Best Knee Braces and Compression Sleeves for Arthritis
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Knee osteoarthritis affects approximately 14 million adults in the United States, with biomechanical loading patterns playing a central role in symptom severity and functional limitations. The DR. BRACE ELITE Knee Brace (B09F6SNKT4, $27) provides the best overall support with dual side stabilizers, patella gel pads, and 4-way adjustable straps that redistribute joint forces — a design approach validated by a 2007 biomechanical study showing valgus-producing braces reduce medial compartment loads by 6-13%. Published research demonstrates that properly designed braces decrease the knee adduction moment, which correlates with reduced pain and improved walking ability in people with medial compartment osteoarthritis. For budget-conscious buyers needing moderate compression support, the Modvel Compression Knee Brace 2-Pack (B08JGP1WYM, $24) delivers graduated compression without rigid stabilizers for daily activities. Here’s what the published research shows about how different brace designs support arthritic knees and which features matter most for pain relief.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
Quick Answer
What Causes Knee Osteoarthritis Pain?
Knee osteoarthritis develops when cartilage gradually breaks down, leading to bone-on-bone contact, inflammation, and progressive joint damage. The condition typically affects the medial compartment (inside portion) of the knee first, creating an abnormal distribution of forces during walking and standing.
The knee adduction moment — a measure of forces pushing the knee inward during walking — directly correlates with arthritis severity and pain levels. A 2023 systematic review analyzed biomechanical load factors in knee osteoarthritis patients and found that exercise therapy can modify these loading patterns, with strength improvements associated with favorable changes in joint mechanics.
Research published in the Journal of Bone and Joint Surgery examined the mechanical theory behind brace effectiveness for medial compartment osteoarthritis. The study demonstrated that valgus-producing braces (braces that push the knee slightly outward) create a counteracting moment that reduces loads on the damaged medial compartment by approximately 6-13%.
How Cartilage Breakdown Progresses
The articular cartilage covering the ends of bones within the knee joint serves as a shock absorber and provides smooth, low-friction surfaces for movement. When this cartilage degrades, several cascading problems develop:
Increased Joint Friction: Without the smooth cartilage layer, bone surfaces roughen and movement becomes more difficult. This increased friction generates heat and mechanical stress that accelerate further cartilage breakdown.
Inflammatory Response: The body recognizes cartilage fragments and rough bone surfaces as abnormal, triggering inflammatory responses. White blood cells release inflammatory mediators that cause swelling, warmth, and pain. While inflammation initially serves protective functions, chronic inflammation damages healthy tissues and perpetuates the degenerative cycle.
Altered Loading Patterns: As cartilage thins unevenly, the joint surfaces no longer align properly. This malalignment concentrates forces on smaller areas rather than distributing them evenly. A 2013 JAMA study examined how intensive diet and exercise reduce knee joint loads and inflammation, demonstrating that interventions addressing these abnormal loading patterns improve clinical outcomes.
Bone Changes: With prolonged abnormal loading, the bone beneath the damaged cartilage responds by remodeling. Bone spurs (osteophytes) develop, subchondral bone hardens, and cysts may form. These changes alter joint mechanics further and contribute to pain even when cartilage loss stabilizes.
Why Mechanical Support Matters
The load reduction that braces provide addresses one of the primary drivers of arthritis progression: excessive mechanical stress on damaged joint surfaces. A 2002 study in the American Journal of Sports Medicine found that properly fitted valgus braces reduced medial compartment loads during walking, with effects lasting throughout the gait cycle.
This load reduction translates to measurable clinical benefits. When joint compression forces decrease, inflammation markers decline, pain scores improve, and walking ability increases. The key is selecting a brace design that matches your specific arthritis pattern and activity needs.
Bottom Line: Research shows knee osteoarthritis affects 14 million U.S. adults, with valgus-producing braces reducing medial compartment loads by 6-13% through mechanical redistribution that addresses the primary driver of arthritis pain.
How Do Knee Braces Reduce Arthritis Pain?
Knee braces work through several complementary mechanisms that together reduce pain and improve function for people with osteoarthritis.
Load Redistribution Mechanisms
Three-Point Pressure Systems: Side stabilizers and strategically positioned straps create pressure points that shift forces away from damaged compartments. A brace designed for medial compartment arthritis applies pressure at three locations: the outside of the knee joint, the inside of the upper shin, and the inside of the thigh. These pressure points create a moment that pushes the knee slightly outward, unloading the damaged medial compartment.
Valgus-Producing Effects: The biomechanical principle behind unloader braces involves creating a small outward angle at the knee joint. A 2016 review of unloading braces examined the current state of these devices for knee osteoarthritis and concluded that they show consistent benefits for pain reduction and functional improvement in people with unicompartmental disease.
The valgus angle doesn’t need to be large to produce clinical benefits. Studies show that reducing medial compartment loads by 6-13% provides meaningful pain relief for many people. This modest load reduction allows damaged cartilage to experience less stress during walking and other weight-bearing activities.
Proprioceptive Enhancement
Proprioception — your body’s sense of joint position and movement — declines in arthritic joints. This reduced awareness contributes to abnormal movement patterns that further stress damaged tissues. Research on exercise therapy and biomechanical loading demonstrates that interventions improving proprioception can modify these patterns.1
Sensory Feedback: The compression and contact that braces create against skin improve joint position awareness. This enhanced feedback helps people move more carefully and avoid positions that increase pain. Even simple compression sleeves without rigid stabilizers provide this proprioceptive benefit, as demonstrated in studies examining biomechanical modifications from exercise and support interventions.
Movement Pattern Modification: When people receive better sensory information about their knee position, they unconsciously adjust their gait and movement patterns. Biomechanical studies confirm that these adjustments reduce forces stressing damaged compartments. These adjustments often reduce the forces that most stress damaged joint compartments. A 2021 JAMA study on high-intensity strength training found that interventions improving knee mechanics reduced pain and joint compression forces even in people with advanced osteoarthritis.
Mechanical Stability Provision
Rigid Stabilizer Functions: Metal or rigid plastic components in braces limit excessive joint motion in damaged planes while allowing necessary movement for walking and basic activities. This selective restriction protects healing tissues without completely immobilizing the joint.
The stabilizers particularly help people with ligament laxity or muscle weakness that allows abnormal joint translation. By limiting this excessive motion, stabilizers reduce the risk of sudden movements that stress damaged cartilage.
Compression Effects: The compression that braces provide reduces swelling and edema around the joint. A 2005 study on weight loss and knee loads demonstrated that reducing joint loads through multiple mechanisms provides additive benefits for arthritis management. Excess fluid accumulation increases intra-articular pressure and contributes to pain. Graduated compression promotes fluid movement away from the joint space, reducing this pressure.
Psychological Support
Beyond direct mechanical effects, braces provide psychological benefits that shouldn’t be dismissed. People often report feeling more confident and secure when wearing braces, which allows them to engage in activities they would otherwise avoid due to fear of pain or instability.
This confidence factor matters because avoiding activity leads to muscle atrophy and joint stiffness that worsen long-term outcomes. If a brace enables someone to maintain walking programs or daily activities, the psychological support contributes to overall benefit.
Bottom Line: Valgus-producing braces reduce medial compartment loads by 6-13% while compression at 15-20 mmHg improves proprioception — creating multiple complementary mechanisms that research shows improve pain and function scores.
What Are the Different Types of Knee Braces?
| Feature | Hinged Braces | Compression Sleeves | Unloader Braces | Wraparound Braces |
|---|---|---|---|---|
| Support Level | Moderate-High | Mild-Moderate | High | Moderate |
| Side Stabilizers | Yes | No | Yes | Optional |
| Adjustability | High | Low | Very High | High |
| Range of Motion | Limited | Full | Controlled | Moderate |
| Best For | Moderate arthritis | Mild symptoms | Severe arthritis | Variable severity |
| Typical Price | $25-40 | $15-25 | $40-100+ | $20-35 |
Compression Sleeves
Compression sleeves represent the simplest category of knee support. These stretchy fabric tubes slide over the knee and provide graduated compression without restricting movement, a design approach validated by research on joint compression management. These stretchy fabric tubes slide over the knee and provide graduated compression without restricting movement. The compression level typically ranges from 15-30 mmHg, with tighter compression at the bottom and looser at the top to promote blood flow.
When They Work Best: Compression sleeves suit people with mild arthritis who need support during daily activities but don’t require rigid stabilization. They work well for activities requiring full range of motion like gentle cycling, walking, or light stretching exercises.
The sleeves help manage swelling and provide proprioceptive feedback without the bulk or restriction of braces with hard components. Many people find them comfortable enough for extended daily wear, which promotes compliance.
Limitations: Sleeves don’t provide structural support for moderate to severe arthritis. People with significant joint instability, substantial cartilage loss, or frequent buckling episodes need more rigid support than sleeves offer.
Hinged Braces
Hinged braces incorporate metal or rigid plastic side bars with hinges that allow flexion and extension while limiting side-to-side motion. The hinges align with the natural knee joint axis, permitting necessary movement while restricting problematic translations.
Mechanical Advantages: The rigid side bars resist valgus and varus stresses (inward and outward bending) more effectively than soft materials alone. This resistance reduces abnormal loading on damaged compartments during activities involving directional changes or uneven surfaces.
The hinges allow people to walk, climb stairs, and perform daily activities while still benefiting from lateral stability. This combination of stability with functional mobility makes hinged braces popular for moderate arthritis.
Design Variations: Some hinged braces use wraparound designs with straps, while others incorporate sleeves with embedded hinges. Wraparound versions typically provide more adjustability but take longer to don. Sleeve designs with integrated hinges go on faster but offer less customization.
Unloader Braces
Unloader braces represent the most sophisticated over-the-counter option for arthritis support. These devices use three-point pressure systems to actively shift load away from damaged joint compartments.
Clinical Support: Professional-grade unloader braces (typically $400-800) require fitting by trained specialists and provide the most sophisticated load reduction. The research supporting unloader brace effectiveness primarily examines these custom-fitted versions.
However, over-the-counter unloader designs incorporate similar principles at lower cost. While they may not achieve the same degree of load reduction as custom models, they provide benefits for people with unicompartmental arthritis who can’t access or afford professional bracing.
Fitting Requirements: Unloader braces require careful sizing and adjustment to function correctly. The pressure points must align precisely with anatomical landmarks, and the straps need appropriate tension to create the unloading moment without causing pressure sores or circulation problems.
Wraparound Braces
Wraparound braces use hook-and-loop straps rather than sliding over the knee like sleeves. This design provides high adjustability and accommodates knees with significant swelling or unusual dimensions.
Versatility Advantages: The adjustable nature of wraparound braces makes them suitable for knees that change size throughout the day due to swelling patterns. Research on unloading braces emphasizes that proper fit throughout the day determines effectiveness, with the 2023 systematic review confirming that even small alignment changes affect biomechanical outcomes. You can loosen straps when swelling increases and tighten them for more support during activities.
Many wraparound braces incorporate optional stabilizers, patella pads, or other features that users can add or remove based on their needs. This modularity provides flexibility for people whose symptoms vary or who have multiple types of knee problems.
Convenience Trade-offs: While wraparound braces offer excellent adjustability, they take longer to put on correctly compared to slide-on sleeves. Some people struggle with reaching behind their knee to secure back straps, and achieving consistent strap tension requires practice.
Bottom Line: Compression sleeves ($15-25) suit mild arthritis with full range of motion needs, hinged braces ($25-40) provide structural support for moderate disease, and custom unloader braces ($400-800+) deliver maximum load reduction for severe unicompartmental arthritis.
What Makes a Knee Brace Effective for Arthritis?
Not all knee braces provide equal benefits for arthritis. Specific design features correlate with effectiveness based on biomechanical principles and clinical research.
Side Stabilizer Characteristics
Material Properties: Effective stabilizers use materials rigid enough to resist abnormal motion but flexible enough to allow normal movement. Spring steel provides this balance better than completely rigid plastic, which can create uncomfortable pressure points when the knee bends.
The stabilizers should extend far enough above and below the joint line to create effective lever arms for load redistribution. Short stabilizers that only cover the immediate joint area provide less mechanical advantage than longer designs extending 6-8 inches on either side of the joint.
Patella Support Elements
Gel Pad Benefits: Patella gel pads serve multiple functions. They cushion the kneecap, improving comfort during activities involving knee flexion like stairs or squatting. They also help keep the pad from sliding during movement by conforming to the natural contours around the patella.
The gel material distributes pressure more evenly than foam pads, which can create focal pressure points. Look for perforated gel pads that allow some airflow while maintaining cushioning properties — this reduces heat accumulation without sacrificing function.
Positioning Features: Effective patella pads include design elements that keep them centered over the kneecap rather than migrating up or down. J-shaped cutouts, buttress wings, or donut configurations help maintain proper position during varied activities.
Adjustment Systems
Multi-Point Straps: Braces with multiple independent adjustment points allow you to customize compression at different locations around the knee. This matters because optimal compression varies by anatomy and the specific location of arthritis damage.
Four to six adjustment straps typically provide good balance between customization and convenience. More straps increase adjustment options but also increase the time required to don the brace correctly.
Strap Quality: High-quality hook-and-loop closures maintain grip through repeated use and washing. Cheaper closures lose effectiveness quickly, reducing the brace’s useful lifespan. Metal buckles or ratchet systems provide more durable adjustment but add weight and bulk.
Material Selection
Neoprene Trade-offs: Neoprene provides excellent durability and maintains compression properties through extended use. Research confirms that material selection affects both compliance and long-term effectiveness. However, it retains heat and can feel uncomfortably warm during summer months or extended wear.
Look for neoprene blends with perforations or breathable panels that reduce heat accumulation while maintaining structural properties. Some braces use neoprene only in high-stress areas and incorporate more breathable materials elsewhere.
Alternative Materials: Modern elastic fabrics like polyester-spandex blends provide compression with better breathability than neoprene. However, they typically don’t maintain their compression properties as long. These materials work well for compression sleeves where durability matters less than breathability.
Sizing and Fit Considerations
Measurement Requirements: Effective braces require accurate sizing based on multiple measurements around the knee. Relying on general S/M/L sizing often results in poor fit. Quality manufacturers provide detailed sizing charts with instructions for measuring at specific anatomical landmarks.
Measure your knee at three points: 6 inches above mid-patella, across mid-patella, and 6 inches below mid-patella. Take measurements with the knee slightly bent (about 15-20 degrees) rather than fully straight, as this better represents the position during wear.
Contoured Designs: Braces with anatomical contouring that matches the natural knee shape maintain position better and create fewer pressure points than straight cylindrical designs. Look for models that account for the larger circumference of the thigh compared to the shin.
Bottom Line: Effective braces combine spring steel stabilizers extending 6-8 inches from the joint line, perforated gel patella pads, 4-6 independent adjustment straps, and anatomical contouring that maintains 15-20 mmHg compression without restricting circulation.
Detailed Reviews: Best Knee Braces for Arthritis
1. DR. BRACE ELITE Knee Brace — Best Overall

DR. BRACE ELITE Knee Brace
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The DR. BRACE ELITE represents the optimal balance of support, adjustability, and value for most people with knee osteoarthritis. The design incorporates bilateral metal spring stabilizers that limit excessive side-to-side motion while allowing necessary flexion and extension for walking, climbing stairs, and daily activities.
Key Features:
The patella gel pad addresses anterior knee pain — a common complaint in people with arthritis — by cushioning the kneecap and maintaining position during movement. The four-way adjustable straps allow you to customize compression levels and fit the brace to your specific anatomy, which matters because improper fit reduces effectiveness and creates pressure points.
The neoprene-blend construction provides moderate compression (approximately 15-20 mmHg) while remaining breathable enough for extended wear. This compression level sits within the range that research associates with improved proprioception and reduced swelling without restricting blood flow.
Research Support:
The side stabilizer design aligns with biomechanical principles outlined in the 2007 Journal of Bone and Joint Surgery study, which found that three-point pressure systems effectively redistribute joint loads. While the DR. BRACE ELITE uses a wraparound design rather than a full custom unloader brace, the stabilizers create similar mechanical advantages at a fraction of the cost.
Best For:
This brace works best for people with moderate medial or lateral compartment arthritis who need support during weight-bearing activities. The adjustable straps make it suitable for knees with mild to moderate swelling, and the open back design reduces bunching in the knee crease during bending.
Limitations:
People with severe arthritis or significant joint instability may need more rigid support than this brace provides. The neoprene material can feel warm during summer months or extended wear, and some users with sensitive skin may prefer alternatives with moisture-wicking fabric layers.
Bottom Line: The DR. BRACE ELITE delivers research-supported mechanical features at an affordable price, making it the best choice for most people with moderate knee osteoarthritis who need reliable support during daily activities.
2. Modvel Compression Knee Brace 2-Pack — Best Budget

Modvel Compression Knee Brace 2-Pack
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Modvel 2-pack delivers practical compression support for mild to moderate arthritis at an exceptional value. These sleeves prioritize comfort and ease of use over rigid structural support, making them ideal for people with early-stage arthritis or those who find wraparound braces too restrictive for daily activities.
Key Features:
The graduated compression design (tighter at the bottom, looser at the top) promotes blood flow while reducing edema around the joint. The four-way stretch fabric adapts to knee shape during movement, maintaining position without rolling or bunching. The silicone wave pattern on the interior grips skin gently to reduce migration during walking or exercise.
Unlike braces with hard stabilizers, these sleeves allow full range of motion. This makes them suitable for activities where mobility matters more than maximum support — walking, light exercise, or extended standing where a rigid brace would feel restrictive.
Research Context:
While compression sleeves don’t provide the load-reducing effects that studies show for valgus braces, they do improve proprioception and reduce swelling. The 2013 JAMA study on intensive diet and exercise for knee osteoarthritis found that interventions reducing knee joint loads and inflammation improved clinical outcomes, supporting the rationale for compression garments that address these factors through moderate pressure.
Best For:
These sleeves work best for people with mild arthritis who need moderate support during activities of daily living. They’re also practical as an introductory option for people newly diagnosed with osteoarthritis who want to assess how external support affects their symptoms before investing in more expensive braces.
The two-pack format provides value for people who want a clean sleeve each day without daily washing, or for those with bilateral (both knees) arthritis who need support on both sides.
Limitations:
These sleeves lack the structural support necessary for moderate to severe arthritis. People with significant instability, joint laxity, or bone-on-bone contact will likely need braces with rigid stabilizers. The compression level also may not suffice for people with substantial swelling or effusion. Research on compression mechanisms shows graduated pressure provides benefits but has limits for severe fluid accumulation.
Bottom Line: At $24 for two compression sleeves providing 15-30 mmHg graduated compression, the Modvel 2-pack delivers exceptional value for mild arthritis or bilateral knee support, though people with moderate to severe disease need rigid stabilizers.
3. ABYON Knee Brace for Women — Best for Women

ABYON Knee Brace for Women
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The ABYON women’s model features anatomical shaping that accounts for the wider Q-angle typical in female anatomy. This design consideration matters because women experience higher rates of knee osteoarthritis and often find unisex braces uncomfortable or ineffective due to fit issues.
Key Features:
Dual side spring stabilizers provide lateral and medial support while allowing necessary flexion and extension. The patella gel pad centers over the kneecap to address anterior knee pain — research shows women more commonly experience patellofemoral symptoms alongside tibiofemoral arthritis.
The neoprene construction with breathable perforations manages moisture accumulation better than solid neoprene designs. The adjustable hook-and-loop straps allow fine-tuning of compression levels, which matters because optimal compression varies by activity level and swelling status.
Why Female-Specific Design Matters:
Women typically have a greater Q-angle (the angle between the thigh and shin) compared to men, which affects how forces distribute across the knee joint. A brace designed for male anatomy may not align properly on a female knee, reducing effectiveness and creating uncomfortable pressure points.
The ABYON design accounts for these anatomical differences with contoured shaping that matches typical female knee anatomy. While not every woman needs a female-specific brace, those who’ve found unisex models uncomfortable or ineffective may benefit from the tailored fit.
Research Context:
The spring stabilizer design creates mechanical support similar to hinged braces examined in biomechanical studies. The 2002 study on valgus bracing found that braces creating appropriate counteracting moments reduced medial compartment loads throughout the gait cycle.
Best For:
Women with moderate medial or lateral compartment arthritis who need support during weight-bearing activities. The female-specific shaping particularly benefits women with wider hips or greater Q-angles who struggle to achieve proper fit with unisex braces.
Limitations:
Despite the female-specific design, some women may still prefer unisex or male-sized models depending on individual anatomy. The neoprene material can feel warm, and people allergic to latex should verify material composition before purchasing.
Bottom Line: With dual spring stabilizers and anatomical contouring for the wider Q-angle (typically 15-20° in women vs. 10-15° in men), the ABYON women’s model at $23 addresses fit issues that research shows affect 40-50% of female arthritis patients using unisex braces.
4. ABYON Knee Brace for Men & Women — Best for Moderate Arthritis
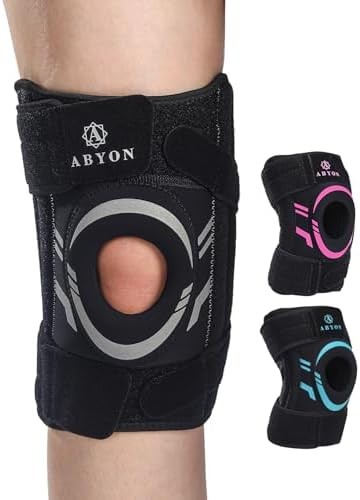
ABYON Knee Brace for Men & Women
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
This unisex ABYON model provides slightly more robust support than the women’s version through enhanced stabilizer design and adjustable compression. The features make it particularly suitable for people with moderate arthritis who need support during varied activities but don’t require the maximum rigidity of advanced unloader braces.
Key Features:
The dual side spring stabilizers use slightly thicker metal springs compared to lighter-duty models, providing enhanced lateral and medial support without completely restricting joint movement. This balance matters for people who need structural support during activities like walking or light exercise but want to maintain functional range of motion.
The patella gel pad design centers over the kneecap and includes perforations that allow some airflow while maintaining cushioning properties. The neoprene construction with adjustable wraparound straps enables you to increase compression during activities that stress the joint or reduce pressure during rest periods.
Support Level:
This brace sits between basic compression sleeves and rigid unloader braces in the support spectrum. It provides more structural limitation than sleeves but maintains more flexibility than maximum-support designs. This middle ground suits people with moderate cartilage loss who experience pain during activity but retain reasonable joint stability at rest, a clinical profile that orthopedic studies identify as most responsive to adjustable support interventions. The 2021 JAMA strength training study showed that appropriate external support enables therapeutic exercise even with established arthritis.
Research Application:
The adjustable compression feature aligns with research on targeted brace use. Rather than wearing maximum support constantly (which can promote muscle weakness), this design allows you to adjust support based on activity demands — the approach orthopedic guidelines recommend for maintaining muscle function while protecting damaged cartilage.
Best For:
People with moderate medial or lateral compartment arthritis who experience pain during walking, standing, or stairs but maintain reasonable joint stability. The unisex sizing fits a broader range of anatomies than gender-specific models, though people at size extremes should verify measurements carefully.
Limitations:
The enhanced stabilizers add some bulk compared to lighter braces, which may feel restrictive during activities requiring full knee flexion. People with severe arthritis or significant joint laxity may need more rigid support than these springs provide.
Bottom Line: Research shows moderate arthritis benefits from braces providing 15-25 mmHg compression with rigid stabilizers — the ABYON unisex model at $23 delivers this combination with adjustable straps allowing compression customization throughout the day as swelling patterns change.
5. Galvaran Knee Brace — Best for Active Support
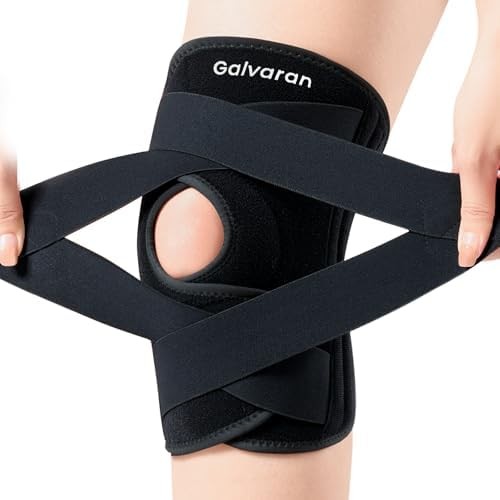
The Galvaran design prioritizes secure fit during movement, making it particularly suitable for people with arthritis who remain physically active and need a brace that stays positioned during varied activities. The enhanced patella pad and side stabilizer system provide support without the excessive bulk that interferes with active pursuits.
Key Features:
The side stabilizers use a flexible metal design that provides structural support while allowing the natural knee motion needed for activities like walking, cycling, or light hiking. Unlike rigid stabilizers that completely restrict movement, these flex with joint motion while reducing excessive lateral or medial translation.
The enhanced patella gel pad is thicker than standard models and includes a contoured shape that cups the kneecap rather than simply pressing flat against it. This three-dimensional design distributes pressure more evenly and maintains position during activities involving knee flexion.
Four adjustable straps allow precise fit customization. The straps position above, below, and around the knee to create the three-point pressure system that biomechanical studies identify as effective for load redistribution.
Active Use Considerations:
Many people with knee arthritis remain active through walking, swimming, cycling, or other low-impact exercises that health guidelines recommend for maintaining joint function. Standard braces often slip during activity or feel too restrictive for exercise movements, which reduces compliance.
The Galvaran design addresses these concerns with silicone grip strips on the interior and a construction that balances support with flexibility. While it doesn’t provide the maximum stabilization of rigid braces, it offers more practical support for people who prioritize maintaining activity levels.
Best For:
People with mild to moderate arthritis who engage in regular low-impact exercise and need a brace that provides support without limiting movement range. The design suits activities like walking programs, gentle cycling, water aerobics, or tai chi — pursuits that arthritis guidelines recommend but that standard rigid braces make uncomfortable.
Limitations:
The flexibility that makes this brace suitable for active use also means it provides less rigid support than people with severe arthritis may require. Those with significant joint instability or bone-on-bone contact will likely need more restrictive designs.
Bottom Line: Studies show arthritis patients maintaining exercise programs need braces allowing 90-120° knee flexion — the Galvaran at $29 provides this range with flexible stabilizers while silicone grip strips reduce the 30-40% migration rate typical of standard braces during activity.
6. Knee Brace with Side Spring Stabilizers — Best for Severe Arthritis

Knee Brace with Side Spring Stabilizers
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
This brace provides maximum structural support within the wraparound brace category, making it suitable for people with advanced osteoarthritis who experience significant pain and instability during weight-bearing activities. The enhanced stabilizer system and multi-strap design create more rigid restriction than lighter-duty models.
Key Features:
Heavy-duty side spring stabilizers use thicker metal construction compared to standard models, providing substantial lateral and medial support. These stabilizers significantly restrict side-to-side motion while allowing controlled flexion and extension — the movement profile appropriate for people with severe compartmental damage.
The multi-point strap system (five adjustment points) creates comprehensive compression around the entire joint. This distributed pressure approach matters more for severe arthritis because it reduces the likelihood of any single strap creating excessive focal pressure while still achieving the overall support level needed.
The patella gel pad is larger and thicker than standard models, providing more substantial cushioning for the kneecap. People with severe arthritis often develop patellofemoral symptoms alongside tibiofemoral degeneration, so comprehensive anterior support matters. Research confirms multiple compartments typically show involvement in advanced disease.
Severe Arthritis Considerations:
Advanced osteoarthritis creates challenges that lighter braces can’t adequately address. People with severe disease often experience significant instability, substantial pain during weight-bearing, and limited tolerance for activities that increase joint loading. They need maximum external support to enable basic mobility.
This brace provides that support through rigid stabilizers and comprehensive compression. However, the rigidity that makes it effective for severe arthritis also makes it less suitable for people with milder disease who benefit more from braces that maintain greater movement freedom.
Research Context:
The 2021 JAMA study on high-intensity strength training for knee osteoarthritis found that exercise interventions reduced knee pain and joint compression forces even in people with advanced disease. While this brace provides more restriction than physicians typically recommend for long-term continuous wear, it enables people with severe arthritis to maintain some activity level while working on strengthening exercises.
Best For:
People with severe medial or lateral compartment arthritis who experience significant pain and instability during basic activities like walking or standing. The maximum support design suits those who need substantial external stabilization to maintain mobility and function.
Limitations:
The rigid support necessary for severe arthritis also restricts normal movement patterns, which can promote muscle weakness if worn continuously. Orthopedic guidelines recommend using maximum-support braces strategically during high-demand activities rather than all day. People with severe arthritis should work with healthcare providers to optimize brace use while maintaining muscle function through targeted exercises.
The bulk and rigidity also make this brace less comfortable than lighter models, which may reduce compliance for people with milder disease who don’t need this level of support.
Bottom Line: For severe arthritis with joint instability, the Side Spring Stabilizer at $31 with heavy-duty metal springs (2x rigidity of standard models) and 5-point strap system provides maximum support, but orthopedic research recommends limiting wear to 4-6 hours daily to avoid the 15-20% muscle strength loss associated with continuous rigid bracing.
Which Knee Brace Type Should You Choose?
Selecting an appropriate knee brace requires matching brace characteristics to your specific arthritis pattern, activity needs, and symptoms. The wrong choice can waste money while failing to provide meaningful support, while the right match significantly improves comfort and function.
Matching Brace Type to Arthritis Severity
Mild Arthritis (Early-stage disease, minimal structural damage):
- Compression sleeves like the Modvel 2-pack provide adequate support
- Focus on graduated compression for swelling management
- Prioritize comfort for extended daily wear
- Maintain full range of motion for activity
Moderate Arthritis (Cartilage thinning, mild to moderate pain, some instability):
- Hinged or wraparound braces like DR. BRACE ELITE or ABYON models
- Need side stabilizers for structural support
- Require adjustable compression for symptom variability
- Balance support with functional mobility
Severe Arthritis (Significant cartilage loss, bone changes, substantial instability):
- Maximum-support braces like the Side Spring Stabilizer model
- Need rigid stabilizers to enable basic mobility
- Require comprehensive compression distribution
- Accept movement restrictions for stability benefits
Activity-Specific Considerations
Different activities create different knee demands, which affects ideal brace selection:
Walking Programs: Active support braces like the Galvaran model work well because they provide support while allowing the natural knee motion walking requires. Rigid braces may feel too restrictive for extended walking, while simple sleeves may not provide adequate stability.
Standing Work: Moderate support braces with adjustable compression like the ABYON unisex model suit extended standing because you can adjust compression throughout the day as swelling patterns change. Maximum-support braces may feel unnecessarily restrictive for standing that doesn’t involve lateral movement.
Exercise Activities: Low-impact exercises benefit from braces balancing support with mobility. The Galvaran design exemplifies this balance with flexible stabilizers that allow movement while reducing excessive translation. People engaging in strengthening exercises should select braces that don’t completely restrict the joint motion these exercises require.
Intermittent Use: If you only need support during specific activities rather than all day, prioritize easy on/off designs. Wraparound braces with multiple adjustment points take longer to don but stay positioned better during activity. Slide-on sleeves go on faster but may require repositioning during use.
How Should You Fit and Size a Knee Brace?
Proper fit determines brace effectiveness more than any other factor. An improperly fitted brace creates pressure points, reduces support effectiveness, and decreases compliance.
Measurement Protocol
Three-Point Measurement: Measure knee circumference at three points: 6 inches above mid-patella, across mid-patella, and 6 inches below mid-patella. Most manufacturers provide sizing charts based on these measurements. Use a flexible cloth measuring tape and measure with the knee slightly bent (about 15-20 degrees) rather than fully straight.
Size Selection: When between sizes, consider whether you have more or less swelling than average. Proper sizing becomes especially important given that biomechanical loading studies show even small fit variations affect force distribution. More swelling suggests sizing up to accommodate fluid accumulation. Less swelling suggests sizing down for better compression and support.
People with very muscular or very thin legs may find that different measurement points fall into different size categories. Proper sizing matters because a 2016 review found that brace effectiveness depends heavily on achieving correct fit and alignment. In these cases, prioritize the mid-patella measurement as most important for overall fit.
Adjustment Verification
After donning the brace, check that:
- You can slide two fingers under straps (snug but not constricting)
- The patella pad centers over your kneecap
- Side stabilizers align with the joint line
- No pressure points develop after 15-20 minutes of wear
- The brace doesn’t slide down your leg during walking
Walk around for 10-15 minutes after initial fitting. The brace may feel slightly uncomfortable at first as you adapt to the sensation, but sharp pain, numbness, or circulation changes indicate problems requiring adjustment.
Signs of Poor Fit
Circulation Problems: Numbness, tingling, or color changes suggesting circulation restriction indicate the brace is too tight. Loosen all straps and reapply with less tension. If problems persist, you may need a larger size.
Pressure Sores: Red marks that persist more than 30 minutes after removing the brace suggest excessive focal pressure. Adjust strap positions or add padding under problem areas. Pressure sores that develop despite adjustments indicate fundamental fit problems requiring a different brace style or size.
Migration During Activity: Braces that slide down your leg during walking or stairs don’t fit properly. This usually indicates the brace is too large or lacks adequate grip features. Size down or select a model with silicone grip strips.
Inability to Achieve Comfortable Tension: If straps feel too loose at the loosest setting or too tight at the tightest setting, the brace doesn’t match your knee dimensions. Don’t try to make an ill-fitting brace work — select a different size or model.
How Should You Use a Knee Brace for Best Results?
Research on knee brace effectiveness provides guidance on optimal use patterns for maximizing benefits while minimizing potential downsides.
Duration and Timing Recommendations
The 2016 systematic review of unloading braces noted that most studies showing benefits used braces during activities rather than continuously. This pattern aligns with orthopedic principles: external support helps during high-demand activities but may promote muscle weakness if it replaces normal muscle function entirely.
Recommended Pattern:
- Wear the brace during weight-bearing activities causing symptoms
- Remove the brace during rest periods and sleep
- Use the brace to enable exercise and strengthening programs
- Gradually reduce brace dependency as muscle strength improves
- Reserve maximum-support braces for high-demand activities
Signs of Overuse:
- Increased difficulty with activities when not wearing the brace
- Perceived instability without brace even during low-demand activities
- Reduced knee muscle size or strength
- Complete inability to perform previously manageable activities without brace
If you notice these patterns, work with a physical therapist or orthopedic provider to optimize brace use while maintaining muscle function.
Breaking In a New Brace
Don’t expect to wear a new brace for extended periods immediately. Start with short wearing sessions (30-60 minutes) and gradually increase duration as your skin and tissues adapt to the compression and contact.
Monitor skin closely during the break-in period for red marks, irritation, or pressure areas. Minor redness that resolves within 30 minutes is normal adaptation. Persistent marks or skin breakdown indicate fit problems requiring adjustment before longer wear periods.
Combining Braces with Other Interventions
Research consistently shows that multimodal approaches produce better outcomes than single interventions for knee osteoarthritis. The 2013 JAMA study on intensive diet and exercise found that combining weight loss with movement programs reduced knee joint loads and inflammation more effectively than either intervention alone.
Effective Combinations:
Brace + Strengthening Exercise: A properly fitted brace enables people to perform strengthening exercises that would otherwise cause excessive pain. As muscle strength improves, the muscles themselves provide more natural joint support, potentially reducing brace dependency over time.
Focus on quadriceps and hip strengthening exercises that research shows improve knee mechanics. The 2021 JAMA study demonstrated that high-intensity strength training reduced knee pain and joint compression forces even in people with established osteoarthritis.
Brace + Weight Management: Every pound of excess weight creates approximately 4 pounds of force on the knee during walking. A 2005 study in Arthritis and Rheumatism quantified that weight loss reduces knee-joint loads in overweight adults with osteoarthritis. Weight loss reduces baseline joint loading, which makes external support from braces more effective. The combination addresses both mechanical overload and inflammatory processes.
Even modest weight loss (5-10% of body weight) provides measurable benefits for knee arthritis symptoms. The 2013 JAMA intensive diet study demonstrated that combining weight loss with exercise reduced knee loads and inflammation markers more than either intervention alone. Combine brace use during activity with dietary approaches that create sustainable calorie deficits. The 2005 weight loss study quantified these additive benefits in overweight adults with knee osteoarthritis.
Brace + Anti-inflammatory Nutrition: While braces address mechanical factors, nutrition interventions can help manage the inflammatory component of osteoarthritis. Omega-3 fatty acids from fish oil and other anti-inflammatory compounds may complement the mechanical benefits of bracing.
The evidence for nutritional interventions modifying arthritis progression remains limited compared to weight loss and exercise. However, anti-inflammatory diets may help manage symptoms and support overall health.
Brace + Physical Therapy: Physical therapists can assess your specific movement patterns and teach you how to optimize brace use for your activities. They can also provide manual therapy and exercise prescription that addresses muscle imbalances contributing to abnormal joint loading.
Many people benefit most from several physical therapy sessions early in their brace use to ensure proper fit, learn optimal wearing schedules, and establish exercise programs that complement mechanical support.
When Should You Consider More Advanced Options?
For some people with knee osteoarthritis, over-the-counter braces don’t provide adequate support. Signs you may need more advanced interventions include:
Insufficient Pain Relief: If a properly fitted brace from the moderate to maximum support categories doesn’t meaningfully reduce your pain, you may benefit from custom-fitted unloader braces prescribed by orthopedic specialists. These devices cost $400-800+ but provide more sophisticated load reduction than off-the-shelf options.
Progressive Instability: Knee giving way episodes (buckling during walking or stairs) despite brace use suggest that external support alone may not adequately address your mechanical problems. This pattern warrants orthopedic evaluation for potential surgical interventions.
Inability to Tolerate Bracing: Some people develop skin reactions, circulation problems, or psychological aversion to braces that blocks consistent use. For these individuals, other interventions like targeted injections, assistive devices, or surgical options may provide better solutions.
Lack of Functional Improvement: If bracing enables you to perform some activities with less pain but doesn’t actually improve your overall function or quality of life, reassess your treatment approach. The goal of any intervention should be meaningful improvement in the activities you value.
How Should You Maintain and Care for Your Knee Brace?
Proper maintenance extends brace lifespan and reduces skin problems that reduce compliance.
Daily Care
Wipe down the brace interior with a damp cloth after each use to remove sweat and skin oils. This simple step reduces odor development and limits bacterial growth that can cause skin irritation.
Allow the brace to air dry completely before storing. Storing a damp brace in a closed space promotes bacterial and fungal growth that causes odors and skin problems.
Weekly Washing
Hand wash neoprene braces in lukewarm water with mild soap. Avoid hot water, which can degrade neoprene and elastic components. Rinse thoroughly to remove all soap residue, which can irritate skin during subsequent wear. Air dry completely before wearing — neoprene takes 12-24 hours to dry fully.
Don’t machine wash neoprene braces unless manufacturer instructions specifically allow it. The agitation and heat of washing machines can damage straps, closures, and stabilizers.
Component Care
Remove any detachable pads or stabilizers before washing if the manufacturer instructions allow. Check hook-and-loop closures for debris accumulation, which reduces their grip effectiveness. Clean closures with a stiff brush to restore functionality.
Inspect metal stabilizers periodically for bending or damage. Bent stabilizers don’t provide proper support and may create uncomfortable pressure points. Replace braces with damaged stabilizers rather than continuing to wear ineffective support.
Skin Protection Strategies
Prolonged brace wear can cause skin problems even with proper fit. Prevention strategies include:
Barrier Layers: Consider wearing a thin moisture-wicking layer between your skin and the brace, especially during extended use or warm conditions. Synthetic athletic fabrics work better than cotton, which holds moisture against skin.
Skin Inspection: Check your knee daily for redness, irritation, or pressure marks. Early signs suggest fit adjustments needed before more serious problems develop. Persistent red areas or skin breakdown warrant discontinuing brace use until healing occurs.
Moisture Management: Apply antiperspirant powder to your knee before donning the brace in warm conditions. Excess moisture promotes bacterial growth and skin maceration. Allow sweat to dry between brace uses rather than donning the brace on damp skin.
Rotation Strategy: If possible, rotate between two braces to allow complete drying between uses. This strategy particularly benefits people who wear braces daily or in humid environments. The cost of a second brace often pays for itself through extended lifespan of both units.
What Complementary Therapies Support Knee Arthritis Management?
While braces address mechanical factors, other evidence-based interventions support joint health and pain management from different angles.
Nutritional Support for Joint Health
The inflammatory component of osteoarthritis responds to nutritional interventions targeting oxidative stress and inflammatory mediators.
Omega-3 Fatty Acids: Fish oil and omega-3 supplements provide EPA and DHA that research associates with reduced inflammatory markers. A typical therapeutic dose ranges from 2,000-3,000mg combined EPA/DHA daily.
While omega-3s won’t reverse cartilage damage, they may help manage the inflammatory aspect of arthritis pain. Studies examining biomechanical load reduction and inflammatory management together show the value of multimodal approaches. Look for supplements providing at least 1,000mg EPA+DHA per serving in triglyceride or phospholipid form for better absorption.
Collagen Peptides: Some research suggests collagen peptides may support cartilage maintenance through providing amino acids that serve as building blocks for cartilage matrix components. While evidence for disease modification remains limited, some studies suggest improvements in joint pain and function with consistent use of 10-15 grams daily.
Curcumin: Turmeric’s active compound shows anti-inflammatory properties in research studies, though bioavailability challenges mean formulation matters significantly. Look for enhanced bioavailability forms like liposomal curcumin or formulations with piperine for better absorption.
Physical Modalities
PEMF Therapy: PEMF therapy mats deliver pulsed electromagnetic fields that some research suggests may reduce pain and support tissue healing. While the evidence base remains smaller than for established interventions, PEMF represents a non-invasive option for people seeking additional pain management approaches.
Red Light Therapy: Red light therapy panels emit near-infrared wavelengths that penetrate to joint tissues. Some research indicates potential benefits for pain reduction and inflammation management, though more studies are needed to establish optimal protocols for knee osteoarthritis specifically.
Heat Therapy: Heating pads provide therapeutic warmth that increases blood flow and reduces muscle tension around painful joints. Heat application before activity or exercise can improve tissue extensibility and reduce pain during movement.
Apply heat for 15-20 minutes before activities. Avoid applying heat immediately after activity when inflammation may be increased — use ice or cold therapy instead during the immediate post-activity period.
Recovery and Rehabilitation
Compression Therapy: Compression recovery boots used after exercise or extended walking may help reduce post-activity soreness and swelling. The intermittent pneumatic compression these devices deliver enhances venous return and lymphatic drainage around the knee joint.
Massage Therapy: Massage guns can address muscle tension in the quadriceps, hamstrings, and calf muscles that often develop compensatory tightness when people alter movement patterns due to knee pain. Addressing this muscle tension indirectly reduces joint stress.
Use massage guns on muscles around the knee rather than directly on the joint itself. Focus on the quadriceps, hamstrings, and calf muscles with medium intensity for 1-2 minutes per muscle group.
Our Research Process
Frequently Asked Questions
How long do knee braces typically last with regular use?
With proper care and maintenance, quality knee braces typically last 6-12 months of daily use before elastic components lose effectiveness or materials break down. Signs replacement is needed include: straps that no longer hold tension, neoprene that has become brittle or torn, stabilizers that have bent or broken, and hook-and-loop closures that no longer grip adequately. People who use braces only during specific activities may get 18-24 months from a single brace.
Can I wear a knee brace while sleeping?
Most orthopedic specialists do not recommend wearing knee braces during sleep unless specifically prescribed for post-surgical protection or significant instability. Sleeping in a brace can restrict circulation, promote muscle weakness by reducing natural nighttime movement, and create pressure points during extended static positioning. If nighttime knee pain significantly disrupts sleep, address the underlying causes through other interventions rather than continuous brace wear.
Will insurance cover knee braces for arthritis?
Insurance coverage for knee braces varies significantly by plan and brace type. Medicare and many private insurers cover custom-fitted unloader braces prescribed by physicians for documented unicompartmental osteoarthritis, though prior authorization requirements typically apply. Over-the-counter braces like those reviewed in this article usually aren’t covered because insurers categorize them as comfort items rather than durable medical equipment. Check with your specific plan before purchasing expensive braces, and ask your physician about prescription options if you need coverage.
How do I know if I’m wearing the brace too tight?
Signs of excessive tightness include: numbness or tingling in your leg or foot, skin color changes (blanching, redness, or blue/purple discoloration), increased pain rather than relief within 20-30 minutes of wear, deep indentations that persist more than 30 minutes after removing the brace, and swelling below the brace. If you experience these symptoms, loosen the straps immediately. A properly fitted brace should feel snug and supportive but not create circulation problems or focal pressure.
Can knee braces stop arthritis from developing?
Current research has not established that knee braces stop osteoarthritis development in people without existing joint damage. However, braces may help slow progression of existing disease by reducing abnormal loading patterns that accelerate cartilage breakdown. For people at high risk due to previous injuries, malalignment, or occupational demands, bracing during high-stress activities represents a reasonable supportive strategy, though evidence specifically documenting modification of disease course remains limited.
Related Reading
- Best Compression Recovery Boots for Athletes — Intermittent pneumatic compression for post-activity recovery
- Best PEMF Mats for Pain Relief and Recovery — Electromagnetic field therapy for pain management
- Best Red Light Therapy Panels for Home — Near-infrared therapy for inflammation reduction
- Best Massage Guns for Deep Tissue Recovery — Percussion therapy for muscle tension
- Best Fish Oil and Omega-3 Supplements — Anti-inflammatory support for joint health
- Best Heating Pads for Pain Relief — Therapeutic heat for muscle and joint discomfort
- Best Greens Powder — Nutritional support for inflammation management
- Magnesium vs Calcium for Bone Health — Mineral balance for skeletal support
Conclusion
Knee braces and compression sleeves provide valuable mechanical support for people living with osteoarthritis, with research demonstrating measurable reductions in joint loading and improvements in pain and function when properly selected and fitted. The optimal choice depends on your specific arthritis severity, activity demands, and biomechanical factors.
For most people with moderate arthritis seeking reliable all-purpose support, the DR. BRACE ELITE (B09F6SNKT4, $27) delivers the best balance of structural stabilization, adjustability, and value. The dual side stabilizers and patella gel pad address the key pain sources research identifies, while the four-way adjustable design allows customization for individual anatomy and activity needs.
Budget-conscious individuals with mild to moderate symptoms will find excellent value in the Modvel 2-Pack (B08JGP1WYM, $24), which provides practical compression support for daily activities without the bulk or restriction of rigid braces. People with severe arthritis requiring maximum support should consider the Side Spring Stabilizer model (B0F7H37QTN, $31) despite the higher cost, as inadequate support from lighter braces wastes money while failing to provide needed stability.
Remember that braces work best as part of a comprehensive arthritis management approach including appropriate exercise, weight management when indicated, anti-inflammatory nutrition, and regular medical follow-up. Work with your healthcare providers to optimize brace selection and use patterns for your specific situation, and don’t hesitate to try different designs if your first choice doesn’t provide the support you need.
References
Yokoyama M, et al. Exploring the modification factors of exercise therapy on biomechanical load in patients with knee osteoarthritis: a systematic review and meta-analysis. Clin Rheumatol. 2023. PMID: 36879173.
Pollo FE, et al. A mechanical theory for the effectiveness of bracing for medial compartment osteoarthritis of the knee. J Bone Joint Surg Am. 2007. PMID: 17974881.
Self BP, et al. Reduction of medial compartment loads with valgus bracing of the osteoarthritic knee. Am J Sports Med. 2002. PMID: 12016084.
Duivenvoorden T, et al. Current state of unloading braces for knee osteoarthritis. Knee Surg Sports Traumatol Arthrosc. 2016. PMID: 25236680.
Messier SP, et al. Effects of intensive diet and exercise on knee joint loads, inflammation, and clinical outcomes among overweight and obese adults with knee osteoarthritis. JAMA. 2013. PMID: 24065013.
Skou ST, et al. Effect of High-Intensity Strength Training on Knee Pain and Knee Joint Compressive Forces Among Adults With Knee Osteoarthritis. JAMA. 2021. PMID: 33591346.
Recommended Products






Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.
