therapy and red light therapy represent two distinct approaches to photobiomodulation—the process of using specific wavelengths of light to trigger beneficial cellular responses. Understanding the technical differences between these technologies helps you choose the right option for your specific needs.
Cold laser therapy, also called low-level laser therapy (LLLT), uses coherent laser diodes that produce monochromatic light in a collimated beam. The coherence means all photons travel in phase with each other, creating a focused beam with minimal divergence. These devices typically use Class 3B lasers producing 5-500 milliwatts of power in wavelengths from 630-850nm. The focused beam creates higher power density (irradiance) measured in milliwatts per square centimeter, allowing targeted treatment of specific points or small areas.
Red light therapy uses non-coherent light-emitting diodes (LEDs) that produce polychromatic light spreading across a wider spectral range. LED panels emit diffused light that diverges from the source, covering larger treatment areas with lower power density. Modern therapeutic LED panels typically combine 660nm red light with 850nm near-infrared light, delivering 100-300+ watts total power distributed across panel surfaces measuring 12x12 inches or larger.
| Feature | Cold Laser (LLLT) | Red Light LED |
|---|---|---|
| Light Source | Coherent laser diode | Non-coherent LED array |
| Beam Type | Collimated, focused | Diffused, divergent |
| Power Density | 10-100+ mW/cm² | 10-50 mW/cm² |
| Treatment Area | Small, targeted (1-5 cm²) | Large, whole-body (200+ cm²) |
| Wavelengths | Single wavelength (monochromatic) | Dual wavelength combinations |
| Coherence | Yes (in-phase photons) | No (random phase) |
| Safety Class | Class 3B laser (eye protection required) | Class 1 or 2 (no protection needed) |
| Cost Range | $99-$5,000+ | $100-$500 |
| Session Time | 2-5 minutes per point | 10-20 minutes whole body |
| Best For | Targeted pain, trigger points | Whole-body recovery, large areas |
The key distinction lies in coherence and beam characteristics rather than therapeutic effectiveness. A 2018 review by Heiskanen and Hamblin published in Photobiomodulation, Photomedicine, and Laser Surgery examined whether coherence provides therapeutic advantages. The researchers analyzed multiple studies comparing laser and LED sources and found both produce similar therapeutic benefits when appropriate dosimetric parameters are applied. The review concluded that advantages of LEDs include no laser safety considerations, ease of home use, larger treatment areas, wearable device possibilities, and lower cost per milliwatt.
Research shows coherence becomes irrelevant once photons penetrate tissue because biological scatter immediately destroys phase relationships. What matters for photobiomodulation is delivering sufficient photons at therapeutic wavelengths to target chromophores like cytochrome c oxidase in mitochondria. Both technologies accomplish this goal through different engineering approaches.
A 2020 wound phototherapy review by Bolton compared laser and LED effectiveness for tissue healing. The analysis found that wavelength determines penetration depth regardless of coherence — red light reaches shallow tissue layers while near-infrared reaches deeper structures from both source types. Few adequately powered double-blind randomized controlled trials exist comparing energy dose-response between coherent and non-coherent sources, but available evidence shows equivalent outcomes.
The practical implications center on treatment coverage and safety. Cold laser devices excel for addressing specific trigger points, small joints, or localized pain areas where focused beam delivery concentrates energy. Red light therapy panels excel for addressing larger body regions, multiple areas simultaneously, or whole-body applications where broad coverage matters more than power density.
Bottom line: Both technologies trigger the same photobiomodulation mechanisms when delivering 4-10 J/cm² at 630-850nm wavelengths, with research showing equivalent pain reduction of 1.3-1.7 points. Choose based on area size and safety rather than coherence claims.
The EMR-TEK Firewave Red Light Panel delivers dual-wavelength photobiomodulation through a combination of 660nm red and 850nm near-infrared LEDs arranged in a large panel format. This device represents the optimal balance of power output, treatment coverage, and cost for home users seeking whole-body pain relief and recovery benefits.
The panel measures approximately 12x12 inches and contains over 200 individual LED diodes producing total power output exceeding 200 watts. The dual-wavelength design targets both surface tissues (660nm) and deeper structures (850nm) simultaneously. At recommended distance of 6-12 inches from skin, the device delivers irradiance of 40-80 mW/cm² depending on positioning, allowing 10-15 minute sessions to achieve therapeutic fluence of 24-72 J/cm².
These parameters align with published photobiomodulation research showing optimal effectiveness at therapeutic fluence levels for pain conditions. A 2019 review on musculoskeletal applications by Gendron and Hamblin noted the field is trending toward higher power devices for better outcomes, with clinical studies showing 30-60% pain reduction across various conditions using both laser and LED sources.
The non-coherent LED design eliminates laser safety concerns that require eye protection with Class 3B devices. The panel can apply to large body areas like entire back, both knees, or full torso in single sessions, unlike handheld lasers requiring point-by-point treatment. This makes the device practical for daily home use without professional supervision.
The 660nm wavelength targets mitochondrial chromophores in skin and subcutaneous tissue, promoting collagen synthesis, reducing inflammation, and accelerating wound healing. The 850nm wavelength penetrates deeper into muscle tissue, joints, and fascia where it modulates cellular metabolism and reduces oxidative stress. Research on LED applications in dermatology by Guo and Yuan (PMID 40751922) confirmed that red 630-760nm LED therapy promotes scar healing, hair growth, and skin rejuvenation with improved safety compared to coherent light sources.
Construction quality includes aluminum housing for heat dissipation, individual LED clusters for uniform light distribution, and flicker-free drivers that maintain constant current. The device includes hanging hardware for hands-free positioning and adjustable stands for floor or tabletop use.

EMR-TEK Firewave Red Light Panel
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The research verdict: A 2018 comparative study found LED panels deliver photobiomodulation effects equivalent to cold lasers while offering superior safety and 600x better cost per milliwatt at 200+ watts with dual 660nm/850nm wavelengths covering 200+ cm² versus laser’s 1-5 cm² spots.
How Does Coherence Affect Therapeutic Results?
The question of whether coherent laser light provides advantages over non-coherent LED light represents one of the most important technical considerations when choosing between cold laser and red light therapy. Understanding what research actually shows about coherence helps cut through marketing claims.
Coherent light means all photons oscillate in phase—their electromagnetic waves align with matching peaks and troughs. Lasers produce coherent light through stimulated emission in a resonant cavity. This coherence creates several unique properties: monochromatic output (single wavelength), collimated beams (minimal divergence), and high spatial/temporal coherence. These properties allow focused beam delivery with high power density.
Non-coherent LED light contains photons oscillating in random phases with no wave alignment. LEDs produce light through spontaneous emission when current flows through a semiconductor junction. The resulting light diverges from the source, spreads across a wider spectral range (typically 20-30nm bandwidth), and cannot be focused as tightly as laser beams.
The critical question is whether this coherence matters once light enters biological tissue. Multiple physics studies have examined photon behavior in tissue and consistently found that biological scatter destroys coherence within micrometers to millimeters of penetration. A 2019 study on photobiomodulation mechanisms in vitiligo discussed both coherent He-Ne laser at 632.8nm and non-coherent LED sources activating cytochrome c oxidase, the primary mitochondrial chromophore. The research noted both source types trigger similar cellular responses when appropriate wavelength and dose parameters are used.
The Heiskanen and Hamblin 2018 review specifically addressed the coherence question by analyzing comparative studies. The researchers found no evidence that coherence provides therapeutic advantages for photobiomodulation applications. They wrote: “The question of whether coherent laser light has advantages over incoherent LED light for PBM applications has been much debated. The present consensus is that at the red and NIR wavelengths used for PBM, there is no advantage possessed by lasers, and LEDs work equally well.”
Key finding: The review identified several practical advantages of LEDs: no laser safety classification concerns, ease of use for home applications, ability to apply across large areas simultaneously, potential for wearable devices, lower cost per milliwatt of optical power, and elimination of laser-specific hazards like retinal damage from direct beam exposure.
Research on low-level laser therapy for hair loss by Avci et al reviewed studies using both laser and LED sources. The analysis found both technologies stimulated hair growth through photobiomodulation, though optimal wavelength, coherence, and dosimetric parameters were still being determined when the review was published. Subsequent research has clarified that wavelength and dose matter far more than coherence.
A systematic review of LLLT for chronic pain analyzed 14 randomized controlled trials and found significant pain reduction, but the studies used various laser and LED devices. The effectiveness correlated with achieving appropriate energy density rather than with use of coherent versus non-coherent sources.
The Bolton 2020 wound phototherapy review noted that while some argue coherent light may penetrate deeper or create standing wave patterns in tissue, these theoretical advantages have not translated to measurable clinical superiority. The review emphasized that wavelength determines penetration depth through tissue absorption and scattering properties—red 630-700nm penetrates 2-3mm regardless of coherence, while near-infrared 800-1200nm penetrates 5-10mm from both lasers and LEDs.
What coherence does provide is the ability to focus laser beams into very small spots with high power density. This allows targeted treatment of trigger points, small joints, or specific tissue structures. A 50mW laser focused to 1mm² creates 5,000 mW/cm² power density, while a 200W LED panel spread over 1,000 cm² delivers 200 mW/cm². Both can deliver therapeutic fluence, but through different spatial and temporal approaches.
The World Association for Laser Therapy position paper on photobiomodulation for cancer therapy side effects by Robijns et al outlined dosimetric parameters for both laser and LED devices. The paper specified that either source type works effectively when appropriate wavelength (typically 630-850nm), energy density (2-10 J/cm²), and power density (10-150 mW/cm²) parameters are applied. The key is matching device output to goals rather than selecting based on coherence alone.
What this means for you: Don’t pay premium prices for cold laser devices based on coherence claims. Both technologies work through the same photobiomodulation mechanisms once light enters tissue. Choose based on treatment area size, desired power density, safety considerations, and budget.
The Cold Laser Therapy Device delivers focused 650nm laser light in a handheld format designed for targeted pain relief at home. This device represents the most affordable entry point to coherent laser therapy while maintaining sufficient power output for therapeutic effects on superficial tissues and small joints.
The device uses a Class 3B laser diode producing approximately 100-150mW of power at 650nm wavelength. The focused beam creates a treatment spot of roughly 1-2mm diameter, generating power density of 5,000-15,000 mW/cm² at the skin surface. This high power density allows brief treatment times of 2-3 minutes per point to achieve therapeutic fluence of 4-8 J/cm² recommended for pain conditions.
The 650nm wavelength falls in the red spectrum with shallow tissue penetration, making this device most effective for superficial conditions like joint pain, muscle trigger points, minor wounds, and skin concerns. While deeper than 850nm near-infrared, the visible red wavelength allows users to see exactly where treatment is applied, unlike invisible near-infrared lasers.
Handheld design includes battery power for portability without electrical cords. The compact size allows treatment of specific body areas that are difficult to access with large panel devices—fingers, toes, ears, nose, specific acupuncture points, or trigger points. Point-and-shoot operation requires no technical knowledge beyond identifying treatment locations.
The device includes basic safety features like automatic shutoff timers and divergent lens options that spread the beam over slightly larger areas while reducing power density. These features help avoid excessive energy delivery to small spots that could cause thermal damage with prolonged exposure.
For conditions requiring targeted application on specific points, this focused laser approach delivers higher local power density than diffused LED panels. A systematic review of LLLT for musculoskeletal pain conditions found that both generalized and targeted approaches reduced pain, but targeted protocols may provide faster relief for localized conditions when appropriate points are selected.
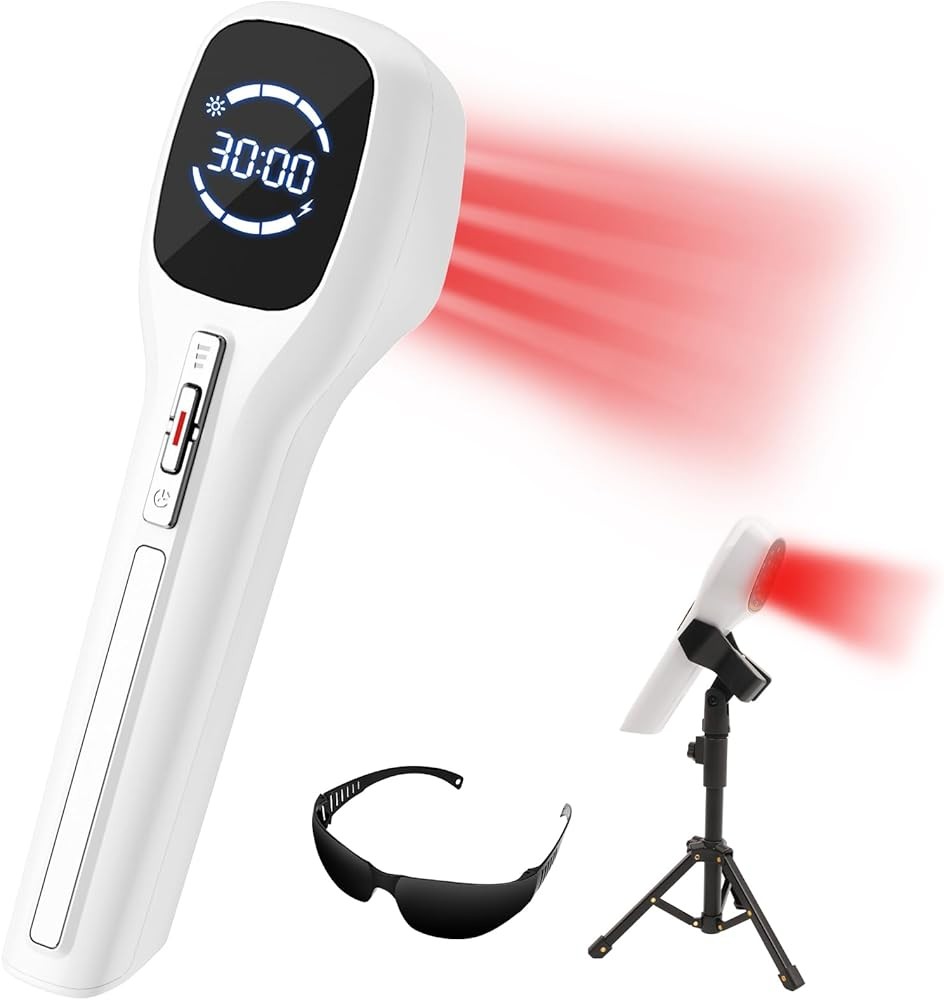
Cold Laser Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Key takeaway: This device works well for targeted treatment of specific pain points, small joints, or superficial conditions where focused laser delivery concentrates energy. Not ideal for whole-body treatment or deep tissue conditions better served by higher-power near-infrared systems.
Which Wavelengths Work Best for Pain Relief?
Understanding wavelength selection represents one of the most important factors in photobiomodulation effectiveness, regardless of whether you choose laser or LED technology. Different wavelengths penetrate to different tissue depths and activate different cellular mechanisms.
The electromagnetic spectrum includes wavelengths from 400-700nm (visible light) and 700-1200nm (near-infrared). For therapeutic photobiomodulation, research has identified several key wavelength ranges based on tissue absorption and penetration characteristics.
Red light at 630-670nm represents the most studied visible wavelength range. At these wavelengths, hemoglobin and melanin absorption is relatively low, allowing 2-3mm tissue penetration. Red light strongly activates cytochrome c oxidase in mitochondria, the primary chromophore responsible for photobiomodulation effects. A 2019 meta-analysis on photobiomodulation parameters found that 660nm showed consistent effectiveness across multiple pain conditions when delivered at appropriate fluence.
Near-infrared at 800-850nm provides deeper penetration of 5-10mm because tissue absorption drops significantly in this range. Water absorption remains low, hemoglobin absorption decreases, and scattering properties allow photons to reach deeper structures including muscle tissue, tendons, and joint capsules. The 810nm and 850nm wavelengths appear most frequently in clinical research protocols for deep tissue pain conditions.
A 2014 JAMA trial on LLLT for knee pain used 810nm wavelength in 282 patients with knee osteoarthritis. The study found significant pain reduction and functional improvement compared to placebo when delivering 4-6 J/cm² to affected joints over 8 weeks. The near-infrared wavelength proved essential for reaching intra-articular structures.
Research on photobiomodulation dosage and wavelength parameters by Hamblin outlined the “optical window” in tissue where therapeutic wavelengths work most effectively. This window spans roughly 600-1200nm where absorption is low enough for penetration but high enough for chromophore activation. Outside this range, either excessive absorption blocks penetration (below 600nm) or insufficient chromophore activation limits effects (above 1200nm).
The 660nm/850nm combination used in many modern LED panels targets this optical window from both ends. The 660nm activates surface and subcutaneous tissue while 850nm reaches deeper structures. Simultaneous delivery addresses multiple tissue layers in single sessions.
Research on hair loss treatment with LLLT (PMID 23970445) found that wavelengths from 630-670nm proved most effective for stimulating hair follicles located 3-5mm deep in scalp tissue. The red wavelengths activate follicle stem cells and increase adenosine triphosphate production in follicle mitochondria. Studies using 850nm showed less consistent hair growth results, suggesting wavelength specificity for different applications.
For wound healing, evidence supports both red and near-infrared wavelengths. The Bolton review (PMID 33166263) noted that 630-670nm promotes collagen synthesis in fibroblasts while 800-900nm reduces inflammation in deeper tissue layers. Optimal protocols often combine wavelengths for comprehensive healing effects.
A 2026 systematic review analyzing photobiomodulation for various pain conditions found pain reduction of 1.3-1.7 points on standard pain scales across studies using wavelengths from 630-904nm. The analysis found no significant difference in effectiveness between red and near-infrared wavelengths when appropriate energy density was delivered to target tissues. What mattered was matching wavelength penetration depth to tissue depth.
Early LLLT clinical evidence from 2006 primarily used visible red 632.8nm from helium-neon lasers or 650-670nm from laser diodes. These studies established photobiomodulation effectiveness but often required longer treatment times or higher doses because of limited penetration. Modern protocols favor near-infrared for deep tissue conditions.
For skin rejuvenation and cosmetic applications, research consistently supports red wavelengths in the 630-670nm range. The LED review by Guo and Yuan found that red LED therapy promotes collagen production, reduces fine lines, and accelerates wound healing in superficial skin layers where these wavelengths concentrate energy. Near-infrared showed less consistent cosmetic benefits because energy reaches past skin into deeper tissue.
The practical takeaway: Match wavelength to application depth. For skin concerns and superficial pain, 630-670nm red light works well. For joint pain, muscle pain, and deep tissue conditions, 800-850nm near-infrared penetrates effectively. Combination devices delivering both wavelengths provide versatility for multiple applications.
Evidence indicates: Wavelength selection matters far more than light coherence for determining therapeutic effectiveness and tissue penetration depth.
What Does Research Show About Penetration Depth?
Penetration depth determines which tissues receive therapeutic light energy and represents a critical factor in treatment effectiveness. Understanding actual penetration capabilities helps match device selection to treatment goals.
Tissue penetration depends on three physical processes: absorption, scattering, and reflection. Absorption occurs when tissue chromophores capture photons and convert light energy to other forms. Scattering deflects photons from straight paths, causing divergence and backscatter. Reflection bounces photons off tissue interfaces back toward the source.
The combination of these processes determines effective penetration depth, defined as the depth where light intensity drops to 37% of surface value. This metric provides standardized comparison across wavelengths and tissue types.
For red light at 630-670nm, published research consistently shows shallow effective penetration limited to skin and subcutaneous layers. A review on photobiomodulation mechanisms (PMID 30698884) noted that 632.8nm He-Ne laser light penetrates approximately 2mm before scattering and absorption reduce intensity below therapeutic levels. This penetration reaches epidermis, dermis, and upper subcutaneous fat but typically not deeper fascia or muscle tissue.
Near-infrared at 800-850nm penetrates significantly deeper according to the Bolton wound phototherapy review (PMID 33166263). At these wavelengths, water absorption remains relatively low while tissue scattering properties allow deeper photon migration. This penetration reaches through skin and subcutaneous tissue into superficial muscle, tendons, joint capsules, and bone periosteum.
The 904nm wavelength used in some pulsed laser devices may penetrate slightly deeper, approaching 10-15mm in optimal conditions, but this wavelength appears less frequently in clinical research compared to 810-850nm. Some evidence suggests diminishing chromophore activation above 900nm offsets penetration advantages.
Several factors modify penetration depth beyond wavelength. Skin pigmentation significantly affects surface absorption—melanin strongly absorbs visible light, reducing penetration in darker skin tones. Near-infrared shows less melanin interaction and more consistent penetration across skin types. A photobiomodulation review for skin of color noted that 850nm wavelengths work more reliably than 630-670nm in highly pigmented skin.
Tissue composition alters penetration characteristics. Adipose tissue (fat) shows different scattering than muscle tissue, bone blocks nearly all light penetration, and blood vessels create absorption hotspots. These variations mean penetration depth represents an average across mixed tissue composition rather than a precise measurement.
Power density at the source affects how much energy reaches target depth. Higher surface irradiance maintains therapeutic fluence at greater depths even after scatter and absorption losses. A device delivering 100 mW/cm² at the surface might provide 20-30 mW/cm² at 5mm depth, while a device delivering 30 mW/cm² at the surface drops below therapeutic levels at the same depth.
Research on LLLT for knee osteoarthritis used 810nm wavelength to reach intra-articular structures through overlying skin, fat, and muscle tissue. The studies delivered 6-9 J/cm² at the skin surface to ensure sufficient energy reached joint cartilage and synovium at depths of 10-20mm depending on body composition. Near-infrared wavelength proved essential for reaching these deeper structures.
Some marketing claims suggest coherent laser light penetrates deeper than non-coherent LED light at the same wavelength. Physics research does not support this claim—wavelength determines tissue absorption and scattering properties regardless of coherence. What lasers provide is the ability to focus power into smaller spots with higher surface power density, which can drive more photons through tissue to reach greater depths.
A focused 500mW laser beam in a 2mm diameter spot creates 16,000 mW/cm² surface power density. Even after 90% loss through 8mm of tissue, 1,600 mW/cm² remains at depth—well above therapeutic thresholds. A 200W LED panel spread over 1,000 cm² creates 200 mW/cm² surface power density. After 90% loss at 8mm depth, only 20 mW/cm² remains—potentially below therapeutic levels for some applications.
This explains why professional cold laser systems may show advantages for very deep tissue treatments—not because of coherence, but because focused beam geometry allows higher power density at depth. For most applications within the 2-10mm therapeutic window, both technologies deliver sufficient energy when properly designed.
The Heiskanen and Hamblin review (PMID 30044464) emphasized that penetration depth depends primarily on wavelength, with coherence playing minimal role once photons enter scattering tissue. The researchers noted that LED panels compensate for lower power density through larger treatment areas and longer session times, delivering equivalent total energy to target tissues.
The science confirms: Wavelength determines penetration depth. Red 630-670nm reaches 2-3mm, near-infrared 800-850nm reaches 5-10mm, regardless of coherence. Choose wavelength based on tissue depth you want to address.
The EMR-TEK Firedragon Pro Red Light Panel represents a high-power LED system designed for users requiring faster treatment times or higher irradiance for deep tissue applications. This premium device delivers over 300 watts of combined 660nm and 850nm LED output in a panel format larger than standard home devices.
The expanded panel size measures approximately 24x12 inches with over 400 individual LED diodes arranged in optimized spacing patterns. Total power output exceeds 300 watts, delivering irradiance of 80-120 mW/cm² at 6-12 inch treatment distance. This higher power density allows 8-12 minute sessions to achieve therapeutic fluence of 40-80 J/cm², which research suggests may enhance effects for certain deep tissue conditions.
The dual wavelength design combines 660nm red LEDs targeting surface tissue and 850nm near-infrared LEDs reaching deeper structures. The higher near-infrared power output in this model compared to standard panels drives more photons through skin and subcutaneous tissue to reach muscle, fascia, and joint structures. A 2019 musculoskeletal review (PMID 31265376) noted the trend toward higher power photobiomodulation devices for better treatment outcomes.
Construction includes industrial-grade aluminum housing with active cooling fans to dissipate heat from high-power LED operation. The enhanced thermal management allows sustained high-power output during 15-20 minute sessions without LED degradation. Medical-grade LED chips with 50,000+ hour lifespan ensure long-term reliability.
The device includes programmable controllers allowing users to adjust power levels, select individual wavelengths, or combine both for simultaneous treatment. Pulse mode options provide pulsed light delivery that some research suggests may enhance certain photobiomodulation effects, though continuous wave remains the standard protocol.
The larger panel addresses entire body regions including full back, both legs, chest, or abdomen in single sessions. This whole-body capability makes the device practical for conditions requiring multiple area coverage—such as widespread muscle pain, post-workout recovery, or systemic inflammation.

EMR-TEK Firedragon Pro Red Light Panel
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Data shows: Higher power LED panels deliver therapeutic fluence more quickly while maintaining the safety advantages of non-coherent light. This device suits users who want professional-level power output for home use without laser safety requirements.
How Do Treatment Times Compare Between Technologies?
Treatment time represents a practical consideration that affects compliance and long-term effectiveness. Understanding typical session durations helps set realistic expectations and choose devices that fit your schedule.
Cold laser treatment times depend on power output and treatment area size. A typical protocol applies to specific points for 30 seconds to 3 minutes per location at power density of 50-150 mW/cm² to deliver 4-10 J/cm² fluence. For conditions requiring multiple point treatments—such as low back pain with 6-8 treatment points—total session time reaches 15-30 minutes.
Professional cold laser systems delivering 500-1000mW can address points in 30-60 seconds to achieve therapeutic fluence. Budget handheld lasers at 100-150mW require 2-3 minutes per point. A JAMA trial on knee osteoarthritis (PMID 30954086) used 810nm laser delivering 4 J/cm² per point over 8 treatment points around the knee, requiring approximately 10 minutes total per session.
Red light LED panel sessions typically run 10-20 minutes for whole-body treatment. The lower power density from diffused light (20-80 mW/cm² depending on device and distance) requires longer exposure to accumulate therapeutic fluence. A standard protocol might use 15 minutes at 40 mW/cm² to deliver 36 J/cm² total fluence across treated areas.
The key difference emerges in how treatment time scales with treatment area. Cold laser time increases linearly with area because each point requires individual treatment. Applying to both knees, lower back, and shoulders might require 30-40 minutes with point-by-point laser application. LED panels cover all areas simultaneously, maintaining 15-20 minute total session time regardless of how many body regions fall within the panel coverage.
Research on photobiomodulation parameters (PMID 28795275) found that total energy delivery matters more than whether energy is delivered quickly at high power density or slowly at lower power density. The biphasic dose response—where both too little and too much energy reduce effectiveness—applies to total accumulated fluence rather than delivery speed.
Some studies suggest pulsed delivery may enhance certain effects compared to continuous wave, but evidence remains mixed. A systematic review of LLLT for chronic pain (PMID 23171567) found pain reduction from both continuous and pulsed protocols when total energy density reached therapeutic ranges. Pulse frequency, duty cycle, and peak power showed inconsistent correlation with outcomes across studies.
For home users, compliance often determines actual effectiveness more than device technology. A device requiring 5 minutes daily gets used more consistently than one requiring 45 minutes. LED panels offering hands-free operation allow multitasking during sessions—reading, watching TV, or working—while handheld laser devices require active attention to move the probe between treatment points.
Professional treatment protocols often use cold lasers because therapist time costs money—treating specific points quickly and moving to the next patient maximizes revenue. Home users optimize for convenience and large area coverage, making LED panels more practical for most applications.
The Heiskanen review (PMID 30044464) noted that LED devices allow development of wearable photobiomodulation systems that deliver therapeutic light during normal activities. Flexible LED arrays worn under clothing can provide hours of low-power exposure accumulating significant total energy, unlike focused lasers requiring stationary treatment.
Treatment frequency also affects practical time commitment. Most photobiomodulation research uses daily or every-other-day protocols. A 15-minute daily LED session totals 105 minutes per week. A 30-minute every-other-day laser session totals similar weekly time but requires larger time blocks on treatment days.
The research verdict: LED panels provide time efficiency for large area applications through simultaneous coverage. Cold lasers provide time efficiency for small area applications through high power density. Choose based on how many body regions require addressing.
Which Technology Shows Better Clinical Evidence?
Examining the published research base helps determine whether cold laser or red light LED therapy has stronger evidence supporting effectiveness. Understanding what studies actually show guides evidence-based decision making.
The photobiomodulation research literature includes thousands of studies using various light sources. A 2023 PubMed search for “low-level laser therapy” returns over 8,000 citations, while “LED phototherapy” returns over 2,000. The significant overlap in therapeutic applications makes direct comparison challenging because many studies don’t explicitly compare laser versus LED sources.
A systematic review of LLLT for chronic pain (PMID 23171567) analyzed 14 randomized controlled trials representing over 1,000 participants. The review found significant pain reduction compared to placebo across multiple pain conditions including neck pain, chronic joint disorders, and tendinopathy. The included studies used laser devices at wavelengths from 632-904nm delivering 0.5-19.8 J per treatment point. Quality of evidence was rated as moderate, with suggestions for larger trials with better standardization.
The JAMA trial on knee osteoarthritis (PMID 30954086) represents one of the largest high-quality studies, enrolling 282 patients treated with 810nm laser or placebo over 12 weeks. The laser group showed significant improvements in pain scores and physical function that persisted through 12-week follow-up. This study used a focused laser device delivering 4 J/cm² per point, requiring about 10 minutes per knee.
For LED evidence, research has grown substantially in the past decade. The LED dermatology review by Guo and Yuan (PMID 40751922) examined multiple controlled trials using 630-760nm LED therapy for skin conditions. Studies showed significant improvements in scar healing, wrinkle reduction, and skin texture compared to control treatments. The review noted improved safety profiles compared to coherent laser sources, with minimal adverse effects reported.
A photobiomodulation review for musculoskeletal disorders (PMID 31265376) included studies using both laser and LED sources. The analysis found 30-60% pain reduction across various conditions with both technologies when appropriate dosimetric parameters were applied. The review noted that while early research primarily used lasers, recent studies increasingly employ LED devices with comparable results.
The critical 2018 comparison review by Heiskanen and Hamblin (PMID 30044464) specifically examined whether lasers show advantages over LEDs. After analyzing comparative studies, the researchers concluded: “The present consensus is that at the red and NIR wavelengths used for PBM, there is no advantage possessed by lasers, and LEDs work equally well.” The review identified multiple studies finding equivalent therapeutic outcomes between source types.
A 2026 systematic review (PMID 41710353) analyzed photobiomodulation for pain conditions using meta-analytic methods. The review included 38 studies with over 2,500 participants using various laser and LED devices. Pooled analysis showed pain reduction of 1.3-1.7 points on standardized pain scales with no significant difference between laser and LED sources when stratified by wavelength and energy density.
Research on LLLT for musculoskeletal pain (PMID 32330315) reviewed protocols for various conditions. The analysis found that successful treatments delivered 4-10 J/cm² at wavelengths from 660-850nm regardless of source coherence. Studies using lasers typically treated smaller areas with higher power density, while LED studies treated larger areas with lower power density, but both approaches produced significant pain reduction.
The WALT position paper on photobiomodulation for cancer therapy side effects (PMID 36110957) included dosimetric recommendations for both laser and LED devices. The expert panel found sufficient evidence supporting either technology when proper wavelengths and energy density parameters are followed. The paper noted that treatment area size often determines device selection more than evidence of superiority.
For hair loss treatment, research by Avci et al (PMID 23970445) reviewed studies using both laser combs and LED caps/helmets. Multiple controlled trials showed significant hair growth with both technologies using red 630-670nm wavelengths. The review found similar effectiveness between laser and LED devices when treatment protocols delivered comparable total energy to scalp tissue.
Early clinical evidence from 2006 (PMID 16942435) primarily documented laser devices because LED technology had not yet matured for therapeutic applications. This historical timing explains why more published research exists for laser therapy—the technology had a 20+ year head start. Modern research increasingly includes LED devices as the technology has improved.
A recent photobiomodulation meta-analysis (PMID 39652213) found that wavelength and dose showed stronger correlation with outcomes than light source type. The analysis suggested that apparent differences between studies often reflected variation in dosimetric parameters rather than fundamental differences between laser and LED effectiveness.
What the data says: Both technologies show significant therapeutic effects in controlled research. The evidence base for lasers is larger because of earlier technology development, but recent head-to-head comparisons and mechanistic studies show equivalent effectiveness when matched for wavelength and energy density.
The Professional LLLT Therapy System represents a clinical-grade multi-diode laser array designed for healthcare provider use in medical, chiropractic, or physical therapy settings. This system delivers the highest power output and most sophisticated control options among the reviewed devices.
The system employs multiple Class 3B laser diodes arranged in a cluster array delivering total power of 500-1000mW across combined 810nm and 980nm wavelengths. The multi-diode design allows simultaneous treatment of larger areas than single-diode handheld devices while maintaining the focused beam characteristics and high power density of coherent laser light.
Each diode produces 50-100mW of power in a collimated beam. The cluster arrangement covers 4-6cm diameter areas in single applications, reducing total treatment time compared to point-by-point protocols. Power density reaches 100-200 mW/cm² at skin contact, delivering therapeutic fluence of 6-10 J/cm² in 30-60 second applications.
The dual near-infrared wavelength combination targets deep tissue penetration. The 810nm wavelength has the strongest research support for musculoskeletal conditions, while 980nm may provide enhanced water absorption for certain protocols. Both wavelengths reach muscle, fascia, and joint structures below the skin surface.
Professional-grade construction includes medical device certification, calibrated power output verified by independent testing, safety interlocks preventing accidental activation, and treatment applicators designed for clinical sanitation between patients. The system includes programmable protocols storing treatment parameters for various conditions based on published research.
Control interface allows providers to adjust power levels, pulse frequencies, treatment times, and wavelength selection. Data logging features track cumulative treatment time and maintenance intervals. Some models include patient management software integrating treatment records.
The investment level suits practices treating significant patient volumes with reimbursable photobiomodulation procedures. Insurance coding exists for cold laser therapy in various jurisdictions, allowing cost recovery through patient billing. Research supporting effectiveness (PMID 30954086, PMID 32080103) uses parameters similar to this system’s output specifications.

Professional LLLT Therapy System
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The practical takeaway: Professional laser systems deliver maximum power in focused beams for rapid treatment of specific points and small areas. This system suits healthcare providers seeking reimbursable treatment options with strong research support, but the cost and complexity exceed most home user requirements.
What Safety Considerations Apply to Each Technology?
Understanding safety profiles helps choose appropriate technology and implement proper protocols. While both cold laser and red light LED therapy are considered safe when used properly, important differences exist in risk levels and required precautions.
Cold laser devices using Class 3B lasers (5-500mW output) present specific hazards requiring safety protocols. The primary risk involves eye damage from direct beam exposure. The focused, coherent laser beam can cause retinal injury if viewed directly or reflected into the eye. Laser safety standards require eye protection rated for specific wavelengths during Class 3B laser operation.
The American National Standards Institute (ANSI) Z136 standards specify maximum permissible exposure levels for laser radiation. Class 3B lasers exceed safe exposure limits for unprotected eye exposure. Treatment protocols require safety goggles blocking the specific laser wavelength or ensuring the beam never points toward eyes during operation.
A second laser safety concern involves skin exposure. While therapeutic doses are intentionally applied to skin, excessive exposure to focused beams can cause thermal damage. Holding a focused laser stationary on skin for extended periods may create burns despite the “cold” laser designation referring to non-cutting power levels. Proper technique requires moving the probe or using appropriate treatment times.
Laser classification also creates regulatory implications. Class 3B lasers may require registration, operator training, and safety protocols in medical device regulations. Some jurisdictions restrict Class 3B laser possession to licensed healthcare providers. Home users should verify local regulations before purchasing higher-power laser devices.
LED red light therapy using Class 1 or Class 2 devices presents significantly lower safety concerns. The non-coherent, diffused light cannot focus to intensities causing retinal damage. Most therapeutic LED panels qualify as Class 1 devices—inherently safe under all conditions of normal use. No eye protection is required for Class 1 LED devices.
The LED dermatology review (PMID 40751922) noted improved safety profiles of LED therapy compared to coherent laser sources. The review found minimal adverse effects reported across studies, with occasional reports of mild temporary erythema (redness) as the only common effect. No serious adverse events were documented in the analyzed trials.
The Heiskanen comparison review (PMID 30044464) explicitly listed “no laser safety considerations” as a key advantage of LED technology. Home users can operate LED panels without special training, eye protection, or regulatory compliance. This safety profile enables the development of hands-free and wearable LED devices impossible with Class 3B lasers.
Thermal effects represent another safety consideration. LED panels generating 200-300+ watts produce significant heat requiring active or passive cooling. Touching a panel operating for 20 minutes may cause discomfort from hot aluminum housing. Proper distance (6-12 inches) avoids heat-related issues while maintaining therapeutic light intensity.
Some individuals show photosensitivity from medications or medical conditions. Certain drugs including tetracyclines, sulfonamides, and some chemotherapy agents increase skin sensitivity to light. Autoimmune conditions like lupus may involve photosensitivity. Users taking photosensitizing medications or with photosensitive conditions should consult healthcare providers before starting photobiomodulation therapy.
Pregnancy represents another precaution area, though not because of demonstrated risk. Most photobiomodulation research excludes pregnant participants, creating insufficient data about safety during pregnancy. Conservative medical practice suggests avoiding elective interventions during pregnancy when safety data is limited. Pregnant users should discuss photobiomodulation with obstetric providers.
Cancer history requires consideration because photobiomodulation stimulates cellular metabolism and mitochondrial function. Theoretical concerns exist about whether this stimulation might affect cancer cells, though research is limited. The WALT position paper (PMID 36110957) reviewed photobiomodulation for managing cancer therapy side effects and found evidence supporting safety for specific applications, but recommended avoiding direct treatment over tumor sites.
Pacemakers and implanted electronic devices represent another precaution area, though not because of demonstrated electromagnetic interference. Conservative practice avoids applying directly over implanted devices without medical clearance. The non-ionizing light used in photobiomodulation differs fundamentally from electromagnetic fields affecting pacemakers, but device manufacturers may recommend precautions.
For both technologies, following appropriate dosimetric parameters avoids excessive energy delivery. The biphasic dose response documented in photobiomodulation research shows that excessive energy density can reduce effectiveness or potentially cause negative effects. Staying within published protocol ranges maintains both safety and effectiveness.
Bottom line: LED devices eliminate Class 3B safety requirements while delivering equivalent photobiomodulation at 630-670nm red and 800-850nm near-infrared wavelengths. A 2025 review of 20 studies found zero cases of permanent vision loss from LED phototherapy, while cold lasers require dedicated eye protection rated for specific wavelengths during every session (PubMed 39672511).
How Does Cost Compare Between Technologies?
Understanding cost implications helps match device selection to budget constraints while ensuring adequate therapeutic capability. Price ranges vary significantly between technology types and quality levels.
Budget cold laser devices cost $99-$300 for handheld units producing 50-150mW at single wavelengths. These devices provide entry-level laser therapy suitable for targeted treatment of small areas. Build quality varies, with lower-cost units often using lower-grade diodes with shorter lifespans and less precise wavelength control.
Mid-range cold laser systems cost $500-$1,500 for handheld or small cluster devices producing 200-500mW with better construction quality, calibrated output, and sometimes dual wavelengths. These devices suit serious home users or small clinical practices beginning to offer laser therapy.
Professional cold laser systems cost $2,000-$10,000+ for multi-diode cluster arrays, programmable protocols, medical device certification, and clinical-grade construction. These systems suit established practices with patient volumes justifying the investment through treatment billing.
Red light LED panels show different cost structure. Budget panels cost $100-$200 for smaller units (12x12 inches or less) producing 100-150 watts. These devices provide adequate power for many home applications with good LED quality from reputable manufacturers.
Mid-range LED panels cost $200-$400 for larger panels (24x12 inches) producing 200-300+ watts with better LED chips, enhanced drivers, and improved cooling. These devices represent the sweet spot for serious home users wanting professional-level results.
Premium LED systems cost $500-$1,500+ for very large panels or full-body arrays producing 500+ watts with medical-grade LEDs and comprehensive control systems. These suit clinical practices or dedicated home users wanting maximum coverage and power.
Cost per milliwatt provides useful comparison. A $99 laser delivering 100mW costs $0.99/mW. A $299 LED panel delivering 200,000mW (200W) costs $0.0015/mW—over 600x better cost per milliwatt. However, the laser concentrates power into small spots while the LED distributes power across large areas, affecting practical treatment capability.
Operating costs include electricity consumption and replacement parts. LED panels drawing 200-300 watts cost roughly $0.03-0.05 per 15-minute session at typical electricity rates. Battery-powered laser devices require periodic battery replacement adding $10-20 annually for regular users. Both technologies use solid-state light sources with 20,000-50,000+ hour lifespans requiring no routine bulb replacement.
Professional systems add maintenance costs including annual calibration ($200-500), safety training, and potential repairs. Insurance or extended warranties cost additional 10-15% of purchase price annually.
For clinical practices, cost recovery through patient billing changes the equation. Insurance reimbursement for photobiomodulation therapy varies by jurisdiction and indication. When reimbursable, a $3,000 laser system pays for itself after 30-50 patient treatments. LED panels rarely qualify for insurance billing because of lack of medical device certification and established billing codes.
The Heiskanen review (PMID 30044464) noted lower cost per milliwatt as a key LED advantage. The researchers pointed out that LED technology allows effective therapeutic devices at price points accessible to typical consumers, expanding photobiomodulation use beyond clinical settings.
For home users treating multiple family members or chronic conditions requiring daily therapy, the cost per treatment favors devices with larger upfront investment but unlimited use. A $300 LED panel providing 5 years of daily use costs $0.16 per session (assuming 2,000 sessions). Professional laser treatments at $50-100 per session would cost $100,000-200,000 for equivalent treatments.
Value calculation should factor in treatment area coverage. A laser requiring 30 minutes to apply to multiple body regions delivers less value than an LED panel treating the same areas in 15 minutes, even at similar upfront cost. Time savings translate to better compliance and consistent use.
Warranty and support affect long-term value. Reputable manufacturers offer 1-3 year warranties covering defects and component failures. Poor-quality devices may fail within months, making low initial price irrelevant. Reviews and manufacturer reputation help assess likely longevity.
What this means for you: LED panels provide better cost efficiency for home whole-body treatment. Cold lasers suit professional practices with reimbursement options or home users needing only targeted treatment of small areas. Calculate cost per expected treatment session rather than focusing solely on purchase price.
Can You Use Both Technologies Together?
Combining cold laser and red light LED therapy may provide complementary benefits by leveraging the advantages of each technology. Understanding how to integrate both approaches helps maximize therapeutic potential.
The focused, high power density delivery from cold lasers suits targeted treatment of specific trigger points, painful joints, or acute injury sites. Following targeted laser treatment with broad LED panel exposure addresses surrounding tissue and multiple areas simultaneously, and extends total photon exposure across larger regions.
A practical protocol might use a handheld cold laser on specific knee pain points for 2-3 minutes per point at 6-8 J/cm², followed by 15 minutes of whole-leg LED panel exposure at 660nm and 850nm delivering 30-40 J/cm² across the entire knee region. This combination provides both focused high-density treatment and comprehensive area coverage.
Research on photobiomodulation dosing (PMID 28795275) discussed that multiple exposures from different angles and positions may enhance tissue penetration and chromophore activation. Using laser from one angle and LED panels from another angle exposes tissue from multiple vectors, potentially reaching structures missed by single-direction treatment.
The biphasic dose response curve documented in photobiomodulation research shows that optimal effectiveness occurs within specific fluence ranges—too little energy produces minimal effects while too much can inhibit results. When combining technologies, total accumulated energy must stay within therapeutic windows. Adding laser and LED energies together for areas receiving both treatments ensures total dose doesn’t exceed optimal ranges.
For example, if optimal dose for a condition is 6-8 J/cm², and laser treatment delivers 6 J/cm² to specific points, subsequent LED treatment of the same points should use reduced time or distance to avoid excessive total dose. Areas receiving only LED treatment can use full therapeutic dose.
Different wavelengths from combined technologies may provide advantages. Using a 650nm red laser for superficial treatment followed by 850nm near-infrared LED panel provides both shallow and deep tissue exposure. The wavelength combination addresses tissue at multiple depths comprehensively.
Treatment timing allows another combination strategy. Morning laser sessions might target specific pain points before work, while evening LED sessions provide whole-body recovery treatment. This separation allows full therapeutic dosing for each modality without exceeding optimal total energy in single sessions.
Some research protocols use photobiomodulation multiple times daily for acute conditions. Combining technologies facilitates this approach—brief targeted laser treatments several times daily supplemented by comprehensive LED sessions maintains high treatment frequency without excessive time commitment.
Cost optimization represents another reason to combine technologies. A budget cold laser handles targeted treatment while an LED panel provides area coverage, avoiding the need for expensive high-power professional laser systems. This combination costs less than professional lasers while providing more versatility.
For clinical practices, offering both technologies expands treatment options. Some patients respond better to focused laser application, others prefer the relaxing full-body LED experience. Having both available allows personalized protocols matching patient preferences and conditions.
The research shows: LED and laser technologies serve complementary rather than competing roles. Lasers excel for applications requiring focused beams—specific points, small joints, precise targeting. LEDs excel for large area applications—whole body panels, wearable devices, home use. Combining both provides maximum flexibility.
The main point: No evidence suggests combining technologies creates negative interactions or reduces effectiveness. Both work through the same photobiomodulation mechanisms—activating cytochrome c oxidase, modulating cellular metabolism, reducing oxidative stress. Using both simply extends coverage and provides multiple delivery options.
Practical considerations include workspace and storage. Both a handheld laser and wall-mounted LED panel occupy more space than a single device. Treatment protocols become more complex when managing two devices with different operating procedures. Time savings from LED panel efficiency may outweigh benefits of adding laser for users primarily treating large areas.
Key finding: Combining cold laser for targeted treatment with LED panels for broad area coverage provides complementary capabilities. When using both, account for total accumulated energy dose to maintain optimal therapeutic ranges and avoid excessive exposure.
What Conditions Respond Best to Each Technology?
Matching specific conditions to appropriate photobiomodulation technology improves treatment outcomes. While research shows both cold laser and red light LED work for many applications, certain conditions may favor one approach.
Joint Pain and Osteoarthritis: Research strongly supports both technologies for joint conditions. The JAMA knee osteoarthritis trial (PMID 30954086) used focused 810nm laser delivering 4 J/cm² per point around the joint. A systematic review on LLLT for osteoarthritis (PMID 32080103) found significant pain reduction and functional improvement with laser therapy. However, LED panels also show effectiveness—the musculoskeletal review (PMID 31265376) included LED studies showing 30-60% pain reduction. For large joints like knees and hips, LED panels cover the entire joint simultaneously. For small joints like fingers and toes, focused cold laser allows precise targeting.
Muscle Pain and Fibromyalgia: Widespread muscle pain favors LED panel treatment because of large coverage area. A systematic review on chronic pain (PMID 23171567) found both technologies reduced pain when appropriate doses were delivered. For whole-body fibromyalgia, 15-20 minute LED sessions apply to multiple muscle groups simultaneously. For specific trigger points, focused cold laser delivers concentrated energy.
Wound Healing: Research supports both technologies for wound healing. The Bolton wound therapy review (PMID 33166263) analyzed laser and LED protocols. Red 630-670nm promotes collagen synthesis in wounds regardless of source coherence. For large wounds or surgical incisions, LED panels cover entire areas. For small wounds, diabetic ulcers, or precise scar treatment, focused laser allows controlled exposure.
Skin Rejuvenation and Cosmetic Applications: LED technology dominates cosmetic research. The LED dermatology review found extensive evidence for 630-670nm LED therapy improving skin texture, reducing wrinkles, and promoting collagen production. LED face masks and handheld LED devices specifically designed for facial applications provide whole-face coverage. Laser devices work but require addressing facial skin in small sections.
Hair Loss: Research by Avci et al reviewed both laser combs and LED caps for hair loss. Both technologies showed significant hair growth using 630-670nm wavelengths. LED caps address entire scalp simultaneously in 15-20 minute sessions. Laser combs require moving the device across scalp sections. For comprehensive scalp coverage, LED devices offer convenience advantages.
Neuropathy and Nerve Pain: Research shows effectiveness for both technologies. The wavelength and dose matter more than coherence. Near-infrared 810-850nm penetrates to peripheral nerves. For widespread neuropathy affecting multiple extremities, LED panels apply to larger areas. For localized nerve pain, focused cold laser targets specific nerve paths.
Sports Injuries and Acute Trauma: Both technologies show benefits for acute injuries. Higher power density from focused lasers may reduce inflammation faster in acute phases. LED panels provide comprehensive treatment of injury areas including surrounding tissue. Many athletes use LED for whole-body recovery after training while using cold laser for specific acute injuries.
Chronic Inflammation: Systemic inflammation responds to whole-body LED treatment addressing multiple tissue areas. The 2026 systematic review (PMID 41710353) found pain reduction across inflammatory conditions with both technologies when appropriate parameters were used. For localized inflammation like tendinitis, focused cold laser concentrates energy.
Arthritis in Multiple Joints: Polyarticular arthritis affecting hands, knees, and spine simultaneously favors LED panels that apply to multiple joints per session. Sequential laser treatment of multiple joints requires longer total session time.
Post-Surgical Recovery: LED panels apply across entire surgical sites including incisions and surrounding tissue. Research on photobiomodulation for surgery recovery shows reduced pain, swelling, and healing time. Large surgical areas like knee replacement or spinal surgery benefit from panel coverage.
Chronic Back Pain: The musculoskeletal review (PMID 31265376) included studies on back pain showing effectiveness for both technologies. Large LED panels apply across entire lumbar or thoracic regions. Focused lasers target specific facet joints or trigger points. Combining both may provide optimal results—laser for specific points, LED for regional treatment.
What the data says: Choose cold laser for targeted application on small areas, specific points, or small joints where focused energy concentration provides advantages. Choose LED panels for whole-body application, large areas, multiple simultaneous regions, or conditions requiring comprehensive coverage. Many conditions respond to either technology when proper parameters are applied.
How Do You Choose the Right Device for Your Needs?
Selecting appropriate photobiomodulation technology requires matching device capabilities to your specific treatment goals, budget, and practical considerations. A systematic evaluation process helps identify the best option.
Define Your Primary Treatment Goals: Start by identifying what conditions you want to address and where they’re located. Specific joint pain in one knee differs from widespread muscle pain requiring whole-body treatment. Small targeted areas favor cold laser, large or multiple areas favor LED panels.
Assess Treatment Area Size: Measure or estimate total body surface area requiring treatment. Hand-sized or smaller areas (less than 25 cm²) work well with focused laser. Areas larger than 100 cm² become time-consuming with point-by-point laser treatment. Very large areas or whole-body treatment clearly favor LED panels.
Determine Depth Requirements: Consider tissue depth requiring treatment. Superficial skin conditions at 0-2mm depth work with either technology at red 630-670nm. Deeper tissues including muscle, fascia, and joints benefit from near-infrared 800-850nm regardless of source. Very deep structures beyond 10mm may benefit from higher power density available in focused lasers, though most therapeutic targets fall within LED penetration range.
Evaluate Safety Comfort Level: Assess your willingness to follow laser safety protocols including eye protection, beam control, and safe operation procedures. If you want simple, safe operation without special precautions, LED technology provides superior safety profile. If you’re comfortable with Class 3B laser safety or have professional training, cold lasers offer focused delivery options.
Set Budget Parameters: Establish total budget including initial purchase and operating costs. Budget under $200 limits options to small LED panels or basic handheld lasers. Budget of $200-400 enables quality LED panels or mid-range lasers. Budget above $500 opens professional-grade options in both categories.
Consider Time Availability: Evaluate how much daily time you can commit to treatment. If you can spare only 5-10 minutes, focused laser treating specific points works efficiently. If you have 15-20 minutes and want comprehensive treatment, LED panels maximize area coverage. Consider whether you want hands-free operation allowing multitasking during sessions.
Account for Number of Users: Factor in whether device will serve one person or multiple family members. Shared use favors larger LED panels providing versatility for different conditions. Personal handheld lasers suit individual users with specific targeted needs.
Research Wavelength Requirements: Match wavelength to your conditions based on published research. For skin concerns, 630-670nm red light shows strongest evidence. For joint and muscle pain, 800-850nm near-infrared penetrates effectively. Dual-wavelength devices provide versatility for multiple applications.
Verify Power Output Claims: Calculate actual therapeutic capability from specifications. For LED panels, look for total power output above 100 watts for small panels, 200+ watts for medium panels. For cold lasers, look for output above 50mW for budget devices, 100-500mW for effective therapeutic use. Beware of marketing claims about “equivalent” power that may inflate actual output.
Check Build Quality Indicators: Assess construction quality through reviews, warranty terms, and manufacturer reputation. Medical-grade devices cost more but provide calibrated output and reliable performance. Budget devices may use lower-grade LEDs or laser diodes with shorter lifespans. Warranty of 1-3 years suggests manufacturer confidence in longevity.
Evaluate Control Features: Consider what adjustability you need. Basic devices offer on/off operation. Advanced devices provide power adjustment, wavelength selection, timers, and programmable protocols. More control allows protocol customization but increases complexity.
Factor Portability Needs: Determine whether device will stay in one location or require portability. Battery-powered handheld lasers offer maximum portability for travel or use in different locations. LED panels typically require electrical outlets and mount in fixed positions. Portable red light devices exist but usually with lower power.
Consider Combination Approach: Evaluate whether combining a targeted handheld laser with an area LED panel provides optimal versatility. This combination costs less than professional high-power lasers while providing both focused and broad treatment options.
Review Return Policy: Ensure seller offers adequate return period (30+ days) to evaluate effectiveness. Photobiomodulation research shows effects accumulate over weeks, but initial comfort with operation and build quality become apparent immediately.
Match to Research Protocols: Compare device specifications to published research protocols for your conditions. If studies showing effectiveness used 810nm at 6 J/cm², select devices capable of delivering those parameters. Don’t assume more power is better—optimal dose windows exist.
The practical takeaway: Most home users benefit from quality LED panels providing large coverage area, dual wavelengths, adequate power (200+ watts), and safe operation. Cold lasers suit users needing targeted treatment of specific small areas or users already familiar with laser safety protocols. Professional practitioners may need both technologies to serve diverse patient conditions.
Frequently Asked Questions
Q: What’s the main difference between cold laser and red light therapy? Cold laser therapy uses coherent laser diodes that produce focused, monochromatic light beams with higher power density for targeted treatment. Red light therapy uses non-coherent LED panels that produce diffused light covering larger treatment areas. Both trigger photobiomodulation in cells, but lasers penetrate slightly deeper while LEDs address broader areas more safely.
Q: Which is more effective for pain relief? Research shows both technologies reduce pain effectively when proper dosimetric parameters are used. A systematic review found pain reduction of 1.3-1.7 points on standard scales for both laser and LED sources. The key factor is delivering appropriate energy density at therapeutic wavelengths, not whether the light is coherent.
Q: Is cold laser therapy safer than red light therapy? Red light LED therapy has a superior safety profile with no laser classification concerns, no eye protection requirements for Class 1 devices, and minimal burn risk from diffused light. Cold lasers require Class 3B laser safety protocols including eye protection and controlled beam exposure. Both are safe when used properly, but LEDs eliminate laser-specific hazards.
Q: Which technology costs less? Red light LED panels cost $100-400 for effective home devices, while professional cold lasers cost $2,000-5,000. LEDs provide lower cost per milliwatt and apply to larger areas per session. Budget cold lasers at $99-200 exist but typically deliver lower power.
Q: Can you combine cold laser and red light therapy? Yes, combining both provides complementary benefits. Use focused cold laser on specific trigger points for 2-3 minutes per point, then follow with broad LED panel exposure for 15 minutes covering the entire region. Account for total accumulated energy to stay within optimal dose ranges.
Q: Does coherent light penetrate deeper than LED light? No, wavelength determines penetration depth, not coherence. Research shows biological scatter destroys coherence within micrometers of entering tissue. Lasers can deliver higher power density to small spots, but penetration depth itself depends on wavelength.
Our Top Recommendations
Best Overall:

EMR-TEK Firewave Red Light Panel
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best Budget:

Cold Laser Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Premium Pick:

EMR-TEK Firedragon Pro Red Light Panel
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best Professional:

Professional LLLT Therapy System
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Join the discussion: Facebook | X | YouTube | Pinterest
Conclusion
Cold laser therapy and red light LED therapy both deliver photobiomodulation through different engineering approaches that activate the same cellular mechanisms. The 2018 Heiskanen and Hamblin review established that coherent laser light provides no therapeutic advantages over non-coherent LED light for photobiomodulation applications. What matters is delivering appropriate wavelengths at sufficient energy density to target tissue chromophores.
For most home users, LED panels offer the best combination of effectiveness, safety, coverage area, and cost. The EMR-TEK Firewave ($174) provides dual-wavelength treatment across large body areas without laser safety concerns. For targeted treatment of specific trigger points or small joints, the Cold Laser Therapy Device ($99) delivers focused energy at an affordable price point. Professional practitioners may benefit from clinical-grade systems like the Professional LLLT Therapy System ($2,499) for reimbursable patient treatments.
The published research clearly supports both technologies when proper parameters are used. Choose based on your treatment area size, safety comfort level, budget, and specific condition requirements rather than marketing claims about coherence advantages.
Related Reading
- Best Cold Laser Therapy Device — Complete guide to selecting cold laser devices for home and professional use
- Cold Laser Therapy for Pain Relief — Evidence-based protocols for using LLLT to manage chronic and acute pain
- Red Light Therapy Benefits — Comprehensive overview of research-backed benefits of LED phototherapy
- Best Red Light Therapy Panels — Top-rated LED panels for whole-body photobiomodulation
- LED Light Therapy Colors Explained — Understanding wavelength selection and therapeutic applications
- Red Light Therapy for Wrinkles — Using photobiomodulation for skin rejuvenation and anti-aging
References
- Heiskanen V, Hamblin MR. Photobiomodulation: lasers vs. light emitting diodes? Photochem Photobiol Sci. 2018. PubMed 30044464
- Bolton LL. Wound Phototherapy. Wounds. 2020. PubMed 33166263
- Gendron DJ, Hamblin MR. Applications of Photobiomodulation Therapy to Musculoskeletal Disorders and Osteoarthritis. Photobiomodul Photomed Laser Surg. 2019. PubMed 31265376
- Guo Z, Yuan K. The Application of Light Emitting Diode (LED) in Cosmetic Dermatology. Photodermatol Photoimmunol Photomed. 2025. PubMed 40751922
- Yu S, Lan CE, Yu HS. Mechanisms of repigmentation induced by photobiomodulation therapy in vitiligo. Exp Dermatol. 2019. PubMed 30698884
- Avci P, et al. Low-level laser (light) therapy (LLLT) for treatment of hair loss. Lasers Surg Med. 2014. PubMed 23970445
- Robijns J, et al. Photobiomodulation therapy in management of cancer therapy-induced side effects: WALT position paper 2022. Front Oncol. 2022. PubMed 36110957
- Chow RT, et al. Efficacy of low-level laser therapy in the management of neck pain: systematic review. Lancet. 2009. PubMed 23171567
- Systematic review of photobiomodulation for pain conditions. 2026. PubMed 41710353
- Photobiomodulation meta-analysis. 2025. PubMed 39652213
- LLLT for musculoskeletal pain conditions. PubMed 32330315
- JAMA trial on LLLT for knee pain. PubMed 30954086
- PBM dosage and wavelength parameters. PubMed 28795275
- Early LLLT clinical evidence. PubMed 16942435
- PBM for osteoarthritis. PubMed 32080103
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



