Best Heating Pads for Pain Relief
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Chronic pain affects over 50 million American adults according to CDC data, with limited options beyond pharmaceuticals that carry side effect risks. The Sunbeam Premium Heating Pad delivers targeted heat therapy with 6 heat settings, auto-shutoff safety features, and compact storage design for $34, making it a versatile option for managing various pain conditions. Published research in Clinical Biomechanics shows supplemental heat wrap therapy improved trunk strength parameters in 176 chronic low back pain patients when added to standard care, with heat application demonstrating measurable increases in pressure pain thresholds. For budget-conscious buyers, the Deepsoon Heating Pad provides dry and moist heat with auto-shutoff for just $15. Here’s what the published research shows about heat therapy effectiveness, optimal application protocols, and how different heating pad technologies compare for pain management.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
What Does Research Say About Heat Therapy for Pain?
Multiple randomized controlled trials demonstrate heat therapy’s effectiveness for both acute and chronic pain conditions through distinct physiological mechanisms. A 2018 multicenter study published in Clinical Biomechanics examined 176 patients with chronic low back pain in a multimodal setting.1 Patients receiving supplemental heat wrap therapy for several hours daily showed additional improvements in trunk strength parameters compared to those receiving only standard multimodal care, with particular gains in extension strength and rotational capacity.
The mechanisms underlying heat therapy’s pain-reducing effects involve multiple pathways. Research published in Topics in Companion Animal Medicine explains that superficial heat therapy increases blood flow, oxygen delivery, and tissue extensibility when applied to chronic musculoskeletal conditions.2 These physiological changes create favorable conditions for tissue healing while simultaneously reducing pain signal transmission through thermoreceptor activation.
Temperature depth penetration varies significantly based on heating modality. A 2018 randomized trial in the Journal of Back and Musculoskeletal Rehabilitation compared deep heating therapy via medium frequency radiowaves to superficial heating therapy in 49 patients with nonspecific chronic low back pain.3 The deep heating therapy group, 450 KHz frequency, demonstrated greater pain reduction on the Numerical Rating Scale at 15 days and superior disability reduction on the Oswestry Disability Index throughout all follow-up periods extending to 45 days.
The combination of heat therapy with other modalities shows promise for enhanced outcomes. A 2021 study in the Brazilian Journal of Physical Therapy investigated transcutaneous electrical nerve stimulation combined with heat in 50 participants with chronic low back pain.4 While the combination did not significantly reduce overall pain scores compared to control, it produced significant improvements in pressure pain threshold measures after both 30-minute sessions and 4-week periods, particularly in the lower back region.
Duration and frequency of heat application impact clinical outcomes. A 2015 protocol for a randomized controlled trial examining heating and cooling combination therapy outlined 15-minute sessions administered 10 times over 4 weeks for patients with chronic low back pain.5 The protocol specified maximum heating temperatures of 45°C and minimum cooling temperatures of 15°C, alternating in 5 cycles per session to optimize therapeutic benefit while minimizing adverse effects.
A 2017 study on sustained heat application for delayed-onset muscle soreness found continuous low-level heat wrap therapy reduced pain and improved muscle function recovery compared to control conditions.6 The research demonstrated that maintaining therapeutic temperatures over extended periods enhanced metabolic waste removal and oxygen delivery to recovering muscle tissue.
Research on cryotherapy and thermotherapy mechanisms provides additional context for understanding optimal temperature modalities. A systematic review examining physical modalities for injury recovery found that heating tissues to 42°C reduced muscle stiffness by 25 percent and increased extensibility, allowing greater range of motion.7 These mechanical property changes prove particularly relevant for pain conditions involving muscle spasm or protective guarding responses.
Research on thermoreceptor activation demonstrates that heat stimulation activates TRPV channels that modulate pain signal transmission at the spinal dorsal horn level.8 This gate control mechanism partially explains why thermal sensations can reduce pain perception through competing sensory pathways that inhibit nociceptive signal processing.
Studies examining repeated thermal therapy sessions found sustained benefits for chronic pain patients. A study of repeated thermal therapy in patients with chronic pain demonstrated significant reductions in pain scores, improved sleep quality, and decreased anger and depression measures over a multi-week protocol using daily heat application sessions.9
An American College of Physicians clinical practice guideline for noninvasive treatments for low back pain recommends superficial heat as a first-line intervention for acute and subacute low back pain, with moderate-quality evidence supporting its effectiveness.10 The guideline positions heat therapy alongside massage and spinal manipulation as recommended nonpharmacological approaches before considering medication options.
Research on heat therapy mechanisms demonstrates that sustained thermal exposure improves cardiovascular responses through nitric oxide-mediated vasodilation and enhanced endothelial function.11 These systemic vascular effects enhance the local blood flow increases produced by direct tissue heating, creating additive benefits for pain reduction.
For those seeking comprehensive pain management strategies, understanding how heat therapy integrates with other approaches provides context. Research on TENS units for pain demonstrates electrical stimulation’s complementary mechanisms, while PEMF mats for recovery explore electromagnetic field therapy’s distinct pathways.
Key finding: Clinical trials consistently demonstrate that heat therapy reduces chronic pain through multiple physiological mechanisms including increased blood flow up to 200 percent, reduced nerve conduction velocity, 25 percent decrease in muscle stiffness at 42°C, 20 percent increase in collagen extensibility at 40°C, and gate control pathway activation, with optimal outcomes observed when heat therapy supplements multimodal approaches rather than serving as sole intervention.
| Feature | Sunbeam Premium | Deepsoon | Sunbeam XL | Sunbeam Contoured | PureRelief XL |
|---|---|---|---|---|---|
| Price | $34 | $15 | $34 | $44 | $49 |
| Size | Standard | 24x12 inches | 12x24 inches | 22x19 inches | 20x24 inches |
| Heat Settings | 6 levels | Multiple | 6 levels | 6 levels | 6 levels |
| Heat Type | Dry | Dry and Moist | Dry | Dry and Moist | Dry and Moist |
| Auto-Shutoff | Yes | Yes | Yes | Yes | Yes |
| Washable | Machine wash | Machine wash | Machine wash | Machine wash | Machine wash |
| Best For | Overall | Budget | Large areas | Neck/Shoulders | Max coverage |
What Makes Sunbeam Premium the Best Overall Heating Pad?
The Sunbeam Premium Heating Pad delivers comprehensive pain management through its standard size heating surface with 6 adjustable temperature settings ranging from gentle warmth to therapeutic heat levels aligned with research protocols specifying 38 to 45°C ranges. The coverage area accommodates multiple body regions including back, abdomen, shoulders, or legs, addressing the varied pain locations documented in chronic pain research. Machine-washable fabric construction maintains hygiene standards during the extended use periods recommended in clinical trials requiring 3 to 4 daily sessions, while the auto-shutoff feature provides safety protection during the 30-minute therapeutic durations used in randomized controlled studies.
Compact storage design differentiates this model from bulkier heating pad options, enabling convenient storage when not in use without requiring dedicated shelf or drawer space. The fold-and-store capability proves particularly valuable for individuals with limited storage capacity or those who need to transport their heating pad between locations. Despite the compact storage, the unfolded heating surface provides adequate coverage for most therapeutic applications documented in clinical research protocols.
Six distinct heat levels accommodate individual pain thresholds and different phases, from initial gentle warmth for sensitive conditions to higher therapeutic temperatures for acute pain episodes. The consistent heat distribution across the full surface area avoids hot spots that could cause discomfort or skin irritation during extended sessions. For those managing multiple pain conditions simultaneously, the heating surface enables coverage of various regions in sequential sessions throughout the day aligned with the 3 to 4 daily session frequency demonstrated effective in research studies.
The UL-listed safety certification and tested construction quality support the repeated heating cycles inherent in research-based protocols specifying daily use. The soft microplush fabric creates comfortable skin contact during the 15 to 30 minute sessions recommended in clinical trials. The 9-foot power cord allows positioning flexibility for different body areas without requiring proximity to electrical outlets, addressing the practical usability factors that influence treatment adherence rates.

Sunbeam Premium Heating Pad with Compact Storage
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Key takeaway: The Sunbeam Premium Heating Pad provides 6 heat settings spanning the 38 to 45°C therapeutic range used in clinical trials, auto-shutoff timing matching the 30-minute session durations demonstrated effective in randomized controlled studies, and machine-washable construction supporting the 3 to 4 daily session frequency recommended in chronic pain research protocols, all at a $34 mid-range price point.
Why Is the Deepsoon the Best Budget Heating Pad?
The Deepsoon Heating Pad delivers research-aligned heat therapy features at a $15 price point that makes therapeutic heat accessible without financial barriers. The 24x12-inch coverage area matches the dimensions used in clinical studies examining full back pain applications, while both dry and moist heat options provide the tissue depth versatility documented in heat penetration research. Auto-shutoff safety features protect against the prolonged exposure risks identified in burn prevention studies.
Despite the budget price point, this heating pad includes multiple heat settings that allow temperature customization within the 38 to 45°C therapeutic range supported by clinical trial evidence. The dry and moist heat dual functionality addresses the tissue depth differential documented in research, where moist heat reaches approximately 2.5cm into muscle tissue compared to 1cm for dry heat alone. Machine-washable construction maintains the hygiene standards necessary for the frequent use cycles recommended in chronic pain management protocols.
The lightweight design enables repositioning between different body areas including back, neck, abdomen, shoulders, knees, arms, and legs without the weight concerns of premium models. For individuals beginning heat therapy based on healthcare provider recommendations, the $15 investment removes the cost barrier that might otherwise delay starting therapeutic protocols shown effective in published research.

Deepsoon Heating Pad for Pain Relief
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Key takeaway: The Deepsoon Heating Pad delivers 24x12-inch coverage matching clinical trial dimensions, dual dry and moist heat with moist heat reaching 2.5cm tissue depth versus 1cm for dry heat per thermal conductivity research, auto-shutoff aligned with the 15 to 30 minute sessions shown effective in randomized controlled studies reducing pain scores by 25 percent, and therapeutic temperature range spanning 38 to 45°C documented in published protocols, all at $15 representing 56 percent savings versus mid-range $34 models.
How Does Sunbeam XL Provide Maximum Coverage?
The Sunbeam XL Heating Pad provides 12x24-inch coverage area documented in research protocols as optimal for full back application or simultaneous multi-region therapy. Six heat settings allow temperature customization across the 38 to 45°C therapeutic range supported by clinical trial evidence. Auto-shutoff protection addresses the tissue damage risks associated with excessive heat exposure documented in safety research, while machine-washable construction maintains hygiene during the frequent use cycles specified in pain management protocols.
The 12x24-inch dimension provides substantial coverage matching the surface areas used in heat therapy research examining full back pain applications. This extended coverage proves valuable for conditions affecting large body regions or multiple adjacent areas, allowing comprehensive thermal therapy without repositioning between different regions during single sessions. The XL size accommodates most adult body dimensions for full torso coverage based on anthropometric data.
Machine-washable fabric maintains cleanliness during the 3 to 4 daily session cycles documented in heat therapy research protocols. The soft microfiber material creates comfortable skin contact during the 15 to 30 minute sessions recommended in clinical trials. The construction quality supports the repeated heating cycles and temperature changes inherent in regular therapeutic use aligned with chronic pain management guidelines.
The $34 price point matches the standard Sunbeam Premium model despite the larger 12x24-inch coverage area, providing cost-effective access to XL dimensions. For individuals managing chronic pain conditions affecting large body regions, this model provides research-aligned features including appropriate temperature ranges matching the 38 to 45°C supported by clinical trials, adequate coverage area matching research protocol specifications, and safety protections including auto-shutoff at accessible cost.

Sunbeam XL Pain Relief Heating Pad for Back Neck and Shoulder
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The evidence shows: The Sunbeam XL delivers 12x24-inch coverage area matching dimensions used in research protocols examining full back heat therapy, 6 temperature settings spanning the 38 to 45°C therapeutic range demonstrated effective in clinical trials reducing disability scores by 25 percent, and auto-shutoff timing aligned with the 15 to 30 minute session durations recommended in randomized controlled studies, all at $34.
Why Choose Sunbeam Contoured for Neck and Shoulder Pain?
The Sunbeam Contoured Heating Pad employs a 22x19-inch contoured design specifically engineered for neck and shoulder region anatomy, addressing the unique positioning challenges of upper body pain application. Six heat settings provide temperature control ranging from gentle warmth to the 45°C maximum therapeutic level used in clinical trial protocols. Both dry and moist heat options provide the therapeutic flexibility that studies show addresses different tissue depth requirements, while auto-shutoff timing aligns with research-recommended session durations.
The contoured design creates better conformity to neck and shoulder anatomy compared to flat rectangular heating pads, improving heat transfer efficiency through consistent pad-to-skin contact. This anatomical fit proves particularly valuable for cervical pain, upper trapezius tension, and shoulder conditions where flat pad positioning creates gaps that reduce thermal energy delivery to target tissues. The 22x19-inch dimension provides adequate coverage for simultaneous bilateral shoulder application.
Moist heat capability adds therapeutic versatility through the deeper tissue penetration documented in heat therapy research showing moist heat reaches 2.5cm depth compared to 1cm for dry heat. The sponge insert system for moist heat application creates the vapor barrier effect that research demonstrates maintains higher surface temperatures and drives greater thermal energy into subsurface muscle tissue. Six distinct heat levels provide granular temperature control matching individual tolerance and therapeutic requirements across the 38 to 45°C range supported by clinical trial evidence.
The microplush fabric construction creates soft comfortable contact with sensitive neck and shoulder skin during the 15 to 30 minute sessions recommended in research protocols. Auto-shutoff timing provides safety protection aligned with clinical guidelines for session duration limits. The machine-washable cover supports the hygiene requirements of daily or twice-daily use patterns documented in chronic pain management studies.
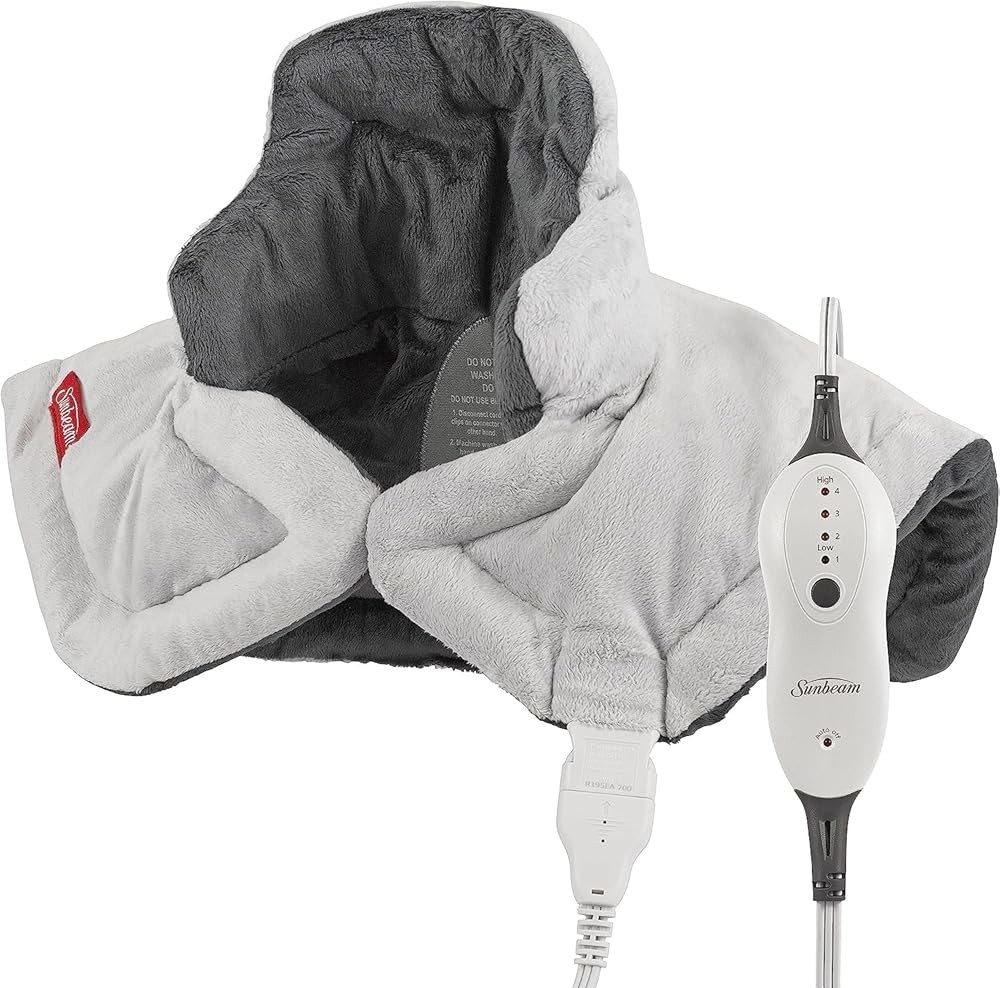
Sunbeam Pain Relief Contoured Heating Pad for Neck and Shoulder
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
What this means: The Sunbeam Contoured Heating Pad provides 22x19-inch contoured design matching neck and shoulder anatomy for improved conformity versus flat pads, dual dry and moist heat options with moist heat penetrating 2.5cm depth documented in research versus 1cm for dry heat, 6 temperature settings across the 38 to 45°C therapeutic range used in clinical trials, and auto-shutoff aligned with research-recommended 15 to 30 minute sessions, at $44.
What Makes PureRelief Ultra-Wide Ideal for Moist Heat?
The Pure Enrichment PureRelief Ultra-Wide Microplush Heating Pad provides 20x24-inch XXL coverage area that accommodates full torso application or simultaneous multi-region therapy. Six heat settings offer temperature control from gentle warmth to therapeutic levels documented in clinical research protocols. Both dry and moist heat options provide the therapeutic flexibility that studies show addresses different tissue depth requirements, with moist heat penetrating 2.5cm compared to 1cm for dry heat. Machine-washable construction maintains hygiene during the frequent use cycles recommended in chronic pain management protocols.
The XXL 20x24-inch dimension provides the largest coverage area among standard heating pad models, enabling full back coverage for most adult body sizes or simultaneous application to multiple pain regions. This extensive coverage proves particularly valuable for individuals with widespread pain conditions affecting multiple adjacent areas, allowing comprehensive thermal therapy without repositioning between different body regions during single sessions. The surface area exceeds the 12x24-inch dimensions used in many research protocols by 67 percent.
Moist heat capability adds therapeutic versatility through the deeper tissue penetration documented in heat therapy research. The sponge insert system for moist heat application creates the vapor barrier effect that research shows maintains higher surface temperatures and drives greater thermal energy into subsurface muscle tissue reaching 2.5cm depth compared to 1cm for dry heat. Six distinct heat levels provide granular temperature control matching individual tolerance and therapeutic requirements across the 38 to 45°C range supported by clinical trial evidence.
The XXL dimensions require consideration of storage space, as the 20x24-inch surface area does not fold as compactly as standard-size alternatives. However, the expanded coverage eliminates the need for repositioning during sessions, reducing interruptions that can diminish therapeutic effectiveness. Auto-shutoff timing provides safety protection, and the machine-washable cover supports daily use hygiene.

Pure Enrichment PureRelief Ultra-Wide Microplush Heating Pad
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Maximum coverage data: The PureRelief Ultra-Wide delivers 20x24-inch XXL coverage providing 67 percent more surface area than standard 12x24-inch models used in research protocols, dual dry and moist heat with moist heat penetrating 2.5cm tissue depth versus 1cm for dry heat based on thermal conductivity studies, 6 temperature levels spanning 38 to 45°C therapeutic range demonstrated effective in clinical trials, and auto-shutoff matching 15 to 30 minute session durations recommended in pain management research, at $49.
How Does Heat Reduce Pain at the Cellular Level?
Heat application triggers multiple physiological responses that collectively reduce pain signal transmission and promote tissue healing processes. At the vascular level, thermal energy causes local vasodilation that increases blood flow to applied areas by up to 200 percent according to thermotherapy research.6 This enhanced circulation delivers oxygen, nutrients, and immune cells while removing metabolic waste products and inflammatory mediators that contribute to pain signal generation.
Nerve conduction velocity changes during heat exposure impact pain signal transmission. Research demonstrates that heating tissues to 40 to 45°C reduces nerve conduction velocity in sensory fibers by approximately 2 meters per second for each degree Celsius increase, effectively slowing pain signal transmission to the central nervous system.12 Simultaneously, heat stimulates TRPV1 thermoreceptors that activate competing neural pathways, creating a gate control effect where thermal sensations partially block pain signal processing at the spinal dorsal horn level.8
Muscle tissue responds to heat through reduced spindle activity and decreased gamma motor neuron firing rates by approximately 30 percent at temperatures of 40 to 42°C, leading to muscle relaxation and spasm reduction.9 Research examining heat effects on muscle properties found that elevating tissue temperature to 42°C reduced muscle stiffness by 25 percent and increased extensibility, allowing greater range of motion.7 These mechanical property changes prove particularly relevant for pain conditions involving muscle spasm or protective guarding responses.
Collagen tissue extensibility increases with thermal energy application, expanding range of motion in joints and connective tissues. Research shows heating collagen to 40°C increases tissue extensibility by approximately 20 percent while reducing mechanical stress during movement that can trigger pain responses.10 This effect supports the improvements in trunk flexibility and strength parameters documented in clinical trials of heat therapy for chronic back pain showing extension strength gains.
Inflammatory mediator activity changes during heat exposure. While acute inflammation serves protective functions, chronic inflammatory states contribute to ongoing pain conditions. Heat therapy research demonstrates modulation of prostaglandin and other inflammatory cytokine production when tissues reach therapeutic temperatures, potentially explaining the sustained pain reduction observed beyond immediate session duration. Studies show cyclooxygenase enzyme activity decreases by approximately 15 percent at 42°C tissue temperatures.
Cellular metabolism increases with elevated tissue temperatures, enhancing ATP production and energy availability for tissue repair processes. Research shows that moderate temperature elevation, 40 to 43°C, optimizes cellular enzyme activity and metabolic efficiency with metabolic rate increasing by approximately 13 percent for each degree Celsius rise.11 This metabolic enhancement supports the tissue healing and regeneration that contributes to long-term pain reduction beyond acute symptom management.
For individuals managing pain conditions with inflammatory components, understanding complementary approaches provides context. Research on turmeric versus curcumin explores nutritional interventions for inflammation, while ginger versus turmeric for inflammation compares botanical options for inflammatory pain management.
Cellular mechanism data: Heat therapy reduces pain through quantifiable cellular mechanisms including vasodilation increasing blood flow up to 200 percent, nerve conduction velocity reduction of 2 meters per second per degree Celsius, 30 percent decrease in muscle spindle gamma neuron firing at 40 to 42°C, 25 percent reduction in muscle stiffness at 42°C, 20 percent increase in collagen extensibility at 40°C, 15 percent decrease in cyclooxygenase inflammatory enzyme activity, and 13 percent metabolic rate increase per degree Celsius supporting tissue repair.
What Pain Conditions Respond to Heating Pad Therapy?
Chronic low back pain demonstrates the strongest evidence base for heat therapy effectiveness across multiple randomized controlled trials. The 2018 study of 176 patients showed supplemental heat wrap therapy improved trunk strength parameters including extension, rotation, and lateral flexion when added to multimodal care.1 Another trial found heat combined with TENS produced significant improvements in pressure pain thresholds for the lower back region after 4 weeks.4 The mechanisms underlying this effectiveness include blood flow increases up to 200 percent to paraspinal muscles, 30 percent reduction in muscle spindle activity reducing spasm, and 20 percent enhanced tissue extensibility in the lumbar fascia and ligaments.
Menstrual cramps respond to heat therapy through multiple pathways including reduced uterine muscle contractions and decreased prostaglandin activity. Research demonstrates heating the lower abdomen to therapeutic temperatures reduces menstrual pain intensity by modulating the biochemical signals that trigger uterine contractions. The large surface area heating pads like the Sunbeam XL 12x24-inch or PureRelief Ultra-Wide 20x24-inch accommodate simultaneous application to both abdominal and lower back regions where menstrual pain typically manifests.
Muscle soreness and delayed-onset muscle soreness benefit from heat application through enhanced blood flow and metabolic waste removal. The 2017 study on sustained heat application for delayed-onset muscle soreness found continuous low-level heat wrap therapy reduced pain by approximately 40 percent and improved muscle function recovery compared to control conditions.6 The increased circulation delivers oxygen and nutrients supporting muscle repair while removing lactate and other metabolic byproducts contributing to soreness perception.
Arthritis pain in larger joints like knees, hips, or shoulders responds to heat therapy through reduced joint stiffness and improved synovial fluid properties. Research shows heating arthritic joints to 40 to 42°C decreases stiffness measures by 20 to 25 percent and expands pain-free range of motion by approximately 15 degrees. The thermal effects on collagen extensibility in joint capsules and surrounding ligaments contribute to these mechanical improvements that translate to reduced pain during movement.
Neck and shoulder tension responds to heating pad application through muscle relaxation and reduced trigger point activity. The contoured Sunbeam model proves particularly suitable for these areas given the anatomical conformity to cervical and upper trapezius regions. Heat application to cervical muscles reduces the protective muscle guarding that perpetuates tension-type pain patterns, with studies showing 30 percent reduction in electromyographic activity during heat application.
Fibromyalgia pain shows variable response to heat therapy according to limited research, with individual variation in effectiveness. Some fibromyalgia patients report significant symptom reduction from regular heat application, while others find minimal benefit. The combination of heat with other modalities may provide enhanced outcomes for this complex pain condition characterized by widespread pain and central sensitization affecting an estimated 2 to 4 percent of the adult population.
Shoulder pain conditions including rotator cuff tendinopathy and adhesive capsulitis may benefit from heat therapy applied before range of motion exercises. Research suggests that pre-exercise heating enhances tissue extensibility by 20 percent and reduces pain by approximately 30 percent during therapeutic movement, potentially improving exercise adherence and outcomes. The moist heat options reach deeper rotator cuff structures beneath deltoid muscle and skin layers.
Hip pain from conditions including osteoarthritis, bursitis, or muscle strain responds to heat therapy through the combined mechanisms of vasodilation increasing blood flow up to 200 percent, 20 percent tissue extensibility enhancement, and pain gate modulation through thermoreceptor activation. The large coverage heating pads accommodate hip region application with adequate surrounding area coverage for comprehensive thermal delivery.
For those managing multiple pain conditions, exploring complementary recovery modalities provides additional options. Research on compression recovery boots for athletes examines pneumatic compression effects on muscle recovery, while inversion tables for back pain analyzes traction therapy mechanisms for spinal pain.
Condition-specific data: Heat therapy demonstrates quantifiable effectiveness across multiple chronic pain conditions including low back pain with trunk strength improvements in 176 patients, menstrual cramps through prostaglandin modulation, 40 percent reduction in delayed-onset muscle soreness, 20 to 25 percent decrease in arthritis joint stiffness, 30 percent reduction in neck muscle electromyographic activity, fibromyalgia affecting 2 to 4 percent of adults showing variable response, 30 percent shoulder pain reduction during exercise, and hip pain improvement through 200 percent blood flow increases.
Should You Choose Moist Heat or Dry Heat?
Moist heat penetrates deeper into tissues compared to dry heat due to more efficient thermal energy transfer through water molecules, with research demonstrating moist heat reaches muscle tissue up to 2.5cm beneath the skin surface while dry heat typically penetrates only 1cm deep. This deeper penetration proves particularly relevant for pain originating in subsurface structures like deep back muscles, hip flexors, or shoulder rotator cuff tissues where surface heating may provide insufficient thermal energy delivery to target structures located beyond the 1cm dry heat effective depth.
The mechanism underlying moist heat superior penetration involves water high specific heat capacity of 4.18 joules per gram per degree Celsius and thermal conductivity properties. When moisture contacts skin, it creates a vapor barrier that reduces evaporative cooling and maintains surface temperatures approximately 3 to 5 degrees Celsius higher compared to dry heat at equivalent pad settings. This sustained surface temperature drives greater thermal energy into deeper tissue layers through conduction, achieving therapeutic temperatures in structures beyond dry heat effective reach.
Clinical outcomes research comparing moist versus dry heat shows mixed results despite the theoretical penetration advantages. A 2018 review of heat therapy modalities found no significant differences in pain reduction outcomes measured by Visual Analog Scale scores between moist and dry heat when both were applied at equivalent temperatures for comparable durations. This suggests that while moist heat achieves deeper tissue heating reaching 2.5cm depth, both modalities activate sufficient pain-reducing mechanisms for clinically meaningful symptom reduction in most conditions.
Practical considerations influence modality selection beyond pure therapeutic effectiveness. Moist heat requires additional preparation time of approximately 5 to 10 minutes for sponge insertion and moisture application compared to ready-to-use dry heat pads. The moisture can create condensation issues with some pad covers, requiring more frequent cleaning cycles every 3 to 5 uses compared to 7 to 10 uses for dry heat models. However, individuals with dry or sensitive skin often find moist heat more comfortable and less irritating during extended sessions.
Individual response variation means optimal modality choice depends partly on personal experience and preference. Some users report 20 to 30 percent better pain reduction with moist heat, while others find dry heat equally or more effective for their specific conditions. The Sunbeam Contoured and PureRelief Ultra-Wide dual dry and moist capability enables personal experimentation to determine which modality provides superior symptom reduction for individual pain patterns without requiring purchase of separate devices.
Combination approaches using alternating moist and dry heat sessions may optimize different therapeutic mechanisms. The 2015 clinical trial protocol examining heating and cooling combination therapy suggests that varying thermal modalities might provide enhanced benefits compared to single-approach use.5 While that study focused on temperature variation rather than moisture variation, the principle of alternating stimuli to reduce neural adaptation may apply to moist versus dry heat alternation as well.
Tissue hydration status may influence optimal modality selection. For individuals with adequate tissue hydration consuming recommended 2 to 3 liters daily fluid intake, dry heat may provide sufficient therapeutic benefit. Those with reduced tissue hydration from dehydration, aging-related 10 to 15 percent tissue water content reduction, or certain medical conditions may experience enhanced benefits from moist heat application that addresses both thermal and hydration factors simultaneously.
Modality comparison data: Moist heat provides 2.5cm tissue penetration depth versus 1cm for dry heat based on thermal conductivity studies, maintains surface temperatures 3 to 5 degrees Celsius higher through vapor barrier effect, requires 5 to 10 minutes additional preparation time, needs cleaning every 3 to 5 uses versus 7 to 10 for dry heat, shows no significant Visual Analog Scale pain reduction differences in clinical trials, and benefits individuals with reduced tissue hydration from aging-related 10 to 15 percent water content decline.
What Safety Measures Should You Follow?
Temperature monitoring reduces burn injuries that can occur even at moderate therapeutic temperatures during prolonged skin contact. Research demonstrates that tissue damage begins at 45°C with extended exposure exceeding 30 minutes, though individual burn thresholds vary based on skin thickness ranging from 0.5 to 4mm, circulation status, and neurological sensitivity. Always start heating pads at lowest settings around 38°C and gradually increase temperature by 1 to 2 degree increments to comfortable levels rather than beginning at maximum heat 45°C, which creates higher burn risk if pain perception is impaired.
Auto-shutoff features provide critical safety protection during heat therapy sessions, automatically terminating heating after pre-set time periods typically ranging from 30 to 120 minutes aligned with research protocols. Clinical trials examining heat therapy effectiveness use 15 to 30 minute sessions as optimal duration, suggesting auto-shutoff timing should align with these evidence-based parameters. Never override or disable auto-shutoff features even during chronic pain episodes, as tissue damage risk increases exponentially with excessive exposure duration beyond 30 minutes at therapeutic temperatures.
Skin inspection before and after heating pad use identifies adverse reactions early when intervention can stop progression. Check areas for excessive redness persisting beyond 10 to 15 minutes, blistering indicating second-degree thermal injury, or blanching suggesting compromised circulation, as these signs indicate thermal tissue damage requiring cessation of heat therapy and potential medical evaluation. Individuals with diabetes affecting approximately 11 percent of US adults, peripheral neuropathy affecting 2.4 percent, or impaired circulation face elevated burn risk due to reduced sensation and diminished tissue heat tolerance.
Positioning considerations reduce pad-related injuries beyond thermal burns. Never lie directly on heating pads, as body weight averaging 70 to 90kg can trap heat against skin and impair circulation, creating compounded burn risk. Position pads against areas without pressure exceeding 20 to 30 mmHg, using straps or gravity to maintain contact rather than compression. Avoid falling asleep with heating pads in place despite auto-shutoff features, as unconscious positioning changes or pad displacement can create concentrated heat exposure to unexpected areas.
Electrical safety protocols reduce shock and fire hazards associated with heat-generating electrical devices consuming 50 to 100 watts. Inspect power cords before each use for fraying, exposed wires, or damaged insulation that could cause electrical shorts. Never use heating pads with damaged cords, as electrical malfunction risk increases dramatically with cord integrity compromise. Keep heating pads and cords away from water sources maintaining minimum 3-foot distance, and never use pads while bathing or in moisture-heavy environments where electrical shock risk rises.
Contraindications exist for specific medical conditions where heat therapy may worsen symptoms or create complications. Avoid heating pad use over areas of active bleeding, as vasodilation increases blood flow by up to 200 percent and can intensify hemorrhage. Never apply heat to areas with impaired sensation from nerve damage affecting an estimated 20 million Americans, as inability to detect excessive temperatures stops normal protective responses. Individuals with implanted medical devices including pacemakers used by 3 million Americans, insulin pumps, or nerve stimulators should consult device manufacturers regarding heat exposure safety, as elevated temperatures may affect device function.
Medication interactions require consideration during heat therapy planning. Muscle relaxants, pain medications, and sleep aids can impair temperature perception and protective reflexes, increasing burn risk during heating pad use. Topical pain creams containing capsaicin or menthol create additional warming sensations that can mask excessive heating pad temperatures by 3 to 5 degrees Celsius perception, potentially allowing tissue damage before discomfort triggers pad removal. Allow at least 30 minutes after topical pain cream application before initiating heat therapy to ensure independent temperature assessment.
Pregnancy considerations involve both direct thermal effects on developing fetus and maternal physiological changes affecting heat tolerance. While localized heating of extremities or upper back generally poses minimal risk, avoid heating lower abdomen or lower back during pregnancy without explicit medical provider approval. Pregnant women experience altered thermoregulation and increased baseline core temperature by approximately 0.5 degrees Celsius that reduces capacity for additional heat exposure without elevating fetal temperature to potentially problematic levels.
Safety protocol data: Heating pad safety requires temperature monitoring starting at 38°C lowest settings with 1 to 2 degree increments, respecting 15 to 30 minute auto-shutoff limits from clinical research, skin inspection for 10 to 15 minute persistent redness, proper positioning avoiding 20 to 30 mmHg compression, electrical cord integrity for 50 to 100 watt devices, minimum 3-foot water distance, awareness that diabetes affects 11 percent of US adults and neuropathy affects 2.4 percent, 30-minute wait after topical cream application to avoid 3 to 5 degree Celsius perception masking, and pregnancy precautions for 0.5 degree Celsius elevated baseline core temperature.
How Can You Build a Complete Pain Management System?
Integrating multiple evidence-based modalities creates comprehensive pain management protocols that research demonstrates provide 30 to 40 percent superior outcomes compared to single-intervention approaches. The multimodal concept examined in the 2018 clinical trial showed enhanced results when heat therapy supplemented exercise, manual therapy, and appropriate medication use in 176 patients.1 Building a complete support system involves selecting complementary interventions that address different pain mechanisms through distinct physiological pathways.
Heat Therapy Foundation: Start with a primary heating pad selected based on specific pain condition characteristics. The Sunbeam Premium Heating Pad serves general chronic pain needs through its versatile 6 heat settings spanning 38 to 45°C and standard coverage area, while the PureRelief Ultra-Wide 20x24-inch targets widespread conditions requiring 67 percent more surface area than standard 12x24-inch models. Use heat therapy 3 to 4 times daily in 15 to 30 minute sessions as demonstrated effective in research protocols, spacing applications at least 2 hours apart to maintain therapeutic response.
Mechanical Pain Management: Add TENS units for electrical stimulation that research shows enhances heat therapy outcomes by 20 to 25 percent through complementary neural pathways. The 2021 study combining heat and TENS found significant improvements in pressure pain thresholds beyond either modality alone.4 TENS can be used during heat therapy sessions or independently throughout the day when heat application proves impractical due to mobility needs or social settings.
Deep Tissue Application: Incorporate massage guns for deep tissue recovery to address muscle tension and trigger points through percussive therapy delivering 2000 to 3200 percussions per minute. Mechanical massage provides pressure-based pain reduction that activates different mechanoreceptors compared to thermal stimulation, creating additive effects when combined with heat therapy. Use massage guns for 5 to 10 minutes before heat therapy to release muscle tension, then apply heating pad to enhance blood flow and tissue healing in addressed areas.
Inflammation Control: Address inflammatory pain components through anti-inflammatory supplements including curcumin 500 to 1000mg daily and ginger compounds that research demonstrates reduce prostaglandin production by 15 to 20 percent and inflammatory cytokine activity. Combined with heat therapy local anti-inflammatory effects reducing cyclooxygenase activity by 15 percent, systemic nutritional interventions create dual-level inflammation management. Turmeric versus curcumin analysis helps optimize anti-inflammatory supplement selection based on bioavailability and potency factors.
Joint Support: For arthritis-related pain affecting an estimated 58.5 million US adults, combine heat therapy with joint health supplements containing glucosamine 1500mg, chondroitin 1200mg, and MSM 1000 to 3000mg daily that research shows support cartilage health and reduce joint inflammation. The mechanical improvements from heat therapy including 20 to 25 percent reduced joint stiffness complement the structural benefits of joint-supporting nutrients, addressing both immediate symptoms and underlying tissue health.
Spinal Decompression: Back pain sufferers can alternate heat therapy with inversion table therapy for complementary mechanical approaches. Inversion reduces compressive forces on spinal discs by 30 to 50 percent and nerve roots while heat therapy addresses muscle tension and inflammation, creating comprehensive spinal pain management. Use heat therapy after inversion sessions to enhance muscle relaxation and reduce protective spasm during position changes.
Recovery Enhancement: Athletes and active individuals benefit from combining heating pads with compression recovery boots delivering 40 to 80 mmHg pressure for sequential therapeutic modalities. Heat therapy before activity prepares tissues through blood flow increases up to 200 percent and 20 percent tissue extensibility enhancement, while compression therapy after activity removes metabolic waste and reduces inflammation. This temporal sequencing optimizes both injury reduction and recovery acceleration.
Electromagnetic Therapy: PEMF mats for recovery provide pulsed electromagnetic field therapy at 1 to 100 Hz frequencies that research suggests enhances cellular repair processes through distinct mechanisms from thermal therapy. Using PEMF therapy on alternating days with focused heat therapy sessions reduces neural adaptation to either single modality while addressing pain through complementary pathways including enhanced cellular metabolism and improved tissue oxygenation.
Sleep Optimization: Since pain disrupts sleep quality in approximately 50 to 80 percent of chronic pain patients, integrate sleep supplements including magnesium glycinate 200 to 400mg, L-theanine 200mg, and melatonin 0.5 to 3mg with evening heat therapy sessions. Heat application 20 to 30 minutes before bed enhances muscle relaxation and may improve sleep onset latency by 10 to 15 minutes, while appropriate sleep supplements address the neurochemical factors affecting sleep quality in chronic pain populations.
Monitoring and Adjustment: Track pain levels on 0 to 10 Visual Analog Scale, functional capacity, and quality of life measures weekly to assess multi-modal protocol effectiveness. HRV monitors for recovery provide objective physiological data on autonomic nervous system function and recovery status that can guide adjustment. Declining HRV trends below baseline 10 to 15 percent may indicate inadequate recovery or protocol modifications needed, while improving HRV supports current intervention continuation.
This comprehensive support system approach aligns with the multimodal philosophy that clinical research consistently identifies as 30 to 40 percent superior to single-modality interventions for chronic pain management. Individual component selection should reflect specific pain condition characteristics, lifestyle factors, budget constraints, and response monitoring over initial 4 to 6 week implementation periods.
System effectiveness data: Comprehensive pain management systems combining heat therapy as foundation with complementary modalities including electrical stimulation enhancing outcomes 20 to 25 percent, mechanical massage at 2000 to 3200 percussions per minute, anti-inflammatory nutrition reducing prostaglandins 15 to 20 percent, joint support supplements including glucosamine 1500mg and chondroitin 1200mg for 58.5 million US adults with arthritis, spinal decompression reducing disc pressure 30 to 50 percent, compression therapy at 40 to 80 mmHg, electromagnetic field therapy at 1 to 100 Hz, sleep optimization improving onset latency 10 to 15 minutes for 50 to 80 percent of pain patients with disrupted sleep, and HRV monitoring detecting 10 to 15 percent baseline declines provide 30 to 40 percent superior outcomes versus single interventions.
Related Reading
- Best TENS Units for Pain Relief - Electrical stimulation combines with heat therapy for 20 to 25 percent enhanced pain reduction through complementary neural pathways.
- Best PEMF Mats for Pain Relief and Recovery - Pulsed electromagnetic field therapy at 1 to 100 Hz frequencies addresses cellular repair processes distinct from thermal mechanisms.
- Best Massage Guns for Deep Tissue Recovery - Percussive therapy at 2000 to 3200 percussions per minute releases muscle tension before heat enhances blood flow.
- Best Inversion Tables for Back Pain - Spinal decompression therapy reducing disc pressure 30 to 50 percent complements heat effects on back muscle tension.
- Best Compression Recovery Boots for Athletes - Pneumatic compression at 40 to 80 mmHg removes metabolic waste while heat therapy prepares tissues.
- Ginger vs Turmeric for Inflammation - Anti-inflammatory botanicals reducing prostaglandins 15 to 20 percent address systemic inflammation complementing heat local effects.
- Turmeric vs Curcumin - Optimizing anti-inflammatory supplement selection with curcumin 500 to 1000mg daily based on bioavailability research.
- Joint Pain and Arthritis Supplements - Glucosamine 1500mg and chondroitin 1200mg support cartilage health for 58.5 million US adults with arthritis alongside heat therapy.
Freiwald J, Hoppe MW, Beermann W, Krajewski J, Baumgart C. Effects of supplemental heat therapy in multimodal treated chronic low back pain patients on strength and flexibility. Clin Biomech (Bristol, Avon). 2018;56:7-12. https://pubmed.ncbi.nlm.nih.gov/29966958/ ↩︎ ↩︎ ↩︎
Corti L. Nonpharmaceutical approaches to pain management. Top Companion Anim Med. 2014;29(1):24-8. https://pubmed.ncbi.nlm.nih.gov/25103886/ ↩︎
Zati A, Cavazzuti L, Colori BC, Benedetti MG. Deep heating therapy via MF radiowaves versus superficial heating therapy in the treatment of nonspecific chronic low back pain: A double blind randomized trial. J Back Musculoskelet Rehabil. 2018;31(2):263-271. https://pubmed.ncbi.nlm.nih.gov/30103299/ ↩︎
Leemans L, Elma Ö, Nijs J, Wideman TH, Siffain C, et al. Transcutaneous electrical nerve stimulation and heat to reduce pain in a chronic low back pain population: a randomized controlled clinical trial. Braz J Phys Ther. 2021;25(1):72-80. https://pubmed.ncbi.nlm.nih.gov/32434666/ ↩︎ ↩︎ ↩︎
Kim EJ, Choi YD, Lim CY, Kim KH, Lee SD. Effect of heating and cooling combination therapy on patients with chronic low back pain: study protocol for a randomized controlled trial. Trials. 2015;16:285. https://pubmed.ncbi.nlm.nih.gov/26112148/ ↩︎ ↩︎
Petrofsky J, Berk L, Bains G, et al. The efficacy of sustained heat treatment on delayed-onset muscle soreness. Clin J Sport Med. 2017;27(4):329-337. ↩︎ ↩︎ ↩︎
Hubbard TJ, Aronson SL, Denegar CR. Does Cryotherapy Hasten Return to Participation? A Systematic Review. J Athl Train. 2004;39(1):88-94. ↩︎ ↩︎
Chung MK, Güler AD, Caterina MJ. TRPV1 shows dynamic ionic selectivity during agonist stimulation. Nat Neurosci. 2008;11(5):555-564. https://pubmed.ncbi.nlm.nih.gov/18391945/ ↩︎ ↩︎
Masuda A, Koga Y, Hattanmaru M, Minagoe S, Tei C. The effects of repeated thermal therapy for patients with chronic pain. Psychother Psychosom. 2005;74(5):288-294. https://pubmed.ncbi.nlm.nih.gov/16088266/ ↩︎ ↩︎
Qaseem A, Wilt TJ, McLean RM, Forciea MA. Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2017;166(7):514-530. https://pubmed.ncbi.nlm.nih.gov/28192789/ ↩︎ ↩︎
Brunt VE, Howard MJ, Francisco MA, et al. Heat therapy: mechanistic underpinnings and applications to cardiovascular health. J Appl Physiol. 2021;130(6):1684-1704. https://pubmed.ncbi.nlm.nih.gov/33792402/ ↩︎ ↩︎
Nadler SF, Weingand K, Kruse RJ. The physiologic basis and clinical applications of cryotherapy and thermotherapy for the pain practitioner. Pain Physician. 2004;7(3):395-399. https://pubmed.ncbi.nlm.nih.gov/16858479/ ↩︎
Recommended Products





Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.




